Infectious Disease — MCQs

On this page
A 9-year-old girl presents with a 3-week history of cough. Her mother reports that initially, she had a runny nose and was tired, with a slight cough, but as the runny nose resolved, the cough seemed to get worse. She further states that the cough is dry sounding and occurs during the day and night. She describes having coughing spasms that occasionally end in vomiting, but between episodes of coughing she is fine. She reports that during a coughing spasm, her daughter will gasp for air and sometimes make a “whooping” noise. A nasopharyngeal swab confirms a diagnosis of Bordetella pertussis. Which of the following statements apply to this patient?
An 18-month-old girl is brought to the emergency department because of stiffening and jerking movements that began in her right arm and then spread to involve her whole body, followed by unresponsiveness that occurred 1 hour ago. Her symptoms lasted < 10 minutes. She has had coryza for 24 hours without any fever. She had an episode of a febrile generalized tonic-clonic seizure 6 months ago. Her past medical history has otherwise been unremarkable. Her vaccination history is up to date. Her uncle has epilepsy. Her temperature is 38.9°C (102.0°F). Other than nasal congestion, physical examination shows no abnormal findings. Which of the following factors most strongly indicates the occurrence of subsequent epilepsy?
An 18-month-old boy is brought to the doctor’s office for evaluation of abdominal pain. The boy looks emaciated and he is now significantly below his growth chart predicted weight. The family history is non-contributory. The vital signs are unremarkable. On physical examination, a non-tender mass is felt in the upper part of the abdomen. A magnetic resonance image (MRI) scan of his abdomen demonstrates a mass in his right adrenal gland. Biopsy of the mass demonstrates an abundance of small round blue cells. With this biopsy result, which 1 of the following findings would confirm the diagnosis?
A 7-year-old boy is brought to his pediatrician by his parents because of a new rash. The family immigrated from Laos one year ago and recently obtained health insurance. A week ago, the boy stated that he was “not feeling well” and asked to stay home from school. At the time, he starting having cough, nasal congestion, and irritated eyes – symptoms that persisted and intensified. His parents recall that at the time they noticed small whitish-blue papules over the red buccal mucosa opposite his molars. Five days ago, his parents noticed a red rash around his face that quickly spread downward to cover most of his arms, trunk, and then legs. His temperature is 102.5°F (39.2°C), blood pressure is 110/85 mmHg, pulse is 102/min, and respirations 25/min. On physical exam, he has intermittent cough, cervical lymphadenopathy, and nonpurulent conjunctivitis accompanied by a confluent, dark red rash over his body. This patient is at risk for which of the following complications later in life?
An 11-month-old boy is brought to the physician for the evaluation of recurrent otitis media since birth. The patient’s immunizations are up-to-date. He is at the 5th percentile for height and weight. Physical examination shows multiple petechiae and several eczematous lesions over the scalp and extremities. The remainder of the examination reveals no abnormalities. Laboratory studies show a leukocyte count of 9,600/mm3 (61% neutrophils and 24% lymphocytes), a platelet count of 29,000/mm3, and an increased serum IgE concentration. Which of the following is the most likely diagnosis?
A 3-year-old girl is brought to the physician because of a cough for 2 days. The cough occurs as paroxysmal spells, with vomiting sometimes occurring afterwards. She takes a deep breath after these spells that makes a whooping sound. She has been unable to sleep well because of the cough. She had a runny nose and low-grade fever 1 week ago. She was admitted at the age of 9 months for bronchiolitis. Her immunizations are incomplete, as her parents are afraid of vaccine-related complications. She attends a daycare center but there have been no other children who have similar symptoms. She appears well. Cardiopulmonary examination shows no abnormalities. Her hemoglobin concentration is 13.3 g/dL, leukocyte count is 41,000/mm3, platelet count is 230,000/mm3 and erythrocyte sedimentation rate is 31 mm/hr. An x-ray of the chest is unremarkable. The patient is at increased risk for which of the following complications?
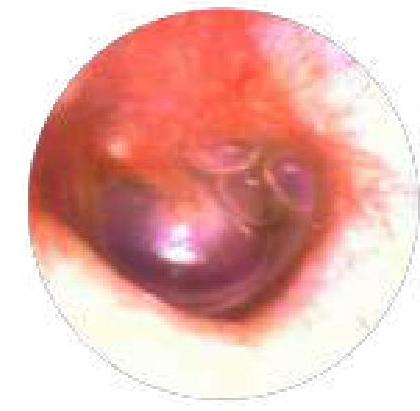
An 11-month-old boy is brought to the pediatrician by his mother due to fever and tugging at his right ear. The mother says that he is currently irritable with a mild fever. About 1 week ago, he had a mild cough, mild fever, body aches, and a runny nose. He was treated with children's Tylenol and the symptoms resolved after a few days. The child lives in an apartment with his mother, grandmother, and father. His grandmother watches him during the day. There have been no sick contacts at home. His father smokes cigarettes on the balcony. There is no pertinent family history. He was born full term by spontaneous vaginal delivery. He is progressing through his developmental milestones and is up to date on his vaccines. His temperature is 39.3°C (102.7°F), pulse is 122/min, and respirations are 24/min. The child appears cranky and requires consoling during the physical exam. His heart and lung exam are normal. He has a red and mildly swollen right ear. Otoscopic evaluation of the right ear reveals the finding shown in the image below. Which of the following most likely contributed to this patient's condition?
A 5-month-old boy is brought to the physician by his mother because of poor weight gain and chronic diarrhea. He has had 3 episodes of otitis media since birth. Pregnancy and delivery were uncomplicated but his mother received no prenatal care. His immunizations are up-to-date. He is at the 10th percentile for height and 5th percentile for weight. Physical examination shows thick white plaques on the surface of his tongue that can be easily scraped off with a tongue blade. Administration of which of the following is most likely to have prevented this patient's condition?
A 2-year-old boy is brought to the pediatrician with complaints of fever and a skin rash for the past 2 days. The boy was born by normal vaginal delivery at full term, and his neonatal period was uneventful. He has a history of severe pain in his legs and difficulty eating. His temperature is 38.6°C (101.4°F), pulse is 102/min, and respiratory rate is 22/min. Physical examination shows multiple papules on the hands, feet, and trunk. His neurologic examination shows decreased muscle strength in the lower limbs. On intraoral examination, multiple reddish 2 mm macules are present on the hard palate. Which of the following is the most likely causal organism?
A 9-year-old girl is brought to the pediatrician by her father for dysuria, genital pruritus, and vaginal discharge. Cultures of the discharge are sent, revealing the causative agent to be a Gram-negative glucose-fermenting, non-maltose fermenting diplococci. Which of the following steps should the physician follow next?
Practice by Chapter
Common childhood exanthems
Practice Questions
Pediatric respiratory infections
Practice Questions
Pediatric gastrointestinal infections
Practice Questions
Urinary tract infections in children
Practice Questions
Bone and joint infections
Practice Questions
Central nervous system infections
Practice Questions
Pediatric tuberculosis
Practice Questions
Pediatric HIV
Practice Questions
Recurrent infections evaluation
Practice Questions
Fever of unknown origin approach
Practice Questions
Emerging infectious diseases in children
Practice Questions
Post-infectious immune complications
Practice Questions
Antimicrobial resistance in pediatrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
