Congenital defects — MCQs

On this page
An 18-month-old boy presents to the pediatrician by his mother for a routine check-up. The mother has no concerns, although she asks about the "hole in his heart" that the patient had at birth. The patient has no history of cyanosis or heart failure; however, a holosystolic, harsh murmur was noted at the 3- and 6-month check-ups. On examination, the patient is playful and alert. He has met all developmental milestones. The cardiac examination reveals a regular rate and rhythm with persistence of the holosystolic, harsh murmur. What is the most likely cause of the murmur in this child?
A 28-year-old primigravid woman is brought to the emergency department after complaining of severe abdominal pain for 3 hours. She has had no prenatal care. There is no leakage of amniotic fluid. Since arrival, she has had 5 contractions in 10 minutes, each lasting 70 to 90 seconds. Pelvic examination shows a closed cervix and a uterus consistent in size with a 38-week gestation. Ultrasound shows a single live intrauterine fetus in a breech presentation consistent with a gestational age of approximately 37 weeks. The amniotic fluid index is 26 and the fetal heart rate is 92/min. The placenta is not detached. She is scheduled for an emergency lower segment transverse cesarean section because of a nonreassuring fetal heart rate. The infant is delivered and APGAR score is noted to be 8 at 1 minute. The doctor soon notices cyanosis of the lips and oral mucosa, which does not resolve when the infant cries. The infant is foaming at the mouth and drooling. He also has an intractable cough. Which of the following is the most likely diagnosis?
Three days after delivery, a 4000-g (8.8-lb) male newborn has several episodes of right-sided arm and leg twitching and lip smacking. These shaking episodes have occurred about six times over the last hour and have lasted for about 40 seconds. He has also had rapid breathing and poor feeding. He has not had fever or trauma. He was born at 37 weeks' gestation. Pregnancy and delivery were uncomplicated. There is no family history of serious illness. His temperature is 37°C (98.6°F), pulse is 230/min, and respirations are 70/min. He appears irritable and jittery. There are intermittent spasms present. The remainder of the examination shows no abnormalities. Laboratory studies show a serum calcium concentration of 6 mg/dL and a serum parathyroid hormone concentration of 150 pg/mL. Which of the following is the most likely underlying cause of this patient's condition?
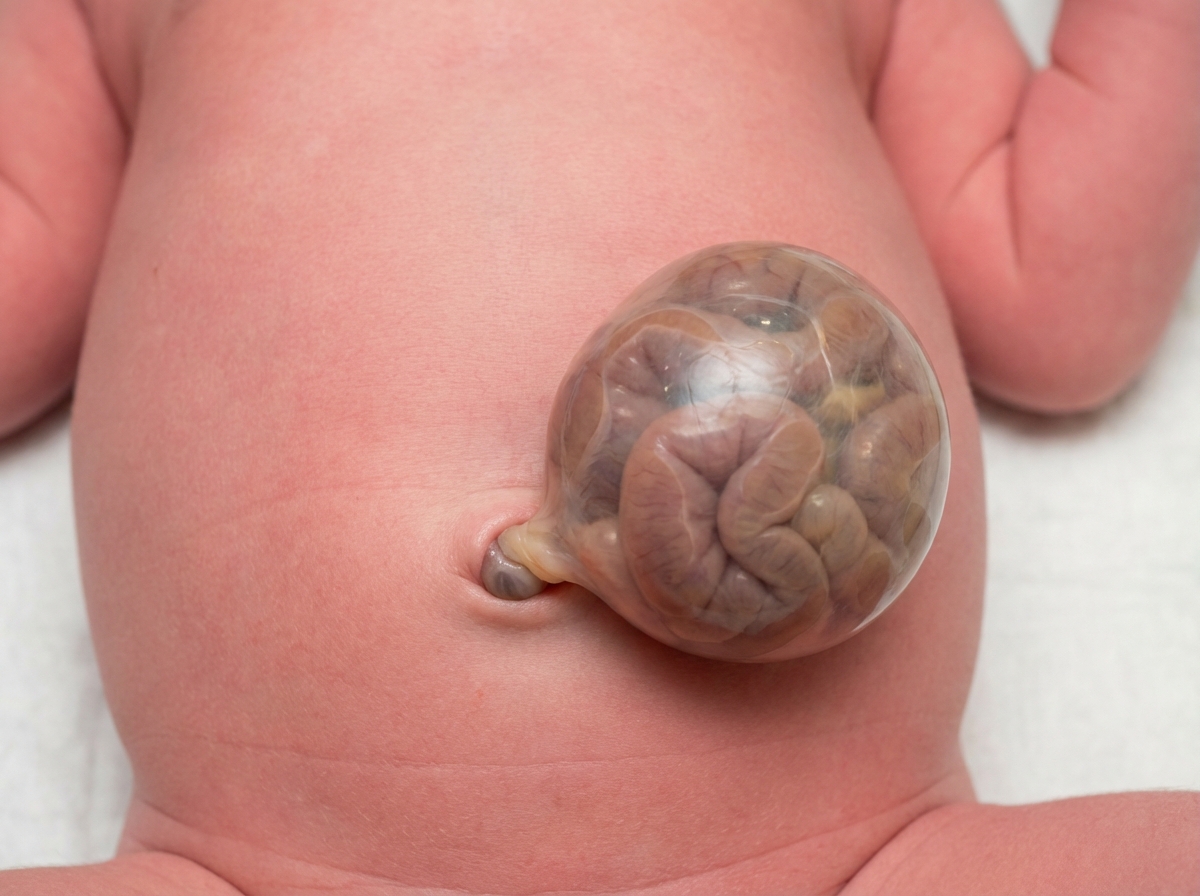
A 42-year-old woman presents to the emergency department in active labor. She has had no prenatal care and is unsure of the gestational age. Labor progresses rapidly and spontaneous vaginal delivery of a baby boy occurs 3 hours after presentation. On initial exam, the child is 1.9 kg (4.2 lb) with a small head and jaw. A sac-like structure containing intestine, as can be seen in the picture, protrudes from the abdominal wall. What complication is closely associated with this presentation?
