Congenital defects — MCQs

On this page
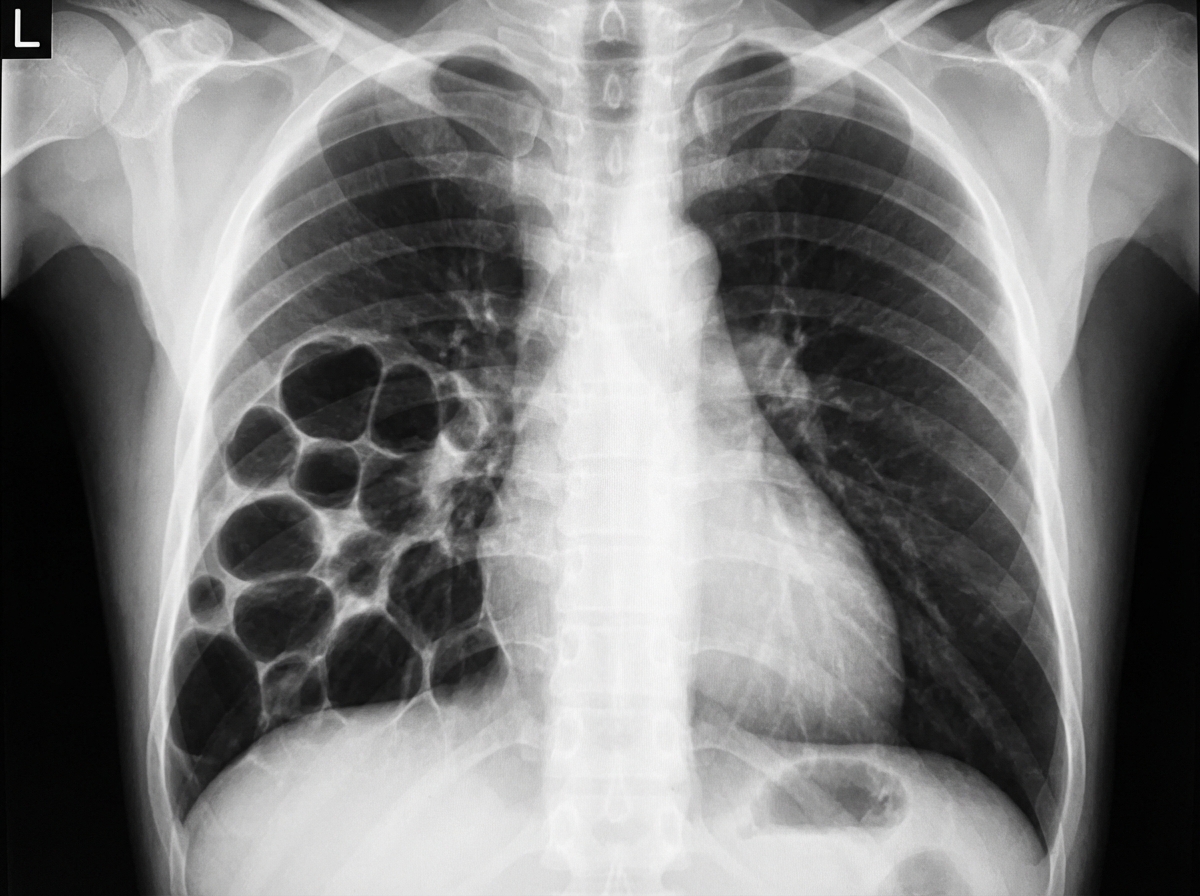
A 3-year-old child presents with respiratory distress and a history of recurrent respiratory infections. Based on the provided imaging, what is the most likely diagnosis?
