Renal pathology — MCQs

On this page
Comment on type of glomerulonephritis present in the kidney biopsy slide. (Recent NEET Pattern 2016-17)
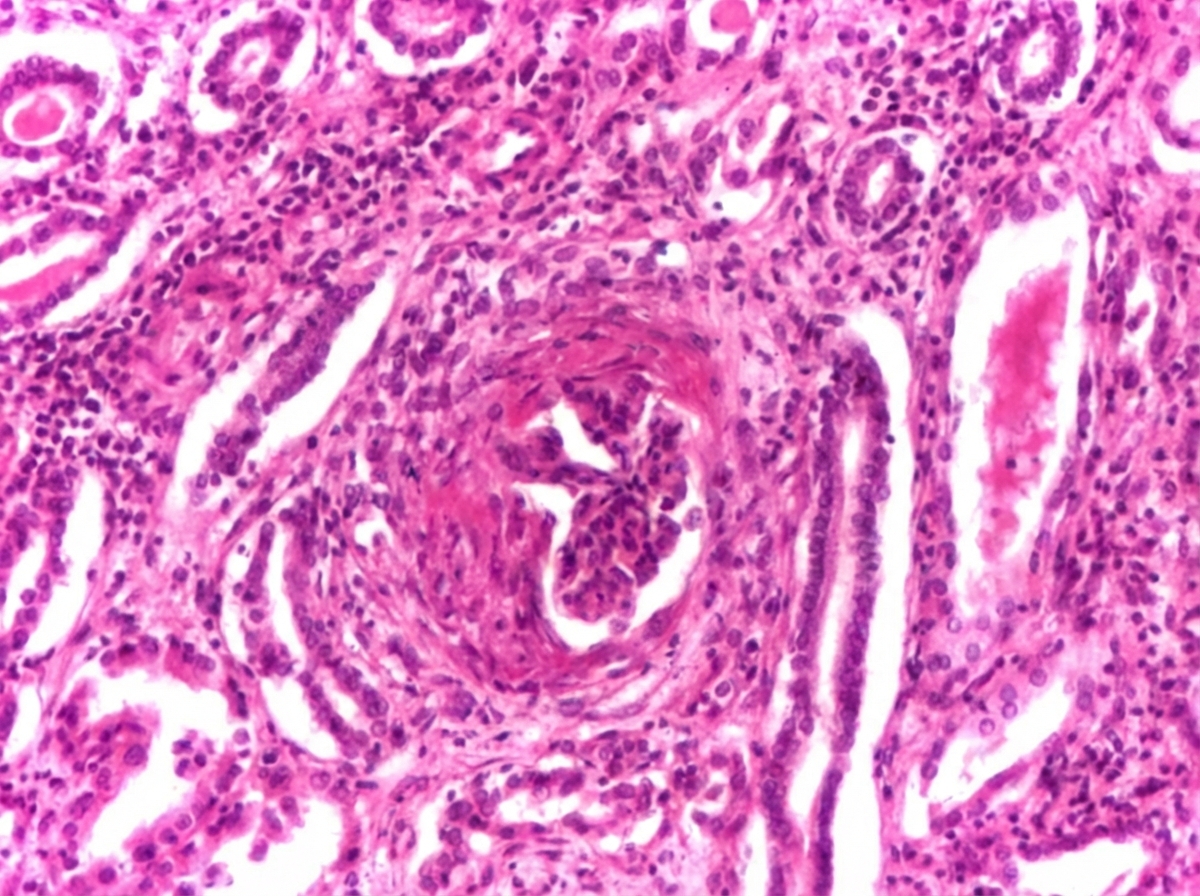
The image shows:
