Congenital defects — MCQs

On this page
A pregnant woman gives birth to her 1st child at the family farm. After delivery, the assisting midwife notices a triangular defect in the lower anterior abdominal wall of the baby. She clamps the umbilical cord with a cloth and urges the family to seek immediate medical care at the nearest hospital. Upon admission, the attending pediatrician further notices an open bladder plate with an exposed urethra, a low set umbilicus, an anteriorly displaced anus, and an inguinal hernia. No omphalocele is noted. The external genitalia is also affected. On physical exam, a shortened penis with a pronounced upward curvature and the urethral opening along the dorsal surface are also noted. What is the most likely diagnosis?
A 2-week-old boy has developed bilious vomiting. He was born via cesarean section at term. On physical exam, his pulse is 140, blood pressure is 80/50 mmHg, and respirations are 40/min. His abdomen appears distended and appears diffusely tender to palpation. Abdominal imaging is obtained (Figures A). Which of the following describes the mechanism that caused this child's disorder?
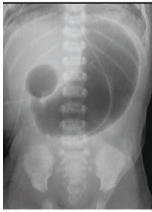
A 4-month-old girl is brought to the office by her parents because they noticed a mass protruding from her rectum and, she has been producing green colored emesis for the past 24 hours. Her parents noticed the mass when she had a bowel movement while changing her diaper. She strained to have this bowel movement 24 hours ago, shortly afterwards she had 3 episodes of greenish vomiting. She has a past medical history of failure to pass meconium for 2 days after birth. Her vital signs include: heart rate 190/min, respiratory rate 44/min, temperature 37.2°C (99.0°F), and blood pressure 80/50 mm Hg. On physical examination, the abdomen is distended. Examination of the anus reveals extrusion of the rectal mucosa through the external anal sphincter, and digital rectal examination produces an explosive expulsion of gas and stool. The abdominal radiograph shows bowel distention and absence of distal gas. What is the most likely cause?
A 3200-g (7.1-lb) female newborn is delivered at 38 weeks' gestation to a 24-year-old woman. The mother had regular prenatal visits throughout the pregnancy. The newborn's blood pressure is 53/35 mm Hg. Examination in the delivery room shows clitoromegaly and posterior labial fusion. One day later, serum studies show: Na+ 131 mEq/L K+ 5.4 mEq/L Cl− 102 mEq/L Urea nitrogen 15 mg/dL Creatinine 0.8 mg/dL Ultrasound of the abdomen and pelvis shows a normal uterus and ovaries. Further evaluation of the newborn is most likely to show which of the following findings?
A 4-year-old Caucasian male suffers from cyanosis and dyspnea relieved by squatting. Which of the following abnormalities is most likely present?
A 4-day-old male infant is brought to the physician because of respiratory distress and bluish discoloration of his lips and tongue. He was born at term and the antenatal period was uncomplicated. His temperature is 37.3°C (99.1°F), pulse is 170/min, respirations are 65/min, and blood pressure is 70/46 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 82%. A grade 3/6 holosystolic murmur is heard over the left lower sternal border. A single S2 that does not split with respiration is present. Echocardiography shows defects in the interatrial and interventricular septae, as well as an imperforate muscular septum between the right atrium and right ventricle. Further evaluation of this patient is most likely to show which of the following?
A 7-month-old boy is brought to the physician for a well-child examination. He was born at 36 weeks' gestation and has been healthy since. He is at the 60th percentile for length and weight. Vital signs are within normal limits. The abdomen is soft and nontender. The external genitalia appear normal. Examination shows a single palpable testicle in the right hemiscrotum. The scrotum is nontender and not enlarged. There is a palpable mass in the left inguinal canal. Which of the following is the most appropriate next best step in management?
A 2600-g (5-lb 8-oz) male newborn is delivered at 34 weeks' gestation to a 22-year-old woman. The mother did not have prenatal care. Upon examination in the delivery room, the newborn's skin appears blue. He is gasping and breathing irregularly. The ears are low-set with broad auricles, and the nasal tip is flattened. The lower jaw is small and displaced backward. The right foot is clubbed. Which of the following is the most likely underlying cause of this patient's condition?
A newborn male is evaluated 30 minutes after birth. He was born at 38 weeks gestation to a 39-year-old gravida 3 via vaginal delivery. The pregnancy was complicated by gestational diabetes, and the patient’s mother received routine prenatal care. The family declined all prenatal testing, including an anatomy ultrasound. The patient’s two older siblings are both healthy. Upon delivery, the patient appeared well and had good respiratory effort. He was noted to have acrocyanosis, and his Apgar scores were 8 and 9 at one and five minutes of life, respectively. The patient’s birth weight is 3840 g (8 lb 7 oz). His temperature is 98.7°F (37.1°C), blood pressure is 66/37 mmHg, pulse is 142/min, and respirations are 34/min. On physical exam, the patient has low-set ears, upslanting palpebral fissures, and a hypoplastic fifth finger. Which of the following is most likely to be found in this patient?
A 3175-g (7-lb) female newborn is delivered at 37 weeks to a 26-year-old primigravid woman. Apgar scores are 8 and 9 at 1 and 5 minutes, respectively. The pregnancy had been uncomplicated. The mother had no prenatal care. She immigrated to the US from Brazil 2 years ago. Immunization records are not available. One day after delivery, the newborn's temperature is 37.5°C (99.5°F), pulse is 182/min, respirations are 60/min, and blood pressure is 82/60 mm Hg. The lungs are clear to auscultation. Cardiac examination shows a continuous heart murmur. The abdomen is soft and nontender. There are several discolored areas on the skin that are non-blanchable upon pressure application. Slit lamp examination shows cloudy lenses in both eyes. The newborn does not pass her auditory screening tests. Which of the following is the most likely diagnosis?
Practice by Chapter
Neural tube defects
Practice Questions
Congenital heart defects
Practice Questions
Gastrointestinal malformations
Practice Questions
Genitourinary anomalies
Practice Questions
Craniofacial anomalies
Practice Questions
Skeletal dysplasias
Practice Questions
Chromosomal disorders
Practice Questions
Teratogenic exposures
Practice Questions
Multiple malformation syndromes
Practice Questions
Prenatal diagnosis of congenital defects
Practice Questions
Surgical management timing
Practice Questions
Long-term outcomes and follow-up
Practice Questions
Preventive strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
