Pulmonary — MCQs

On this page
A 15-year-old boy is brought to the emergency department with a 30 minute history of difficulty breathing. He was playing basketball in gym class when he suddenly felt pain in the right side of his chest that got worse when he tried to take a deep breath. Physical exam reveals a tall, thin boy taking rapid shallow breaths. There are decreased breath sounds in the right lung fields and the right chest is hyperresonant to percussion. Which of the following is true of the lesions that would most likely be seen in this patient's lungs?
A 56-year-old man comes to the physician for a follow-up examination one week after a chest x-ray showed a solitary pulmonary nodule. He has no history of major medical illness. He has smoked 1 pack of cigarettes daily for the past 30 years. Physical examination shows no abnormalities. A tuberculin skin test is negative. A CT scan of the chest shows a 2.1-cm well-circumscribed, calcified nodule in the periphery of the right lower lung field. A CT-guided biopsy of the lesion is performed. Histological examination of the biopsy specimen shows regions of disorganized hyaline cartilage interspersed with myxoid regions and clefts of ciliated epithelium. Which of the following is the most likely diagnosis?
A 72-year-old retired shipyard worker received a chest x-ray as part of a routine medical work-up. The radiologist reported incidental findings suggestive of an occupational lung disease. Which of the following descriptions is most consistent with this patient's film?
A 66-year-old man presents with severe respiratory distress. He was diagnosed with pulmonary hypertension secondary to occupational pneumoconiosis. Biopsy findings of the lung showed ferruginous bodies. What is the most likely etiology?
A 58-year-old man is brought to the emergency department after a witnessed tonic-clonic seizure. His wife says he has had a persistent dry cough for 6 months. During this time period, he has also had fatigue and a 4.5-kg (10-lb) weight loss. The patient has no history of serious illness and does not take any medications. He has smoked 1 pack of cigarettes daily for 35 years. He is confused and oriented only to person. Laboratory studies show a serum sodium concentration of 119 mEq/L and glucose concentration of 102 mg/dL. An x-ray of the chest shows an irregular, poorly demarcated density at the right hilum. Microscopic examination of this density is most likely to confirm which of the following diagnoses?
A 68-year-old man presents to the office with progressive shortness of breath and cough. A chest X-ray shows prominent hilar lymph nodes and scattered nodular infiltrates. Biopsy of the latter reveals noncaseating granulomas. This patient most likely has a history of exposure to which of the following?
