Congenital defects — MCQs

On this page
A female infant is born with a mutation in PKD1 on chromosome 16. An abdominal ultrasound performed shortly after birth would most likely reveal which of the following?
A previously healthy 2-year-old girl is brought to the physician because of a 1-week history of yellow discoloration of her skin, loss of appetite, and 3 episodes of vomiting. Her parents also report darkening of her urine and light stools. During the last 2 days, the girl has been scratching her abdomen and arms and has been crying excessively. She was born at 38 weeks' gestation after an uncomplicated pregnancy and delivery. Her family emigrated from Japan 8 years ago. Immunizations are up-to-date. Her vital signs are within normal limits. Examination shows jaundice of her skin and sclerae. Abdominal examination shows a mass in the right upper abdomen. Serum studies show: Bilirubin (total) 5 mg/dL Direct 4.2 mg/dL Aspartate aminotransferase (AST) 20 U/L Alanine aminotransferase (ALT) 40 U/L γ-Glutamyltransferase (GGT) 110 U/L Abdominal ultrasonography shows dilation of the gall bladder and a fusiform dilation of the extrahepatic bile duct. Which of the following is the most likely diagnosis?
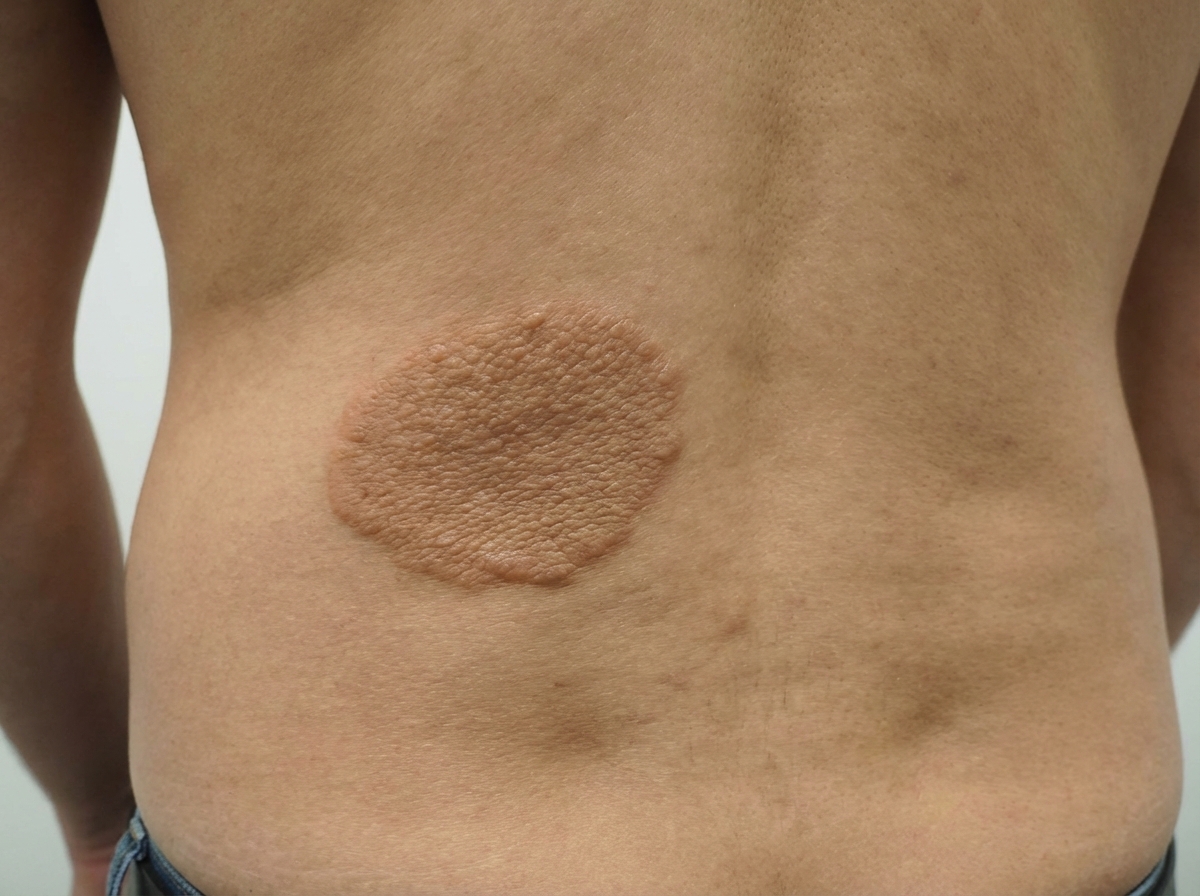
An 8-year-old boy presents with a skin lesion on his back as shown in the picture. On physical examination, there are synchronous spasmodic movements of the neck, trunk, and extremities. The physician explains that this is likely due to a genetic condition, and further testing would be necessary to confirm the diagnosis. Which of the following genes is involved in the development of this patient’s condition?
