Congenital defects — MCQs

On this page
A 24-hour-old neonate girl is brought to the clinic by her mother because of cyanotic discoloration of the skin. Her mother says she is from a rural area and did not receive any prenatal care including vaccinations and prenatal counseling. On physical examination, a continuous murmur is heard over the left upper sternal border on auscultation. Which of the following cardiac findings is most likely in this patient?
A 5-year-old girl is brought to her pediatrician for vaccinations and a physical. She is a generally healthy child with no thumb on her right hand and a shortened and deformed left thumb. She was born at 39 weeks gestation via spontaneous vaginal delivery and is up to date on all vaccines and meeting all developmental milestones. On physical examination her vital signs are stable. On auscultation of the heart, the pediatrician notes a wide fixed split in the second heart sound (S2) and a medium-pitched systolic ejection murmur at the left sternal border. The murmur is not harsh in quality and is not accompanied by a thrill. Her echocardiogram confirms the diagnosis of acyanotic congenital heart defect with left-to-right shunt. Which of the following genetic syndromes is most consistent with this girl's congenital defects?
A 15-year-old boy is brought to the emergency department by his mother because of a 5-hour history of right lower quadrant pain, vomiting, and abdominal distention. Examination shows a palpable mass in the right lower quadrant of the abdomen. An x-ray of the abdomen shows a dilated ascending colon with an air-fluid level in the small intestine. A test is performed in which electrodes are placed on the nasal epithelium and the nose is perfused with several different solutions. When a chloride-free solution is administered, hyperpolarization across the nasal epithelium is absent. Which of the following is the most common cause of mortality in patients with the condition described here?
A six-month-old male presents to the pediatrician for a well-child visit. His mother reports that the patient has just started eating solids and sleeps well throughout the night. She notes that she often puts the patient to sleep on his stomach because he seems to breathe more easily in that position. The patient’s mother has noticed that the patient’s breathing becomes more “strained” when lying on his back. She cannot remember when this problem began, but she believes it