Infectious Disease — MCQs

On this page
A previously healthy 5-year-old boy is brought to the physician by his parents because of a 2-day history of poor balance and difficulty walking. He has fallen multiple times and is unable to walk up the stairs unassisted. He has also had difficulty tying his shoes and dressing himself. His family adheres to a vegetarian diet. He has not yet received any routine childhood vaccinations. His mother has a history of anxiety. He is at the 70th percentile for height and 30th percentile for weight. Vital signs are within normal limits. He is alert and oriented to person, place, and time. Physical examination shows a broad-based, staggering gait. He has difficulty touching his nose and cannot perform rapidly-alternating palm movements. Strength is 5/5 in the upper and lower extremities. Deep tendon reflexes are 1+ bilaterally. Skin examination shows several faint hyperpigmented macules on the chest. Which of the following is the most likely underlying cause of this patient's symptoms?
A 5-year-old girl is brought to the physician by her mother because of a 3-week history of a foul-smelling discharge from the left nostril. There was one episode of blood-tinged fluid draining from the nostril during this period. She has been mouth-breathing in her sleep for the past 4 days. She was born at term. Her 1-year-old brother was treated for viral gastroenteritis 3 weeks ago. She is at 60th percentile for height and at 70th percentile for weight. Her temperature is 37°C (98.6°F), pulse is 96/min, respirations are 23/min, and blood pressure is 96/54 mm Hg. Examination shows mucopurulent discharge in the left nasal cavity. Oral and otoscopic examination is unremarkable. Endoscopic examination of the nose confirms the diagnosis. Which of the following is the most appropriate next step in management?
A 4-year-old girl is brought to the physician because of a nonpruritic, painless rash that has been on her face for 5 days. She was born at term and has been healthy throughout childhood. Her 62-year-old maternal grandmother has bullous pemphigoid. Her development is adequate for her age and immunizations are up-to-date. She appears healthy and well-nourished. Her temperature is 37.0°C (98.6°F) pulse is 90/min, and respiratory rate is 18/min. Examination shows a crusted rash on the right side of the patient's face. An image of the patient's lower face is shown. The remainder of the examination shows no abnormalities. Which of the following is the most appropriate next step in management?
