Congenital defects — MCQs

On this page
An 18-month-old boy is brought to the physician for a well-child examination. His mother is concerned because he is unable to walk on his own. He has been increasingly irritable over the past month, has been feeding poorly, and has had multiple episodes of vomiting. His immunizations are up-to-date. He is at the 50th percentile for height, 40th percentile for weight, and 98th percentile for head circumference. He appears lethargic. His vital signs are within normal limits. Examination shows a bulging anterior fontanelle. The child is unable to stand without support and falls if he attempts to walk. Muscle tone is increased and deep tendon reflexes are 4+ in the lower extremities. Examination of the back is unremarkable. An MRI of the brain shows symmetrical enlargement of all four ventricles. Which of the following is the most appropriate treatment in this patient?
A newborn infant is resuscitated and transferred to the neonatal intensive care unit. The infant has notable limb deformities as well as low-set ears and a flattened nose. He was born at 34 weeks gestation to a healthy mother who received regular obstetric follow-up. Resuscitation was notable for difficulty maintaining oxygenation in the newborn. Despite appropriate interventions, the infant is still struggling to maintain adequate oxygenation. Which of the following is most likely the cause of this patient's symptoms?
A 6-month-old male presents with a painless, enlarged left scrotum. After examining the patient, you suspect this enlargement is secondary to serous fluid entering and accumulating in the scrotum through a patent processus vaginalis. Which of the following would be the most useful next step in confirming the diagnosis of this patient’s condition?
A 5-year-old boy is brought to his neurologist for continued treatment of muscle spasms. His past medical history is significant for a brain abnormality that was detected neonatally when it presented with an enlarged posterior fossa as well as a malformed cerebellar vermis. Since birth, he has had developmental delay, high muscle tone, difficulty with coordination, and speech delay. He has been treated with a number of therapies to relax his muscle tone such as baclofen. Which of the following conditions is associated with this patient's most likely condition?
A 2-month-old boy is brought to the emergency department by his mother because of an 8-hour history of difficulty feeding and decreased arousability. His mother says that the symptoms began after he rolled over and fell from the bed. His vital signs are within normal limits. Examination shows tense fontanelles. Fundoscopy shows bilateral optic disc swelling with dot-and-blot hemorrhages extending to the ora serrata. Which of the following is the most likely diagnosis?
A 4-year-old girl is brought to the pediatrician by her parents for a 1-year history of gradual loss of speech and motor skills. Pregnancy and delivery were uncomplicated, and development was normal until the age of 3 years. Her parents say she used to run and speak in short sentences but now is only able to walk slowly and cannot form sentences. She avoids eye contact and constantly rubs her hands together. There are no dysmorphic facial features. Neurologic examination shows marked cognitive and communicative delay. She has a broad-based gait and is unable to hold or pick up toys on her own. Which of the following mutations is the most likely underlying cause of this patient's condition?
A 4-year-old-female presents with a flattened, reddish 2 cm lump located at the base of the tongue. The patient's mother reports her having trouble swallowing, often leading to feeding difficulties. The mother also reports lethargy, constipation, dry skin, and hypothermia. Which of the following is the most appropriate management of this patient’s presentation?
A 2720-g (6-lb) female newborn is delivered at term to a 39-year-old woman, gravida 3, para 2. Examination in the delivery room shows micrognathia, prominent occiput with flattened nasal bridge, and pointy low-set ears. The eyes are upward slanting with small palpebral fissures. The fists are clenched with fingers tightly flexed. The index finger overlaps the third finger and the fifth finger overlaps the fourth. A 3/6 holosystolic murmur is heard at the lower left sternal border. The nipples are widely spaced and the feet have prominent heels and convex, rounded soles. Which of the following is the most likely cause of these findings?