has gotten worse in recent weeks. The patient was born at 40 weeks gestation and has no other past medical history. The patient’s temperature is 98.0°F (36.7°C), blood pressure is 75/55 mmHg, pulse is 115/min, and respirations are 24/min. His oxygen saturation is 98% on room air. On physical exam, the patient appears comfortable and has inspiratory stridor that improves while leaning forward. His lungs are otherwise clear to auscultation bilaterally. Which of the following is the most likely cause of this patient’s respiratory symptoms?
A male newborn is delivered at term to a 30-year-old woman. Pregnancy and delivery were uncomplicated. At birth, the umbilical cord is noted to be large. When the newborn cries, straw-colored fluid leaks from the umbilicus. The external genitalia appear normal. Which of the following is the most likely cause of this newborn's symptoms?
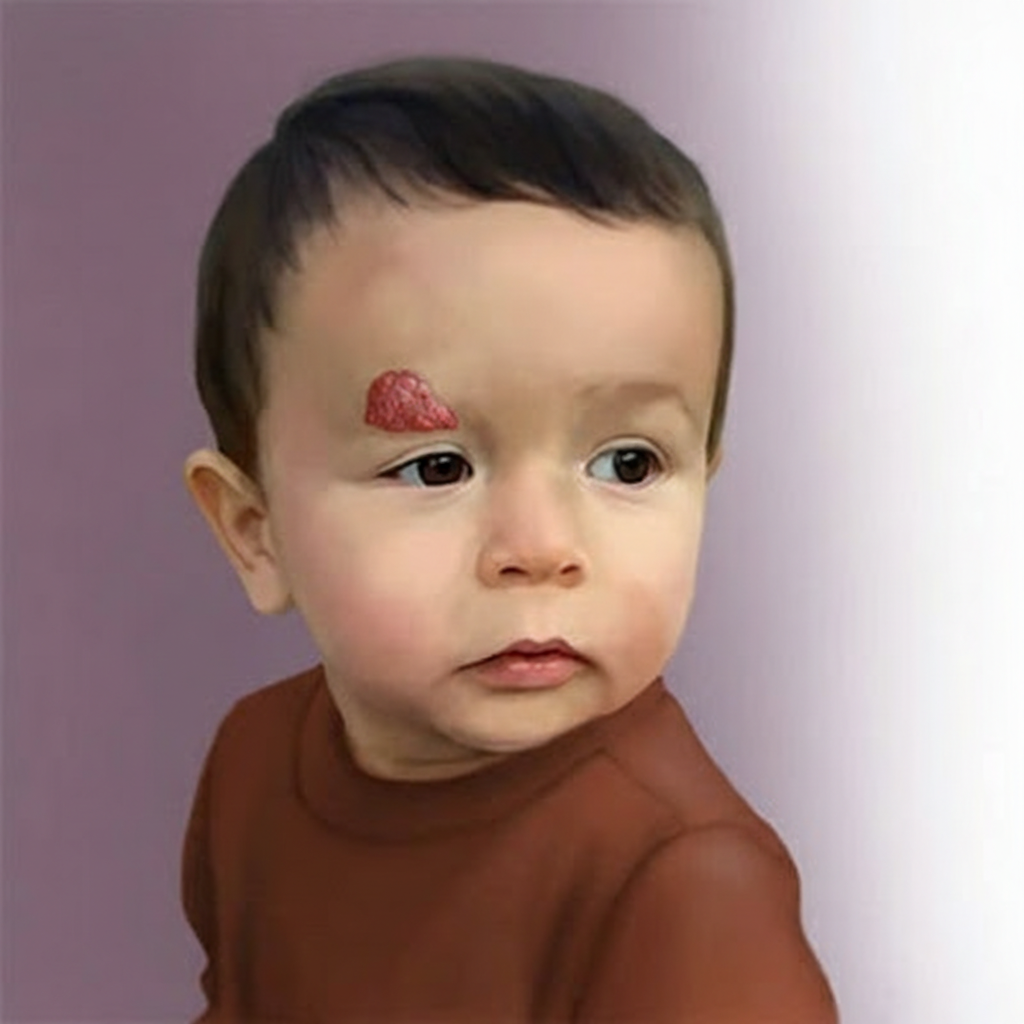
A 4-year-old boy is brought to the physician by his mother because of painless lesions on his face that he has had since shortly after birth. They recently moved to the USA from Indonesia where they had limited access to healthcare. A photograph of the lesions is shown. Which of the following is the most likely diagnosis?
A 4080-g (9-lb) male newborn is delivered at term to a 32-year-old woman, gravida 2, para 1. Apgar scores are 8 and 9 at 1- and 5-minutes, respectively. Examination in the delivery room shows both feet pointing downwards and inwards. Both the forefeet are twisted medially in adduction, with the hindfeet elevated and the midfeet appearing concave. Both Achilles tendons are taut on palpation. There are skin creases on the medial side of both feet. The deformity persists despite attempts to passively straighten the foot. X-rays of both feet confirm the suspected diagnosis. Which of the following is the most appropriate next step in the management of this patient?
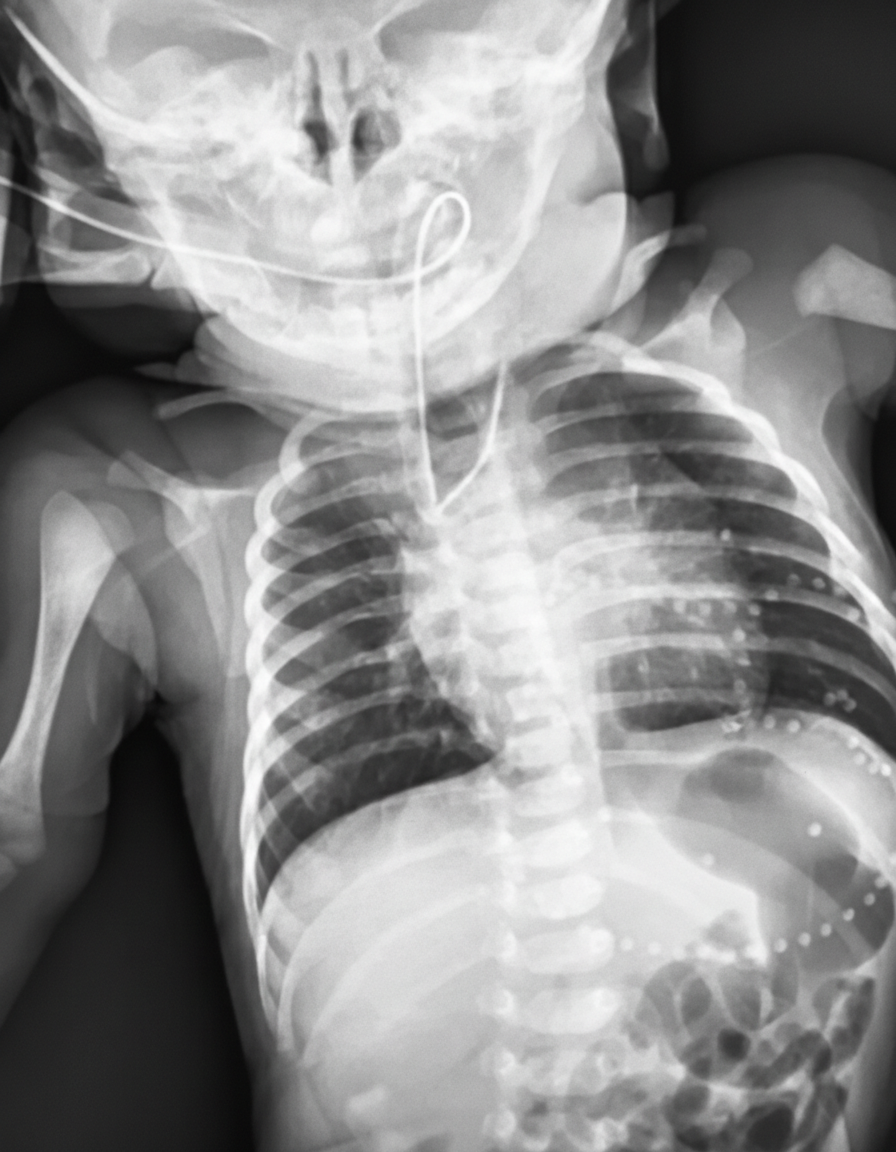
Thirty minutes after delivery, a 3400-g (7.5-lb) female newborn develops cyanosis of her lips and oral mucosa. She was born at 36 weeks of gestation to a 30-year-old woman, gravida 1, para 0. Apgar scores are 7 and 8 at 1 and 5 minutes, respectively. Pregnancy was complicated by polyhydramnios. The patient's temperature is 37°C (98.6°F), pulse is 144/min, respirations are 52/min, and blood pressure is 70/40 mm Hg. Examination shows foaming and drooling at the mouth. Bilateral crackles are heard at the lung bases. There is a harsh 3/6 systolic murmur along the left sternal border. The abdomen is soft and mildly distended. There is an anterior ectopic anus. Insertion of a nasogastric tube is attempted. An x-ray of the chest and abdomen is shown. Which of the following is the most likely diagnosis?