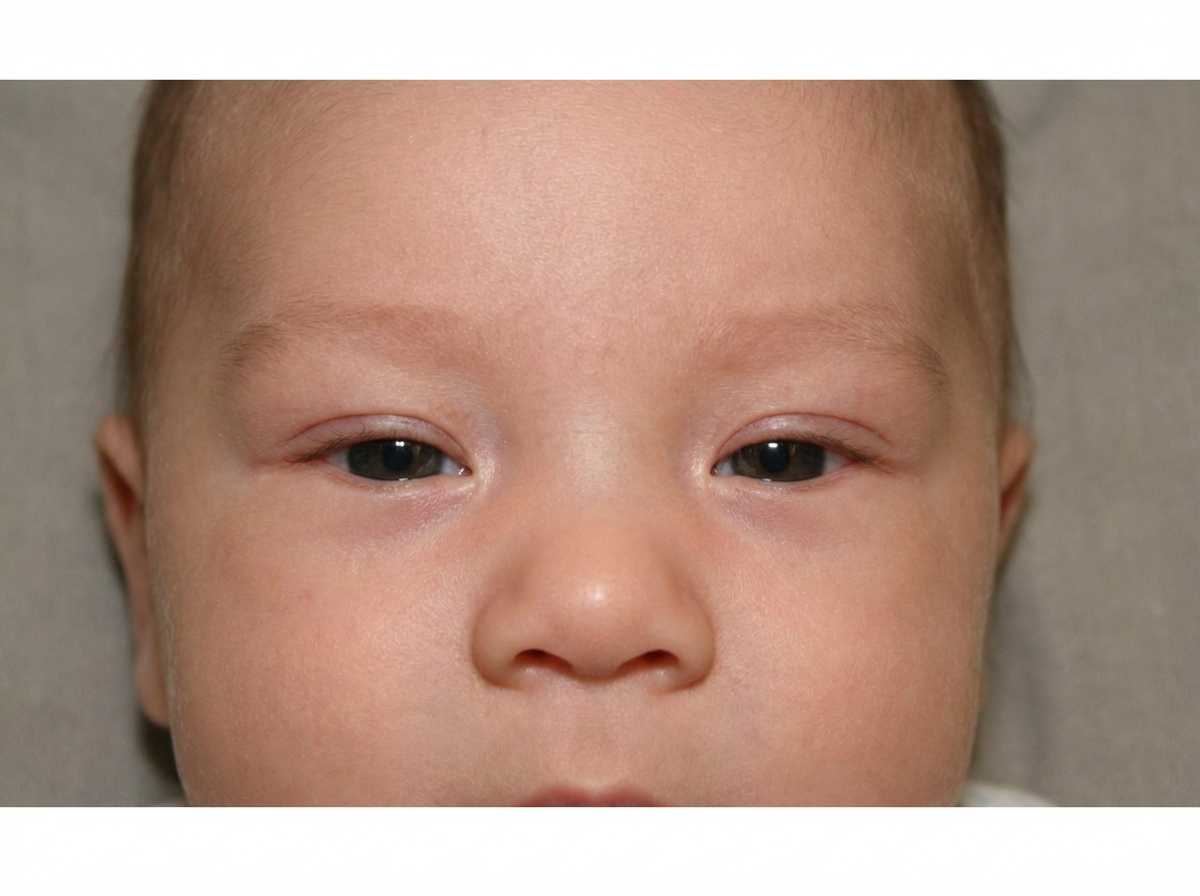
A 2 -month-old child presents with the following condition as shown in the image. What is the ideal management protocol?
A 13-year-old boy presents with jaundice, fatigue, muscle stiffness, tremors, and behavioral changes. Examination reveals an enlarged liver and spleen. A Kayser-Fleischer ring was noted. What is the definitive diagnostic test?
