Renal pathology — MCQs

On this page
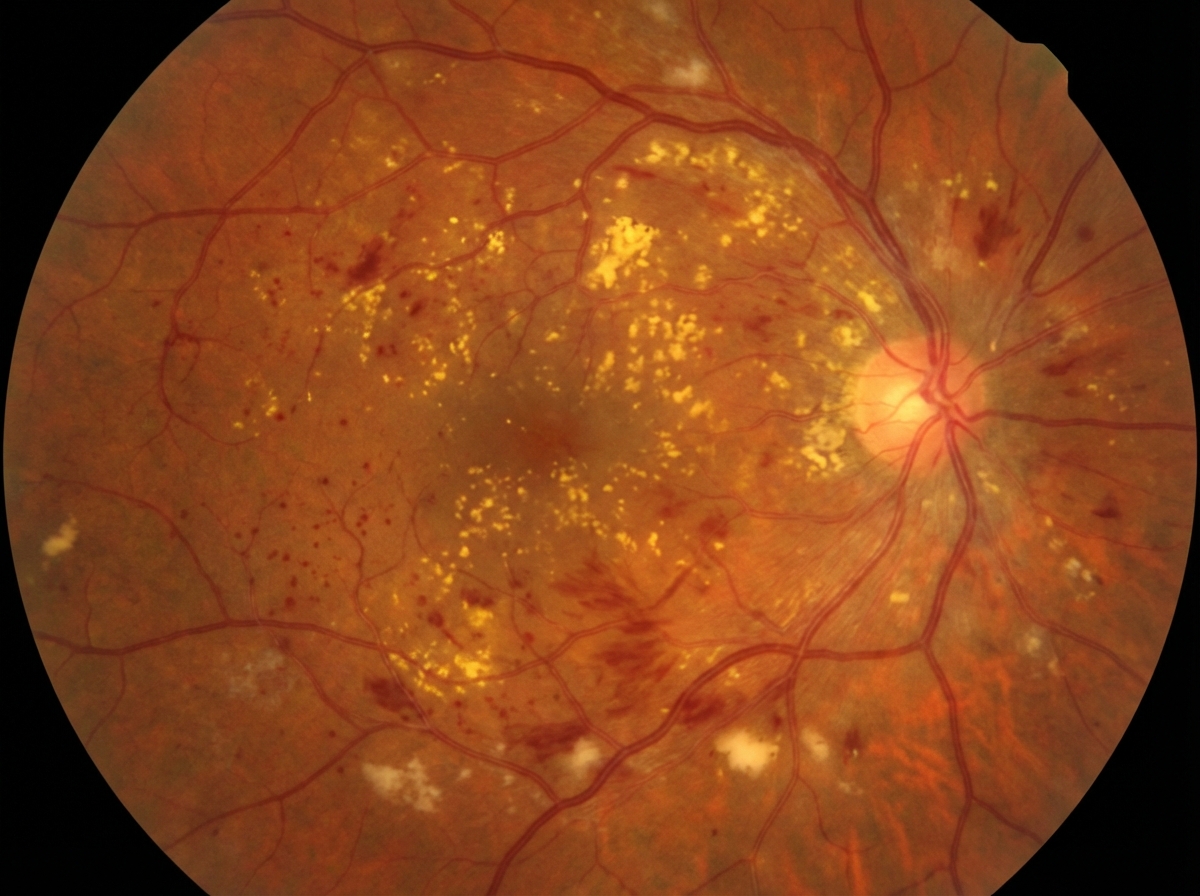
A 58-year-old woman with HbA1c of 10 % is referred to an ophthalmologist because of vision loss. An image of her retina is shown below, If this patient were to undergo renal biopsy, what will be the pathologic findings?
