Gastrointestinal malformations — MCQs

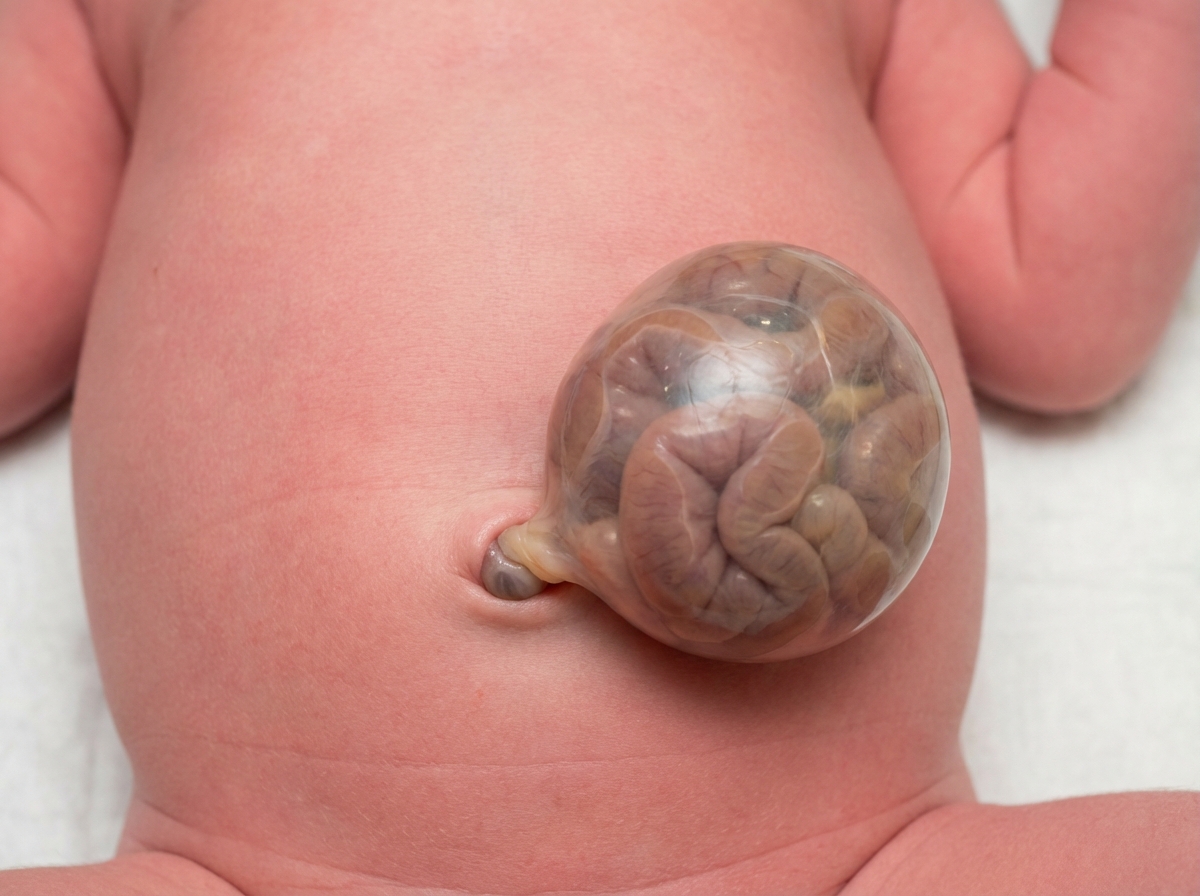
A 42-year-old woman presents to the emergency department in active labor. She has had no prenatal care and is unsure of the gestational age. Labor progresses rapidly and spontaneous vaginal delivery of a baby boy occurs 3 hours after presentation. On initial exam, the child is 1.9 kg (4.2 lb) with a small head and jaw. A sac-like structure containing intestine, as can be seen in the picture, protrudes from the abdominal wall. What complication is closely associated with this presentation?