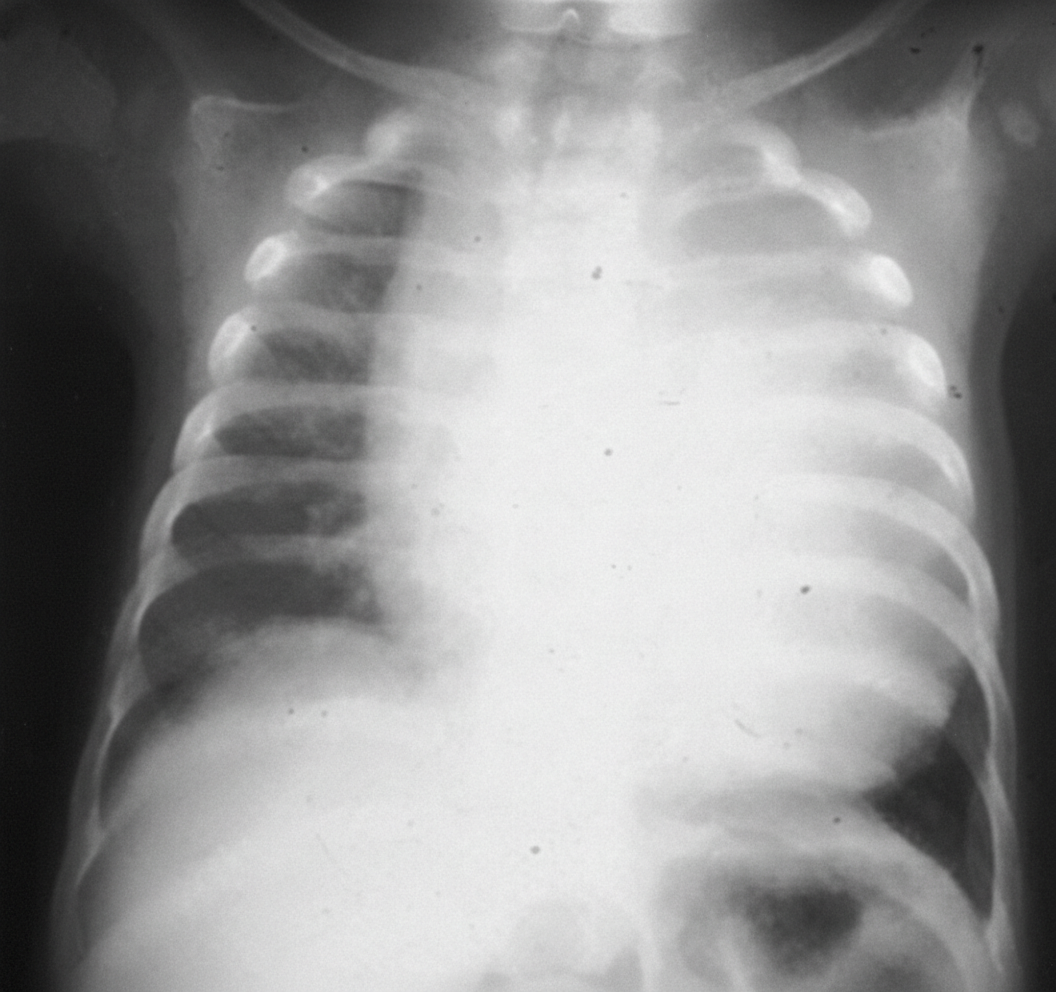
A patient presents with an X-ray showing cardiomegaly, along with symptoms of hypotonia, macroglossia, hepatomegaly, and floppy baby syndrome. The X ray of the infant is shown below. What is the most likely diagnosis?
