Central nervous system infections — MCQs

A 6-year-old boy and his parents present to the emergency department with high-grade fever, headache, and projectile vomiting. The boy was born at 39 weeks gestation via spontaneous vaginal delivery. He is up to date on all vaccines and is meeting all developmental milestones. Past medical history is noncontributory. He has had no sick contacts at school or at home. The family has not traveled out of the area recently. He likes school and playing videogames with his younger brother. Today, his blood pressure is 115/76 mm Hg, heart rate is 110/min, respiratory rate is 22/min, and temperature is 38.4°C (101.2°F). On physical exam, the child is disoriented. Kernig’s sign is positive. A head CT was performed followed by a lumbar puncture. Several aliquots of CSF were distributed throughout the lab. Cytology showed high counts of polymorphs, biochemistry showed low glucose and elevated protein levels, and a gram smear shows gram-positive lanceolate-shaped cocci alone and in pairs. A smear is prepared on blood agar in an aerobic environment and grows mucoid colonies with clearly defined edges and alpha hemolysis. On later evaluation they develop a ‘draughtsman’ appearance. Which one of the following is the most likely pathogen?
A 7-year-old boy is brought to the emergency department because of high-grade fever and lethargy for 4 days. He has had a severe headache for 3 days and 2 episodes of non-bilious vomiting. He has sickle cell disease. His only medication is hydroxyurea. His mother has refused vaccinations and antibiotics in the past because of their possible side effects. He appears ill. His temperature is 40.1°C (104.2°F), pulse is 131/min, and blood pressure is 92/50 mm Hg. Examination shows nuchal rigidity. Kernig and Brudzinski signs are present. A lumbar puncture is performed. Analysis of the cerebrospinal fluid (CSF) shows a decreased glucose concentration, increased protein concentration, and numerous segmented neutrophils. A Gram stain of the CSF shows gram-negative coccobacilli. This patient is at greatest risk for which of the following complications?
A 65-year-old patient presents with rapidly progressive dementia, myoclonus, and ataxia over 3 months. Laboratory studies, including serum vitamin B12 (cyanocobalamin), thyroxine (T4), and thyroid-stimulating hormone concentrations, are within normal limits. A lumbar puncture is performed. Cerebrospinal fluid (CSF) analysis is most likely to show which of the following?
A 3-day-old boy is brought to the physician by his mother because of irritability and feeding intolerance for 1 day. His temperature is 39.2°C (102.6°F). Physical examination shows a bulging anterior fontanelle. A photomicrograph of a Gram stain of the cerebrospinal fluid is shown. Further evaluation shows that the organism expresses the K1 capsular polysaccharide. Which of the following is the most likely causal pathogen?
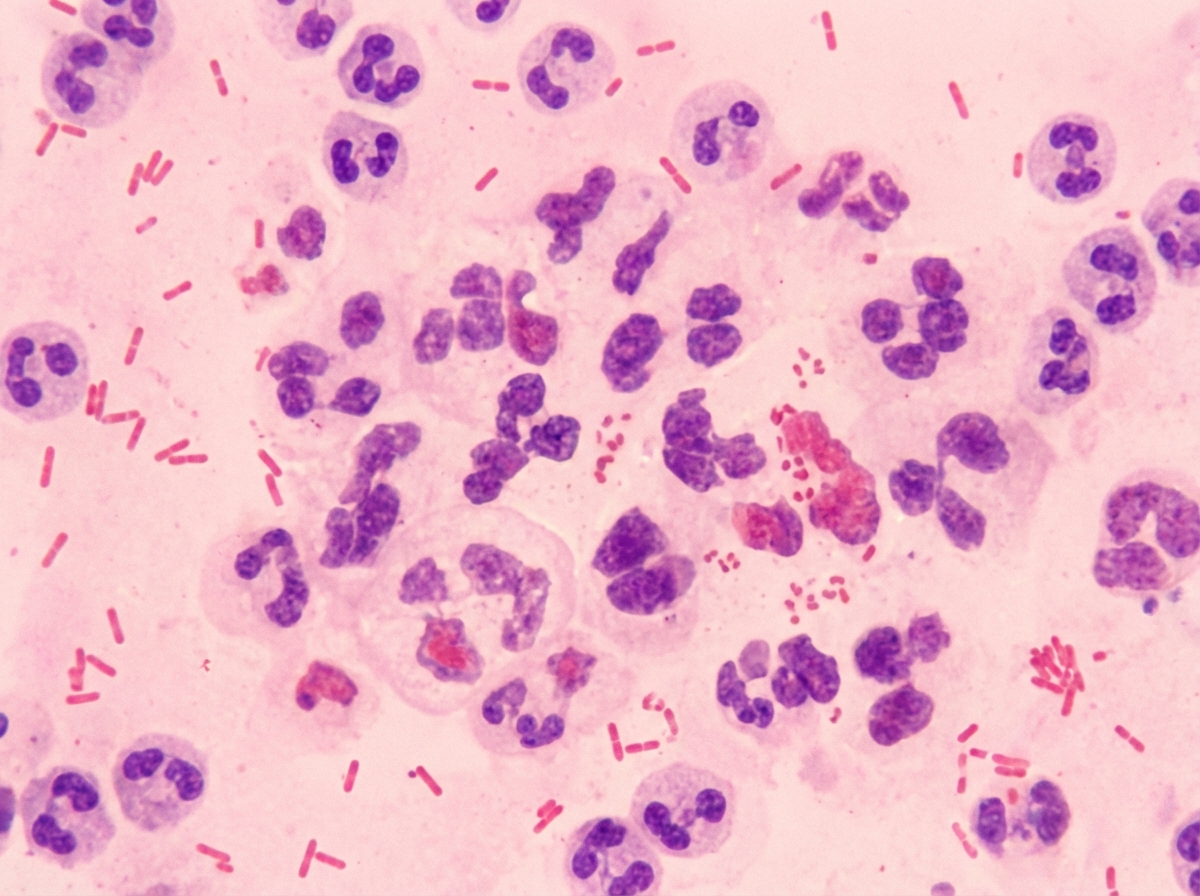
A 6-month old child is brought to the ER by parents for one day of fever, decreased feeding, and lethargy. They report that neither she nor her siblings are immunized due to their concerns about vaccinations. On exam, the infant is toxic-appearing. Antibiotics are started and lumbar puncture reveals bacterial meningitis caused by a gram-negative, encapsulated organism that requires chocolate agar and the two factors shown in Image A for growth. Which organism does this best describe?

