Infectious Disease — MCQs

On this page
A 5-year-old boy is brought to his pediatrician's office by his parents for a scheduled visit. His father tells the physician that he has observed, on several occasions, that his son has difficulty breathing. This is more prominent when he is outside playing with his friends. These symptoms are increased during the spring and winter seasons, and, of late, the boy has one such episode almost every week. During these episodes, he usually wheezes, coughs, and seems to be winded as if something was restricting his ability to breathe. These symptoms have not affected his sleep at night. This breathlessness does not limit his daily activities, and whenever he does have an episode it subsides after he gets some rest. He does not have any other pertinent medical history and is not on any medication. His physical examination does not reveal any significant findings. The pediatrician checks his expiratory flow rate in the office and estimates it to be around 85% after conducting it three times. Which of the following drugs is the pediatrician most likely to start this patient on?
A 4-year-old boy presents with a dry cough. The patient’s mother states that the cough started a week ago and has not improved. She says the patient will have fits of forceful coughing that will last for minutes, followed by gasping as he catches his breath. Occasionally, the patient will vomit after one of these episodes. Past medical history is significant for a recent upper respiratory infection 4 weeks ago that has resolved. No current medications. Patient immunization status is incomplete because his mother believes they are harmful. Vitals are temperature 37.0°C (98.6°F), blood pressure 105/65 mm Hg, pulse 101/min, respiratory rate 27/min, and oxygen saturation 99% on room air. Cardiac exam is normal. Lungs are clear to auscultation. There are conjunctival hemorrhages present bilaterally. Which of the following correctly describes the stage of this patient’s most likely diagnosis?
A 24-year-old newly immigrated mother arrives to the clinic to discuss breastfeeding options for her newborn child. Her medical history is unclear as she has recently arrived from Sub-Saharan Africa. You tell her that unfortunately she will not be able to breastfeed until further testing is performed. Which of the following infections is an absolute contraindication to breastfeeding?
A 7-year-old boy presents to your office with facial eczema. He has a history of recurrent infections, including multiple episodes of pneumonia that lasted several weeks and otitis media. Laboratory measurements of serum immunoglobulins show increased IgE and IgA but decreased IgM. Which of the following additional abnormalities would you expect to observe in this patient?
A 7-year-old girl is brought to the physician by her father because of a dry cough, nasal congestion, and intermittent wheezing during the past 2 months. Since birth, she has had four upper respiratory tract infections that resolved without treatment and one episode of acute otitis media treated with antibiotics. She has a history of eczema. Her temperature is 37.1°C (98.7°F), and respirations are 28/min. Physical examination shows a shallow breathing pattern and scattered expiratory wheezing throughout both lung fields. Which of the following is the most appropriate next step in diagnosing this patient’s condition?
A 6-month-old infant is brought to the physician’s office by his parents due to a fever, cough, and shortness of breath. The cough is dry and has been progressively worsening for the past 48 hours along with the shortness of breath. His fever never exceeded 37.8°C (100.0°F) at home. The parents say that he has also had abundant nasal drainage and loss of appetite. He is irritable and vomited twice during this period. He has no relevant medical or family history. His vitals are the following: Pulse rate 165/min Respiratory rate 77/min Temperature 38.0°C (100.4°F) On physical examination, there is nasal congestion with thick secretions, accompanied by nasal flaring. On chest examination, intercostal retractions are seen and diffuse wheezing on both sides are heard on auscultation. What is the most likely cause?
A 7-year-old boy presents to the emergency department with several days of high fever accompanied by runny nose, cough, and red itchy eyes. Upon further history, you learn that the family is undocumented and has not had access to primary health services. Upon physical examination you see a red, slightly bumpy rash extending from the head to the mid-chest level. If you had examined this child prior to the development of the rash, which of the following signs may you have observed?
A 9-month-old infant is brought to the physician because of a generalized nonpruritic rash for 2 days. The rash began on her trunk and spread to her extremities. Five days ago, she was taken to the emergency department for fever of 40.5°C (104.9°F) and a 1-minute generalized tonic-clonic seizure. She was born at term and has no history of serious illness. Her immunizations are up-to-date. Current medications include acetaminophen. Her temperature is 37.2°C (99.0°F) and pulse is 120/min. Examination shows a maculopapular rash that blanches on pressure. A photograph of the rash is shown. Posterior auricular lymphadenopathy is present. Which of the following is the most likely diagnosis?