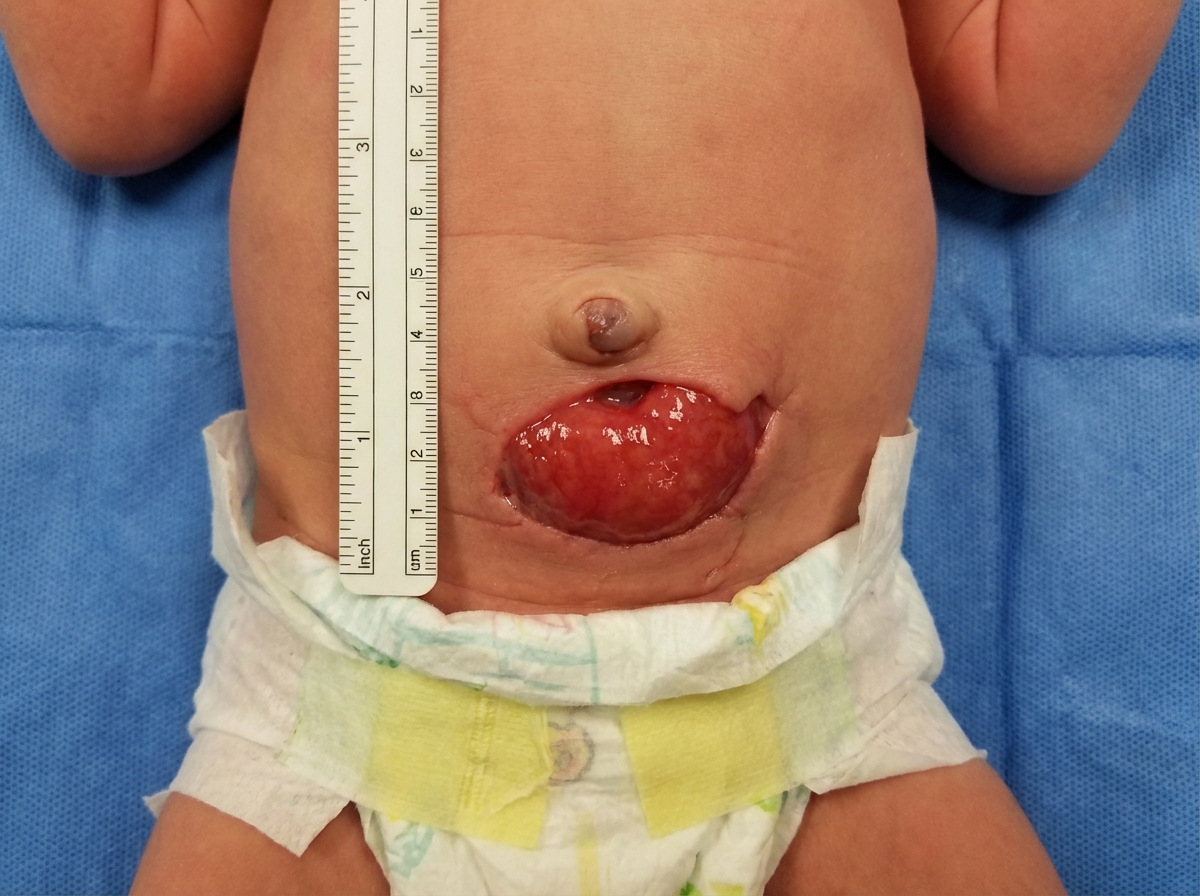
What is the diagnosis based on the image shown 
A 6-week-old baby is brought in by the mother with complaints of vomiting. An X-ray shows a single bubble appearance. What is the most likely diagnosis?
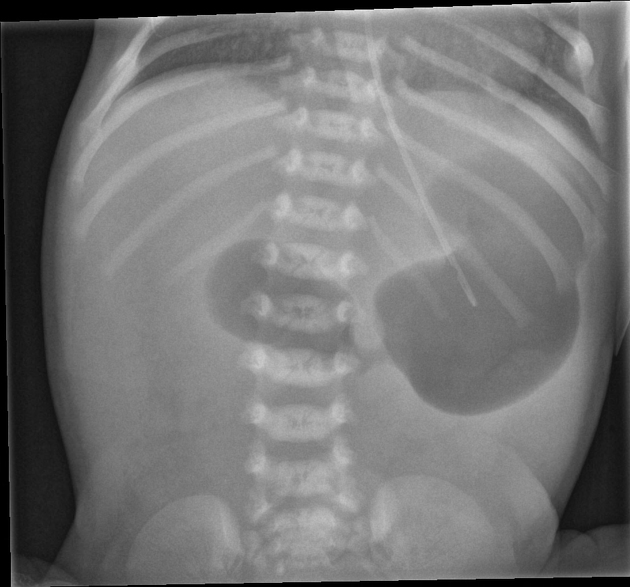
A 3-year-old child presents to the OPD with a history of recurrent urinary tract infections, poor urinary stream, and difficulty voiding. The radiological image is shown below. What is the most appropriate management?
