Neoplasia — MCQs

On this page
A 6-year-old boy is brought to a primary care provider by his adoptive parents for evaluation of a 3-month history of jaw swelling. He has a travel history of recent immigration from equatorial Africa where his deceased mother was positive for HIV and died from related complications. On physical exam, extensive lymph node swelling on the left side of his jaw is noted. There is also an ulceration that appears to be infected. Fine needle biopsy of the lymph node yields a diagnosis of Burkitt’s lymphoma by the pathologist. Which of the following is most likely associated with the involvement of lymph nodes around his jaw?
A 74-year-old man comes to the physician for evaluation of a skin lesion on his right arm. The lesion first appeared 3 months ago and has since been slowly enlarging. Physical examination shows a 1.5-centimeter, faintly erythematous, raised lesion with irregular borders on the dorsum of the right forearm. A biopsy specimen is obtained. If present, which of the following histopathological features would be most consistent with carcinoma in situ?
A 45-year-old woman presents to the emergency department after sustaining a gunshot wound to her shoulder. During the course of the physical exam, the physician notes her spleen is palpable 10 cm below the left costal margin. Additionally, radiography of her shoulder showed several 'punched-out' areas of lytic bone. While this was considered an incidental finding at the time, she was referred to her primary care physician for further workup. Subsequent biopsy of the spleen demonstrated that this patient’s splenomegaly was caused by an infiltrative process. Which of the following processes would most likely result in splenomegaly in this patient?
A 67-year-old man presents to the emergency department with increased fatigue. He states that he has been feeling very tired lately but today lost consciousness while walking up the stairs. He reports mild abdominal distension/discomfort, weight loss, a persistent cough, and multiple episodes of waking up drenched in sweat in the middle of the night. The patient does not see a primary care physician but admits to smoking 2 to 3 packs of cigarettes per day and drinking 1 to 3 alcoholic beverages per day. He recently traveled to Taiwan and Nicaragua. His temperature is 99.5°F (37.5°C), blood pressure is 177/98 mmHg, pulse is 100/min, respirations are 17/min, and oxygen saturation is 98% on room air. On physical exam, you note a fatigued appearing elderly man who is well-groomed. Cardiopulmonary exam reveals mild expiratory wheezes. Abdominal exam is notable for a non-pulsatile mass in the left upper quadrant. Laboratory values are ordered as seen below. Hemoglobin: 12 g/dL Hematocrit: 36% Leukocyte count: 105,500/mm^3 Platelet count: 197,000/mm^3 Serum: Na+: 139 mEq/L Cl-: 100 mEq/L K+: 4.3 mEq/L HCO3-: 25 mEq/L BUN: 20 mg/dL Glucose: 92 mg/dL Creatinine: 1.4 mg/dL Ca2+: 10.2 mg/dL Leukocyte alkaline phosphatase score: 25 (range 20 - 100) AST: 12 U/L ALT: 17 U/L Which of the following is the most likely diagnosis?
A previously healthy 50-year-old woman is brought to the emergency department 30 minutes after she was observed having a seizure. On arrival, she is conscious and reports that she feels drowsy. An MRI of the brain shows a 4-cm, round, sharply demarcated mass. She undergoes resection of the mass. A photomicrograph of a section of the resected specimen is shown. This patient's mass is most likely derived from which of the following?
