Kawasaki disease — MCQs

On this page
A 4-year-old boy is brought to the physician by his parents because of fever and mild abdominal pain for 7 days. His parents report that he developed a rash 2 days ago. He has had no diarrhea or vomiting. Four weeks ago, he returned from a camping trip to Colorado with his family. His immunization records are unavailable. His temperature is 39.4°C (102.9°F), pulse is 111/min, respirations are 27/min, and blood pressure is 96/65 mm Hg. Examination shows bilateral conjunctival injections and fissures on his lower lips. The pharynx is erythematous. There is tender cervical lymphadenopathy. The hands and feet appear edematous. A macular morbilliform rash is present over the trunk. Bilateral knee joints are swollen and tender; range of motion is limited by pain. Which of the following is the most appropriate treatment for this patient's condition?
A 4-year-old boy is brought to a pediatrician by his parents with a history of fever for the last 5 days and irritability, decreased appetite, vomiting, and swelling of the hands and feet for the last 3 days. The patient’s mother mentions that he has been taking antibiotics and antipyretics prescribed by another physician for the last 3 days, but there has been no improvement His temperature is 39.4°C (103.0°F), pulse is 128/min, respiratory rate is 24/min, and blood pressure is 96/64 mm Hg. On physical examination, there is significant edema of the hands and feet bilaterally. There is a 2.5 cm diameter freely moveable, nontender cervical lymph node is palpable on the right side. A strawberry tongue and perianal erythema are noted. Conjunctival injection is present bilaterally. Laboratory findings reveal mild anemia and a leukocytosis with a left-shift. Erythrocyte sedimentation rate (ESR) and serum C-reactive protein (CRP) are increased. If not treated appropriately, this patient is at increased risk of developing which of the following complications?
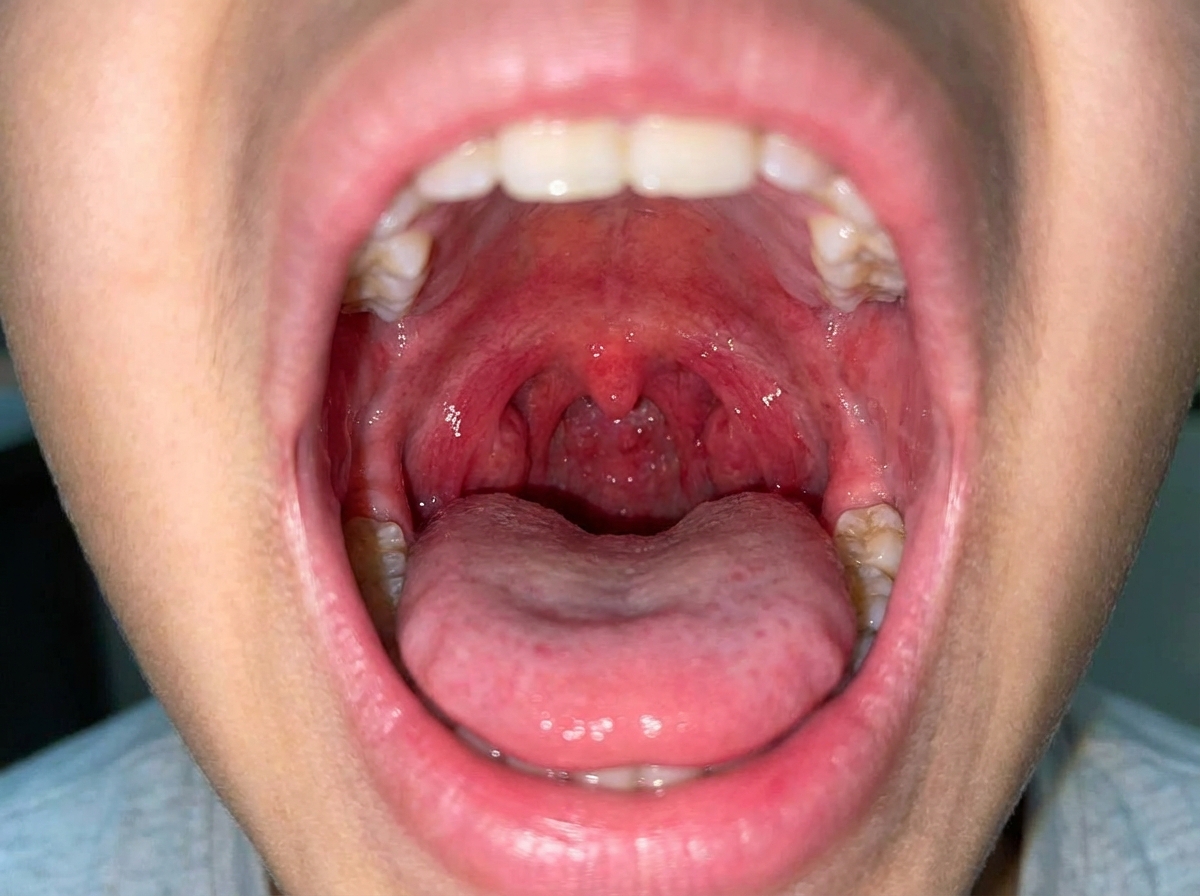
A 5-year-old girl presents with a rash and a persistent fever of 41.0°C (105.8°F), not relieved by Tylenol. The patient's mother says that her symptoms started 5 days ago and have not improved. The rash started on her trunk and now is present everywhere including the palms and soles. Her birth history is normal. Her pulse is 120/min and respiratory rate is 22/min. On physical examination, the patient is agitated and ill-appearing. There is significant swelling of the distal upper and lower extremities bilaterally. The pharynx is hyperemic (see image). Generalized edema with palpable cervical lymphadenopathy is noted. Muscle tone is normal. Remainder of exam is unremarkable. Laboratory findings are significant for the following: Laboratory test Hb 9 g/dL RBC 3.3/mm3 Neutrophilic leukocytosis 28,000/mm3 Normal platelet count 200,000/mm3 Serum ɣ-GT increased Hyperbilirubinemia 2.98 mg/dL AST and ALT are normal, but there is markedly increased serum CRP. Which of the following is the most likely diagnosis in this patient?