A 9-year-old girl is admitted to the hospital with a one-day history of acute abdominal pain and vomiting. She also has a two-day history of fever, headache, and neck pain. Her immunizations are up-to-date. She is confused and oriented only to place and person. Her temperature is 39.7°C (103.5°F), pulse is 148/min, blood pressure is 90/50 mm Hg, and respiratory rate is 28/min. Cervical range of motion is limited by pain. The remainder of the neurologic examination shows no abnormalities. Laboratory studies show: Hemoglobin 10.9 g/dL Leukocyte count 44,000/mm3 Serum pH 7.33 Na+ 130 mEq/L Cl- 108 mEq/L K+ 6.1 mEq/L HCO3- 20 mEq/L Urea nitrogen 34 mg/dL Glucose 180 mg/dL Creatinine 2.4 mg/dL Urine ketones negative A CT scan of the head shows enhancement of the arachnoid and pia mater. Cerebrospinal fluid analysis shows a leukocyte count of 3,400/μL (90% neutrophils), a glucose concentration of 50 mg/dL, protein concentration of 81 mg/dL, and no erythrocytes. Gram stain of the CSF shows gram-negative diplococci. This patient is at increased risk for which of the following complications?
A 3-year-old girl is brought to the emergency room because of a 5-day history of high fever and fatigue. During this time she has been crying more than usual and eating less. Her mother says that the child has also complained about pain in her arms and legs for the past 3 days. She was born at term and has been otherwise healthy. She appears ill. Her temperature is 39.5°C (103.1°F), pulse is 128/min, and blood pressure is 96/52 mm Hg. The lungs are clear to auscultation. A grade 3/6 systolic murmur is heard at the apex. There is mild tenderness to palpation of the left upper quadrant with no guarding or rebound. The spleen is palpated 3 cm below the left costal margin. There is no redness or swelling of the joints. Laboratory studies show: Hemoglobin 11.8 g/dL Leukocyte count 16,300/mm3 Platelet count 220,000/mm3 Erythrocyte sedimentation rate 50 mm/h Serum Glucose 96 mg/dL Creatinine 1.7 mg/dL Total bilirubin 0.4 mg/dL AST 18 U/L ALT 20 U/L Urine Protein 2+ RBC casts rare RBC 10/hpf WBC 1–2/hpf Which of the following is the most appropriate next step in management?
A 32-year-old woman presents with a 3-month history of intermittent blurred vision and problems walking. The patient states that she often feels “pins and needles” in her legs that cause her problems when she’s walking. The patient is afebrile, and her vital signs are within normal limits. An autoimmune disorder is suspected. Which of the following findings would most likely be present in this patient?
A 21-year-old G3P2 woman presents to her obstetrician at 6 weeks gestation for routine prenatal care. Her past medical history includes obesity and gestational diabetes. She has had two spontaneous vaginal deliveries at term. One infant was macrosomic with hypoglycemia, but otherwise, she has had no complications. Her physician informs her that she must start taking a multivitamin with folic acid daily. The defect that folic acid supplementation protects against arises in tissue that is derived from which germ cell layer?
A 3-year-old boy is brought to the physician for the evaluation of recurrent skin lesions. The episodes of lesions started at the age of 3 months. He has also had several episodes of respiratory tract infections, enlarged lymph nodes, and recurrent fevers since birth. The boy attends daycare. The patient's immunizations are up-to-date. He is at the 5th percentile for length and 10th percentile for weight. He appears ill. Temperature is 38°C (100.4°F). Examination shows several raised, erythematous lesions of different sizes over the face, neck, groin, and extremities; some are purulent. Bilateral cervical and axillary lymphadenopathy are present. What is the most likely underlying mechanism of this patient's symptoms?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