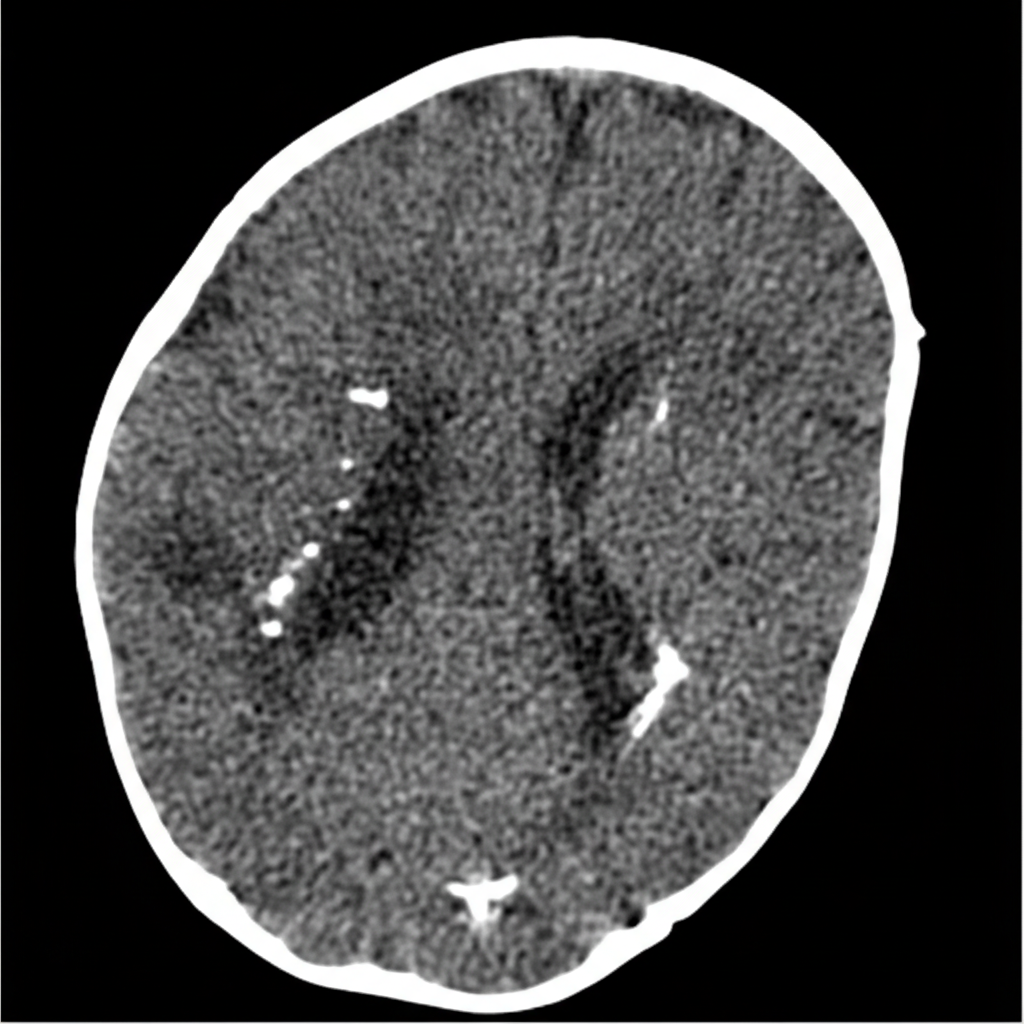
A 2-day-old boy, born at 38-weeks gestation, presents with jaundice and microcephaly. Social history reveals his mother is an animal caretaker. The vital signs include: temperature 37.0°C (98.6°F), blood pressure 75/40 mm Hg, pulse 150/min, respiratory rate 40/min, and oxygen saturation 99% on room air. Physical examination reveals hepatosplenomegaly. A CT and MRI of the head are significant for the following findings (see picture). Which of the following diseases contracted during pregnancy is the most likely cause of this patient's condition?
A 3000-g (6-lb 10-oz) male newborn delivered at 38 weeks' gestation develops respiratory distress shortly after birth. Physical examination shows low-set ears, retrognathia, and club feet. Within a few hours, the newborn dies. Examination of the liver at autopsy shows periportal fibrosis. Which of the following is the most likely underlying cause of the neonate's presentation?
Practice by Chapter
Neural tube defects
Practice Questions
Congenital heart defects
Practice Questions
Gastrointestinal malformations
Practice Questions
Genitourinary anomalies
Practice Questions
Craniofacial anomalies
Practice Questions
Skeletal dysplasias
Practice Questions
Chromosomal disorders
Practice Questions
Teratogenic exposures
Practice Questions
Multiple malformation syndromes
Practice Questions
Prenatal diagnosis of congenital defects
Practice Questions
Surgical management timing
Practice Questions
Long-term outcomes and follow-up
Practice Questions
Preventive strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
