Congenital defects — MCQs

On this page
A 2-month-old infant boy is brought into the clinic for a well-child check. Mom reports a healthy pregnancy with no complications. Though she said the ultrasound technician saw “some white deposits in his brain” during a prenatal check, mom was not concerned. The baby was delivered at 38 weeks of gestation during a home birth. When asked if there were any problems with the birthing process, mom denied any difficulties except that “he was small and had these blue dots all over.” Physical exam was unremarkable except for the absence of object tracking. What other finding would you expect?
A 4-year-old girl is being followed by the pediatric oncology team after her pediatrician found a palpable abdominal mass towards the right flank 2 weeks ago. Abdominal ultrasonography detected a solid mass in the right kidney without infiltration of the renal vein and inferior vena cava. The contrast-enhanced computed tomography (CT) confirmed the presence of a solitary mass in the right kidney surrounded by a pseudocapsule consisting of a rim of normal tissue, displacing it medially, and distorting the collecting system. No nodal involvement was detected. In which of the following chromosomes would you expect a genetic abnormality?
A 3175-g (7-lb) female newborn is delivered at term. Initial examination shows a distended abdomen and a flat perineal region without an opening. A dark green discharge is coming out of the vulva. Which of the following is the most likely diagnosis?
A 7-year-old Caucasian girl with asthma presents to her pediatrician with recurrent sinusitis. The patient’s mother states that her asthma seems to be getting worse and notes that ‘lung problems run in the family’. The patient has had 2 episodes of pneumonia in the last year and continues to frequently have a cough. Her mother says that 1 of her nieces was recently diagnosed with cystic fibrosis. On physical examination, the child has clubbing of the nail beds on both hands. A chloride sweat test is performed on the patient, and the child’s sweat chloride concentration is found to be within normal limits. The physician is still suspicious for cystic fibrosis and believes the prior asthma diagnosis is incorrect. Which of the following diagnostic tests would aid in confirming this physician’s suspicions?
A 7-year-old boy is being evaluated in pediatric cardiology clinic. He appears grossly normal, but suddenly becomes tachypneic and cyanotic when his mom takes a toy away from him. These symptoms resolve somewhat when he drops into a squatting position. Transthoracic echocardiography reveals pulmonic stenosis, a ventricular septal defect, right ventricular hypertrophy, and an overriding aorta. Which of the following best predicts the degree of cyanosis and other hypoxemic symptoms in this patient?
A 3400-g (7-lb 8-oz) female newborn is delivered at term to a 28-year-old primigravid woman. Apgar scores are 7 and 8 at 1 and 5 minutes, respectively. Vital signs are within normal limits. Examination shows swelling of bilateral upper and lower extremities and low-set ears. The posterior hair line is low and the chest appears broad. There are skin folds running down the sides of the neck to the shoulders. A grade 2/6 systolic ejection murmur and systolic click is heard at the apex. Which of the following is the most likely cause of this patient's swelling?
