Coronary artery aneurysms — MCQs

A 6-year-old boy presents to his pediatrician accompanied by his mother for evaluation of a rash. The rash appeared a little over a week ago, and since that time the boy has felt tired. He is less interested in playing outside, preferring to remain indoors because his knees and stomach hurt. His past medical history is significant for an upper respiratory infection that resolved uneventfully without treatment 2 weeks ago. Temperature is 99.5°F (37.5°C), blood pressure is 115/70 mmHg, pulse is 90/min, and respirations are 18/min. Physical exam shows scattered maroon macules and papules on the lower extremities. The abdomen is diffusely tender to palpation. There is no cervical lymphadenopathy or conjunctival injection. Which of the following will most likely be found in this patient?
A 4-year-old boy is brought to the emergency department by his mother with a rash on his trunk, malaise, and fever with spikes up to 38.5°C (101.3°F) for the past 2 weeks. The patient's mother says she tried giving him Tylenol with little improvement. Past medical history includes a spontaneous vaginal delivery at full term. The patient's vaccines are up-to-date and he has met all developmental milestones. On physical examination, his lips are cracking, and he has painful cervical lymphadenopathy. The rash is morbilliform and involves his trunk, palms, and the soles of his feet. There is fine desquamation of the skin of the perianal region. Which of the following anatomical structures is most important to screen for possible complications in this patient?
A 5-year-old girl is brought to the emergency department by her father due to a 6-day history of fevers and irritability. His father reports that the fevers have ranged from 101-104°F (38.3-40°C). He tried to give her ibuprofen, but the fevers have been unresponsive. Additionally, she developed a rash 3 days ago and has refused to wear shoes because they feel "tight." Her father reports that other than 2 ear infections she had when she was younger, the patient has been healthy. She is up-to-date on her vaccinations except for the vaccine boosters scheduled for ages 4-6. The patient's temperature is 103.5°F (39.7°C), blood pressure is 110/67 mmHg, pulse is 115/min, and respirations are 19/min with an oxygen saturation of 98% O2 on room air. Physical examination shows bilateral conjunctivitis, palpable cervical lymph nodes, a diffuse morbilliform rash, and desquamation of the palms and soles with swollen hands and feet. Which of the following is the next step in management?
A 62-year-old man with a past medical history of previous myocardial infarction, angina, hypertension, hyperlipidemia, diabetes mellitus, peripheral vascular disease, and below knee amputation has developed new chest pain. His medication includes insulin, hydrochlorothiazide, lisinopril, metoprolol, daily aspirin, atorvastatin, and nitroglycerin as needed. His vitals include: blood pressure 135/87 mm Hg, pulse 52/min, and respirations 17/min. Coronary arteriography shows a reduced ejection fraction, a 65% stenosis of the left anterior descending artery, and a 75% stenosis of the left circumflex artery. Which of the following is the recommended treatment for the patient?
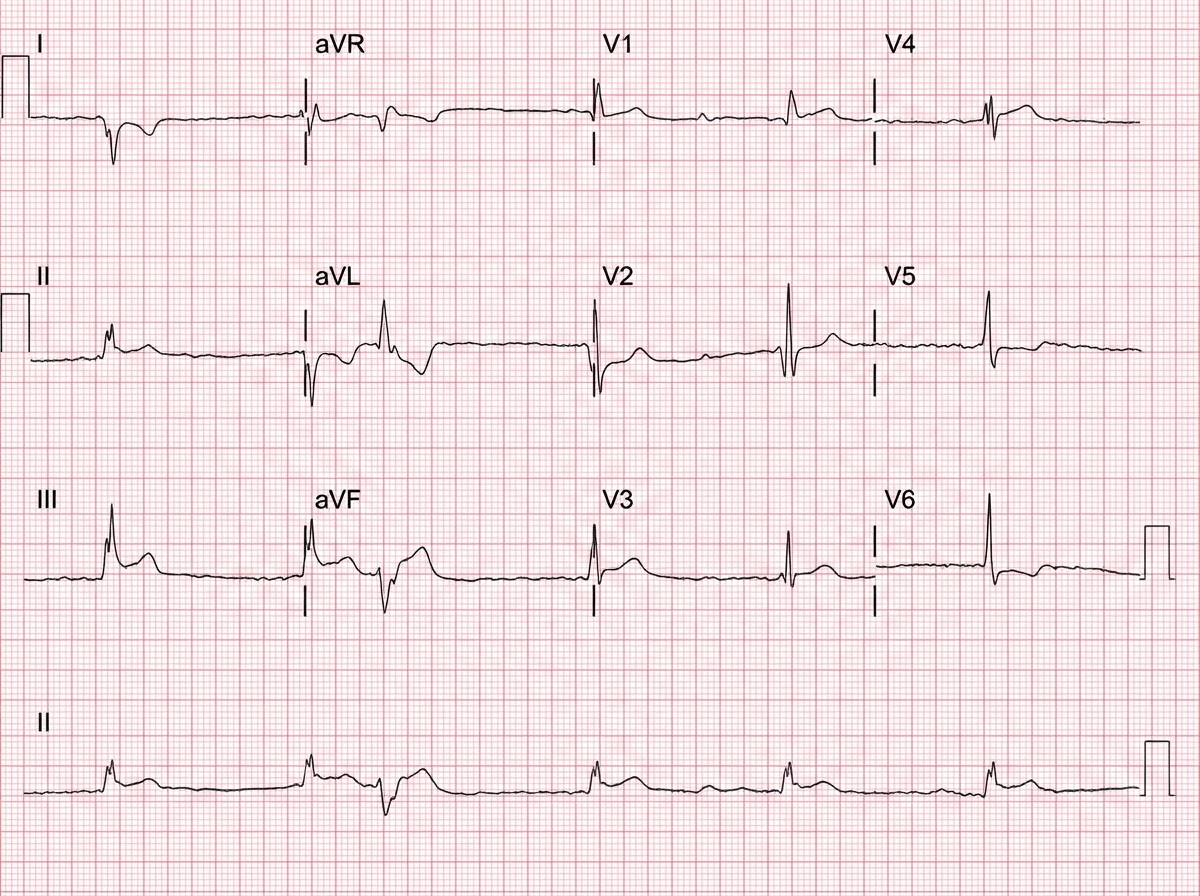
A 49-year-old man was brought to the emergency department by ambulance with complaints of sudden-onset chest pain that radiates into his neck and down his left arm. This substernal pain started 2 hours ago while he was having dinner. His past medical history is remarkable for hypercholesterolemia that is responsive to therapy with statins and coronary artery disease. His temperature is 37.0°C (98.6°F), blood pressure is 155/90 mm Hg, pulse is 112/min, and respiratory rate is 25/min. Troponin I levels are elevated. A 12-lead ECG was performed (see image). What is the most likely etiology of this patient’s presentation?