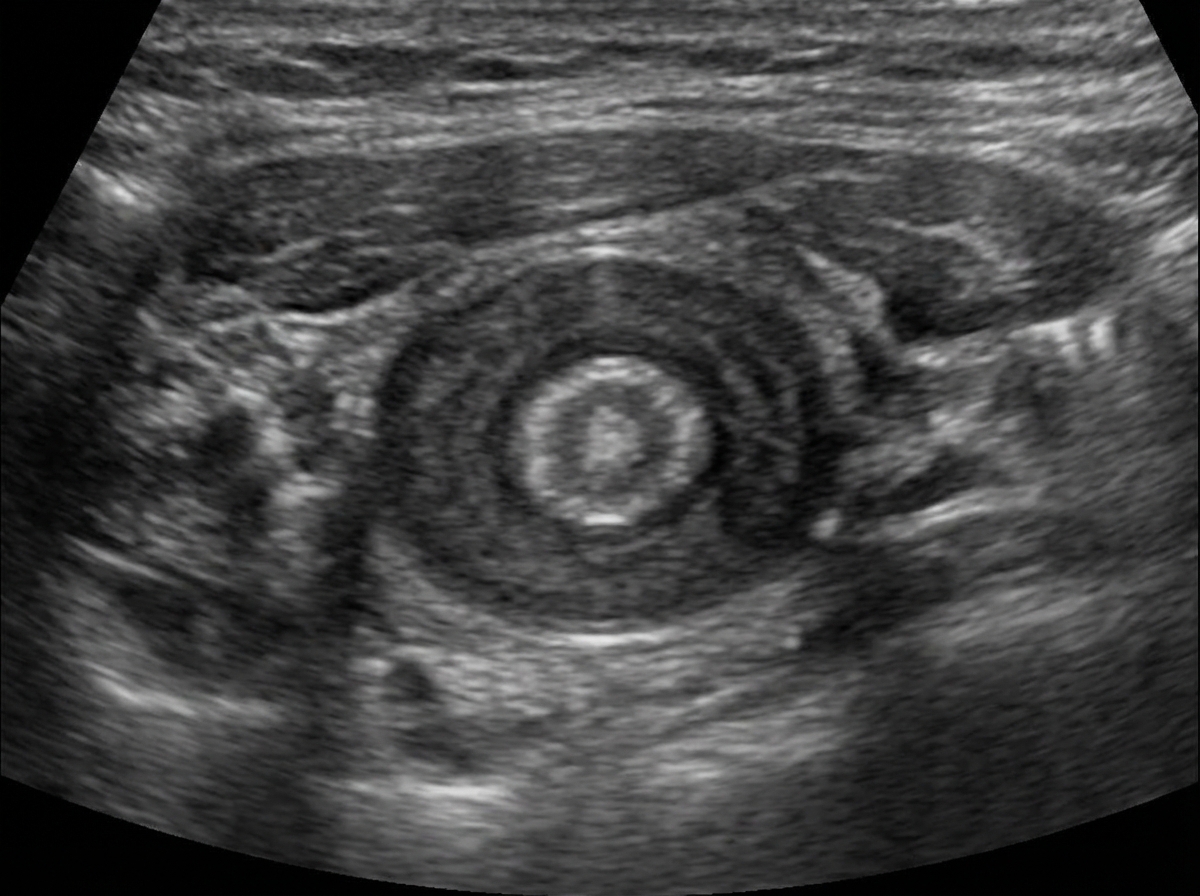
A 6-week-old child with a history of vomiting undergoes an ultrasound, which shows an antral nipple sign or target sign, as shown in the image. What is the diagnosis?
