Infectious Disease — MCQs

On this page
A 7-year-old boy is brought to the emergency department because of a 3-day history of generalized fatigue, myalgia, and fever. He has sickle cell disease. His current medications include hydroxyurea and folic acid. He appears ill. His temperature is 39.2°C (102.6°F), pulse is 103/min, and respirations are 28/min. Examination shows pale conjunctivae. The lungs are clear to auscultation. The abdomen is soft and nontender. Neurologic examination shows no focal findings, His hemoglobin concentration is 10.3 g/dL and leukocyte count is 14,100/mm3. Intravenous fluid is administered and blood cultures are obtained. Which of the following is the most appropriate next step in treatment?
A 7-year-old male is admitted to the hospital with his fourth episode of wheezing and dyspnea. His symptoms are exacerbated by mold and pollen. Which of the following is most likely to be observed in this patient?
A 2-month-old girl is admitted to the hospital because of a 1-day history of fever and difficulty breathing. She has also had nasal congestion for 2 days. She was born at 28 weeks' gestation and weighed 1105 g (2 lb 7 oz); she currently weighs 2118 g (4 lb 11 oz). Her neonatal course was complicated by respiratory distress syndrome. She required supplemental oxygen for 36 days following birth. She was diagnosed with bronchopulmonary dysplasia 3 weeks ago. The infant missed an appointment with the pediatrician 2 weeks ago. Her only medication is vitamin D drops. She appears lethargic. Her temperature is 38.6°C (101.4°F), pulse is 160/min, respirations are 55/min, and blood pressure is 80/45 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 87%. Physical examination shows moderate subcostal retractions. Wheezing is heard on auscultation of the chest. Her hemoglobin concentration is 10.5 g/dL, leukocyte count is 13,000/mm3, and platelet count is 345,000/mm3. Mechanic ventilatory support is initiated. After 4 days in the pediatric intensive care unit, the patient dies. Administration of which of the following is most likely to have prevented this patient's outcome?
A 7-year-old boy presents to the pediatric emergency department for knee pain. The child fell while riding his skateboard yesterday. He claims that ever since then he has had swelling and knee pain that is severe. His parents state that he has trouble walking due to the pain. The child has a past medical history of seasonal allergies and asthma. His current medications include loratadine, albuterol, and fluticasone. His temperature is 99.5°F (37.5°C), blood pressure is 95/48 mmHg, pulse is 110/min, respirations are 17/min, and oxygen saturation is 98% on room air. On physical exam, you note a young boy laying on the stretcher in pain. Cardiopulmonary exam is within normal limits. Inspection of the patient's left knee reveals an erythematous knee that is tender and warm to the touch. Passive movement of the knee elicits pain. The patient refuses to walk so you are unable to assess his gait. Which of the following is the best initial step in management?
Multiple patients present to your office with hematuria following an outbreak of Group A Streptococcus. Biopsy reveals that all of the patients have the same disease, characterized by large, hypercellular glomeruli with neutrophil infiltration. Which patient has the best prognosis?
A 12-year-old African American boy is brought to the emergency room due to a severely painful penile erection for the past 5 hours. He was attending a class at his school when his penis became spontaneously tumescent. A complete blood count and a cavernous blood gas analysis showed the following: Hemoglobin (Hb) 11.5 g/dL; 14.5 g/dL (-2SD 13.0 g/dL) for boys 12–18 years of age Mean corpuscular volume (MCV) 95 fL; 80–96 fL Platelet count 250,000/mm3 pO2 38 mm Hg pCO2 65 mm Hg pH 7.25 sO2 % 60% HCO3- 10 mEq/L A peripheral blood smear reveals RBCs with Howell-Jolly bodies. Rapid detumescence is achieved after aspiration of blood and administration of an adrenergic agonist and analgesia. Which of the following etiologies should be considered in this patient?