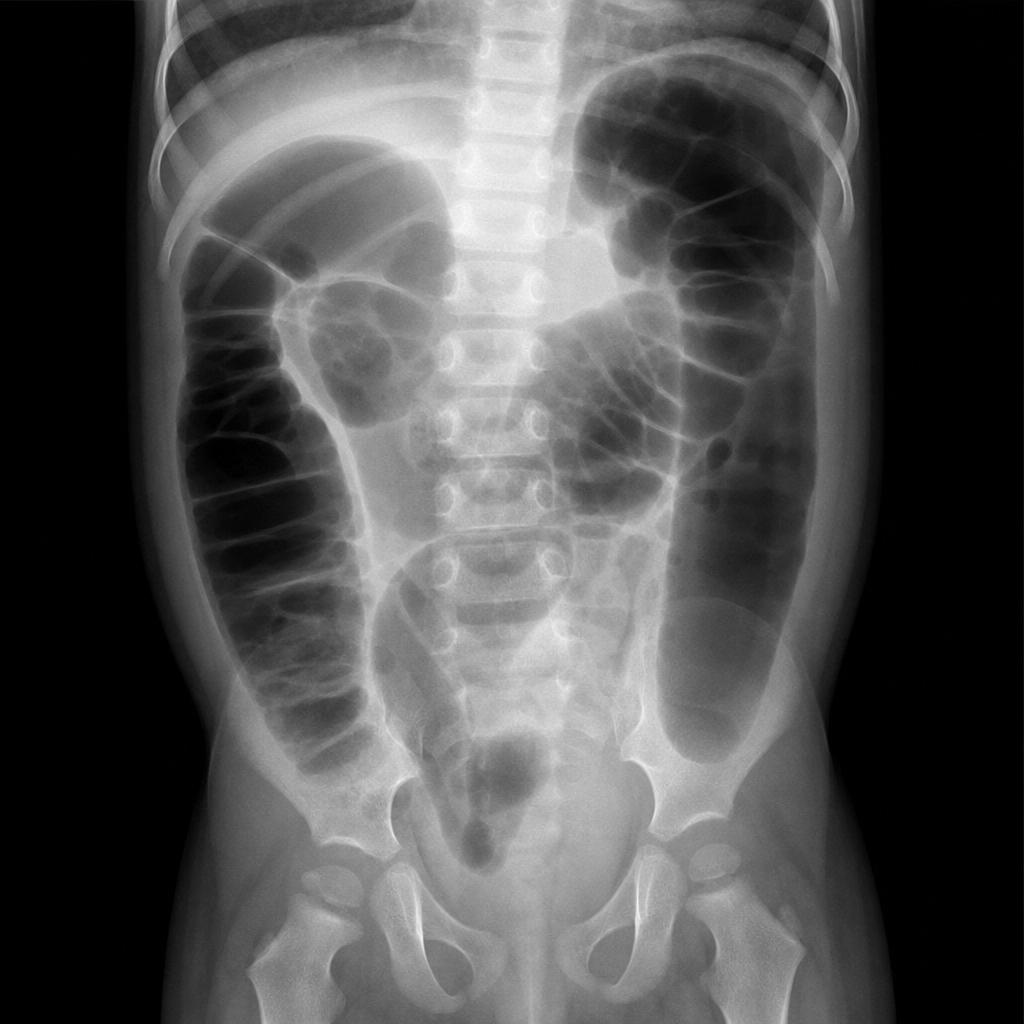
A 5-year-old boy with Down syndrome presents with his mother. The patient’s mother says that he isn’t playing or eating as much as he used to and seems lethargic. Expected developmental delays are present and stable. Physical examination reveals dry mucous membranes and abdominal distention with no tenderness to palpation. An abdominal radiograph is shown in the image below. Which of the following is the most likely diagnosis in this patient?
A new mother expresses her concerns because her 1-day-old newborn has been having feeding difficulties. The child vomits after every feeding and has had a continuous cough since shortly after birth. The mother denies any greenish coloration of the vomit and says that it is only composed of whitish milk that the baby just had. The child exhibits these coughing spells during the exam, at which time the physician notices the child’s skin becoming cyanotic. The mother states that the child was born vaginally with no complications, although her records show that she had polyhydramnios during her last ultrasound before the delivery. Which of the following is the most likely cause of the patient’s symptoms?
A 5-week-old male infant is brought to the physician by his mother because of a 4-day history of recurrent nonbilious vomiting after feeding. He was born at 36 weeks' gestation via spontaneous vaginal delivery. Vital signs are within normal limits. Physical examination shows a 2-cm epigastric mass. Further diagnostic evaluation of this patient is most likely to show which of the following?