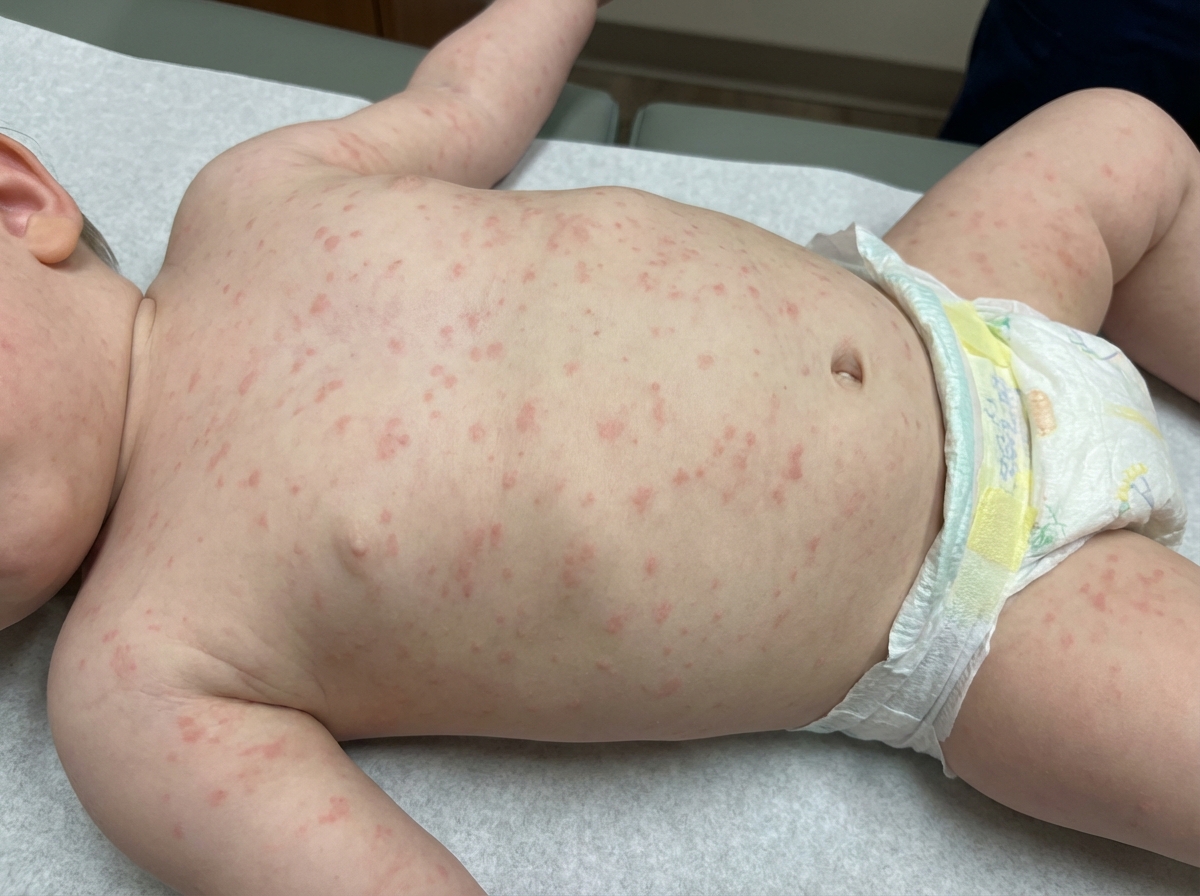
A 6-year-old girl is brought to the physician because of a generalized pruritic rash for 3 days. Her mother has noticed fluid oozing from some of the lesions. She was born at term and has been healthy except for an episode of bronchitis 4 months ago that was treated with azithromycin. There is no family history of serious illness. Her immunization records are unavailable. She attends elementary school but has missed the last 5 days. She appears healthy. Her temperature is 38°C (100.4°F). Examination shows a maculopapular rash with crusted lesions and vesicles over the entire integument, including the scalp. Her hemoglobin concentration is 13.1 g/dL, leukocyte count is 9800/mm3, and platelet count is 319,000/mm3. Which of the following is the most appropriate next best step?
A 3-month-old boy is brought to the emergency room by his mother for 2 days of difficulty breathing. He was born at 35 weeks gestation but has otherwise been healthy. She noticed a cough and some trouble breathing in the setting of a runny nose. His temperature is 100°F (37.8°C), blood pressure is 64/34 mmHg, pulse is 140/min, respirations are 39/min, and oxygen saturation is 93% on room air. Pulmonary exam is notable for expiratory wheezing and crackles throughout and intercostal retractions. Oral mucosa is noted to be dry. Which of the following is the most appropriate diagnostic test?
Practice by Chapter
Common childhood exanthems
Practice Questions
Pediatric respiratory infections
Practice Questions
Pediatric gastrointestinal infections
Practice Questions
Urinary tract infections in children
Practice Questions
Bone and joint infections
Practice Questions
Central nervous system infections
Practice Questions
Pediatric tuberculosis
Practice Questions
Pediatric HIV
Practice Questions
Recurrent infections evaluation
Practice Questions
Fever of unknown origin approach
Practice Questions
Emerging infectious diseases in children
Practice Questions
Post-infectious immune complications
Practice Questions
Antimicrobial resistance in pediatrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
