Bone and joint infections — MCQs

A 3-year-old patient is brought to the emergency department by her mother due to inability to walk. The child has been limping recently and as of this morning, has refused to walk. Any attempts to make the child walk or bear weight result in crying. She was recently treated for impetigo and currently takes a vitamin D supplement. Physical exam is remarkable for an anxious appearing toddler with knee swelling, erythema, and limited range of motion due to pain. Her mother denies any recent trauma to the child's affected knee. Temperature is 103°F (39.4°C), pulse is 132/min, blood pressure is 90/50 mmHg, respirations are 18/min, and oxygen saturation is 99% on room air. Which of the following is the best initial step in management?
A 22-year-old female with no past medical history presents to her primary care physician with a 3-day history of knee pain. She denies any recent injury or trauma. On physical examination her knee is warm, erythematous, and has diminished range of movement. The patient reports having multiple sexual partners over the last year and does not use protection regularly. Her blood pressure is 124/85 mmHg, heart rate is 76/min, and temperature is 38.3℃ (101.0℉). A joint aspiration is performed and a growth of gram-negative diplococci is noted on bacterial culture. What is the treatment of choice for this patient's condition?
A 42-year-old woman comes to the emergency department because of worsening severe pain, swelling, and stiffness in her right knee for the past 2 days. She recently started running 2 miles, 3 times a week in an attempt to lose weight. She has type 2 diabetes mellitus and osteoporosis. Her mother has rheumatoid arthritis. She drinks one to two glasses of wine daily. She is sexually active with multiple partners and uses condoms inconsistently. Current medications include metformin and alendronate. She is 161 cm (5 ft 3 in) tall and weighs 74 kg (163 lb); BMI is 29 kg/m2. Her temperature is 38.3°C (100.9°F), pulse is 74/min, and blood pressure is 115/76 mm Hg. She appears to be in discomfort and has trouble putting weight on the affected knee. Physical examination shows a 2-cm, painless ulcer on the plantar surface of the right toe. The right knee is swollen and tender to palpation. Arthrocentesis of the right knee with synovial fluid analysis shows a cell count of 55,000 WBC/μL with 77% polymorphonuclear (PMN) cells. Which of the following is the most likely underlying cause of this patient's presenting condition?
A 32-year-old man comes into your office because of pain in his right knee, left elbow, and left wrist. It started about a week ago but has particularly localized to his wrist. The patient states that he has 2 sexual partners. He states he has also had some white discharge from his penis with pruritis and pain during urination. His temperature is 97.6°F (36.4°C), blood pressure is 124/84 mmHg, pulse is 80/min, respirations are 12/min, and oxygen saturation is 98% on room air. Physical exam reveals pain upon palpation of the patient's left wrist which also appears erythematous and swollen. What is the best next step in management for this patient?
A 15-year-old boy presents to the emergency department for evaluation of an ‘infected leg’. The patient states that his right shin is red, swollen, hot, and very painful. The body temperature is 39.5°C (103.2°F). The patient states there is no history of trauma but states he has a history of poorly managed sickle cell anemia. A magnetic resonance imaging (MRI) scan is performed and confirms a diagnosis of osteomyelitis. Which of the following is the most likely causative agent?
A 7-year-old boy is brought to the emergency department because of a 3-day history of generalized fatigue, myalgia, and fever. He has sickle cell disease. His current medications include hydroxyurea and folic acid. He appears ill. His temperature is 39.2°C (102.6°F), pulse is 103/min, and respirations are 28/min. Examination shows pale conjunctivae. The lungs are clear to auscultation. The abdomen is soft and nontender. Neurologic examination shows no focal findings, His hemoglobin concentration is 10.3 g/dL and leukocyte count is 14,100/mm3. Intravenous fluid is administered and blood cultures are obtained. Which of the following is the most appropriate next step in treatment?