Cardiac surgery is consulted on a newborn with a large ventricular septal defect. The child has poor weight gain and feeding difficulties. He requires furosemide and captopril to avoid dyspnea. On physical examination his temperature is 36.9°C (98.4°F), pulse rate is 158/min, respiratory rate is 30/min, and blood pressure is 94/62 mm Hg. Chest auscultation reveals a holosystolic murmur along the left lower sternal border and a mid-diastolic low-pitched rumble at the apex. Abdominal examination reveals the presence of hepatomegaly. An echocardiogram confirms a diagnosis of a membranous VSD while hemodynamic studies show a Qp:Qs ratio of 2.8:1. Which of the following is the best management option?
A 3-week-old firstborn baby girl is brought to the pediatric emergency room with projectile vomiting. She started vomiting while feeding 12 hours ago and has been unable to keep anything down since then. After vomiting, she appears well and hungry, attempting to feed again. The vomitus has been non-bloody and non-bilious. The last wet diaper was 10 hours ago. The child was born at 40 weeks gestation to a healthy mother. On examination, the child appears sleepy but has a healthy cry during the exam. The child has dry mucous membranes and delayed capillary refill. There is a palpable olive-shaped epigastric mass on palpation. Which of the following is the most likely cause of this patient's condition?
A 28-year-old woman gives birth to a male infant. During her third-trimester antenatal sonogram, the radiologist noted a suspected congenital heart defect, but the exact nature of the defect was not clear. The pediatrician orders an echocardiogram after making sure that the baby’s vital signs are stable. This reveals the following findings: atresia of the muscular tricuspid valve, pulmonary outflow tract obstruction, open patent ductus arteriosus, a small ventricular septal defect, and normally related great arteries. The pediatrician explains the nature of the congenital heart defect to the infant's parents. He also informs them about the probable clinical features that are likely to develop in the infant, the proposed management plan, and the prognosis. Which of the following signs is most likely to manifest first in this infant?
A 3-week-old boy has non-bilious projectile vomiting that occurred after feeding. After vomiting, the infant is still hungry. The infant appears dehydrated and malnourished. A firm, “olive-like” mass of about 1.5 cm in diameter is palpated in the right upper quadrant, by the lateral edge of the rectus abdominus muscle. On laboratory testing, the infant is found to have a hypochloremic, hypokalemic metabolic alkalosis. Which of the following is most likely the cause of this patient’s symptoms?
A 12-day-old male newborn is brought to the emergency department because of a high-grade fever for 3 days. He has been lethargic and not feeding well during this period. He cries incessantly while passing urine. There is no family history of serious illness. He was delivered at 37 weeks' gestation and pregnancy was complicated by mild oligohydramnios. His immunizations are up-to-date. He is at the 35th percentile for length and 40th percentile for weight. His temperature is 39°C (102.2°F), pulse is 165/min, respirations are 60/min, and blood pressure is 55/30 mm Hg. Examination shows open anterior and posterior fontanelles. There is a midline lower abdominal mass extending 2–3 cm above the symphysis. Cardiopulmonary examination shows no abnormalities. The child is diagnosed with a urinary tract infection and broad spectrum antibiotic therapy is begun. This patient will most likely benefit the most from which of the following interventions?
A 2-year-old boy is brought to the physician by his parents for a well-child visit. During his last well-child visit 9 months ago, the patient had not begun talking. The parents report that their son frequently avoids eye contact and has no friends at daycare. He was born at term and has been healthy except for an episode of otitis media 6 months ago, which was treated with amoxicillin. His immunizations are up-to-date. He is at the 95 percentile for height, 20 percentile for weight, and 95 percentile for head circumference. He appears shy. His temperature is 37°C (98.6°F), pulse is 120/min, and blood pressure is 100/55 mm Hg. Examination shows elongated facial features and large ears. The patient does not speak. He does not follow instruction to build a stack of 2 blocks. Throughout the examination, he continually opens and closes his mother's purse and does not maintain eye contact. Which of the following findings is most likely to confirm the diagnosis?
A 14-year-old girl is brought to the physician because she frequently experiences cramping and pain in her legs during school sports. She is at the 10th percentile for height. Her blood pressure is 155/90 mm Hg. Examination shows a high-arched palate with maloccluded teeth and a low posterior hairline. The patient has a broad chest with widely spaced nipples. Pelvic examination shows normal external female genitalia with scant pubic hair. Without appropriate treatment, this patient is at the greatest risk of developing which of the following complications?
Practice by Chapter
Neural tube defects
Practice Questions
Congenital heart defects
Practice Questions
Gastrointestinal malformations
Practice Questions
Genitourinary anomalies
Practice Questions
Craniofacial anomalies
Practice Questions
Skeletal dysplasias
Practice Questions
Chromosomal disorders
Practice Questions
Teratogenic exposures
Practice Questions
Multiple malformation syndromes
Practice Questions
Prenatal diagnosis of congenital defects
Practice Questions
Surgical management timing
Practice Questions
Long-term outcomes and follow-up
Practice Questions
Preventive strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