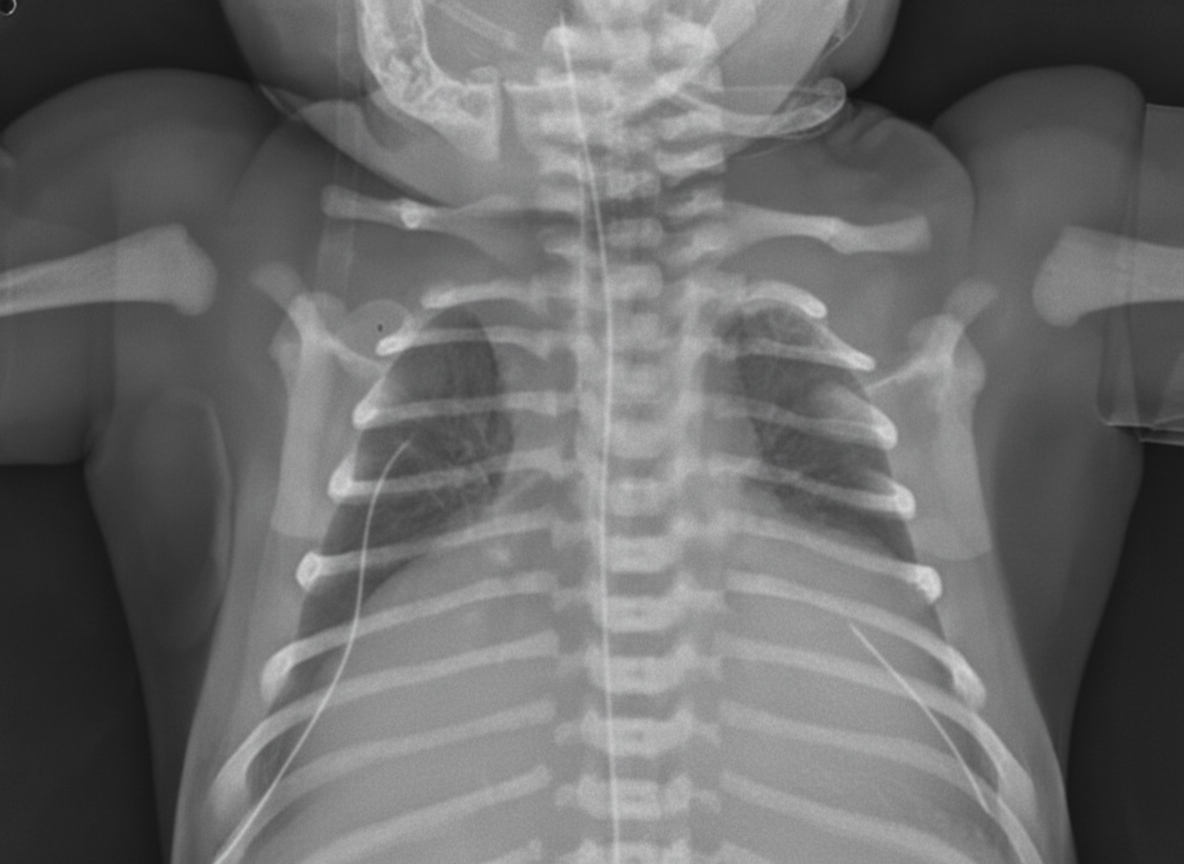
A 2-hours-old neonate is found to have bluish discoloration throughout his body, including lips and tongue. The boy was born at 39 weeks gestation via spontaneous vaginal delivery with no prenatal care. Maternal history is positive for type 2 diabetes mellitus for 11 years. On physical examination, his blood pressure is 55/33 mm Hg, his heart rate is 150/min, respiratory rate is 45/min, temperature of 37°C (98.6°F), and oxygen saturation is 84% on room air. Appropriate measures are taken. Auscultation of the chest reveals a single second heart sound without murmurs. Chest X-ray is shown in the exhibit. Which of the following is the most likely diagnosis?
A 2-year-old boy is brought in to the pediatrician by his mother because she is concerned that he is not gaining weight. She reports that the patient has a good appetite, eats a varied diet of solid foods, and drinks 2 cups of milk a day. The patient's mother also reports that he has foul-smelling stools over 6 times a day. The patient has a history of recurrent bronchiectasis and chronic sinusitis. On physical examination, multiple nasal polyps are appreciated and scattered rhonchi are heard over both lung fields. The patient is below the 25th percentile in height and weight. Genetic testing is ordered to confirm the suspected diagnosis. Which of the following is the most common complication associated with the patient's most likely diagnosis?
A 6-year-old boy is brought to the physician by his mother who is concerned about his early sexual development. He has no history of serious illness and takes no medications. He is at the 99th percentile for height and 70th percentile for weight. His blood pressure is 115/78 mm Hg. Examination shows greasy facial skin and cystic acne on his forehead and back. There is coarse axillary and pubic hair. Serum studies show: Cortisol (0800 h) 4 μg/dL Deoxycorticosterone 2.5 ng/dL (N = 3.5–11.5) Dehydroepiandrosterone sulfate 468 mcg/dL (N = 29–412) Which of the following is the most likely underlying cause of this patient's symptoms?
An 8-year-old girl is brought to the physician because of a progressive swelling of her neck for the past 6 months. She has no pain, dyspnea, or dysphagia. She is at the 60th percentile for height and the 55th percentile for weight. Vital signs are within normal limits. Examination shows a 3-cm cystic, nontender swelling in the midline of the neck. The swelling moves upwards on protrusion of the tongue. There is no cervical lymphadenopathy. Her serum thyroid-stimulating hormone level is 2.1 μU/mL. Which of the following is the most appropriate next step in management?
Practice by Chapter
Neural tube defects
Practice Questions
Congenital heart defects
Practice Questions
Gastrointestinal malformations
Practice Questions
Genitourinary anomalies
Practice Questions
Craniofacial anomalies
Practice Questions
Skeletal dysplasias
Practice Questions
Chromosomal disorders
Practice Questions
Teratogenic exposures
Practice Questions
Multiple malformation syndromes
Practice Questions
Prenatal diagnosis of congenital defects
Practice Questions
Surgical management timing
Practice Questions
Long-term outcomes and follow-up
Practice Questions
Preventive strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
