Pulmonary — MCQs

On this page
A lung mass of a 50 pack-year smoker is biopsied. If ADH levels were grossly increased, what would most likely be the histologic appearance of this mass?
A 73-year-old man is brought to the emergency department because of fever, malaise, dyspnea, and a productive cough with purulent sputum for the past day. His temperature is 39.2°C (102.6°F). Pulmonary examination shows crackles over the right upper lung field. Sputum Gram stain shows gram-positive cocci. Despite the appropriate treatment, the patient dies 5 days later. At autopsy, gross examination shows that the right lung has a pale, grayish-brown appearance and a firm consistency. Microscopic examination of the tissue is most likely to show which of the following?
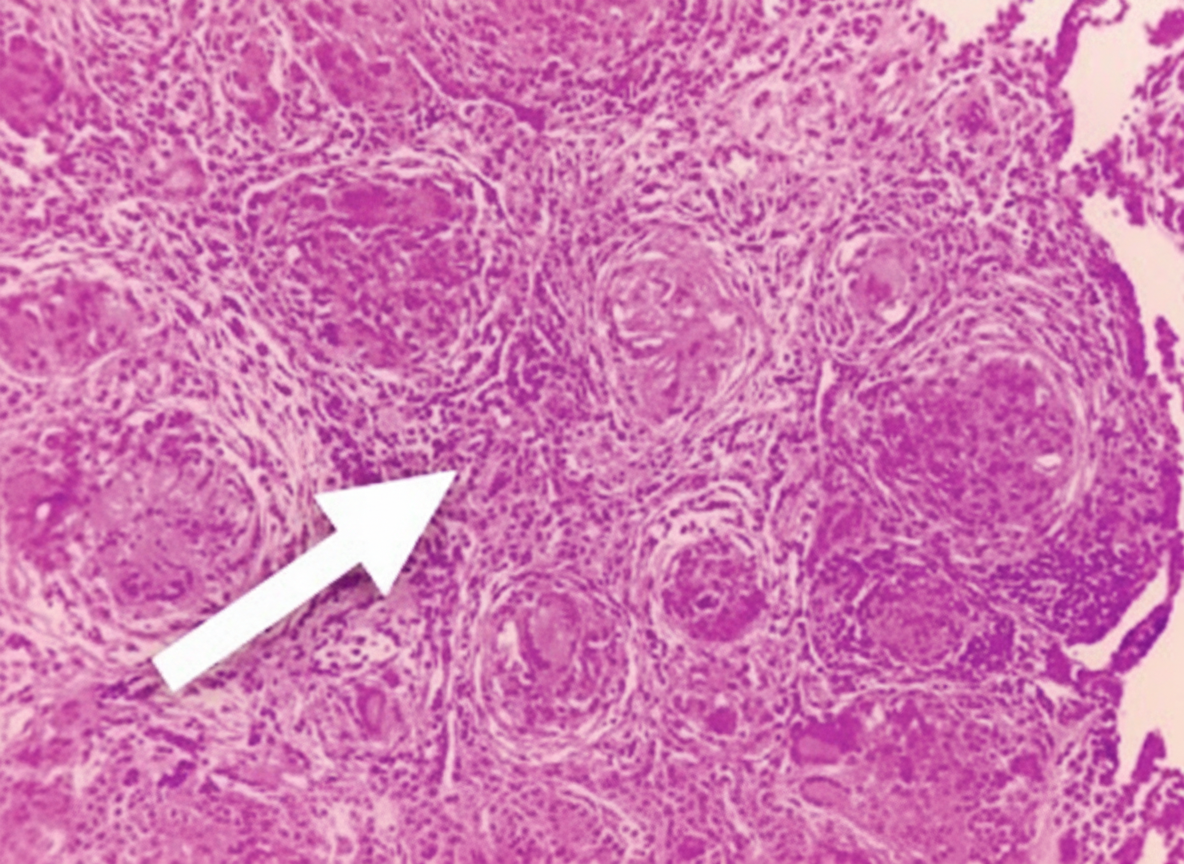
A 38-year-old man comes to the physician because of fever, malaise, cough, and shortness of breath for 2 months. He has had a 4-kg (9-lb) weight loss during the same period. He works at a flour mill and does not smoke cigarettes. His temperature is 38.1°C (100.6°F) and pulse oximetry shows 95% on room air. Diffuse fine crackles are heard over both lung fields. A chest x-ray shows patchy reticulonodular infiltrates in the mid and apical lung fields bilaterally. A photomicrograph of a lung biopsy specimen is shown. Which of the following cytokines have the greatest involvement in the pathogenesis of the lesion indicated by the arrow?
