Down syndrome — MCQs

A 32-year-old woman, gravida 2, para 1, at 14-weeks' gestation comes to the physician for a prenatal visit. Routine first trimester screening shows increased nuchal translucency, decreased β-hCG concentration, and decreased levels of pregnancy-associated plasma protein A. Amniocentesis shows trisomy of chromosome 13. This fetus is at increased risk for which of the following?
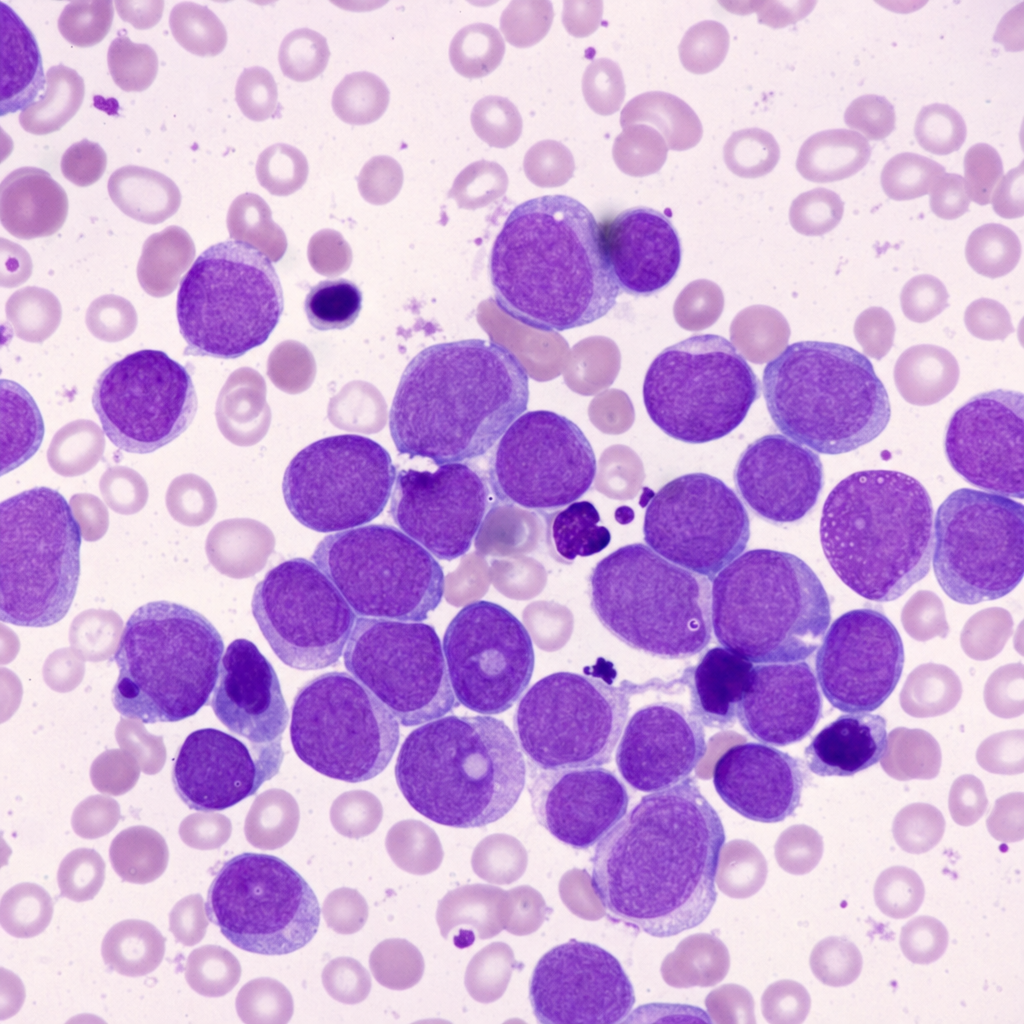
A 2-month-old baby boy and his mother present to his pediatrician for vaccination as per the immunization schedule. His mother denies any active complaints but mentions that he has not smiled yet. The boy was born at 39 weeks gestation via spontaneous vaginal delivery. His mother received minimal prenatal care. On physical examination, his vitals are stable, but a general examination shows the presence of generalized hypotonia. His face is characterized by upwardly slanting palpebral fissures, small dysplastic ears, and a flat face. His little fingers are short, with clinodactyly, and both palms have single palmar creases. The results of a karyotype are shown in the image. If this infant has also inherited a mutation in the GATA1 gene, for which of the following conditions is he most likely to be at increased risk?
