Infectious Disease — MCQs

On this page
A 5-year-old boy is brought to the emergency department for evaluation of a progressive rash that started 2 days ago. The rash began on the face and progressed to the trunk and extremities. Over the past week, he has had a runny nose, a cough, and red, crusty eyes. He immigrated with his family from Turkey 3 months ago. His father and his older brother have Behcet disease. Immunization records are unavailable. The patient appears irritable and cries during the examination. His temperature is 40.0°C (104°F). Examination shows general lymphadenopathy and dry mucous membranes. Skin turgor is decreased. There is a blanching, partially confluent erythematous maculopapular exanthema. Examination of the oral cavity shows small white spots with erythematous halos on the buccal mucosa. His hemoglobin concentration is 11.5 g/dL, leukocyte count is 6,000/mm3, and platelet count is 215,000/mm3. Serology confirms the diagnosis. Which of the following is the most appropriate next step in management?
A 3-year-old boy is brought to the emergency department with abdominal pain. His father tells the attending physician that his son has been experiencing severe stomach aches over the past week. They are intermittent in nature, but whenever they occur he cries and draws up his knees to his chest. This usually provides some relief. The parents have also observed mucousy stools and occasional bloody stools that are bright red with blood clots. They tell the physician that their child has never experienced this type of abdominal pain up to the present. The boy was born at 39 weeks gestation via spontaneous vaginal delivery. He is up to date on all vaccines and is meeting all developmental milestones. On physical exam, his vitals are generally normal with a slight fever and mild tachycardia. The boy appears uncomfortable. An abdominal exam reveals a sausage-shaped mass in the right upper abdomen. Which of the following is the LEAST likely cause of these symptoms?
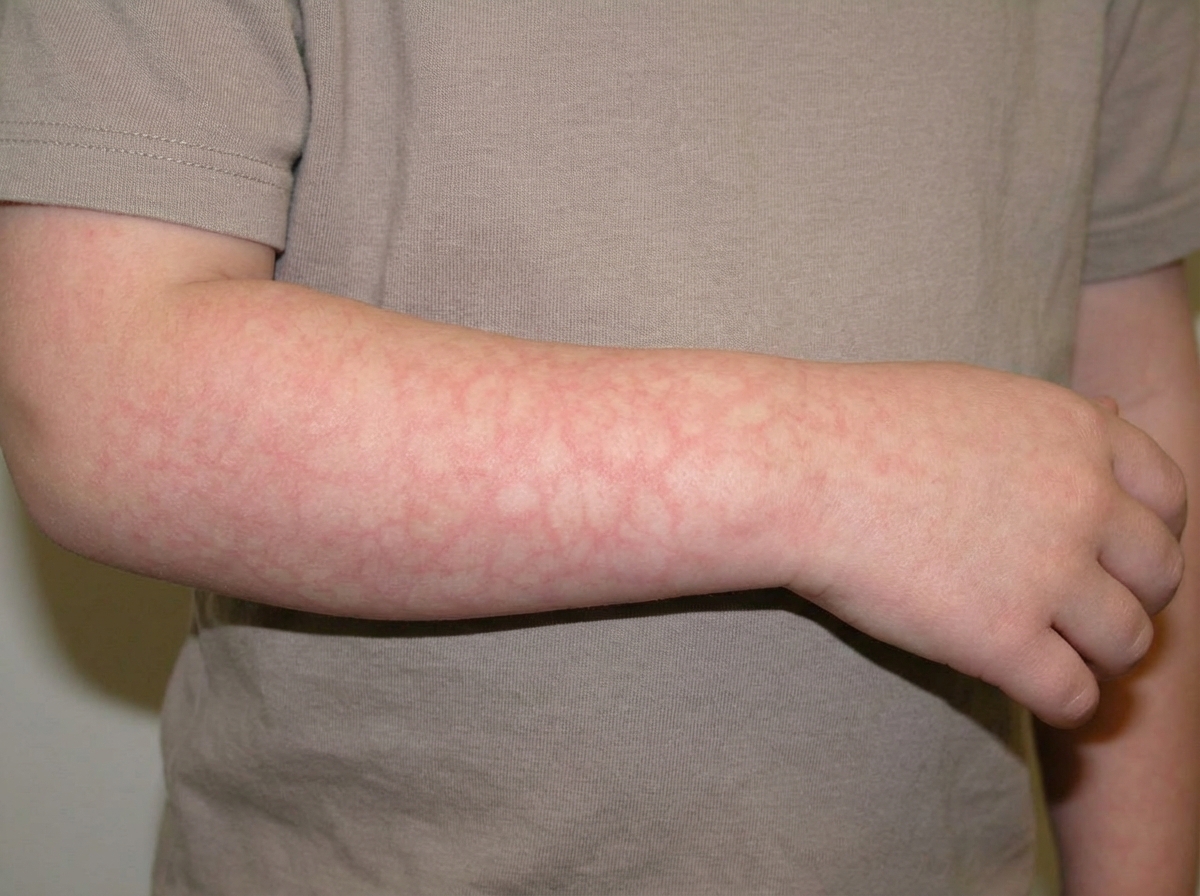
An 11-year-old girl is brought to the physician by her parents because of a mildly pruritic rash on her trunk and extremities for 2 days. One week ago, she developed a low-grade fever, rhinorrhea, and headache, followed by a facial rash 4 days later. The facial rash did not involve the perioral skin. Her temperature is 37.4°C (99.3°F). A photograph of the rash on her lower arms is shown. Which of the following is the most likely diagnosis?
