Congenital defects — MCQs

On this page
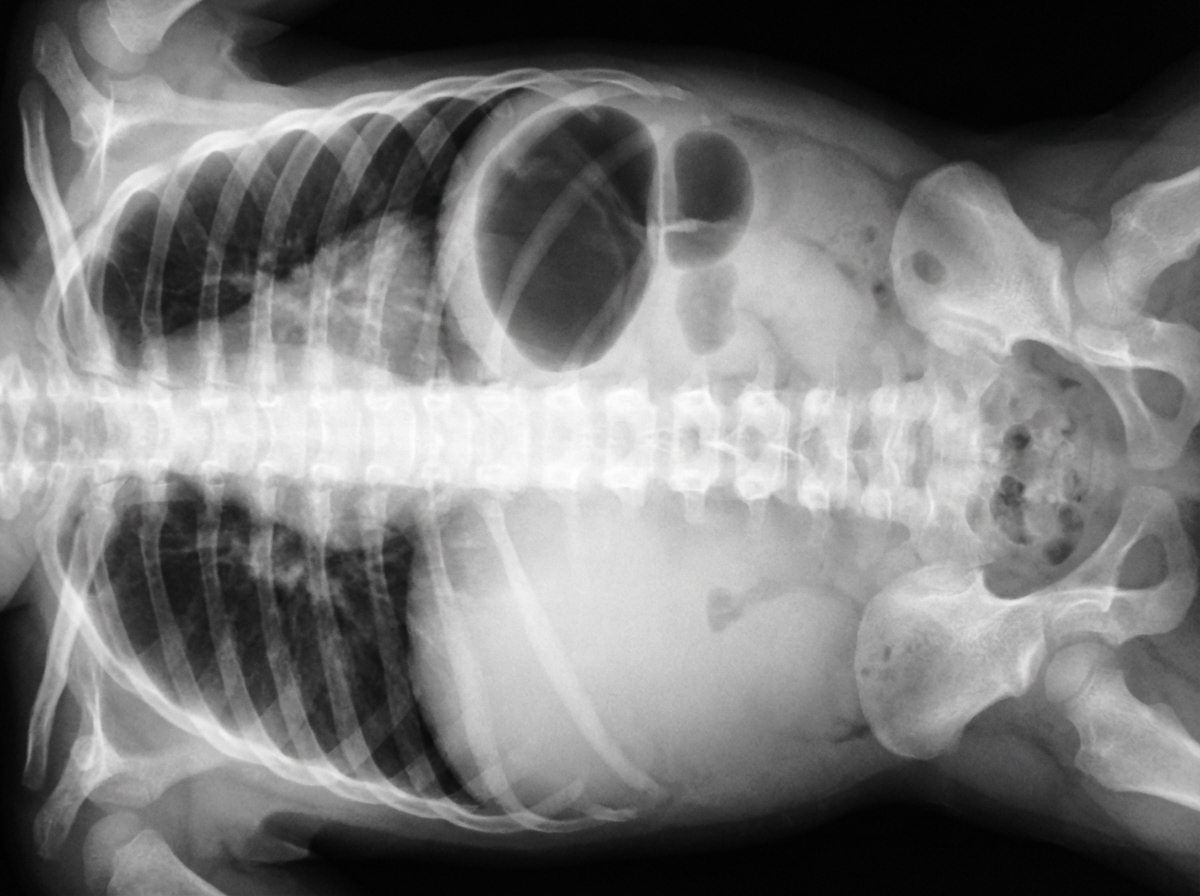
A female newborn delivered at 38 weeks’ gestation is evaluated for abdominal distention and bilious vomiting 24 hours after delivery. The pregnancy and delivery were uncomplicated. She appears lethargic and her fontanelles are sunken. An x-ray of the abdomen is shown. This infant most likely has a congenital obstruction affecting which of the following anatomic structures?
A 16-year-old boy is brought to the physician by his parents because of a 6-month history of progressive fatigue and worsening shortness of breath on exertion. The parents report that the boy “has always been tired out a bit more easily than other kids.” The family recently immigrated to the United States from rural South Korea. Pulse oximetry on room air shows an oxygen saturation of 96% on bilateral index fingers. Radial pulses are bounding. There is mild bluish discoloration and bulbous enlargement of the distal toes bilaterally. Echocardiography is most likely to show which of the following?