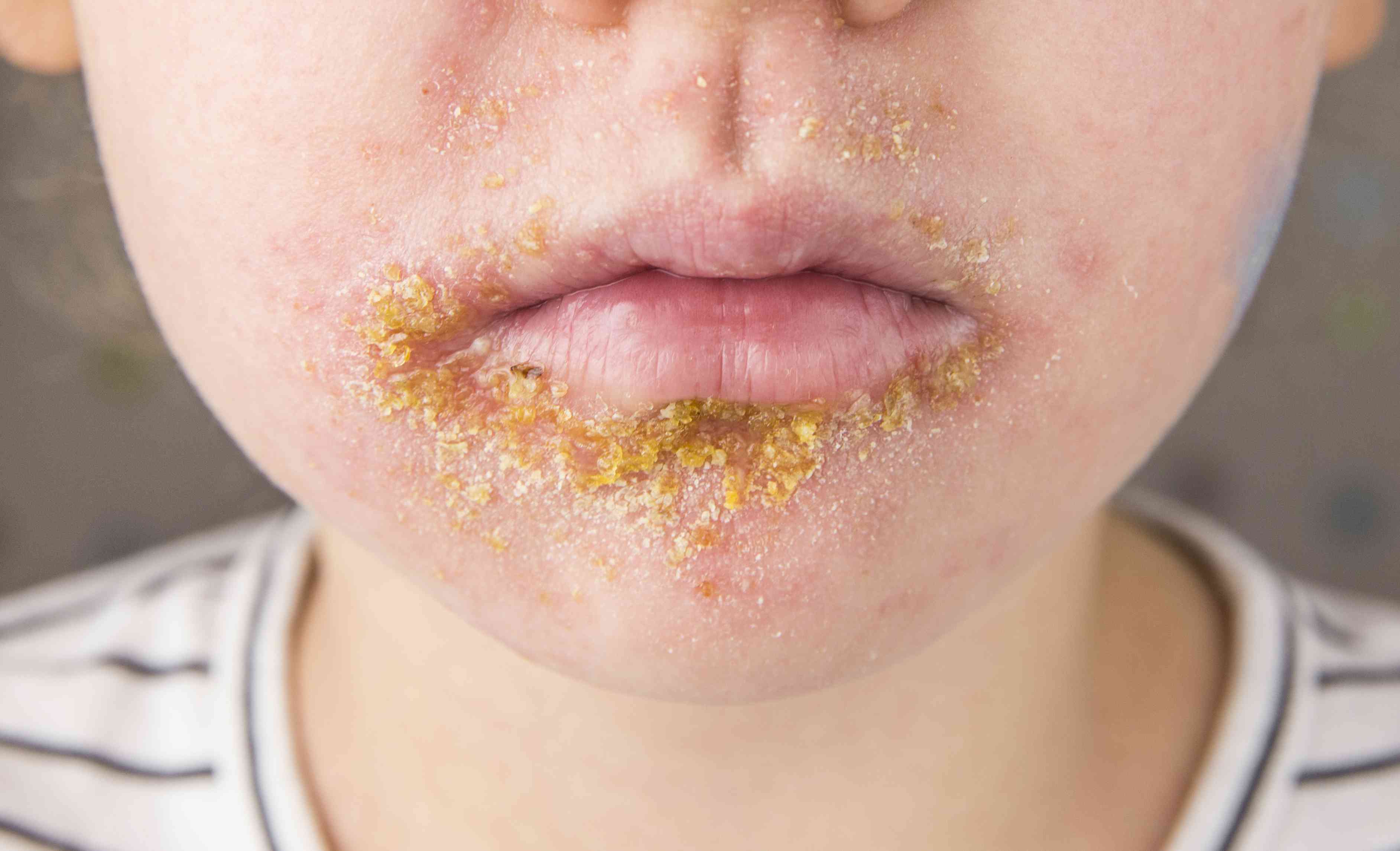
A 3-year-old boy is brought to the emergency department because of persistent fever and cough. Three days ago, he was diagnosed with pneumonia and acute otitis media. He was started on ampicillin-sulbactam and clarithromycin, but his symptoms did not improve. The mother reports that her son has been hospitalized 3 times due to pneumonia. He was first diagnosed with pneumonia at the age of 10 months. She also reports several episodes of bilateral otitis media and recurrent respiratory tract infections. His immunizations are up-to-date. He is at the 50th percentile for height and 20th percentile for weight. He appears fatigued. His temperature is 38°C (100.4°F). Pneumatic otoscopy shows purulent otorrhea bilaterally. Pulmonary examination shows decreased breath sounds over both lung fields. The palatine tonsils and adenoids are hypoplastic. Which of the following is the most likely underlying cause of this patient's condition?
A 16-year-old boy comes to the emergency department because of painful urination and urethral discharge for 3 days. He has multiple sexual partners and only occasionally uses condoms. His vital signs are within normal limits. The result of nucleic acid amplification testing for Neisseria gonorrhoeae is positive. The patient requests that his parents not be informed of the diagnosis. Which of the following initial actions by the physician is most appropriate?
An 8-month-old girl is brought to the emergency department because of fever, vomiting, and diarrhea for 3 days. Her parents report at least 10 watery stools daily. She has had three upper respiratory tract infections since she started daycare 2 months ago, but has otherwise been developing normally. Her mother has a history of celiac disease. The patient is at the 57th percentile for height and the 65th percentile for weight. Her immunizations are incomplete. Her temperature is 38.5°C (101.3°F), pulse is 145/min, and blood pressure is 92/54 mm Hg. Examination shows dry mucous membranes and decreased skin turgor. Bowel sounds are hyperactive. A complete blood count and serum concentrations of glucose, urea nitrogen, and creatinine are within the reference range; there is hypokalemia. In addition to intravenous fluid resuscitation, which of the following is the most appropriate next step in management?