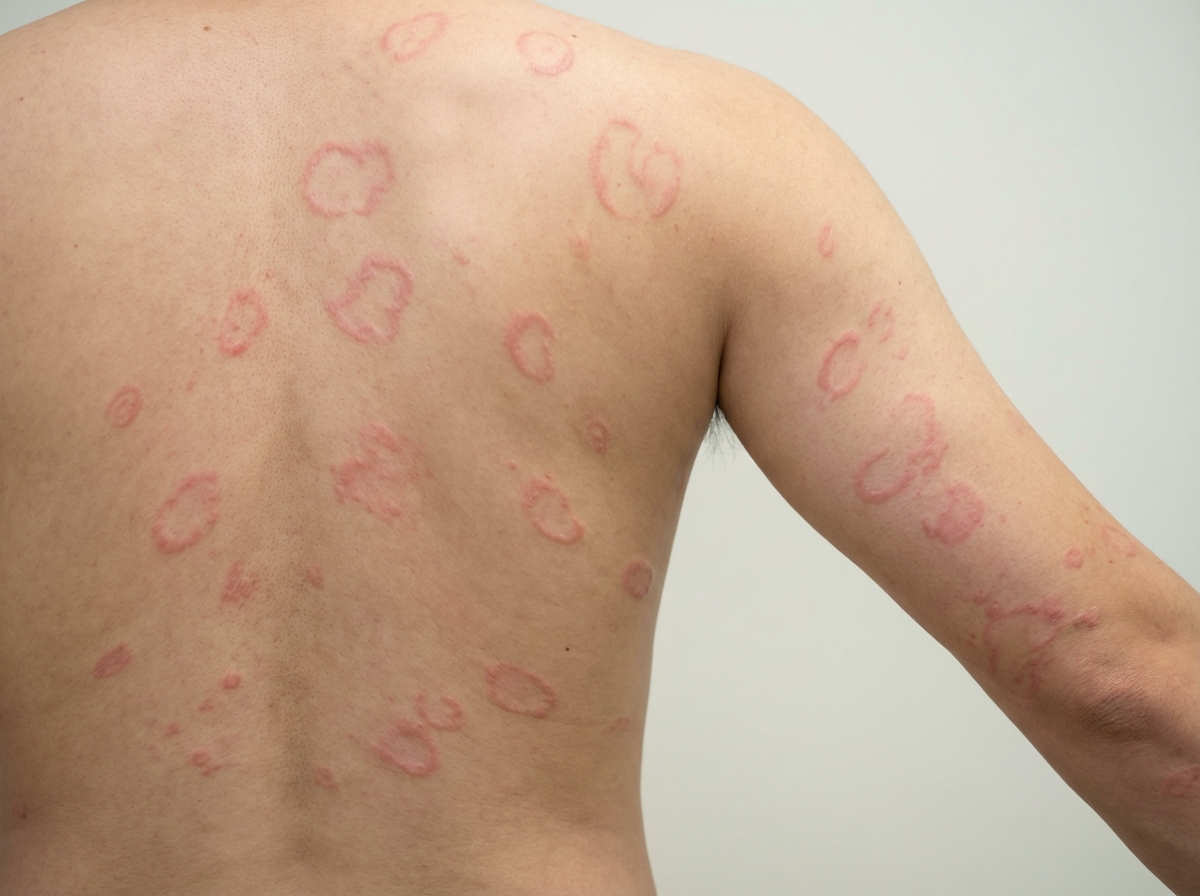
An 11-year-old boy presents with fever and joint pain for the last 3 days. His mother says that he had a sore throat 3 weeks ago but did not seek medical care at that time. The family immigrated from the Middle East 3 years ago. The patient has no past medical history. The current illness started with a fever and a swollen right knee that was very painful. The following day, his knee improved but his left elbow became swollen and painful. While in the waiting room, his left knee is also becoming swollen and painful. Vital signs include: temperature 38.7°C (101.6°F), and blood pressure 110/80 mm Hg. On physical examination, the affected joints are swollen and very tender to touch, and there are circular areas of redness on his back and left forearm (as shown in the image). Which of the following is needed to establish a diagnosis of acute rheumatic fever in this patient?
An 11-year-old boy presents to the emergency department with sudden pain. The patient's parents state the child suddenly felt pain in his hands an hour ago. He has not eaten anything new lately. He did play football earlier this morning and admits to being tackled forcefully multiple times. The child is doing well in school and is proud that he has a new girlfriend. The child has a past medical history of obesity and is not currently on any medications. His temperature is 100°F (37.8°C), blood pressure is 120/68 mmHg, pulse is 100/min, respirations are 11/min, and oxygen saturation is 98% on room air. Cardiopulmonary exam is within normal limits. On physical exam of the patient's extremities, there was painful and symmetrical swelling of his hands and feet but no rashes were present. The patient is started on analgesics. Which of the following is the most likely cause of this patient's presentation?
An 8-year-old boy presents to his pediatrician accompanied by his father with a complaint of chronic cough. For the past 2 months he has been coughing up yellow, foul-smelling sputum. He has been treated at a local urgent care center for multiple episodes of otitis media, sinusitis, and bronchitis since 2 years of age. His family history is unremarkable. At the pediatrician's office, his temperature is 99.2°F (37.3°C), blood pressure is 110/84 mmHg, pulse is 95/min, and respirations are 20/min. Inspection shows a young boy who coughs occasionally during examination. Pulmonary exam demonstrates diffuse wheezing and crackles bilaterally. Mild clubbing is present on the fingers. The father has brought an electrocardiogram (ECG) from the patient’s last urgent care visit that shows pronounced right axis deviation. Which of the following is the most likely etiology of this patient’s condition?
A 3-year-old girl is brought to the emergency room because of a 5-day history of high fever and fatigue. During this time she has been crying more than usual and eating less. Her mother says that the child has also complained about pain in her arms and legs for the past 3 days. She was born at term and has been otherwise healthy. She appears ill. Her temperature is 39.5°C (103.1°F), pulse is 128/min, and blood pressure is 96/52 mm Hg. The lungs are clear to auscultation. A grade 3/6 systolic murmur is heard at the apex. There is mild tenderness to palpation of the left upper quadrant with no guarding or rebound. The spleen is palpated 3 cm below the left costal margin. There is no redness or swelling of the joints. Laboratory studies show: Hemoglobin 11.8 g/dL Leukocyte count 16,300/mm3 Platelet count 220,000/mm3 Erythrocyte sedimentation rate 50 mm/h Serum Glucose 96 mg/dL Creatinine 1.7 mg/dL Total bilirubin 0.4 mg/dL AST 18 U/L ALT 20 U/L Urine Protein 2+ RBC casts rare RBC 10/hpf WBC 1–2/hpf Which of the following is the most appropriate next step in management?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
