Congenital defects — MCQs

On this page
A 15-year-old adolescent is brought to the physician by her parents. She is concerned that she has not started menstruating yet. She is also self-conscious because her chest has not yet developed and all of her friends are taller and much more developed. Past medical history is noncontributory. Her mother started menstruating around the age of 13 and her older sister at the age of 12. The patient is more concerned about her poor performance in sports. She says that she can not participate in sports like before and gets tired very early. Today, her heart rate is 90/min, respiratory rate is 17/min, blood pressure is 110/65 mm Hg, and temperature of 37.0°C (98.6°F). On physical exam, her heart has a regular rate and rhythm and lungs are clear to auscultation bilaterally. On physical exam, her brachial pulses appear bounding (4+) and her femoral pulses are diminished (2+). Her legs also appear mildly atrophic with poor muscle development bilaterally. Her neck appears short with excessive skin in the lateral neck area. This patient’s symptoms are most likely associated with which of the following conditions?
A newborn girl is rushed to the neonatal ICU after an emergency cesarean section due to unstable vital signs after delivery. The pregnancy was complicated due to oligohydramnios and pulmonary hypoplasia. Gestation was at 38 weeks. APGAR scores were 6 and 8 at 1 and 5 minutes respectively. The newborn’s temperature is 37.0°C (98.6°F), the blood pressure is 60/40 mm Hg, the respiratory rate is 45/min, and the pulse is 140/min. Physical examination reveals irregularly contoured bilateral abdominal masses. Abdominal ultrasound reveals markedly enlarged echogenic kidneys (5 cm in the vertical dimension) with multiple cysts in the cortex and medulla. This patient is at highest risk of which of the following complications?
A 6-month-old boy is brought to the physician because of a right-sided scrotal swelling for the past 2 months. The swelling is intermittent and appears usually after the patient has been taken outdoors in a baby carrier, and disappears the next morning. The patient was born at term without complications and has been healthy. Examination shows a 3-cm, soft, nontender, and fluctuant right scrotal mass that is reducible and does not extend into the inguinal area. A light held behind the scrotum shines through. There are no bowel sounds in the mass. The remainder of the examination shows no abnormalities. Which of the following is the most appropriate next step in the management of this patient?
A 5-day-old boy is brought to see his pediatrician after his newborn blood screening showed elevated levels of immunoreactive trypsinogen, a marker for cystic fibrosis. The boy was born at 39 weeks gestation after regular prenatal care. He has 2 siblings that tested negative on screening. On physical exam, his vitals are normal and he appears healthy. Which of the following tests should be performed next to evaluate the newborn for cystic fibrosis?
A 4-month-old boy is brought by his mother to the pediatrician for a routine check-up. He was born at 39 weeks' gestation with a birth weight of 2.1 kg. Apgar scores were 6 and 8 at 1 and 5 minutes, respectively. The child has had feeding difficulties requiring supplemental feeding and frequent awakening at night. He has delayed developmental milestones and does not yet smile spontaneously. He is behind on his vaccination schedule due to frequent illnesses. His temperature is 98.6°F (37°C), blood pressure is 95/60 mmHg, pulse is 140/min, and respirations are 35/min. On physical examination, he has microcephaly, a prominent forehead, hypertelorism, a broad nasal bridge, and micrognathia. He also has hypotonia and is unable to hold his head steady when unsupported. This patient's condition is associated with a mutation in which of the following chromosomes?
A 1-month-old infant is brought to the physician for a well-child examination. His mother reports that she had previously breastfed her son every 2 hours for 15 minutes but is now feeding him every 4 hours for 40 minutes. She says that the infant sweats a lot and is uncomfortable during feeds. He has 6 wet diapers and 2 stools daily. He was born at 36 weeks' gestation. He currently weighs 3500 g (7.7 lb) and is 52 cm (20.4 in) in length. He is awake and alert. His temperature is 37.1°C (98.8°F), pulse is 170/min, respirations are 55/min, and blood pressure is 80/60 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 99%. Cardiopulmonary examination shows a 4/6 continuous murmur along the upper left sternal border. After confirming the diagnosis via echocardiography, which of the following is the most appropriate next step in the management of this patient?
A 14-month-old boy has iron-deficiency anemia refractory to iron therapy. His stool is repeatedly positive for occult blood. The parents bring the child to the emergency room after they notice some blood in his stool. Which of the following is the diagnostic gold standard for this patient's most likely condition?
A 31-year-old woman delivers a healthy boy at 38 weeks gestation. The delivery is vaginal and uncomplicated. The pregnancy was unremarkable. On examination of the newborn, it is noted that his head is tilted to the left and his chin is rotated to the right. Palpation reveals no masses or infiltration in the neck. The baby also shows signs of left hip dysplasia. Nevertheless, the baby is active and exhibits no signs of other pathology. What is the most probable cause of this patient's condition?
Over the course of a year, 5 children with identical congenital heart defects were referred to a pediatric cardiac surgeon for evaluation. All 5 children had stable vital signs and were on appropriate medication. Upon review of medical records, all of them had a loud holosystolic murmur over the third intercostal space at the left sternal border. The surgeon ordered echocardiograms for all 5 children and recommended surgical closure of the defect in one of them. Which of the following patients required surgical repair of their defect?