A 2-year-old boy is brought to the physician because of progressive difficulty breathing and a productive cough for the past 2 days. During the past 6 months, he has had recurrent episodes of pneumonia treated with antibiotics. He has not gained weight in this time period. His temperature is 38.5°C (101.3°F), pulse is 130/min, respirations are 18/min, and blood pressure is 100/60 mm Hg. Auscultation of the lungs shows decreased breath sounds over the right lung fields. Ocular examination shows periorbital subcutaneous bleeding and bulging of both eyes. His leukocyte count is 16,000/mm3. An x-ray of the chest shows a right-sided opacity and a collapsed right lung. An MRI of the chest shows a heterogeneous mass in the posterior mediastinum that compresses the heart and the great vessels to the left side. Further evaluation is most likely to show which of the following?
A 9-month-old infant is brought to the pediatrician for immunizations and assessment. His parents report that he is eating well and produces several wet diapers every day. He is a happy and curious child. The boy was born at 39 weeks gestation via spontaneous vaginal delivery. He is up to date on all vaccines and is meeting all developmental milestones. The infant's vital signs are normal. Physical growth is appropriate for his age. The physician notes a loud holosystolic murmur at the left sternal border (grade IV) and orders an echocardiogram which confirms the diagnosis of congenital heart defect. Based on echocardiogram findings, the pediatrician reassures the parents that the infant will be monitored, but most likely will not require surgical intervention. Which of the following is the most likely diagnosis?
A 7-year-old child with a history of abdominal and thigh pain that runs in his family is brought into the emergency room by his mother. His mother states they have a "blood disease." She also states the child was coughing and had fever to 101.1 F over the last three days and has been suddenly feeling much worse. On exam, the vitals are HR 110, BP 100/60, RR 20, T 101.5 F. CBC is significant for Hgb 3.2, WBC 2.1, Hct 10, Plts 30000. The reticulocyte count is 1% and the MCV is 81. Bone marrow biopsy shows hypocellular marrow with fatty tissue. What is the most likely diagnosis?
A 3-year-old boy is brought to the physician for a follow-up examination. He has suffered from seizures since the age of 8 months. His mother has noticed he often has unprovoked bouts of laughter and loves playing with water. She describes him as having a happy, excitable demeanor. He can stand without support but cannot walk. His responses are rarely verbal, and when they are, he uses single words only. His only medication is sodium valproate. He is at the 2nd percentile for head circumference, 30th percentile for height, and 60th percentile for weight. Examination shows a wide-based stance and mandibular prognathism. Tongue thrusting and difficulty standing is present. Muscle tone is increased in all extremities. Deep tendon reflexes are 4+ bilaterally. Which of the following is the mechanism most likely to explain these findings?
A 5-month-old boy is brought to the emergency department by his mother because his lips turned blue for several minutes while playing earlier that evening. She reports that he has had similar episodes during feeding that resolved quickly. He was born at term following an uncomplicated pregnancy and delivery. He is at the 25th percentile for length and below the 5th percentile for weight. His temperature is 37°C (98.6°F), pulse is 130/min, blood pressure is 83/55 mm Hg, and respirations are 42/min. Pulse oximetry on room air shows an oxygen saturation of 90%. During the examination, he sits calmly in his mother's lap. He appears well. The patient begins to cry when examination of his throat is attempted; his lips and fingers begin to turn blue. Further evaluation of this patient is most likely to show which of the following?
A 4-week-old newborn is brought to the physician for a well-child examination. He was born at 40 weeks' gestation and weighed 3300 g (7 lb 4 oz). He now weighs 4300 g (9 lbs 1 oz). There is no family history of serious illness. He is at the 50th percentile for height and 50th percentile for weight. Vital signs are within normal limits. Examination shows a grade 3/6 harsh holosystolic murmur at the left lower sternal border and a soft mid-diastolic murmur over the cardiac apex. The lungs are clear to auscultation. The remainder of the examination shows no abnormalities. Which of the following is the most likely explanation for this patient's physical findings?