A previously healthy 4-year-old boy is brought to the physician by his parents because he has had a fever, diffuse joint pain, and a rash on his abdomen for the past week. Acetaminophen did not improve his symptoms. He emigrated from China with his family 2 years ago. He attends daycare. His immunization records are not available. His temperature is 38.5°C (101.3°F), pulse is 125/min, and blood pressure is 100/60 mm Hg. Examination shows polymorphous truncal rash. The eyes are pink with no exudate. The tongue is shiny and red, and the lips are cracked. The hands and feet are red and swollen. There is right-sided anterior cervical lymphadenopathy. Which of the following is the most appropriate next step in management?
A 4-year-old boy is brought to the emergency department by his mother with a rash on his trunk, malaise, and fever with spikes up to 38.5°C (101.3°F) for the past 2 weeks. The patient's mother says she tried giving him Tylenol with little improvement. Past medical history includes a spontaneous vaginal delivery at full term. The patient's vaccines are up-to-date and he has met all developmental milestones. On physical examination, his lips are cracking, and he has painful cervical lymphadenopathy. The rash is morbilliform and involves his trunk, palms, and the soles of his feet. There is fine desquamation of the skin of the perianal region. Which of the following anatomical structures is most important to screen for possible complications in this patient?
A previously healthy 3-year-old girl is brought to the physician by her parents for the evaluation of recurrent episodes of pain in her left wrist and right knee for 4 months. She has not had any trauma to the knee or any previous problems with her joints. She attends daycare. Her mother has rheumatoid arthritis. Her vital signs are within normal limits. Examination of the right knee and left wrist shows mild swelling, tenderness, warmth, and erythema; range of motion is slightly decreased. No other joints are affected. The remainder of the examination shows no abnormalities. Laboratory studies show: Hemoglobin 12.4 g/dL Leukocyte count 9,000/mm3 Platelet count 200,000/mm3 Erythrocyte sedimentation rate 50 mm/h Serum Antinuclear antibodies 1:320 Rheumatoid factor negative This patient is at increased risk for which of the following complications?