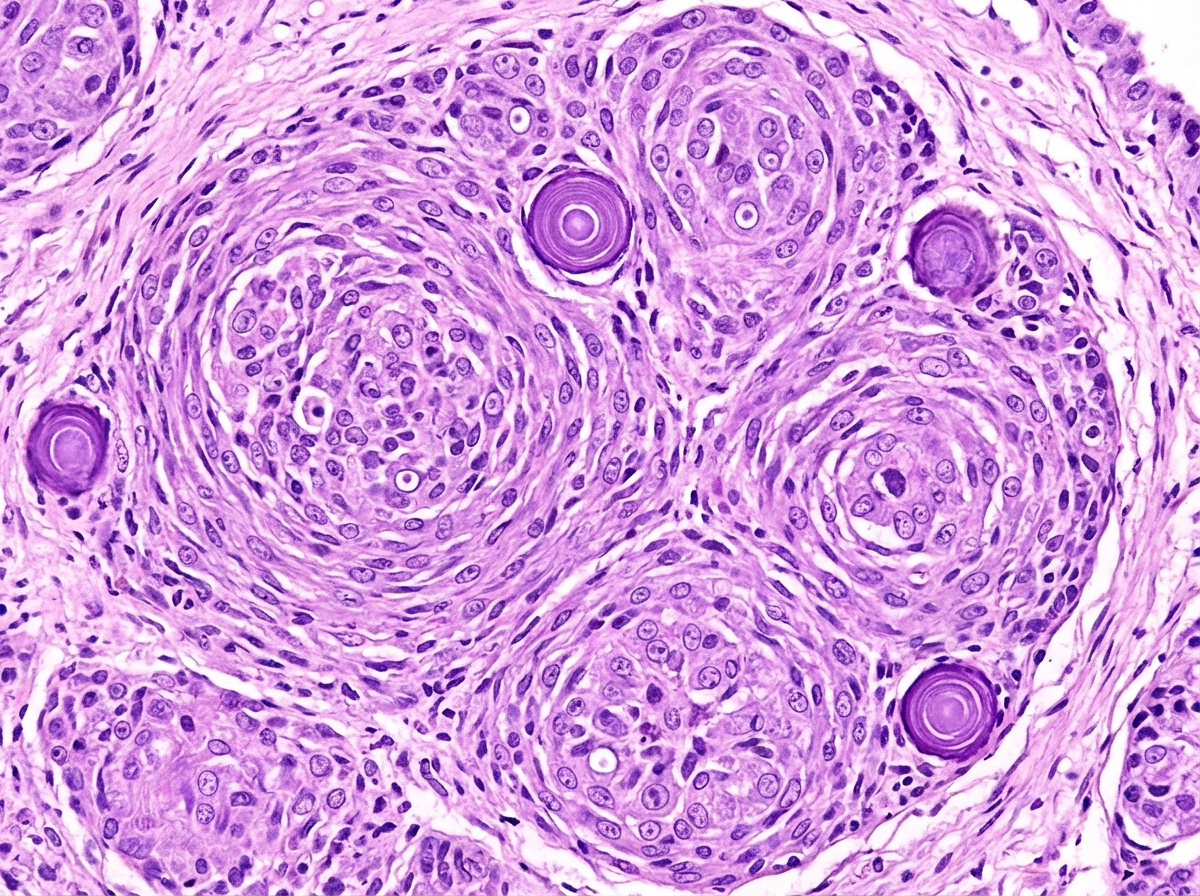
A 9-year-old boy presents with polydipsia, polyuria, and a serum osmolality of 325 mOsm/L. A neurologic examination reveals bitemporal hemianopia. The lesion is believed to be derived from Rathke's pouch remnants. Which of the following is the most likely histologic finding?
A 38-year-old man presents with concerns after finding out that his father was recently diagnosed with colon cancer. Family history is only significant for his paternal grandfather who also had colon cancer. A screening colonoscopy is performed, and a polyp is found in the ascending (proximal) colon, which on biopsy shows adenocarcinoma. A mutation in a gene that is responsible for which of the following cellular functions is the most likely etiology of this patient’s cancer?
A 71-year-old man comes to the physician for a routine health maintenance examination. He has occasional fatigue but otherwise feels well. He has a history of hypertension and type 2 diabetes mellitus. He is a retired chemist. His only medication is ramipril. His temperature is 37.8°C (100°F), pulse is 72/min, respirations are 18/min, and blood pressure is 130/70 mm Hg. Physical examination shows nontender cervical and axillary lymphadenopathy. The spleen is palpated 7 cm below the costal margin. Laboratory studies show a leukocyte count of 12,000/mm3 and a platelet count of 210,000/mm3. Further evaluation is most likely to show which of the following?
A 44-year-old woman presents for her annual physical checkup. She says she first noticed a mass in her right breast while taking a shower 3 months ago, which has progressively increased in size. She denies any weight loss, fever, night sweats, discharge from or change in her nipples. Her family history is negative for breast, ovarian, and endometrial cancer. She is afebrile, and her vital signs are within normal limits. Physical examination reveals a smooth, multinodular, firm 5 cm x 5 cm mass in the right breast that is mobile and painless. The skin over the mass appears to be stretched and shiny without ulcerations, erythema, or vascular demarcation. On follow-up 6 weeks later, an interval ultrasound of the right breast reveals a well-circumscribed hypoechoic mass with some cystic components that now measures 8 cm x 7 cm. A core needle biopsy of the mass is performed. Which of the following diagnosis is most likely expected to be confirmed by the core needle biopsy in this patient?
A 27-year-old man comes to the physician because of a 4-month history of recurrent episodes of headaches, palpitations, and sweating. He was adopted shortly after birth and does not know his biological parents. His pulse is 103/min and blood pressure is 160/105 mm Hg. Physical examination shows multiple soft, yellow papules on the tip of the tongue. There is a 2-cm, firm thyroid nodule. He has long and slender upper extremities, and his elbows and knees can be hyperextended. The most likely cause of this patient's condition is a mutation in which of the following genes?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