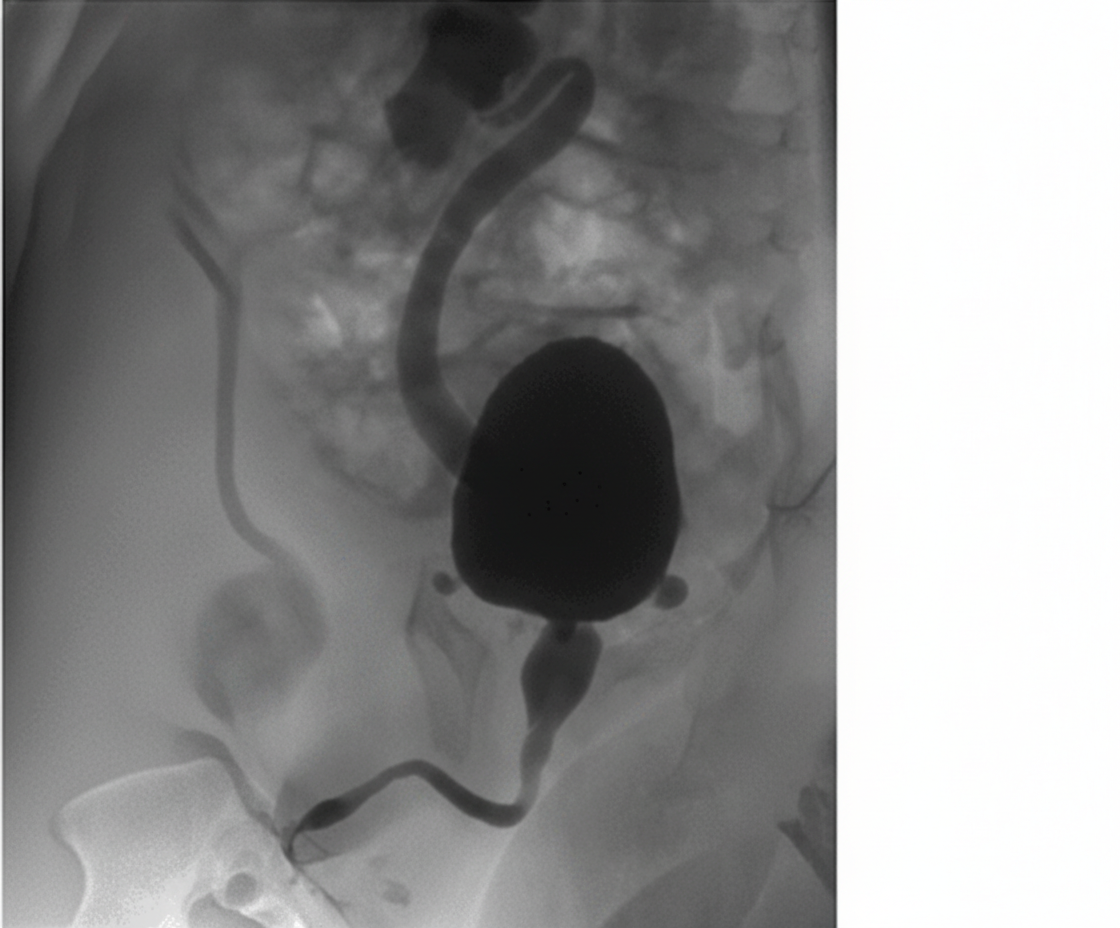
A 2-year-old boy presents with a history of recurrent urinary tract infections, poor urinary stream, and failure to thrive. A voiding cystourethrogram (VCUG) is performed, and the images provided show dilated posterior urethra and a thickened bladder wall with a keyhole appearance. Based on these findings, the diagnosis of posterior urethral valves (PUV) is made. What is the management for this condition?