A 3-year-old boy is brought to the emergency department because of increasing shortness of breath for 2 days. He is at 30th percentile for height and at 25th percentile for weight. His temperature is 37.1°C (98.8°F), pulse is 144/min, respirations are 40/min, and blood pressure is 80/44 mm Hg. Bilateral crackles are heard at the lung bases. A grade 3/6 holosystolic murmur is heard over the left lower sternal border. A grade 2/6 mid-diastolic murmur is heard best in the left fourth intercostal space. Without treatment, this patient is at risk of developing which of the following?
An 18-month-old boy is brought to the emergency department after losing consciousness. His mother states that he was running with other kids in the park when he suddenly fell down and became unresponsive for less than 1 minute. He has not had any immunizations due to their religious beliefs. The parents report that he plays with other children, but tires easily. He has had difficulty feeding, but there was no follow-up with a pediatrician. The heart rate was 120/min and the oxygen saturation was 91%. The height is in the 40th percentile and the weight is in the 50th percentile. On examination, the boy is crying with perioral cyanosis. The lung sounds are clear. S-1 is normal and there is a single S-2. A grade 2/6 systolic ejection murmur is appreciated at the left upper sternal border. When the child squats, the murmur is intensified and the cyanosis improves. What is the most appropriate next step in the management of this patient?
Practice by Chapter
Neural tube defects
Practice Questions
Congenital heart defects
Practice Questions
Gastrointestinal malformations
Practice Questions
Genitourinary anomalies
Practice Questions
Craniofacial anomalies
Practice Questions
Skeletal dysplasias
Practice Questions
Chromosomal disorders
Practice Questions
Teratogenic exposures
Practice Questions
Multiple malformation syndromes
Practice Questions
Prenatal diagnosis of congenital defects
Practice Questions
Surgical management timing
Practice Questions
Long-term outcomes and follow-up
Practice Questions
Preventive strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