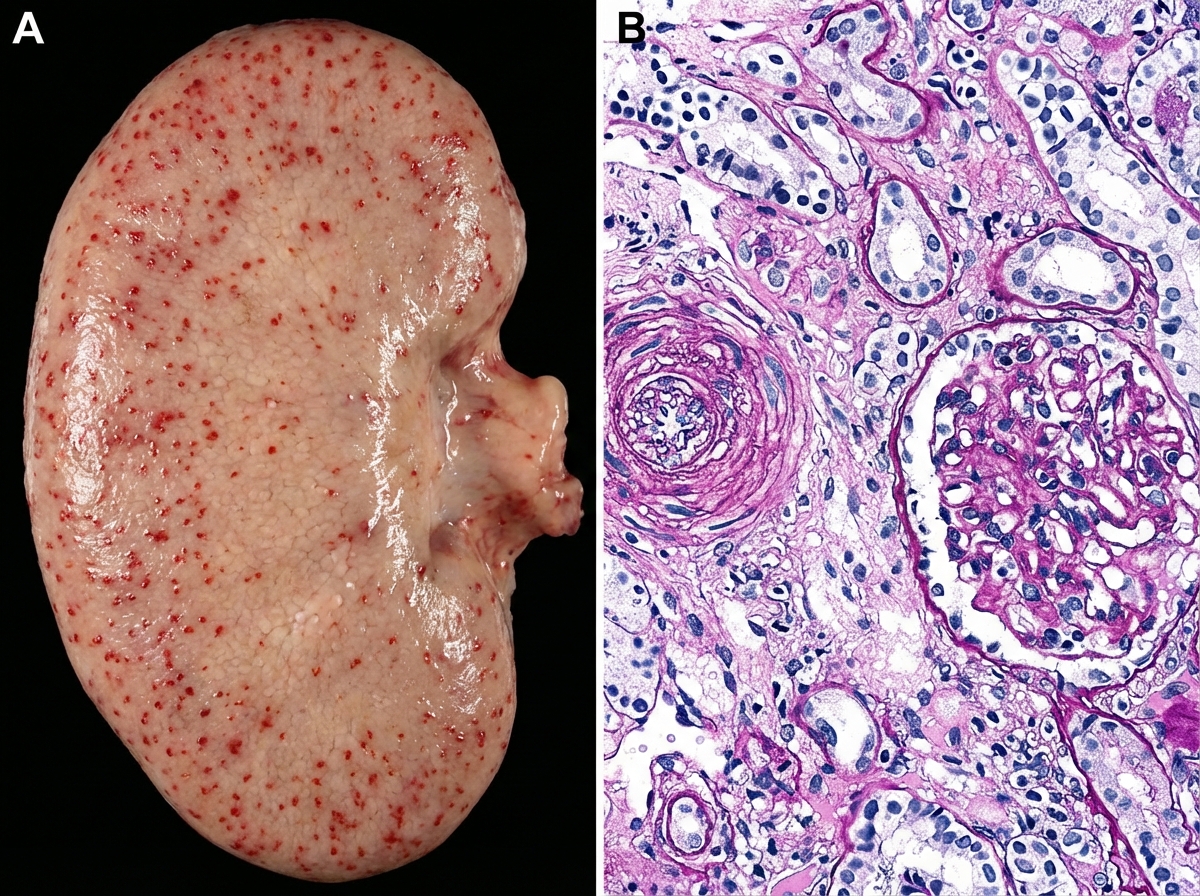
Kidney specimen of 40 -year-old man is shown below. All are true about the condition shown in the figure except:
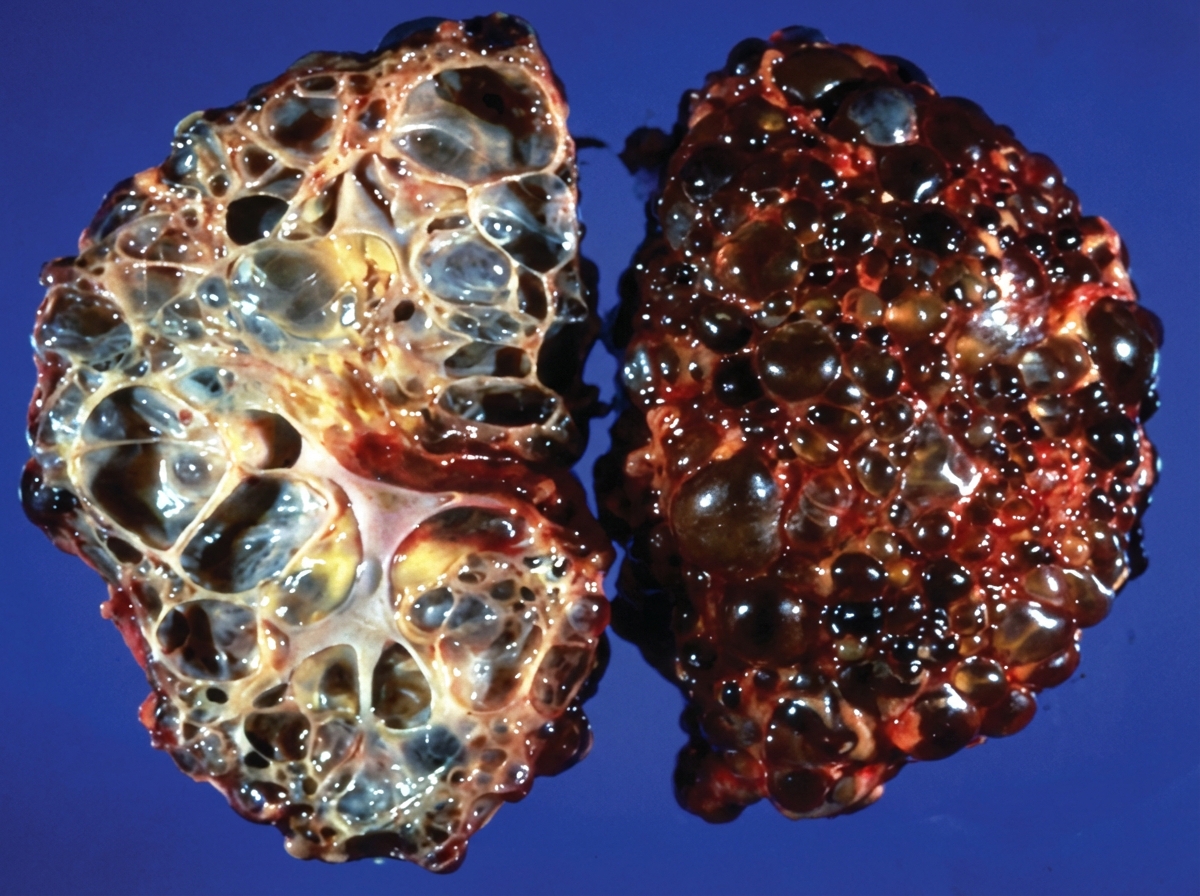