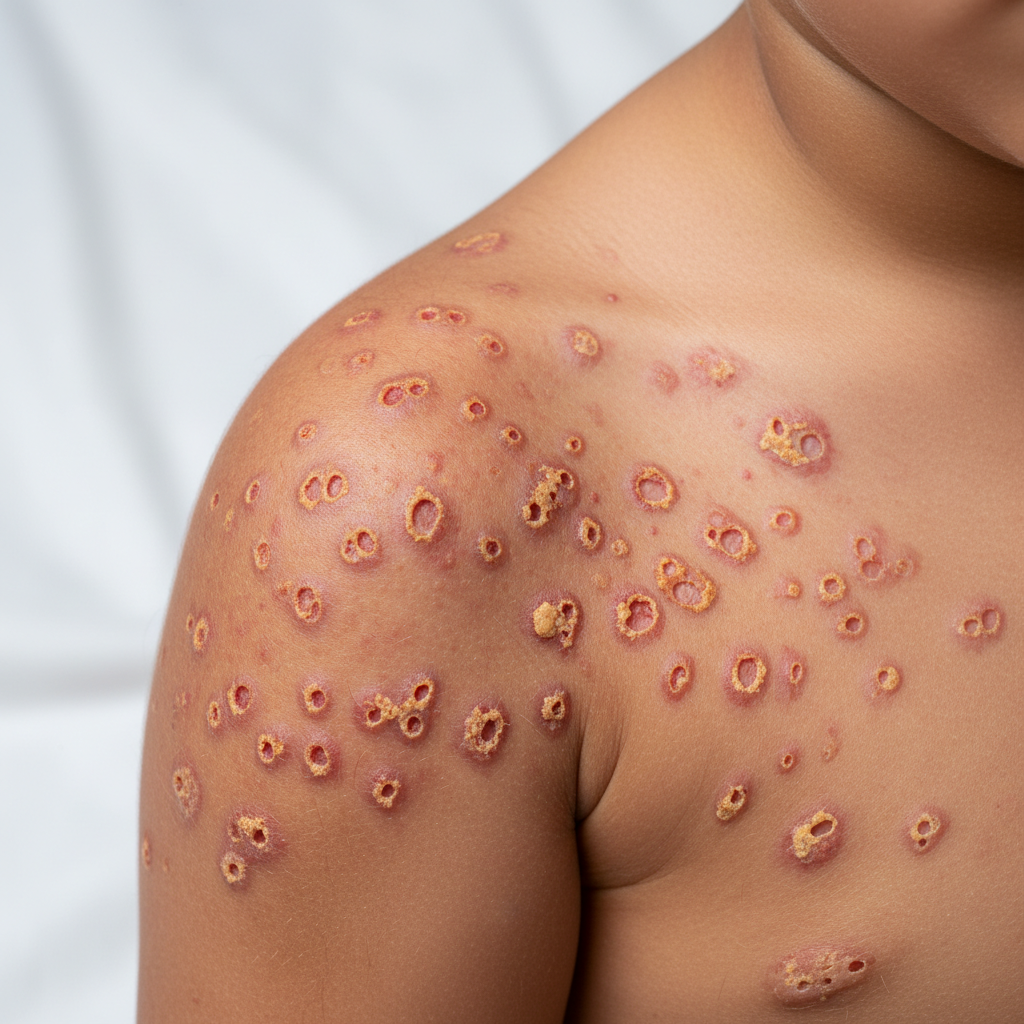
A 12-year-old boy is brought to the physician because of fever, malaise, and a painful, itchy rash on the right shoulder for 2 weeks. The patient's mother says the boy's condition has worsened over the past 4 days. He has a history of atopic dermatitis. He has lived with his mother at several public shelters since she separated from his physically abusive father 2 months ago. His immunizations are up-to-date. There is cervical lymphadenopathy. Laboratory studies show no abnormalities. A photograph of the rash is shown. Which of the following is the most likely diagnosis?
A 10-year-old girl is brought to the physician because of a severe, throbbing headache for 1 hour. The headache is located in the right frontotemporal region. It is her fifth such headache in the past 2 months. Her mother says that all the previous episodes started after soccer practice, following which the child would lock herself in her room, close the curtains, and sleep for a few hours. After waking up, the headache is either diminished or has stopped entirely. One month ago, the child was diagnosed with myopic vision and has been wearing glasses since. Her 4-year-old brother had herpetic gingivostomatitis 2 months ago. Her vital signs are within normal limits. Funduscopic examination is inconclusive because the child is uncooperative. The remainder of the examination shows no abnormalities. Which of the following is the most appropriate next step in management?
A 3-year-old girl is brought to the physician by her parents because of a barking cough, a raspy voice, and noisy breathing for the last 3 days. Five days ago, she had a low-grade fever and runny nose. She attends daycare. Her immunizations are up-to-date. Her temperature is 37.8°C (100°F) and respirations are 33/min. Physical examination shows supraclavicular retractions. There is a high-pitched sound present on inspiration. Examination of the throat shows erythema without exudates. Which of the following is the most likely location of the anatomic narrowing causing this patient's symptoms?
