Neoplasia — MCQs

On this page
A 19-year-old man comes to the physician for evaluation of night sweats, pruritus, and enlarging masses in his right axilla and supraclavicular area for 2 weeks. Physical examination shows painless, rubbery lymphadenopathy in the right axillary, supraclavicular, and submental regions. An excisional biopsy of an axillary node is performed. If present, which of the following features would be most concerning for a neoplastic process?
A 62-year-old man seeks evaluation at a local walk-in clinic for mid-low back pain of several weeks. He has tried different rehabilitation therapies and medications with no improvement. He was prescribed some pain medications and sent home last week, but the patient presents today with difficulty walking and worsening of his back pain. He was referred to the ER, where he was examined and found to have hypoesthesia from T12 to S4–S5, significant muscle weakness in both lower limbs, and reduced knee and ankle deep tendon reflexes. A hypotonic anal sphincter with conserved deep anal pressure was demonstrated on digital rectal examination, as well as a multinodular, asymmetric prostate. Imaging studies showed multiple sclerotic bone lesions along the spine. Subsequently, a prostate core biopsy was obtained which confirmed the diagnosis of prostate cancer. Which of the following characteristics would you expect in the specimen?
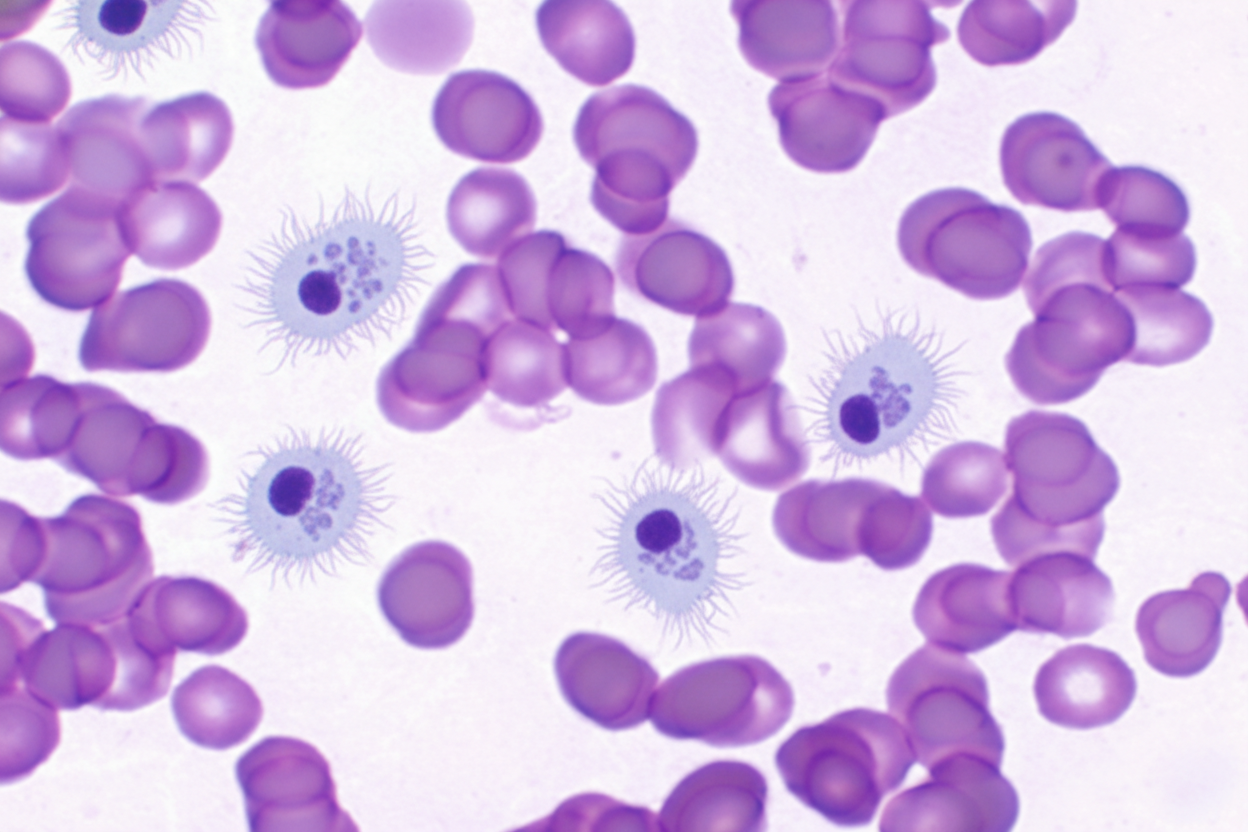
A 62-year-old man comes to the physician because of easy bruising and recurrent nosebleeds over the past 4 months. During the same time period, the patient has felt weak and has had a 10-kg (22-lb) weight loss. Physical examination shows mucosal pallor and bruising on the upper and lower extremities in various stages of healing. The spleen is palpated 4 cm below the left costal margin. Laboratory studies show anemia and thrombocytopenia. A photomicrograph of a peripheral blood smear is shown. Histologic examination of a bone marrow biopsy in this patient is most likely to show which of the following findings?