The image shows presence of:
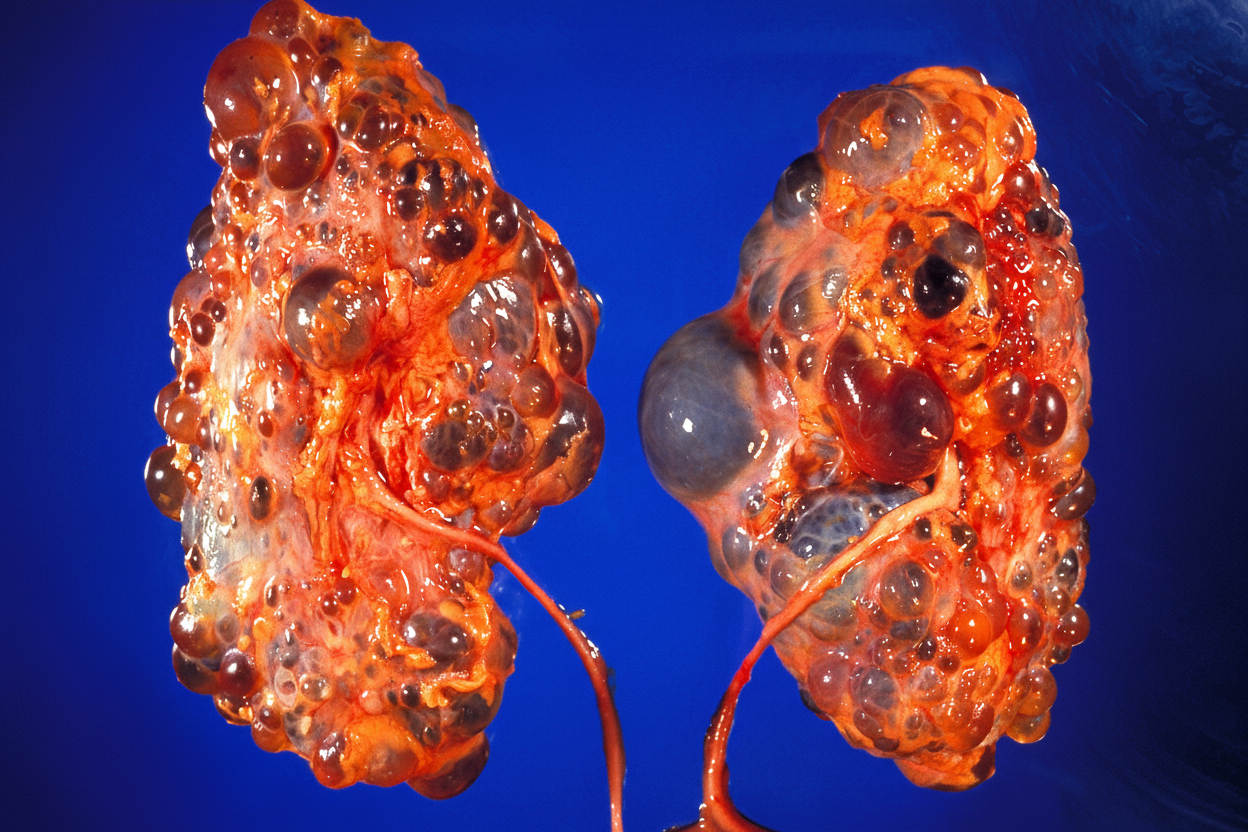
The kidneys shown in this image are from a 24 -yearold man. What would have been the most likely cause of his death?