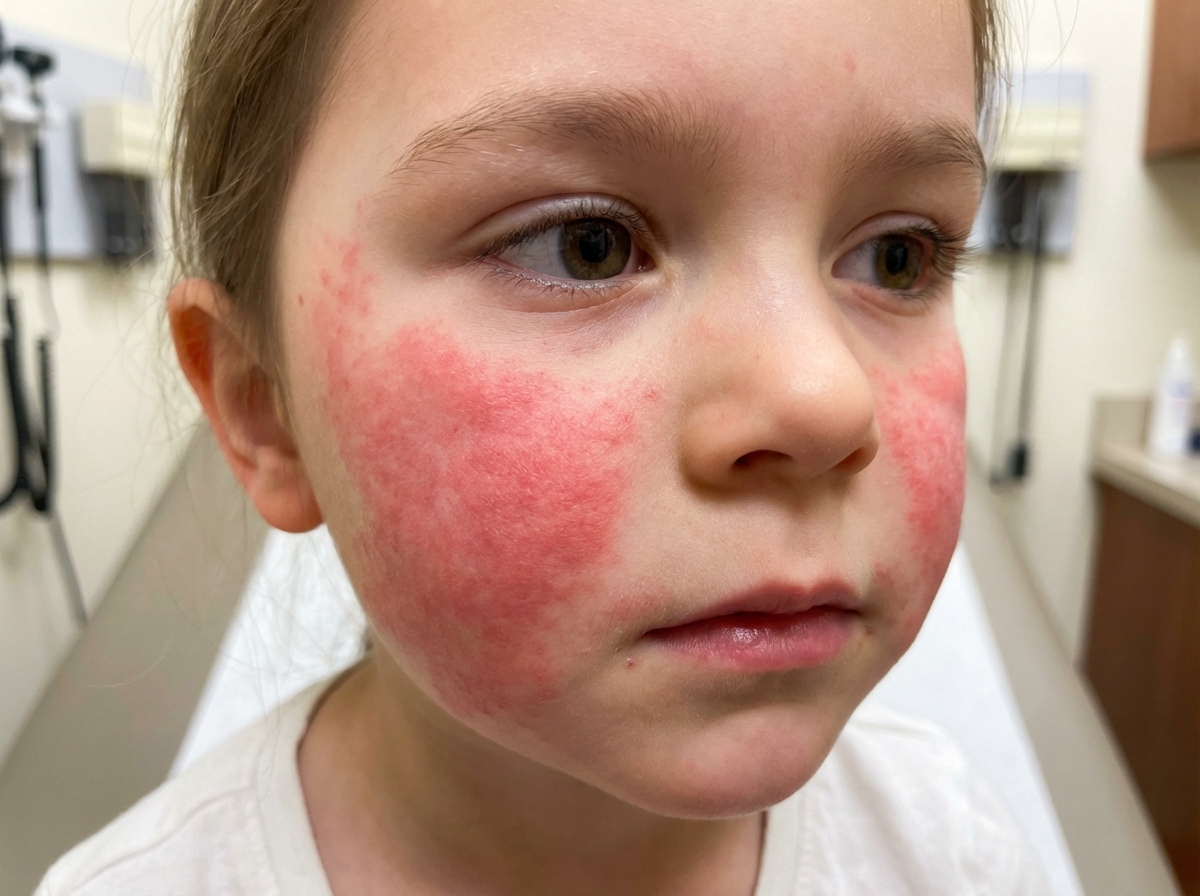
A 4-year-old boy is brought to the clinic by his mother with fever and a rash. The patient’s mother says his symptoms started 1 week ago with the acute onset of fever and a runny nose, which resolved over the next 3 days. Then, 4 days later, she noted a rash on his face, which, after a day, spread to his neck, torso, and extremities. The patient denies any pruritus or pain associated with the rash. No recent history of sore throat, chills, or upper respiratory infection. The patient has no significant past medical history and takes no medications. The vital signs include: temperature 37.2°C (99.9°F) and pulse 88/min. On physical examination, there is a maculopapular rash on his face, torso, and extremities, which spares the palms and soles. The appearance of the rash is shown in the exhibit (see image below). Which of the following would most likely confirm the diagnosis in this patient?
A 7-year-old boy comes to the physician because of a generalized rash for 3 days. Over the past 5 days, he has also had a high fever and a sore throat. His 16-year-old sister was treated for infectious mononucleosis 2 weeks ago. He returned from a summer camp a week ago. His immunizations are up-to-date. Three years ago, he required intubation after an allergic reaction to dicloxacillin. The patient appears ill. His temperature is 38.2°C (100.8°F). Examination shows circumferential oral pallor. Cervical lymphadenopathy is present. There is tonsillar erythema and exudate. A confluent, blanching, punctate erythematous rash with a rough texture is spread over his trunk and extremities. His hemoglobin concentration is 13.3 g/dL, leukocyte count is 12,000/mm3, and erythrocyte sedimentation rate is 43 mm/h. Which of the following is the most appropriate next step in management?
Practice by Chapter
Common childhood exanthems
Practice Questions
Pediatric respiratory infections
Practice Questions
Pediatric gastrointestinal infections
Practice Questions
Urinary tract infections in children
Practice Questions
Bone and joint infections
Practice Questions
Central nervous system infections
Practice Questions
Pediatric tuberculosis
Practice Questions
Pediatric HIV
Practice Questions
Recurrent infections evaluation
Practice Questions
Fever of unknown origin approach
Practice Questions
Emerging infectious diseases in children
Practice Questions
Post-infectious immune complications
Practice Questions
Antimicrobial resistance in pediatrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
