Congenital defects — MCQs

On this page
A 3-year-old is brought to the pediatrician by his mother. She is concerned that he appears fatigued all the time. She also mentions that he struggles to get out of his seat after eating his meals and that he waddles when he walks now. The child was born at 39 weeks via spontaneous vaginal delivery. He is up to date on all his vaccines and meeting all developmental goals. A maternal uncle had similar symptoms that started in early childhood. He has a heart rate of 90/min, respiratory rate of 22/min, blood pressure of 110/65 mm Hg, and temperature of 37.0°C (98.6°F). The child appears lethargic. He was much more active during his previous well-child visit. Upon examination, the child has thick calves and uses his hands to support himself as he stands up from a sitting position. His reflexes are decreased bilaterally. Lab studies show elevated creatinine phosphokinase (CPK) and lactate dehydrogenase (LDH). Which of the following is the most likely cause of this patient's condition?
A 2-week-old newborn girl is brought to the physician for a follow-up examination after the initial newborn examination showed asymmetry of the legs. She was born at term to a 26-year-old woman, gravida 3, para 2. Pregnancy was complicated by a breech presentation and treated with an emergency lower-segment transverse cesarean section. The newborn's head circumference is 35 cm (13.7 in). She is at the 60th percentile for length and 75th percentile for weight. Cardiac examination shows no abnormalities. The spine and overlying skin do not indicate significant abnormalities. Abduction of the right hip after cupping the pelvis and flexing the right hip and knee causes a palpable clunk. The feet exhibit no deformities. Ultrasonography of the hip revealed a 50° angle between the lines along the bone acetabulum and the ilium. Which of the following is the most appropriate next step in management?
A 2-week-old newborn is brought to the physician because of worsening feeding difficulty since birth. Examination shows a grade 2/6 harsh holosystolic murmur, heard most clearly at the left lower sternal border, and a soft mid-diastolic rumble over the cardiac apex. Echocardiography shows shunting of blood through the ventricular septum during systole. The patient undergoes surgery for closure of the defect. Which of the following sets of changes are expected after successful repair of this cardiac defect? Left atrial pressure | Left ventricular pressure | Right ventricular pressure
A 4-year-old girl is brought to the physician by her mother for a follow-up examination. She has a history of recurrent asthma attacks. The mother reports that her daughter has also had mild abdominal pain for the past 2 weeks. The patient's current medications include daily inhaled fluticasone and inhaled albuterol as needed. She appears well. Her temperature is 37°C (98.6°F), pulse is 100/min, and blood pressure is 130/85 mm Hg. The lungs are clear to auscultation. Cardiac examination shows no murmurs, rubs, or gallops. Abdominal examination shows a left-sided, nontender, smooth abdominal mass that does not cross the midline. The remainder of the examination shows no abnormalities. A complete blood count and serum concentrations of electrolytes, urea nitrogen, and creatinine are within the reference range. Which of the following is the most likely diagnosis?
An otherwise healthy 15-year-old boy comes to the physician for a routine health maintenance examination. He feels well and is doing well in school. He has no history of serious illness. Vital signs are within normal limits. The lungs are clear to auscultation. Cardiac auscultation shows no murmur, but a wide-split S2 that does not change with respiration. If left untreated, this patient is at increased risk for which of the following complications?
A 6-year-old boy presents to his pediatrician’s office for muscle weakness. The patient is accompanied by his mother who states that he has difficulty running and walking up the stairs. The mother has noticed mild weakness when the patient attempts to sit up from a supine position since he was 4-years-old. Medical history is significant for fractures involving the arms and legs secondary to falling. On physical exam, the child does not appear to be in distress and is conversational. He has a waddling gait along with lumbar lordosis and bilateral calf enlargement. The patient uses his hands to push himself into an upright position when arising from the floor. He has absent patellar and ankle-jerk reflexes. Which of the following is the best next step to confirm the diagnosis?
A 6-year-old boy is brought to the physician because of inability to concentrate and difficulties completing assignments at school. His mother says that he frequently interrupts others during conversations at home and that his teachers often reprimand him for talking excessively in school. He refuses to play with the other children and often has physical altercations with his classmates. He can jump up and down but he cannot hop on one foot. He eats without assistance but has difficulty using silverware. He cannot follow three-step directions. There is no family history of serious illness. Examination shows a small head, wide-spaced eyes, and short palpebral fissures. His upper lip is thin and flat. He has a sunken nasal bridge and a small jaw. There is a 3/6 pansystolic murmur heard along the left lower sternal border. Which of the following is the most likely cause of these findings?
A 28-year-old pregnant female presents for a prenatal check-up at 20 weeks gestation, which includes routine screening ultrasound. Fetal ultrasound demonstrates bilateral multicystic dysplastic kidneys. Her pregnancy has been complicated by persistent oligohydramnios. The child requires significant pulmonary support upon delivery. Which of the following clinical findings is most likely present in this child as a result of these abnormalities?