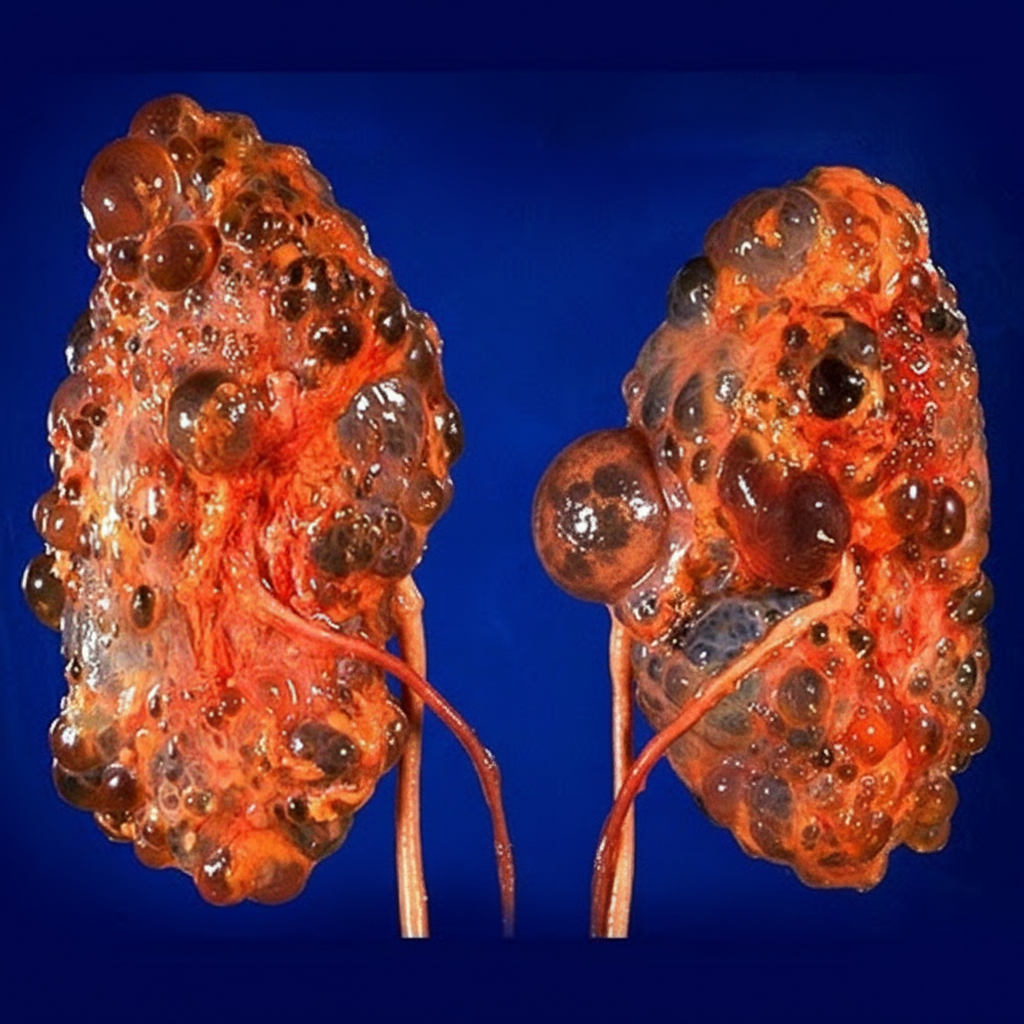
A 28-year-old female with history of urinary tract infection presents with flank pain. On surgical extraction of the kidney, patient's presentation is similar to that given