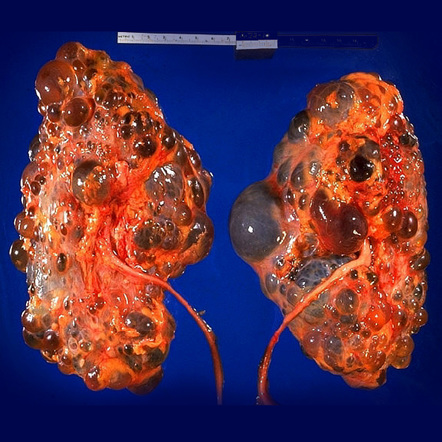
All are true about the condition shown except:
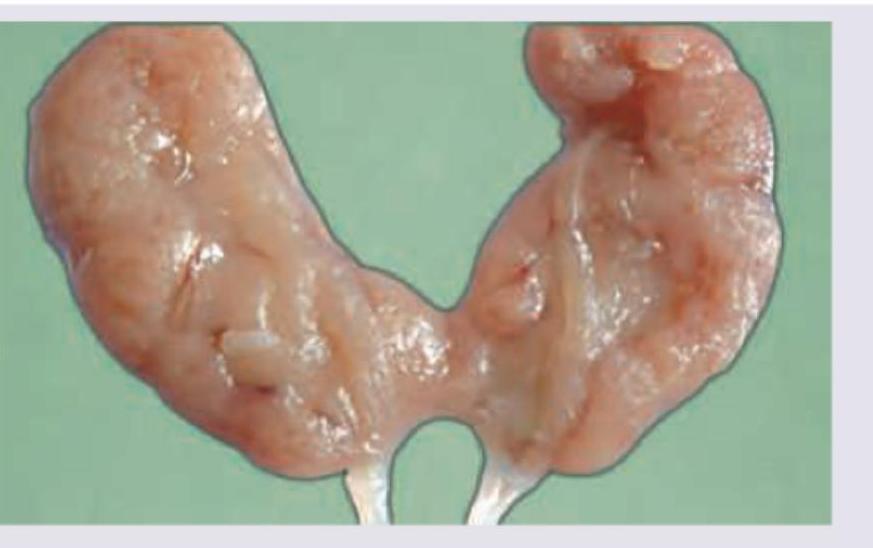
Which is not a true statement about this anomaly of kidney?
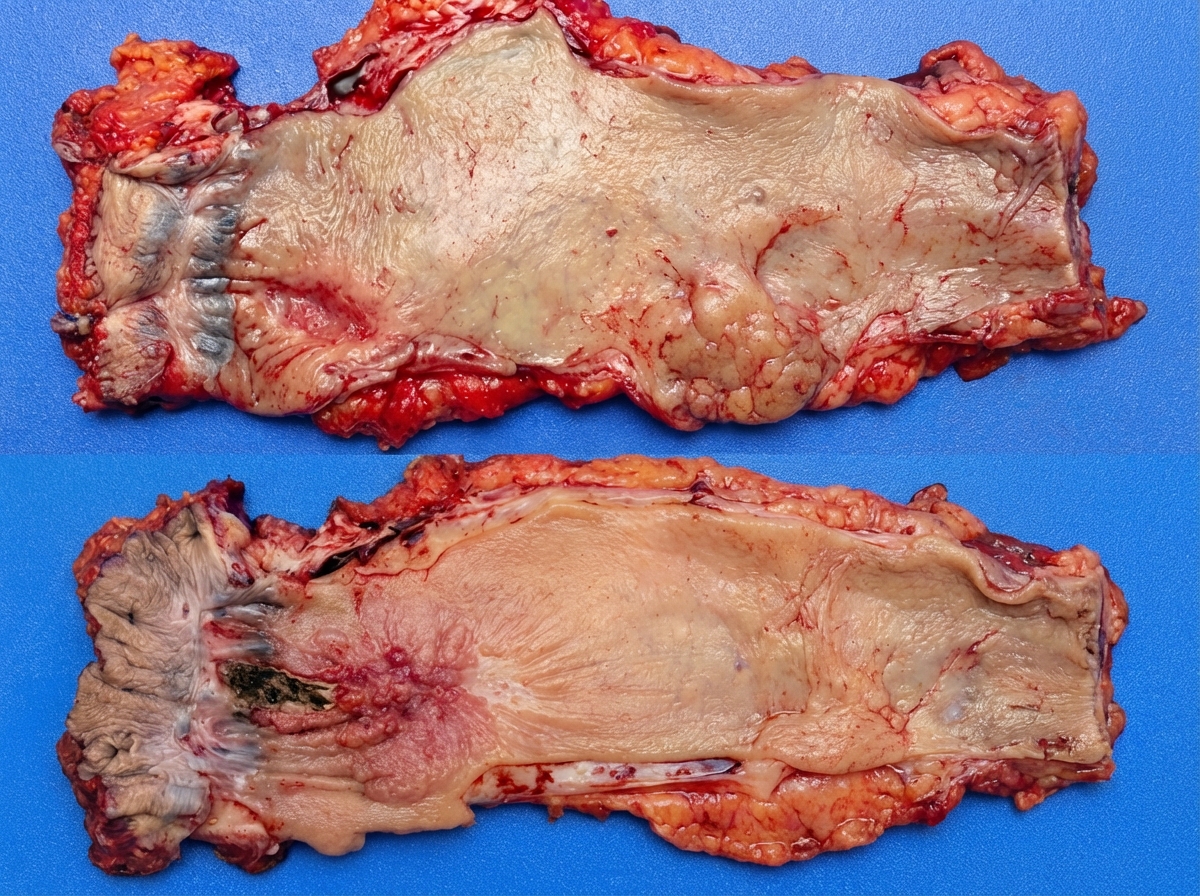
All are correct about the condition shown in the image except: (NEET Pattern 2018)
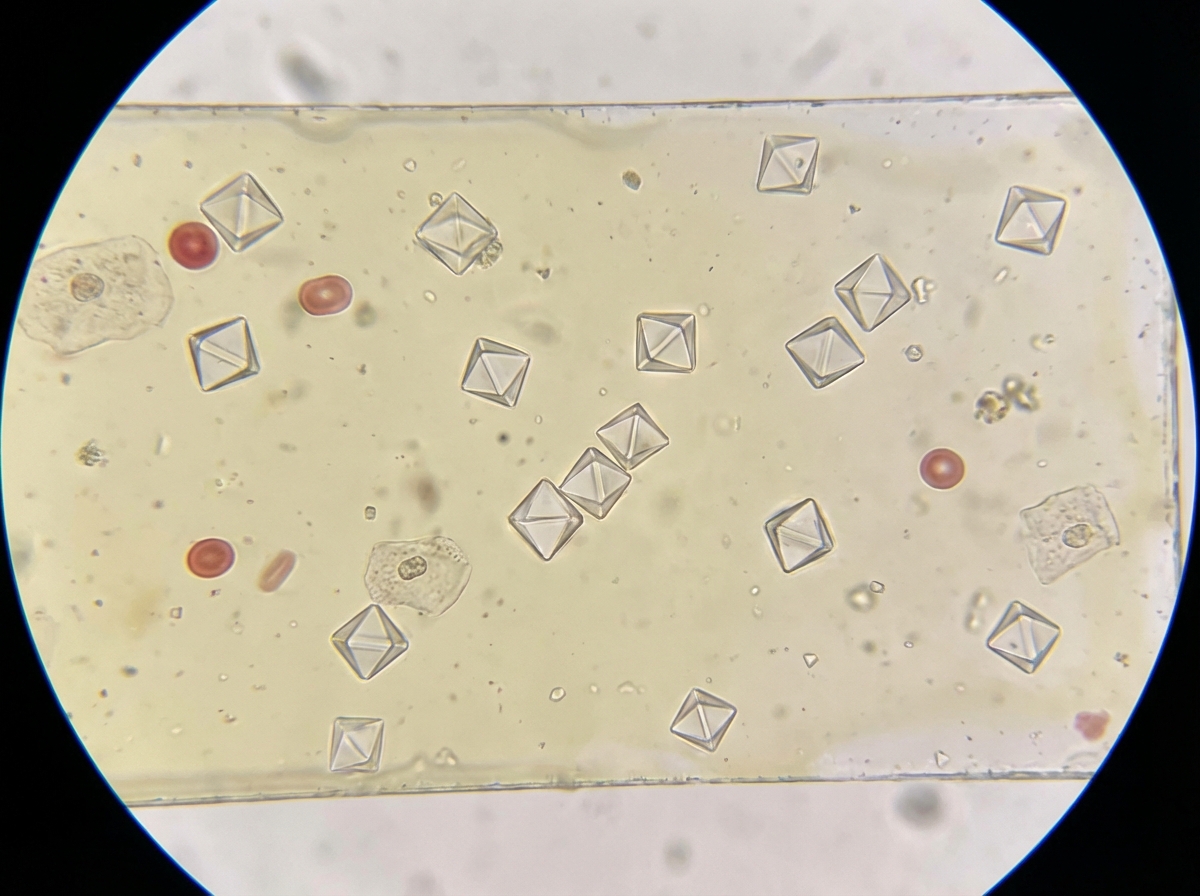
Which urine crystals are shown in the figure below?
Practice by Chapter
Congenital renal anomalies
Practice Questions
Glomerular diseases overview
Practice Questions
Nephritic syndrome disorders
Practice Questions
Nephrotic syndrome disorders
Practice Questions
Rapidly progressive glomerulonephritis
Practice Questions
Tubulointerstitial diseases
Practice Questions
Acute tubular necrosis
Practice Questions
Renal vascular diseases
Practice Questions
Pyelonephritis and urinary tract infections
Practice Questions
Renal cystic diseases
Practice Questions
Obstructive uropathies
Practice Questions
Renal tumors
Practice Questions
Kidney transplant pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