A 61-year-old male presents to your office with fever and dyspnea on exertion. He has been suffering from chronic, non-productive cough for 1 year. You note late inspiratory crackles on auscultation. Pulmonary function tests reveal an FEV1/FVC ratio of 90% and an FVC that is 50% of the predicted value. Which of the following would you most likely see on a biopsy of this patient's lung?
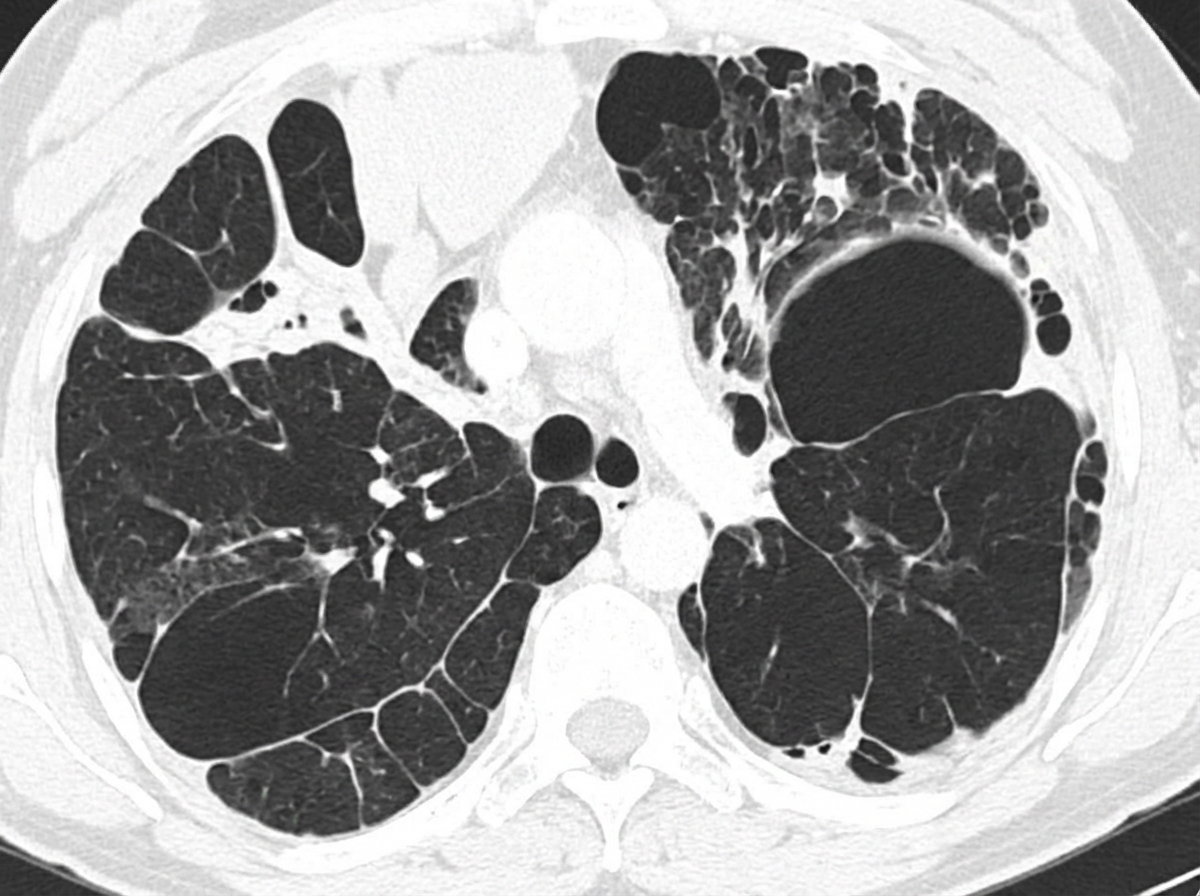
A 58-year-old woman presents to the physician with a cough that began 6 years ago, as well as intermittent difficulty in breathing for the last year. There is no significant sputum production. There is no history of rhinorrhea, sneezing or nose congestion. She has been a chronic smoker from early adulthood. Her temperature is 36.9°C (98.4°F), the heart rate is 80/min, the blood pressure is 128/84 mm Hg, and the respiratory rate is 22/min. A physical examination reveals diffuse end-expiratory wheezing with prolonged expiration on chest auscultation; breath sounds and heart sounds are diminished. There is no cyanosis, clubbing or lymphadenopathy. Her chest radiogram shows hyperinflated lungs bilaterally and a computed tomography scan of her chest is shown in the picture. Which of the following best describes the pathogenesis of the condition of this patient?
A 32-year-old man comes to the physician for a 1-month history of fever, chest pain with deep breathing, and a 4-kg (9 lb) weight loss. His temperature is 38°C (100.4°F). An x-ray of the chest shows a subpleural nodule in the right lower lobe with right hilar lymphadenopathy. Histological examination of a right hilar lymph node biopsy specimen shows several granulomas with acellular cores. Which of the following is the most likely diagnosis?
An investigator is studying the effects of influenza virus on human lung tissue. Biopsy specimens of lung parenchyma are obtained from patients recovering from influenza pneumonia and healthy control subjects. Compared to the lung tissue from the healthy control subjects, the lung tissue from the affected patients is most likely to show which of the following findings on histopathologic examination?
Practice by Chapter
Atelectasis
Practice Questions
Pulmonary edema
Practice Questions
Acute respiratory distress syndrome
Practice Questions
Obstructive lung diseases (emphysema, bronchitis)
Practice Questions
Asthma pathology
Practice Questions
Bronchiectasis
Practice Questions
Restrictive lung diseases
Practice Questions
Interstitial lung diseases
Practice Questions
Pulmonary vascular disorders
Practice Questions
Pulmonary infections
Practice Questions
Lung tumors (primary and metastatic)
Practice Questions
Pleural diseases
Practice Questions
Congenital lung anomalies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
