Congenital defects — MCQs

On this page
A 4-hour-old male newborn has perioral discoloration for the past several minutes. Oxygen by nasal cannula does not improve the cyanosis. He was delivered by cesarean delivery at 37 weeks' gestation to a 38-year-old woman, gravida 3, para 2. Apgar scores were 8 and 9 at 1 and 5 minutes, respectively. The mother has type 2 diabetes mellitus that was well-controlled during the pregnancy. She has not received any immunizations since her childhood. The newborn's temperature is 37.1°C (98.8°F), pulse is 170/min, respirations are 55/min, and blood pressure is 80/60 mm Hg. Pulse oximetry shows an oxygen saturation of 85%. Cardiopulmonary examination shows a 2/6 holosystolic murmur along the lower left sternal border. The abdomen is soft and non-tender. Echocardiography shows pulmonary arteries arising from the posterior left ventricle, and the aorta rising anteriorly from the right ventricle. Which of the following is the most appropriate next step in the management of this patient?
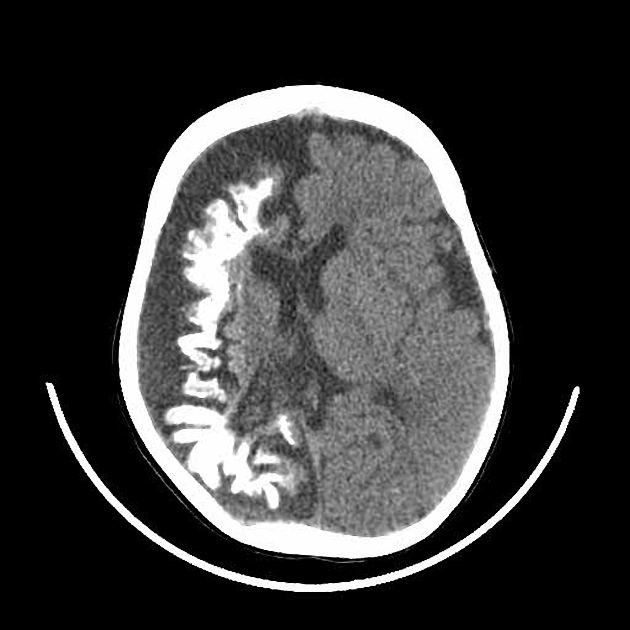
A 10-year-old boy is brought to a family physician by his mother with a history of recurrent headaches. The headaches are moderate-to-severe in intensity, unilateral, mostly affecting the left side, and pulsatile in nature. Past medical history is significant for mild intellectual disability and complex partial seizures that sometimes progress to secondary generalized seizures. He was adopted at the age of 7 days. His birth history and family history are not available. His developmental milestones were slightly delayed. There is no history of fever or head trauma. His vital signs are within normal limits. His height and weight are at the 67th and 54th percentile for his age. Physical examination reveals an area of bluish discoloration on his left eyelid and cheek. The rest of the examination is within normal limits. A computed tomography (CT) scan of his head is shown in the exhibit. Which of the following additional clinical findings is most likely to be present?
A 1-week-old baby is brought to the pediatrician’s office for a routine checkup. On examination, she is observed to have microcephaly with a prominent occiput. She also has clenched fists and rocker-bottom feet with prominent calcanei. A cardiac murmur is evident on auscultation. Based on the clinical findings, a diagnosis of nondisjunction of chromosome 18 is suspected. The pediatrician orders a karyotype for confirmation. He goes on to explain to the mother that her child will face severe growth difficulties. Even if her daughter progresses beyond a few months, she will not be able to reach developmental milestones at the appropriate age. In addition to the above, which of the following is most likely a consequence of this genetic disturbance?
An 8-year-old child with “elfin” facial features is very friendly with strangers. He has a history of mild mental retardation, and a hemizygous deletion on chromosome 7q11.23, that includes a portion of the elastin gene. Which of the following is most likely true in this patient?