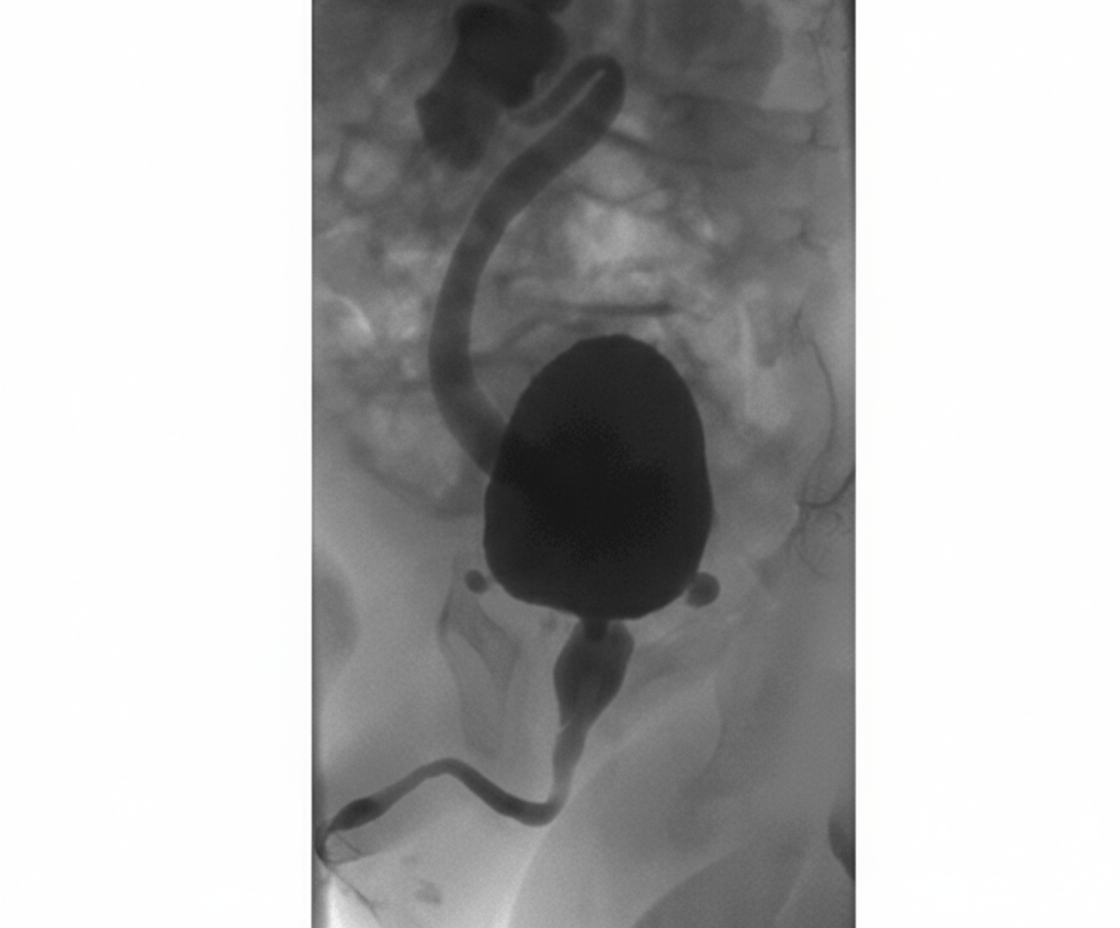
A child presents with a webbed neck, short stature, and a low posterior hairline. What is the most likely diagnosis?
Practice by Chapter
Neural tube defects
Practice Questions
Congenital heart defects
Practice Questions
Gastrointestinal malformations
Practice Questions
Genitourinary anomalies
Practice Questions
Craniofacial anomalies
Practice Questions
Skeletal dysplasias
Practice Questions
Chromosomal disorders
Practice Questions
Teratogenic exposures
Practice Questions
Multiple malformation syndromes
Practice Questions
Prenatal diagnosis of congenital defects
Practice Questions
Surgical management timing
Practice Questions
Long-term outcomes and follow-up
Practice Questions
Preventive strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