A 6-year-old boy is brought in for evaluation by his adopted mother due to trouble starting 1st grade. His teacher has reported that he has been having trouble focusing on tasks and has been acting out while in class. His family history is unknown as he was adopted 2 years ago. His temperature is 36.2°C (97.2°F), pulse is 80/min, respirations are 20/min, and blood pressure 110/70 mm Hg. Visual inspection of the boy's face shows a low set nasal bridge, a smooth philtrum, and small lower jaw. Which of the following findings would also likely be found on physical exam?
A 2-year-old child is brought to the emergency department with rapid breathing and a severe cyanotic appearance of his lips, fingers, and toes. He is known to have occasional episodes of mild cyanosis, especially when he is extremely agitated. This is the worst episode of this child’s life, according to his parents. He was born with an APGAR score of 8 via a normal vaginal delivery. His development is considered delayed compared to children of his age. History is significant for frequent squatting after strenuous activity. On auscultation, there is evidence of a systolic ejection murmur at the left sternal border. On examination, his oxygen saturation is 71%, blood pressure is 81/64 mm Hg, respirations are 42/min, pulse is 129/min, and temperature is 36.7°C (98.0°F). Which of the following will most likely be seen on chest x-ray (CXR)?
A 2-year-old boy with a history of recurrent respiratory infections is brought to the physician for a follow-up examination. His height and weight are both at the 20th percentile. Crackles are heard in both lower lung fields. Cardiac auscultation shows a grade 3/6 holosystolic murmur over the left lower sternal border and a diastolic rumble heard best at the apex. If left untreated, this patient is most likely to develop which of the following?
A 3-year-old child is brought to the emergency department by his parents. The child presents with significant rapid breathing and appears unwell. On examination, his liver size is 1.5 times larger than children of his age, and he has mild pitting edema in his legs. This child is also in the lower weight-age and height-age percentiles. On auscultation, mild rales were noted and a fixed split S2 was heard on inspiration. There is no family history of congenital disorders or metabolic syndromes. Which of the following is the likely diagnosis?
A 7-year-old boy is brought by his parents to his pediatrician due to progressive fatigue and shortness of breath while playing sports. He is otherwise healthy with no known medical disorders and no other symptoms. The boy was born at 39 weeks gestation via spontaneous vaginal delivery. He is up to date on all vaccines and is meeting all developmental milestones. On physical examination, his temperature is 36.9ºC (98.4ºF), pulse rate is 90/min, blood pressure is 100/70 mm Hg, and respiratory rate is 18/min. Pulses in all four extremities are equal and normally palpated; there is no radio-femoral delay. The pediatrician suspects a congenital heart disease after auscultation of the heart. Which of the following congenital heart diseases is most likely to present with the clinical features listed above?
A 2200-g (4-lbs 13-oz) female newborn is delivered at term to a 37-year-old gravida 2, para 1 woman. The newborn is at the 10th percentile for length, 14th percentile for weight, and 3rd percentile for head circumference. Examination shows “punched-out“ skin lesions on the scalp, cleft lip, and a small chin. There is a convex-shaped deformity of the plantar surface of the feet. Auscultation shows a holosystolic murmur heard best at the left lower sternal border. Some of her intestines protrude through the umbilicus, covered by a thin membranous sac. An MRI of the brain shows a single ventricle and a fusion of the basal ganglia. Which of the following additional findings is most likely to be seen in this patient?
Practice by Chapter
Neural tube defects
Practice Questions
Congenital heart defects
Practice Questions
Gastrointestinal malformations
Practice Questions
Genitourinary anomalies
Practice Questions
Craniofacial anomalies
Practice Questions
Skeletal dysplasias
Practice Questions
Chromosomal disorders
Practice Questions
Teratogenic exposures
Practice Questions
Multiple malformation syndromes
Practice Questions
Prenatal diagnosis of congenital defects
Practice Questions
Surgical management timing
Practice Questions
Long-term outcomes and follow-up
Practice Questions
Preventive strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