A 75-year-old Caucasian man presents to the emergency department with abdominal pain. The patient states he was at home eating dinner when he began to experience severe abdominal pain. The patient has a past medical history of diabetes, hypertension, and atherosclerosis. He lives at home alone, smokes cigarettes, and drinks 1 to 2 alcoholic drinks per day. The patient is given IV morphine and an ultrasound is obtained demonstrating a dilated abdominal aorta. The patient states that his father died of a similar finding and is concerned about his prognosis. Which of the following is the greatest risk factor for this patient's presentation?
A 65-year-old man is brought to the emergency department with central chest pain for the last hour. He rates his pain as 8/10, dull in character, and says it is associated with profuse sweating and shortness of breath. He used to have heartburn and upper abdominal pain associated with food intake but had never experienced chest pain this severe. He has a history of diabetes, hypertension, and hypercholesterolemia. His current medication list includes amlodipine, aspirin, atorvastatin, insulin, valsartan, and esomeprazole. He has smoked 1 pack of cigarettes per day for the past 35 years. Physical examination reveals: blood pressure 94/68 mm Hg, pulse 112/min, oxygen saturation 95% on room air, and BMI 31.8 kg/m2. His lungs are clear to auscultation. An electrocardiogram (ECG) shows ST-segment elevations in the inferior leads. The patient is discharged home after 3 days on aspirin, clopidogrel, and atenolol in addition to his previous medications. He is advised to get an exercise tolerance test (ETT) in one month. A month later at his ETT, his resting blood pressure is 145/86 mm Hg. The pre-exercise ECG shows normal sinus rhythm with Q waves in the inferior leads. After 3 minutes of exercise, the patient develops chest pain that is gradually worsening, and repeat blood pressure is 121/62 mm Hg. No ischemic changes are noted on the ECG. What is the most appropriate next step?
A 60-year-old male presents for a routine health check-up. The patient complains of reduced exercise tolerance for the past 2 years. Also, in the past year, he has noticed chest pain after climbing the stairs in his home. He has no significant past medical history or current medications. The patient reports a 45-pack-year smoking history. The vital signs include temperature 37.0°C (98.6°F), blood pressure 160/100 mm Hg, pulse 72/min, respiratory rate 15/min, and oxygen saturation 99% on room air. His body mass index (BMI) is 34 kg/m2. Physical examination is unremarkable. Laboratory studies show: Serum total cholesterol 265 mg/dL HDL 22 mg/dL LDL 130 mg/dL Triglycerides 175 mg/dL HDL: high-density lipoprotein; LDL: low-density lipoprotein Which of the following vascular pathologies is most likely present in this patient?
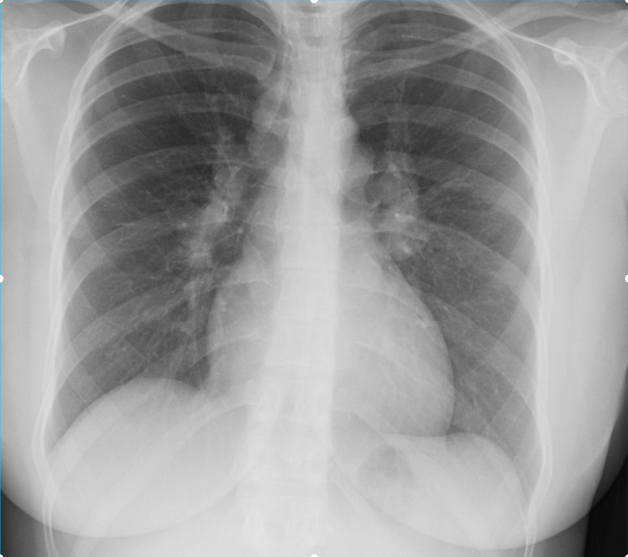
A 26-year-old man comes to the physician because of a 1-week history of left-sided chest pain. The pain is worse when he takes deep breaths. Over the past 6 weeks, he had been training daily for an upcoming hockey tournament. He does not smoke cigarettes or drink alcohol but has used cocaine once. His temperature is 37.1°C (98.7°F), pulse is 75/min, and blood pressure is 128/85 mm Hg. Physical examination shows tenderness to palpation of the left chest. An x-ray of the chest is shown. Which of the following is the most appropriate initial pharmacotherapy?
A 49-year-old man with a past medical history of hypertension on amlodipine presents to your office to discuss ways to lessen his risk of complications from heart disease. After a long discussion, he decides to significantly decrease his intake of trans fats in an attempt to lower his risk of coronary artery disease. Which type of prevention is this patient initiating?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
