Congenital defects — MCQs

On this page
Two days following the home birth of her son, a mother brings the infant to the pediatric emergency room because of bilious vomiting. He is unable to pass meconium and his abdomen is distended. Endoscopic biopsy of the distal rectum demonstrates an absence of Meissner's and Auerbach's plexi in the bowel wall. Which of the following is the most likely diagnosis?
A 3550-g (7-lb 13-oz) male newborn is delivered at 37 weeks' gestation to a 28-year-old woman. Apgar scores are 9 and 10 at 1 and 5 minutes, respectively. His vital signs are within normal limits. Physical examination shows no abnormalities. Routine neonatal screening tests show mildly elevated TSH concentrations. Ultrasonography of the neck shows a complete absence of both lobes of the thyroid gland. This patient's normal physical examination findings, despite the total absence of a thyroid gland, is best explained by which of the following mechanisms?
A 14-year-old boy presents as a new patient to your practice. While conducting your physical exam, you observe the findings depicted in Figures A and B. Which of the following additional findings would most likely be found in this patient?
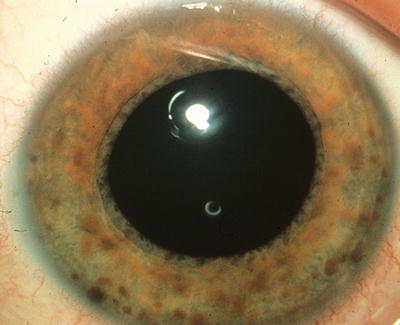
A 3000-g (6.6-lb) female newborn is delivered at term to a 23-year-old primigravid woman. The mother has had no prenatal care. Immunization records are not available. Cardiac examination shows a continuous heart murmur. There are several bluish macules on the skin that do not blanch with pressure. Slit lamp examination shows cloudy lenses in both eyes. The newborn does not pass his auditory screening tests. Which of the following is the most likely diagnosis?
A 7-month-old infant with Tetralogy of Fallot is brought to the emergency department by her parents because of a 1-day history of fever, cough, and difficulty breathing. She was born at 29 weeks of gestation. Her routine immunizations are up-to-date. She is currently in the 4th percentile for length and 2nd percentile for weight. She appears ill. Her temperature is 39.1°C (102.3°F). Physical examination shows diffuse wheezing, subcostal retractions, and bluish discoloration of the fingertips. Administration of which of the following would most likely have prevented this patient's current condition?
A 5-week-old infant born at 36 weeks' gestation is brought to the physician for a well-child examination. Her mother reports that she previously breastfed her for 15 minutes every 2 hours but now feeds her for 40 minutes every 4 hours. The infant has six wet diapers and two stools daily. She currently weighs 3500 g (7.7 lb) and is 52 cm (20.4 in) in length. Vital signs are with normal limits. Cardiopulmonary examination shows a grade 4/6 continuous murmur heard best at the left infraclavicular area. After confirming the diagnosis via echocardiography, which of the following is the most appropriate next step in management of this patient?
A 4-year-old boy is brought to the physician because of swelling around his eyes for 4 days. The swelling is most severe in the morning and milder by bedtime. Ten days ago, he had a sore throat that resolved spontaneously. His temperature is 37°C (98.6°F), pulse is 103/min, and blood pressure is 88/52 mm Hg. Examination shows 3+ pitting edema of the lower extremities and periorbital edema. The remainder of the examination shows no abnormalities. Laboratory studies show: Hemoglobin 15.3 g/dL Leukocyte count 10,500/mm3 Platelet count 480,000/mm3 Serum Urea nitrogen 36 mg/dL Glucose 67 mg/dL Creatinine 0.8 mg/dL Albumin 2.6 mg/dL Urine Blood negative Glucose negative Protein 4+ RBC none WBC 0–1/hpf Fatty casts numerous Protein/creatinine ratio 6.8 (N ≤0.2) Serum complement concentrations are within the reference ranges. Which of the following is the most appropriate next step in management?
A 26-year-old G1P0 woman at 32-weeks gestation presents for follow-up ultrasound. She was diagnosed with gestational diabetes during her second trimester, but admits to poor glucose control and non-adherence to insulin therapy. Fetal ultrasound reveals an asymmetric, enlarged interventricular septum, left ventricular outflow tract obstruction, and significantly reduced ejection fraction. Which of the following is the most appropriate step in management after delivery?
An 8-month-old boy is brought to a medical office by his mother. The mother states that the boy has been very fussy and has not been feeding recently. The mother thinks the baby has been gaining weight despite not feeding well. The boy was delivered vaginally at 39 weeks gestation without complications. On physical examination, the boy is noted to be crying in his mother’s arms. There is no evidence of cyanosis, and the cardiac examination is within normal limits. The crying intensifies when the abdomen is palpated. The abdomen is distended with tympany in the left lower quadrant. You suspect a condition caused by the failure of specialized cells to migrate. What is the most likely diagnosis?
A 13-year-old girl presents to a medical office for the evaluation of a lump on the front of her neck. The patient denies pain, but states that the mass bothers her because “it moves when I swallow”. The physical examination reveals a midline neck mass that is above the hyoid bone but below the level of the mandible. The mass is minimally mobile and feels fluctuant without erythema. The patient is afebrile and all vital signs are stable. A complete blood count and thyroid function tests are performed and are within normal limits. What is the most likely cause of this patient’s presentation?
Practice by Chapter
Neural tube defects
Practice Questions
Congenital heart defects
Practice Questions
Gastrointestinal malformations
Practice Questions
Genitourinary anomalies
Practice Questions
Craniofacial anomalies
Practice Questions
Skeletal dysplasias
Practice Questions
Chromosomal disorders
Practice Questions
Teratogenic exposures
Practice Questions
Multiple malformation syndromes
Practice Questions
Prenatal diagnosis of congenital defects
Practice Questions
Surgical management timing
Practice Questions
Long-term outcomes and follow-up
Practice Questions
Preventive strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