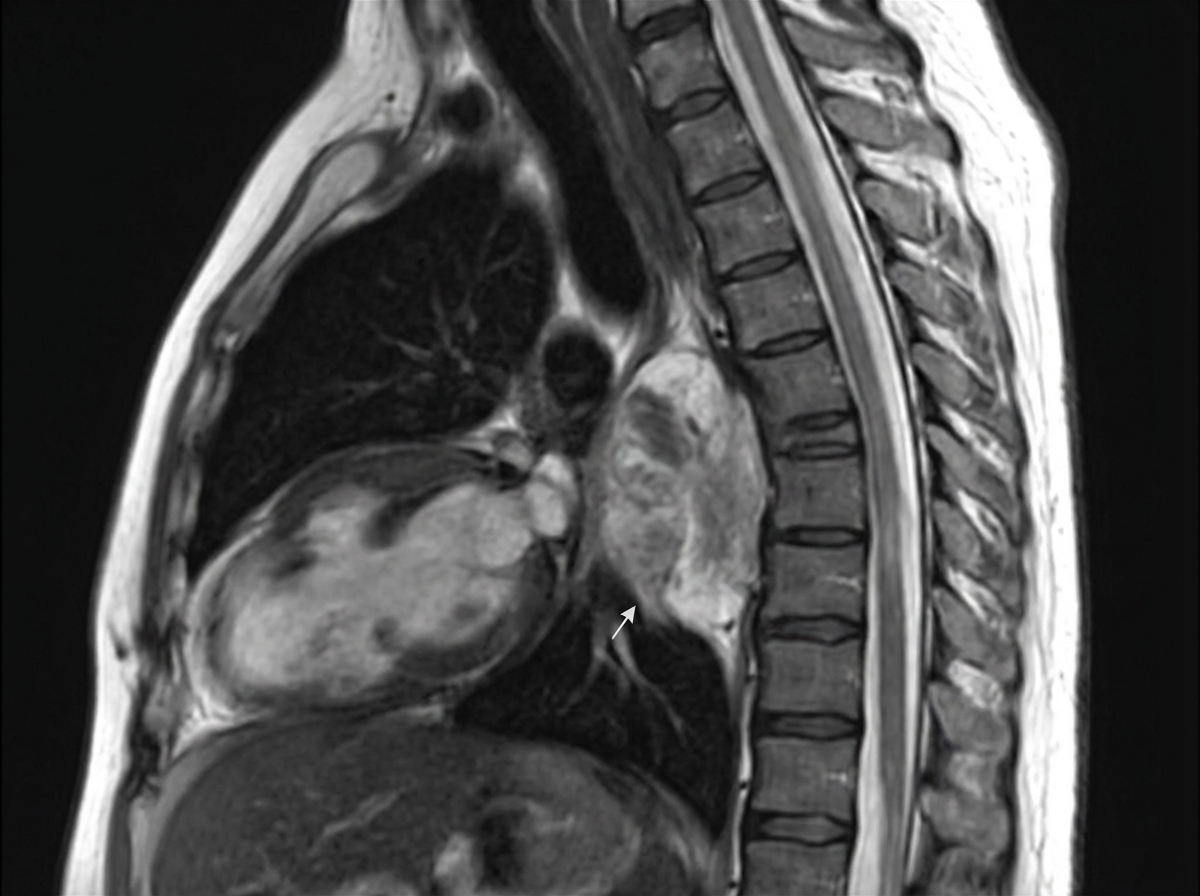
A 7-year-old girl presents with a lump in her neck which she noticed a few days ago. The patient's mother states that her daughter's left eyelid seems to be drooping, making her left eye look small. There is no significant past medical history. On neurological examination, the patient has normal bilateral pupillary reflexes but a miotic left pupil. A lateral radiograph of the chest reveals a mass in the posterior mediastinum with no evidence of bone erosion. An MRI is performed and the results are shown in the image. An imaging-guided biopsy of the mass reveals spindle-shaped cells arranged chaotically, with moderate cytoplasm and small nuclei. Scattered mature ganglion cells with abundant cytoplasm and round to oval nuclei are also present. The biopsy tissue is analyzed with immunohistochemistry and found to be positive for S-100, synaptophysin, and chromogranin. Which of the following factors is associated with poor prognosis for this patient's most likely diagnosis?
Practice by Chapter
Neural tube defects
Practice Questions
Congenital heart defects
Practice Questions
Gastrointestinal malformations
Practice Questions
Genitourinary anomalies
Practice Questions
Craniofacial anomalies
Practice Questions
Skeletal dysplasias
Practice Questions
Chromosomal disorders
Practice Questions
Teratogenic exposures
Practice Questions
Multiple malformation syndromes
Practice Questions
Prenatal diagnosis of congenital defects
Practice Questions
Surgical management timing
Practice Questions
Long-term outcomes and follow-up
Practice Questions
Preventive strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