A 15-year-old boy is brought to the physician by his mother for a well-child examination. He recently stopped attending his swim classes. The patient is at the 97th percentile for height and the 50th percentile for weight. Examination shows decreased facial hair, bilateral breast enlargement, and long extremities. Genital examination shows scant pubic hair, small testes, and a normal-sized penis. Further evaluation is most likely to show which of the following karyotypes?
A 5-year-old girl is brought to the emergency department by her mother with seizures. The blood glucose is 94 mg/dl and the serum calcium is 5.3 mg/dl; however, the PTH levels are low. The medical history includes a delay in achieving developmental milestones. Her mother also says she needs frequent hospital visits due to recurrent bouts with the flu. The cardiovascular examination is within normal limits. What is the most likely cause underlying this presentation?
A 14-year-old boy is brought to the physician because of increasing swelling of his legs and generalized fatigue for 1 month. During this period he has also had a productive cough and shortness of breath. He has been unable to carry out his daily activities. He has a history of recurrent respiratory tract infections and chronic nasal congestion since childhood. He has a 3-month history of foul-smelling and greasy stools. He is at 4th percentile for height and weight. His temperature is 37°C (98.6°F), pulse is 112/min, respirations are 23/min, and blood pressure is 104/64 mm Hg. Examination shows clubbing of his fingers and scoliosis. There is 2+ pitting edema of the lower extremities. Jugular venous distention is present. Inspiratory crackles are heard in the thorax. Cardiac examination shows a loud S2. The abdomen is mildly distended and the liver is palpated 2 cm below the right costal margin. Hepato-jugular reflux is present. Which of the following is the most likely diagnosis?
A 6-year-old male presents to the pediatrician with seizures. His mother reports that the patient has had two seizures lasting about 30 seconds each over the last three days. She reports that the patient has previously had seizures a few times per year since he was 12 months of age. The patient’s past medical history is otherwise notable for intellectual disability. He rolled over at 14 months of age and walked at 24 months of age. The patient’s mother denies any family history of epilepsy or other neurologic diseases. The patient is in the 3rd percentile for height and the 15th percentile for weight. On physical exam, he has a happy demeanor with frequent smiling. The patient has strabismus and an ataxic gait accompanied by flapping of the hands. He responds intermittently to questions with one-word answers. This patient is most likely to have which of the following genetic abnormalities?
A 4-month-old male infant is brought to the physician by his father because of swelling of his left hemiscrotum. He has otherwise been healthy and is gaining weight appropriately. Physical examination shows a nontender left scrotal mass that transilluminates. The mass increases in size when the boy cries but is easily reducible. Which of the following is the most likely underlying cause of this patient's findings?
An inconsolable mother brings her 2-year-old son to the emergency room after finding a large amount of bright red blood in his diaper, an hour ago. She states that for the past week her son has been having crying fits while curling his legs towards his chest in a fetal position. His crying resolves either after vomiting or passing fecal material. Currently, the child is in no apparent distress. Physical examination with palpation in the gastric region demonstrates no acute findings. X-ray of the abdominal area demonstrates no acute findings. His current temperature is 36.5°C (97.8°F), heart rate is 93/min, blood pressure is 100/64 mm Hg, and respiratory rate is 26/min. His weight is 10.8 kg (24.0 lb), and height is 88.9 cm (35.0 in). Laboratory tests show the following: RBC count 5 million/mm3 Hematocrit 36% Hemoglobin 12 g/dL WBC count 6,000/mm3 Mean corpuscular volume 78 fL What is the most likely underlying embryological cause predisposing to this condition?
Practice by Chapter
Neural tube defects
Practice Questions
Congenital heart defects
Practice Questions
Gastrointestinal malformations
Practice Questions
Genitourinary anomalies
Practice Questions
Craniofacial anomalies
Practice Questions
Skeletal dysplasias
Practice Questions
Chromosomal disorders
Practice Questions
Teratogenic exposures
Practice Questions
Multiple malformation syndromes
Practice Questions
Prenatal diagnosis of congenital defects
Practice Questions
Surgical management timing
Practice Questions
Long-term outcomes and follow-up
Practice Questions
Preventive strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