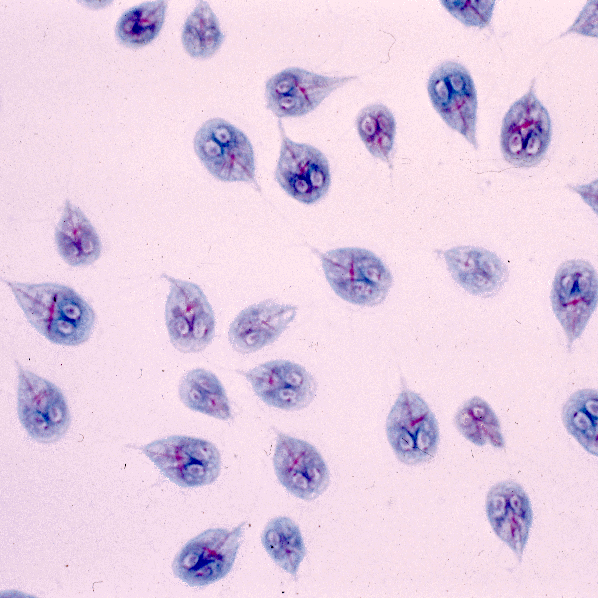
A 5-year-old boy is brought to the physician because of intermittent abdominal cramps and recurrent episodes of foul-smelling greasy diarrhea for 3 months. He has a history of recurrent upper respiratory infection. The abdomen is diffusely tender to palpation and resonant to percussion. A photomicrograph of a stool sample is shown. This patient is at increased risk for which of the following?
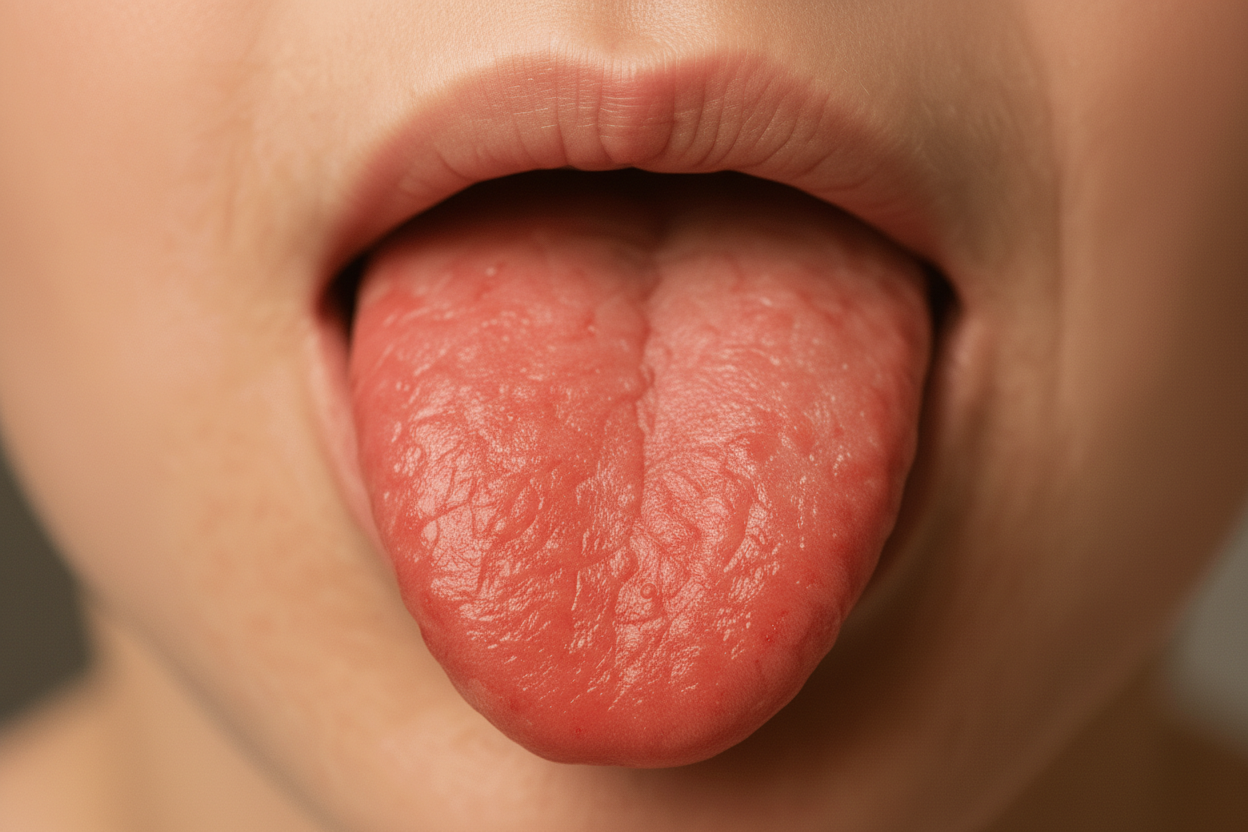
A 6-year-old girl is brought to a clinic with complaints of fever and sore throat for 2 days. This morning, she developed a rash on her face and neck which is progressing towards the trunk. The teachers in her school report that none of her classmates has similar symptoms. She has a normal birth history. On physical examination, the child looks healthy. The heart rate is 90/min, respiratory rate is 20/min, temperature is 39.0°C (102.2°F), and blood pressure is 90/50 mm Hg. An oropharyngeal examination reveals circumoral pallor with a red tongue, as shown in the photograph below. The chest and cardiac examinations are within normal limits. No hepatosplenomegaly is noted. What is the most likely diagnosis?