in the image. What is the likely diagnosis?
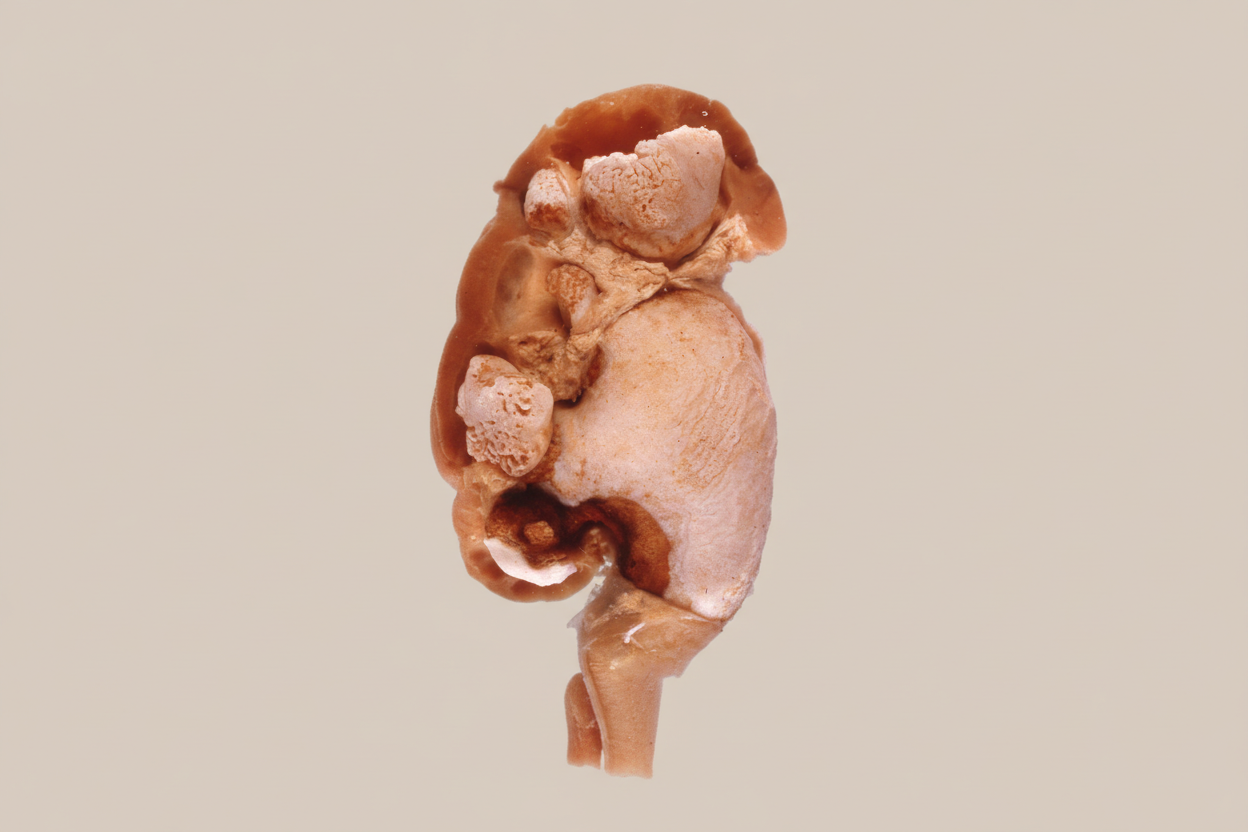
A 58-year-old diabetic patient presents with frothiness in the urine. Which of the following is the diagnosis?