A 4-year-old boy is brought to the emergency department by his parents after 10 days of fever, varying from 38.0–40.0°C (100.4–104.0°F). On physical examination, the child is ill-looking with an extensive rash over his trunk with patchy desquamation. His hands are swollen, and he also shows signs of a bilateral conjunctivitis. The laboratory test results are as follows: Hemoglobin 12.9 g/dL Hematocrit 37.7% Mean corpuscular volume 82.2 μm3 Leukocyte count 10,500/mm3 Neutrophils 65% Lymphocytes 30% Monocytes 5% Platelet count 290,000/mm3 Erythrocyte sedimentation rate (ESR) 35 mm/h What is the next best step in the management of this patient’s condition?
A 9-year-old boy is brought to the emergency department because of progressively worsening shortness of breath for 3 days. He has had fever and malaise for the past 5 days. He had a sore throat 3 weeks ago that resolved without treatment. He appears ill. His temperature is 38.6°C (101.5°F), pulse is 98/min and blood pressure is 84/62 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 93%. Examination shows jugular venous distension and bilateral ankle edema. There are erythematous, ring-shaped macules and patches over his trunk that are well-demarcated. Auscultation of the chest shows crackles at the lung bases bilaterally. An S3 is heard on cardiac auscultation. His hemoglobin concentration is 12.2 g/dL, leukocyte count is 13,600/mm3, and platelet count is 280,000/mm3. A urinalysis is normal. An x-ray of the chest shows cardiac silhouette enlargement with prominent vascular markings in both the lung fields. Which of the following is the most likely etiology of this patient's symptoms?
A 5-year-old girl is brought to the emergency department by her father due to a 6-day history of fevers and irritability. His father reports that the fevers have ranged from 101-104°F (38.3-40°C). He tried to give her ibuprofen, but the fevers have been unresponsive. Additionally, she developed a rash 3 days ago and has refused to wear shoes because they feel "tight." Her father reports that other than 2 ear infections she had when she was younger, the patient has been healthy. She is up-to-date on her vaccinations except for the vaccine boosters scheduled for ages 4-6. The patient's temperature is 103.5°F (39.7°C), blood pressure is 110/67 mmHg, pulse is 115/min, and respirations are 19/min with an oxygen saturation of 98% O2 on room air. Physical examination shows bilateral conjunctivitis, palpable cervical lymph nodes, a diffuse morbilliform rash, and desquamation of the palms and soles with swollen hands and feet. Which of the following is the next step in management?
A 4-year-old male is brought to the pediatrician for a low-grade fever. His mother states that he has had a waxing and waning fever for the past 6 days with temperatures ranging from 99.8°F (37.7°C) to 101.0°F (38.3°C). She reports that he had a similar episode three months ago. She also reports symmetric joint swelling in the child’s knees and wrists that has become increasingly noticeable over the past 8 weeks. He has not had a cough, difficulty breathing, or change in his bowel movements. The child was born at 40 weeks gestation. His height and weight are in the 45th and 40th percentiles, respectively. He takes no medications. His temperature is 100.1°F (37.8°C), blood pressure is 100/65 mmHg, pulse is 105/min, and respirations are 18/min. On examination, there is a non-pruritic, macular, salmon-colored truncal rash. Serological examination reveals the following: Serum: Rheumatoid factor: Negative Anti-nuclear antibody: Negative Anti-double stranded DNA: Negative Anti-SSA: Negative Anti-SSB: Negative Human leukocyte antigen B27: Positive Erythrocyte sedimentation rate: 30 mm/h This patient is most likely at increased risk of developing which of the following?
Practice by Chapter
Diagnostic criteria and clinical features
Practice Questions
Atypical Kawasaki presentation
Practice Questions
Laboratory findings
Practice Questions
Cardiac complications and evaluation
Practice Questions
Acute phase management
Practice Questions
IVIG resistance
Practice Questions
Coronary artery aneurysms
Practice Questions
Long-term cardiac follow-up
Practice Questions
Differential diagnosis
Practice Questions
Recurrence risk
Practice Questions
Pathophysiology theories
Practice Questions
Age-specific considerations
Practice Questions
Long-term outcomes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