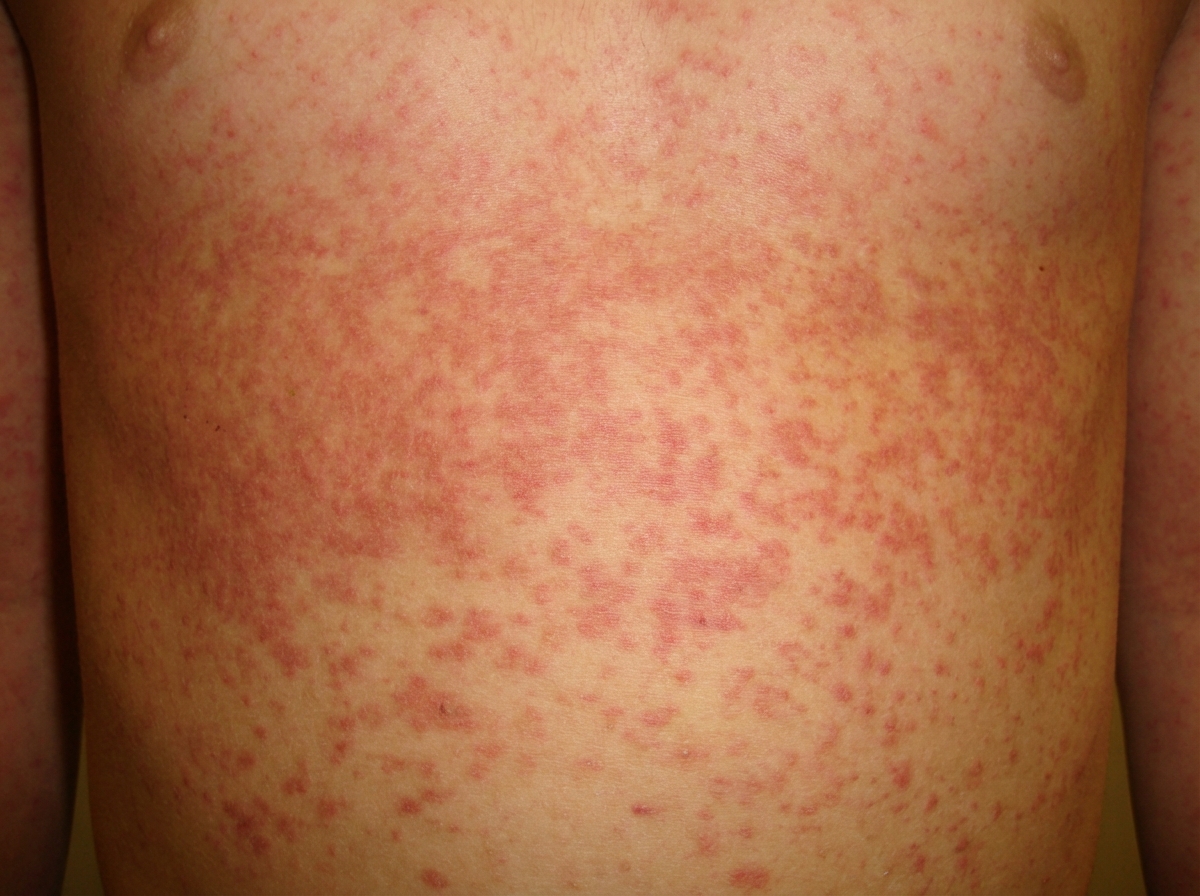
A 4-year-old boy is brought to the physician by his father because of a 3-day history of generalized rash. The rash is not pruritic. He has no cough. He has had a fever and a sore throat for 4 days. He was born at term and has been healthy except for an episode of tonsillitis 6 months ago treated with erythromycin. His immunizations are up-to-date. His temperature is 38.5°C (101.3°F). Examination shows cervical lymphadenopathy. The tongue is bright red. There is tonsillar erythema without any exudate. A photograph of the rash is shown. Which of the following is the most appropriate next step in management?
Practice by Chapter
Common childhood exanthems
Practice Questions
Pediatric respiratory infections
Practice Questions
Pediatric gastrointestinal infections
Practice Questions
Urinary tract infections in children
Practice Questions
Bone and joint infections
Practice Questions
Central nervous system infections
Practice Questions
Pediatric tuberculosis
Practice Questions
Pediatric HIV
Practice Questions
Recurrent infections evaluation
Practice Questions
Fever of unknown origin approach
Practice Questions
Emerging infectious diseases in children
Practice Questions
Post-infectious immune complications
Practice Questions
Antimicrobial resistance in pediatrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