A 45-year-old woman comes to the office with a 2-week history of rectal bleeding that occurs every day with her bowel movements. She denies any pain during defecation. Apart from this, she does not have any other complaints. Her past medical history is insignificant except for 5 normal vaginal deliveries. Her vitals are a heart rate of 72/min, a respiratory rate of 15/min, a temperature of 36.7°C (98.1°F), and a blood pressure of 115/85 mm Hg. On rectovaginal examination, there is a palpable, non-tender, prolapsed mass that can be pushed back by the examiner's finger into the anal sphincter. What is the most likely diagnosis?
A 3-week-old firstborn baby girl is brought to the pediatric emergency room with projectile vomiting. She started vomiting while feeding 12 hours ago and has been unable to keep anything down since then. After vomiting, she appears well and hungry, attempting to feed again. The vomitus has been non-bloody and non-bilious. The last wet diaper was 10 hours ago. The child was born at 40 weeks gestation to a healthy mother. On examination, the child appears sleepy but has a healthy cry during the exam. The child has dry mucous membranes and delayed capillary refill. There is a palpable olive-shaped epigastric mass on palpation. Which of the following is the most likely cause of this patient's condition?
A 2-week-old boy has developed bilious vomiting. He was born via cesarean section at term. On physical exam, his pulse is 140, blood pressure is 80/50 mmHg, and respirations are 40/min. His abdomen appears distended and appears diffusely tender to palpation. Abdominal imaging is obtained (Figures A). Which of the following describes the mechanism that caused this child's disorder?
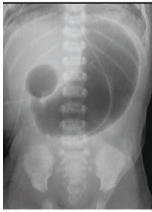
A newborn boy born vaginally to a healthy 37-year-old G3P1 from a pregnancy complicated by hydramnios fails to pass meconium after 24 hours of life. The vital signs are within normal limits for his age. The abdomen is distended, the anus is patent, and the rectal examination reveals pale mucous with non-pigmented meconium. Based on a barium enema, the boy is diagnosed with sigmoid colonic atresia. Disruption of which structure during fetal development could lead to this anomaly?
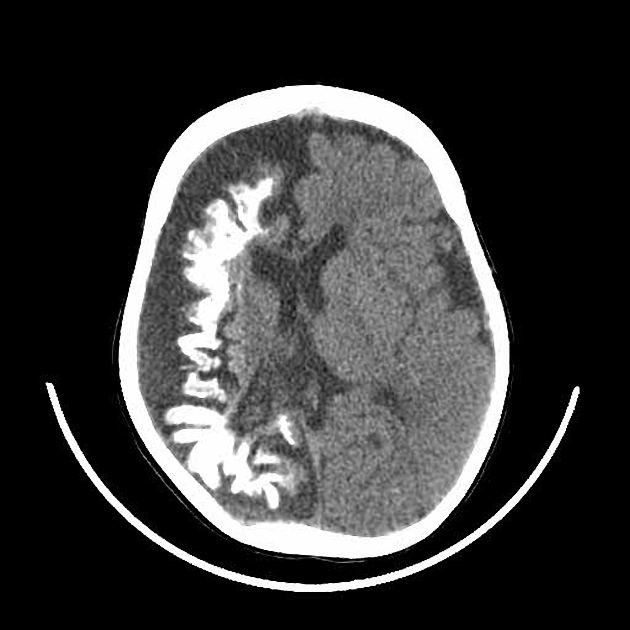
A 10-year-old boy is brought to a family physician by his mother with a history of recurrent headaches. The headaches are moderate-to-severe in intensity, unilateral, mostly affecting the left side, and pulsatile in nature. Past medical history is significant for mild intellectual disability and complex partial seizures that sometimes progress to secondary generalized seizures. He was adopted at the age of 7 days. His birth history and family history are not available. His developmental milestones were slightly delayed. There is no history of fever or head trauma. His vital signs are within normal limits. His height and weight are at the 67th and 54th percentile for his age. Physical examination reveals an area of bluish discoloration on his left eyelid and cheek. The rest of the examination is within normal limits. A computed tomography (CT) scan of his head is shown in the exhibit. Which of the following additional clinical findings is most likely to be present?
A 26-year-old G1P0 mother is in the delivery room in labor. Her unborn fetus is known to have a patent urachus. Which of the following abnormalities would you expect to observe in the infant?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