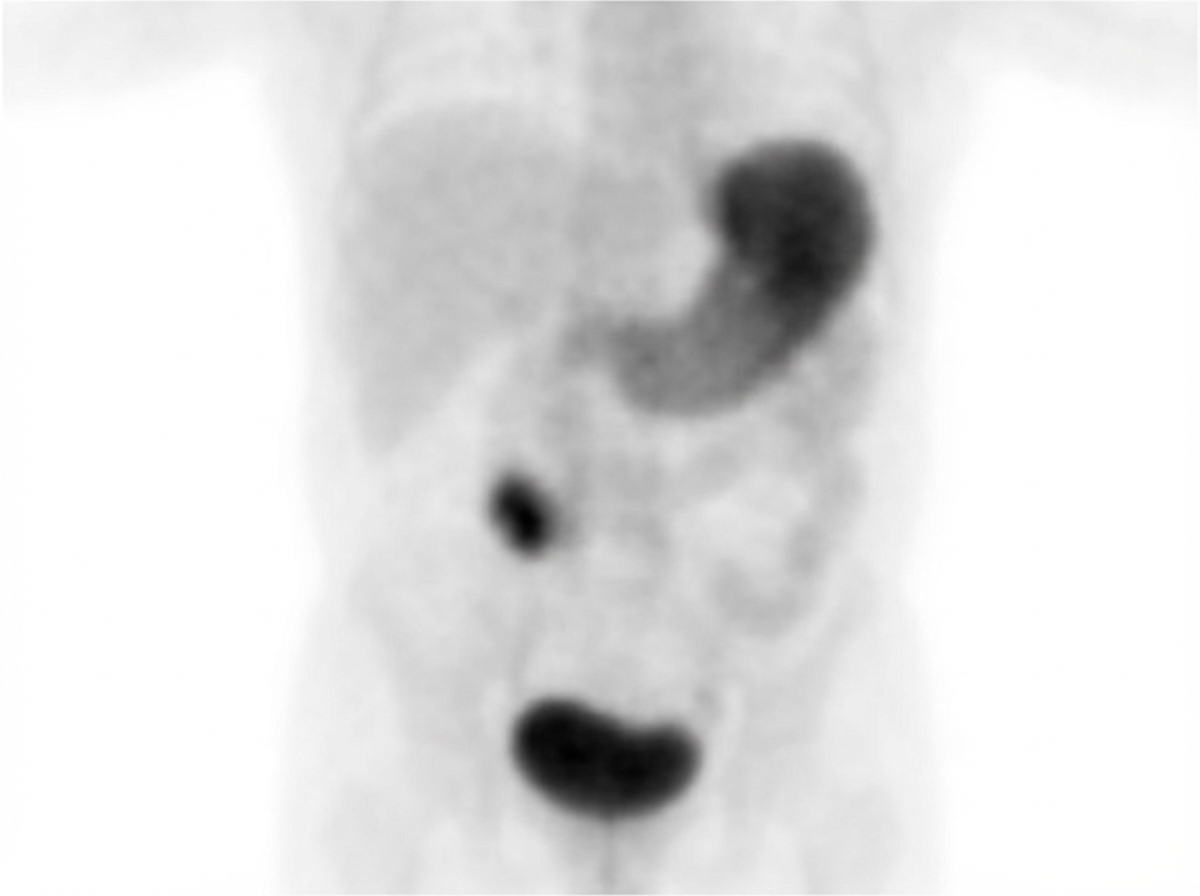
A 2-year-old, previously healthy female presents to the emergency department complaining of 7 hours of 10/10 intermittent abdominal pain, vomiting, and dark red stools. On exam, there is tenderness to palpation in the right lower quadrant and high-pitched bowel sounds. Technetium-99m pertechnetate scan was performed (Image A). Which of the following is true about this patient's condition?
A 2-year-old boy is brought to the emergency department because of a 5-minute episode of repetitive, involuntary, twitching movements of his left arm that occurred 1 hour ago. His symptoms began while playing with some toys. His parents say that he began to stand with support at 18 months and has recently started to walk with support. He speaks in bisyllables. He is at the 70th percentile for length and 80th percentile for weight. His vital signs are within normal limits. Examination shows a purple-pink patch over the right cheek that extends to the right eyelid. The right eyeball is firm. Neurologic examination shows left arm hypotonia and absent bicep reflex on the left side. Fundoscopy shows cupping of the right optic disc. Which of the following is the most likely cause of this patient's symptoms?
Practice by Chapter
Neural tube defects
Practice Questions
Congenital heart defects
Practice Questions
Gastrointestinal malformations
Practice Questions
Genitourinary anomalies
Practice Questions
Craniofacial anomalies
Practice Questions
Skeletal dysplasias
Practice Questions
Chromosomal disorders
Practice Questions
Teratogenic exposures
Practice Questions
Multiple malformation syndromes
Practice Questions
Prenatal diagnosis of congenital defects
Practice Questions
Surgical management timing
Practice Questions
Long-term outcomes and follow-up
Practice Questions
Preventive strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