A 37-year-old woman presents for prenatal counseling at 18 weeks gestation. The patient tells you that her sister recently had a child with Down's syndrome, and the patient would like prenatal screening for Down's in her current pregnancy. Which of the following prenatal screening tests and results would raise concern for Down's syndrome?
A 23-year-old pregnant woman (gravida 1, para 0) presents during her 16th week of pregnancy for a check-up. The course of her current pregnancy is unremarkable. She had normal results on the previous ultrasound examination. Her human chorionic gonadotropin (hCG) level measured at week 12 of pregnancy was 0.9 multiples of the normal median (MoM). She is human immunodeficiency virus (HIV), hepatitis B virus (HBV), and hepatitis C virus (HCV)-negative. She undergoes a quadruple test which shows the following results: Serum alpha-fetoprotein Low Unconjugated estriol Low Beta-hCG High Inhibin A High The risk of which condition indicates these results?
A 19-year-old male from rural West Virginia presents to his family medicine doctor to discuss why he is having trouble getting his wife pregnant. On exam, he is 6 feet 2 inches with a frail frame and broad hips for a male his size. He is noted to have mild gynecomastia, no facial hair, and small, underdeveloped testes. He claims that although he has a lower libido than most of his friends, he does have unprotected sex with his wife. His past medical history is notable for developmental delay and difficulties in school. What is the most likely chromosomal abnormality in this patient?
A 38-year-old woman, gravida 3, para 2, at 12 weeks' gestation comes to her obstetrician for a prenatal visit. Screening tests in the first trimester showed a decreased level of pregnancy-associated plasma protein and an increased level of β-hCG. A genetic disorder is suspected. Which of the following results from an additional diagnostic test is most likely to confirm the diagnosis?
A 28-year-old G2P1 female is concerned that she may give birth to another child with Down syndrome. She states that she may not be able to take care of another child with this disorder. Which of the following tests can confirm the diagnosis of Down syndrome in utero?
A 2300-g (5.07-lb) male newborn is delivered at term to a 39-year-old woman. Examination shows a sloping forehead, a flat nasal bridge, increased interocular distance, low-set ears, a protruding tongue, a single palmar crease and an increased gap between the first and second toe. There are small white and brown spots in the periphery of both irises. The abdomen is distended. An x-ray of the abdomen shows two large air-filled spaces in the upper quadrant. This patient's condition is most likely associated with which of the following cardiac anomalies?
A 2-year-old boy is brought to a pediatrician because his parents have noticed that he seems to be getting tired very easily at home. Specifically, they have noticed that he is often panting for breath after walking around the house for a few minutes and that he needs to take naps fairly often throughout the day. He has otherwise been well, and his parents do not recall any recent infections. He was born at home, and his mom did not receive any prenatal care prior to birth. Physical exam reveals a high-pitched, harsh, holosystolic murmur that is best heard at the lower left sternal border. No cyanosis is observed. Which of the following oxygen tension profiles would most likely be seen in this patient? (LV = left ventricle, RV = right ventricle, and SC = systemic circulation).
A 1-day-old infant in the general care nursery, born at full term by uncomplicated cesarean section delivery, is noted to have a murmur, but otherwise appears well. On examination, respiratory rate is 40/min and pulse oximetry is 96%. Precordium is normoactive. With auscultation, S1 is normal, S2 is single, and a 2/6 systolic ejection murmur is heard at the left upper sternal border. Echocardiography shows infundibular pulmonary stenosis, overriding aorta, ventricular septal defect and concentric right ventricular hypertrophy. Which of the following correlate with the presence or absence of cyanosis in this baby?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