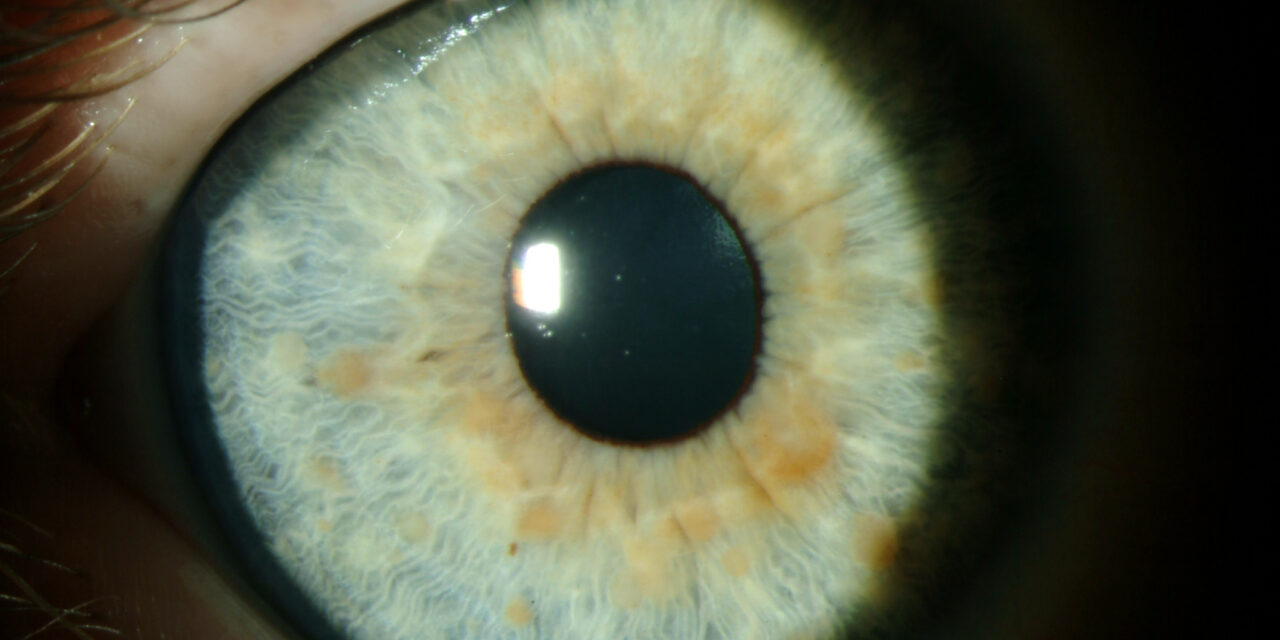
A 9-year-old girl is brought to her pediatrician by her mother for the evaluation of recent-onset seizures. She has had 2 episodes of generalized tonic-clonic seizures in the past 3 days. Each episode lasted for 1–2 minutes and aborted spontaneously. There is no history of fever, headache, altered behavior, diarrhea, vomiting, or previous seizure episodes. Past medical history is unremarkable. Physical examination reveals: blood pressure 102/64 mm Hg, heart rate 89/min, respiratory rate 16/min, and temperature 37.0°C (98.6°F). She looks anxious but oriented to time and space. Multiple flat hyperpigmented spots are present over her body, each more than 5 mm in diameter. Axillary freckling is present. Cranial nerves are intact. Muscle strength is normal in all 4 limbs with a normal sensory examination. Gait is normal. An eye examination is shown in the exhibit. What is the most likely diagnosis?
A 4-year-old boy is brought to the pediatrician’s office for a flu-like episode. His father tells the physician that his child has fallen ill several times over the past few months. He also has occasional bouts of night sweats and loss of appetite. He has lost 5 lbs (2.3 kg) in the last 6 months. At the pediatrician’s office, his temperature is 38.9°C (102°F), pulse is 105/min and respiration rate is 18/min. On physical examination, the pediatrician observes a flattened facial profile, prominent epicanthal folds, and a single palmar crease. There are petechiae on the arms and legs. Blood count shows pancytopenia. Bone marrow aspiration is diagnostic for ALL (acute lymphoblastic leukemia), but all cells also show a trisomy. Children with similar genetic anomalies are at an increased risk of developing which of the following neurological conditions as they grow older?
Practice by Chapter
Neural tube defects
Practice Questions
Congenital heart defects
Practice Questions
Gastrointestinal malformations
Practice Questions
Genitourinary anomalies
Practice Questions
Craniofacial anomalies
Practice Questions
Skeletal dysplasias
Practice Questions
Chromosomal disorders
Practice Questions
Teratogenic exposures
Practice Questions
Multiple malformation syndromes
Practice Questions
Prenatal diagnosis of congenital defects
Practice Questions
Surgical management timing
Practice Questions
Long-term outcomes and follow-up
Practice Questions
Preventive strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