A 61-year-old man presents with gradually increasing shortness of breath. For the last 2 years, he has had a productive cough on most days. Past medical history is significant for hypertension and a recent admission to the hospital for pneumonia. He uses a triamcinolone inhaler and uses an albuterol inhaler as a rescue inhaler. He also takes lisinopril and a multivitamin daily. He has smoked a pack a day for the last 32 years and has no intention to quit now. Today, his blood pressure is 142/97 mm Hg, heart rate is 97/min, respiratory rate is 22/min, and temperature is 37.4°C (99.3°F). On physical exam, he has tachypnea and has some difficulty finishing his sentences. His heart has a regular rate and rhythm. Auscultation of his lungs reveals wheezing and rhonchi that improves after a deep cough. Fremitus is absent. Pulmonary function tests show FEV1/FVC of 55% with no change in FEV1 after albuterol treatment. Which of the following is the most likely pathology associated with this patient's disease?
A 53-year-old man is admitted to the intensive care unit from the emergency department with severe pancreatitis. Overnight, he starts to develop severe hypoxemia, and he is evaluated by a rapid response team. On exam the patient is breathing very quickly and has rales and decreased breath sounds bilaterally. He is placed on 50% FiO2, and an arterial blood gas is collected with the following results: pH: 7.43 pCO2: 32 mmHg pO2: 78 mmHg The oxygen status of the patient continues to deteriorate, and he is placed on ventilator support. Which of the following would most likely be seen in this patient?
A 73-year-old female with no past medical history is hospitalized after she develops a fever associated with increasing shortness of breath. She states that 1 week prior, she had a cold which seemed to be resolving. Yesterday, however, she noticed that she started to feel feverish, measured her temperature to be 101.5°F (38.6°C), and also developed an unproductive dry cough and difficulty breathing. On exam, her temperature is 100.8°F (38.2°C), blood pressure is 110/72 mmHg, pulse is 96/min, and respirations are 16/min. Her exam demonstrates decreased breath sounds at the right lung base. The chest radiograph shows a right-sided pleural effusion with an opacity in the right lower lobe that is thought to be a bacterial pneumonia. Which of the following can be expected on a sample of the effusion fluid?
A 48-year-old woman with alpha-1-antitrypsin deficiency undergoes a lung transplant. She tolerates the surgery well, but 3 years later develops inflammation and fibrosis in her terminal bronchioles. Which of the following best describes the pathophysiology of this patient's deterioration?
In which of the following pathological states would the oxygen content of the trachea resemble the oxygen content in the affected alveoli?
An 82-year-old woman is admitted to the hospital because of wet gangrene on her right leg. Two days after admission, she becomes increasingly confused and tachypneic. She is intubated and ventilatory support is initiated. Her temperature is 39.6°C (102.5°F), pulse is 127/min, and blood pressure is 83/47 mm Hg. The ventilator is set at a FiO2 of 100% and a respiratory rate of 20/min. An arterial blood gas checked 30 minutes after intubation shows a PCO2 of 41 mm Hg and a PO2 of 55 mm Hg. Despite appropriate care, the patient dies from respiratory failure. Further evaluation of this patient is most likely to show which of the following findings?
Practice by Chapter
Atelectasis
Practice Questions
Pulmonary edema
Practice Questions
Acute respiratory distress syndrome
Practice Questions
Obstructive lung diseases (emphysema, bronchitis)
Practice Questions
Asthma pathology
Practice Questions
Bronchiectasis
Practice Questions
Restrictive lung diseases
Practice Questions
Interstitial lung diseases
Practice Questions
Pulmonary vascular disorders
Practice Questions
Pulmonary infections
Practice Questions
Lung tumors (primary and metastatic)
Practice Questions
Pleural diseases
Practice Questions
Congenital lung anomalies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