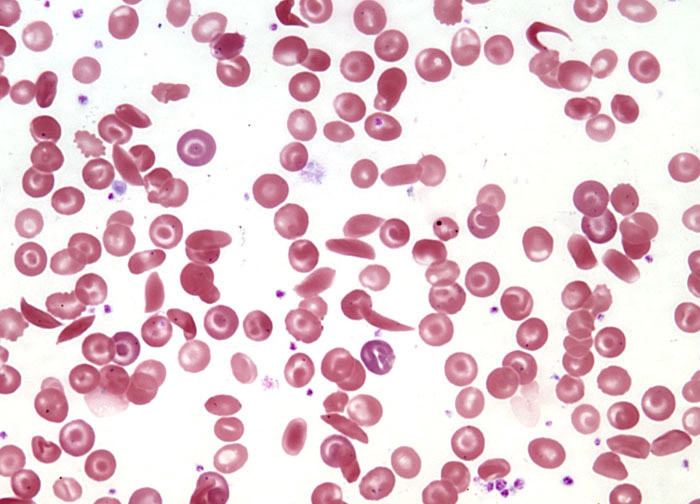
A 6-year-old right-handed boy is brought to the emergency department because of difficulty speaking and inability to raise his right arm. The patient’s mother says his symptoms started suddenly 1 hour ago and have not improved. She says he has never had these symptoms before. No other significant past medical history. The patient was born full-term via spontaneous transvaginal delivery and has met all developmental goals. The family immigrated from Nigeria 3 months ago, and the patient is currently following a vaccination catch-up schedule. His vital signs include: temperature 36.8°C (98.2°F), blood pressure 111/65 mm Hg, pulse 105/min. Height is at the 30th percentile and weight is at the 25th percentile for age and sex. Physical examination is remarkable for generalized pallor, pale conjunctiva, jaundice, and complete loss of strength in the right arm (0/5). His peripheral blood smear is shown in the picture. Which of the following is the most effective preventive measure for this patient’s condition?
A 14-year-old girl is brought to the physician because of a 1-week history of fever, malaise, and chest pain. She describes the pain as 6 out of 10 in intensity and that it is more severe if she takes a deep breath. The pain is centrally located in the chest and does not radiate. Three weeks ago, she had a sore throat that resolved without treatment. She has no personal history of serious illness. She appears ill. Her temperature is 38.7°C (101.7°F). Examination shows several subcutaneous nodules on the elbows and wrist bilaterally. Breath sounds are normal. A soft early systolic murmur is heard best at the apex in the left lateral position. Abdominal examination is unremarkable. Laboratory studies show: Hemoglobin 12.6 g/dL Leukocyte count 12,300/mm3 Platelet count 230,000/mm3 Erythrocyte sedimentation rate 40 mm/hr Serum Antistreptolysin O titer 327 U/mL (N < 200 U/mL) She is treated with aspirin and penicillin and her symptoms resolve. An echocardiography of the heart done 14 days later shows no abnormalities. Which of the following is the most appropriate next step in management?
Practice by Chapter
Common childhood exanthems
Practice Questions
Pediatric respiratory infections
Practice Questions
Pediatric gastrointestinal infections
Practice Questions
Urinary tract infections in children
Practice Questions
Bone and joint infections
Practice Questions
Central nervous system infections
Practice Questions
Pediatric tuberculosis
Practice Questions
Pediatric HIV
Practice Questions
Recurrent infections evaluation
Practice Questions
Fever of unknown origin approach
Practice Questions
Emerging infectious diseases in children
Practice Questions
Post-infectious immune complications
Practice Questions
Antimicrobial resistance in pediatrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