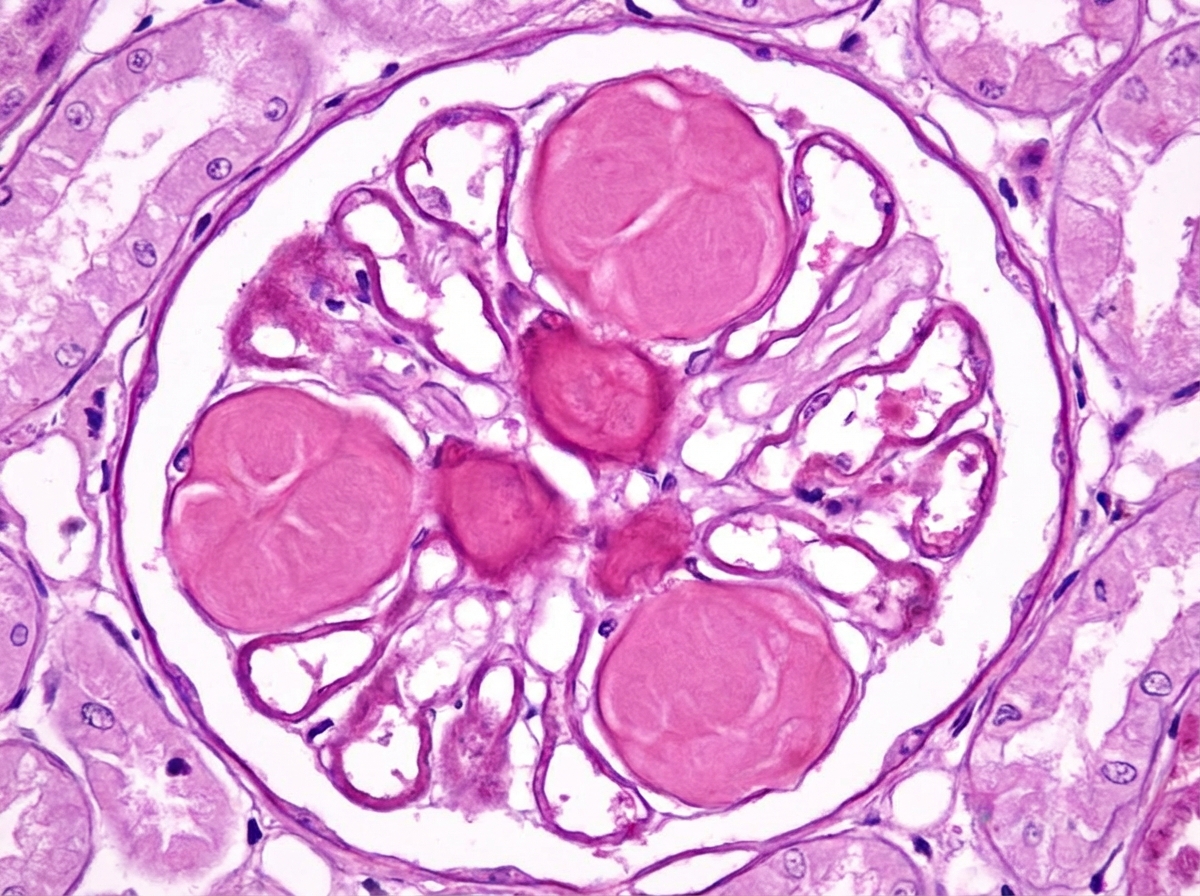
Which urine crystals are shown in the figure below?

The resected specimen of a kidney is seen below. What is the diagnosis?
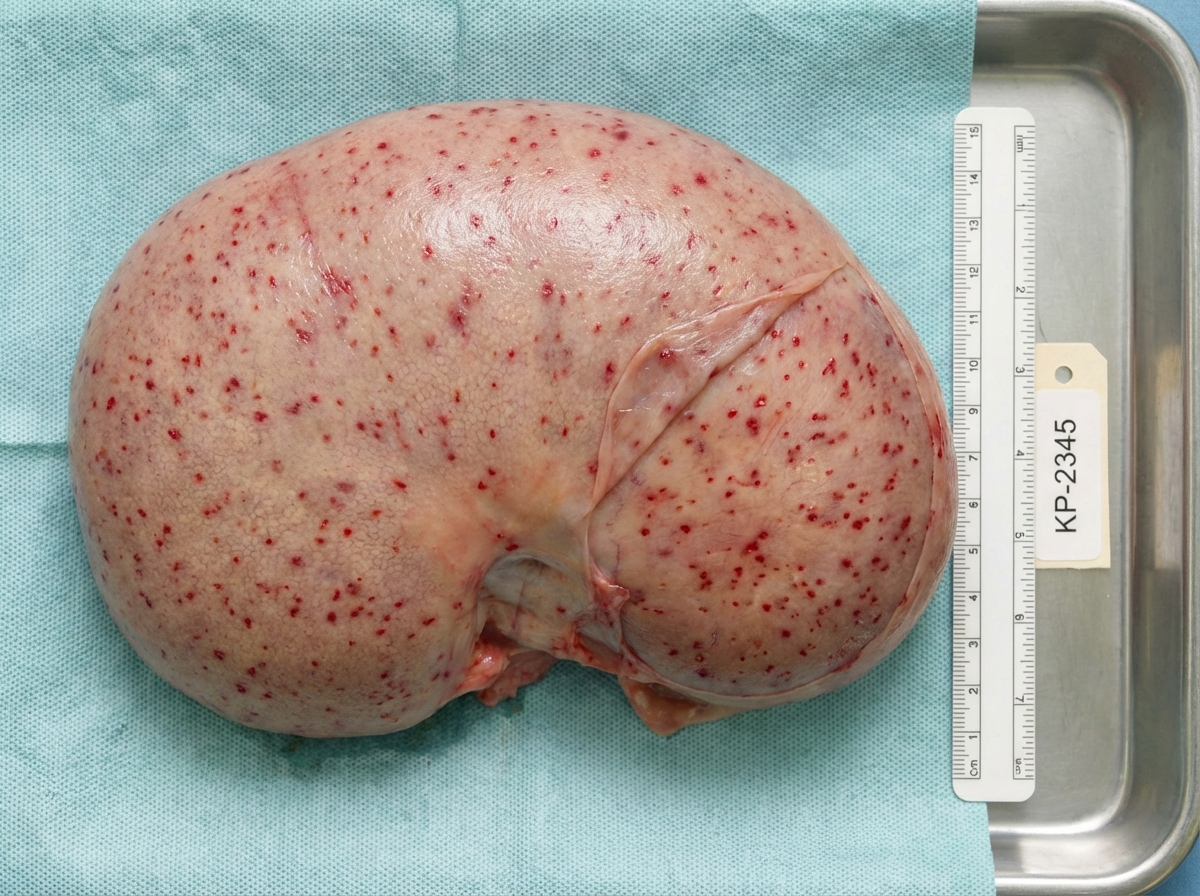
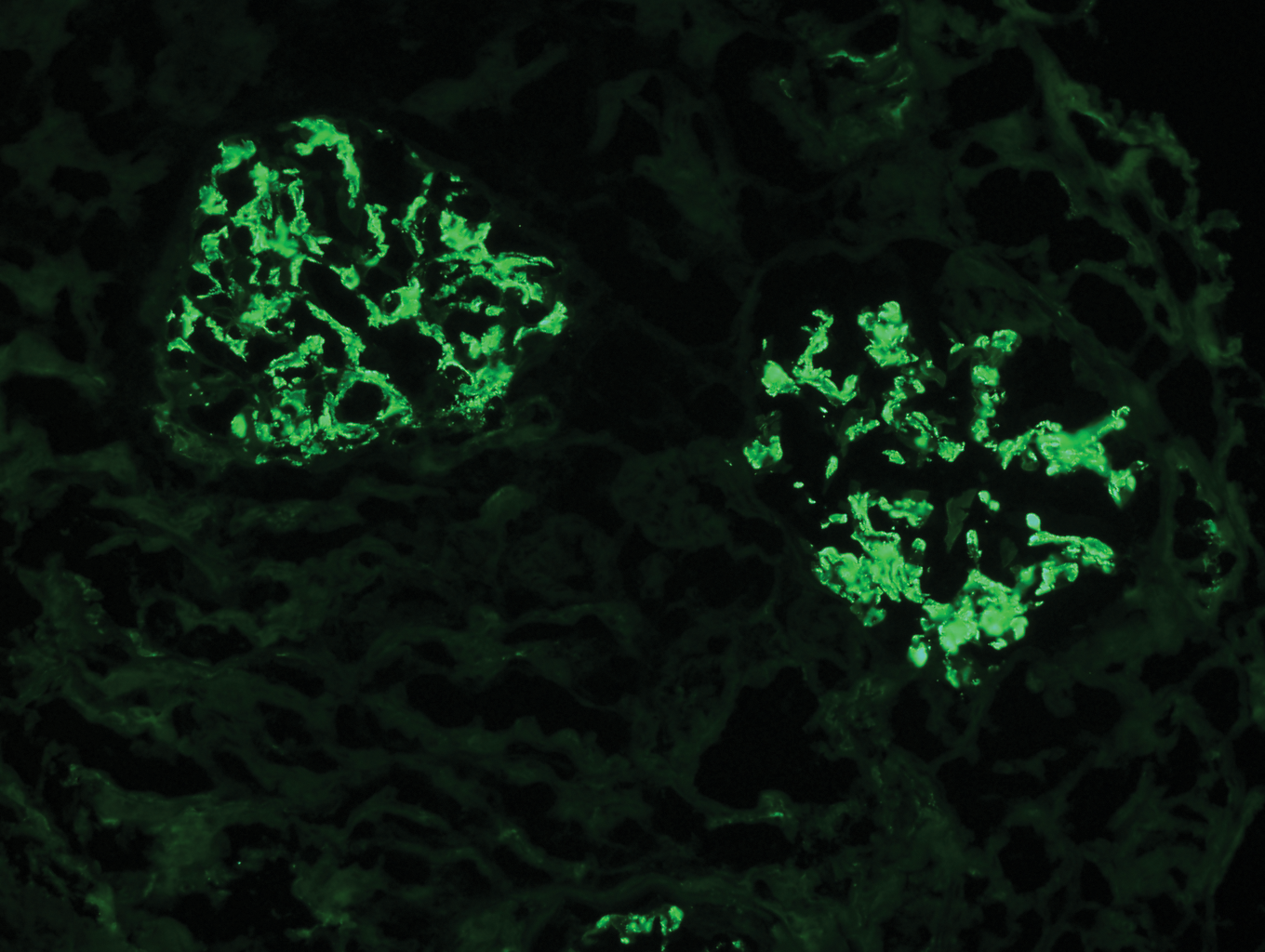
The following is the FITC for IgG stained kidney specimen. What is this suggestive of?
Practice by Chapter
Congenital renal anomalies
Practice Questions
Glomerular diseases overview
Practice Questions
Nephritic syndrome disorders
Practice Questions
Nephrotic syndrome disorders
Practice Questions
Rapidly progressive glomerulonephritis
Practice Questions
Tubulointerstitial diseases
Practice Questions
Acute tubular necrosis
Practice Questions
Renal vascular diseases
Practice Questions
Pyelonephritis and urinary tract infections
Practice Questions
Renal cystic diseases
Practice Questions
Obstructive uropathies
Practice Questions
Renal tumors
Practice Questions
Kidney transplant pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