An otherwise healthy 66-year-old man comes to the physician for evaluation of rough skin over his forehead and the back of his hands. He has tried applying different types of moisturizers with no improvement. He has worked on a farm all his life. Physical examination shows two erythematous papules with a gritty texture and central scale over the left temple and three similar lesions over the dorsum of his hands. This patient's skin lesions increase his risk of developing a skin condition characterized by which of the following findings on histopathology?
A 62-year-old woman presents to the clinic for a 2-month history of ‘fogginess’. She reports that for the last couple of months she feels like she has "lost a step" in her ability to think clearly, often forgetting where she parked her car or to lock the front door after leaving the house. She also feels that her mood has been low. On further questioning, she reports mild constipation and that she has had a bothersome, progressively worsening cough over the past couple of months, accompanied by 6.8 kg (15 lb) unintentional weight loss. She has a history of hypertension for which she takes amlodipine daily. She has smoked 1.5 packs of cigarettes per day for the last 40 years. Physical exam is unremarkable. Laboratory studies show: Na+ 138 mg/dL K+ 3.9 mg/dL Cl- 101 mg/dL HCO3- 24 mg/dL BUN 10 mg/dL Cr 0.6 mg/dL Glucose 86 mg/dL Ca2+ 13.6 mg/dL Mg2+ 1.9 mg/dL Parathyroid hormone (PTH) 2 pg/mL (10–65) 1,25-hydroxyvitamin D 15 pg/mL (20–45) Quantiferon-gold negative Which of the following best describes this patient's most likely underlying pathology?
A 63-year-old man comes to the physician because of increasing generalized fatigue for 3 months. He is having more difficulty with keeping up with his activities of daily living and has lost 2.5 kg (5.5 lb) over the past month. He has hypertension and hyperlipidemia. He does not smoke and drinks two to three beers on weekends. His medications include lisinopril, hydrochlorothiazide, and atorvastatin. His temperature is 37.1°C (98.8°F), pulse is 85/min, respirations are 15/min, and blood pressure is 125/73 mm Hg. Examination shows pale conjunctivae. The remainder of the examination shows no abnormalities. His hematocrit is 27.3%, leukocyte count is 4500/mm3, and platelet count is 102,000/mm3. A peripheral blood smear shows numerous blast cells that stain positive for myeloperoxidase, CD33, and CD34. Which of the following is the most likely diagnosis?
A 62-year-old man comes to the physician because of progressive fatigue and dyspnea on exertion for 3 months. During this time, he has also had increased straining during defecation and a 10-kg (22-lb) weight loss. He has no personal or family history of serious medical illness. Physical examination shows conjunctival pallor. Laboratory studies show microcytic anemia. Test of the stool for occult blood is positive. Colonoscopy shows an exophytic mass in the ascending colon. Pathologic examination of the mass shows a well-differentiated adenocarcinoma. A gain-of-function mutation in which of the following genes is most likely involved in the pathogenesis of this patient's condition?
A 52-year-old man arrives to the clinic for arthritis and leg swelling. The patient reports that the joint pains began 8 months ago. He has tried acetaminophen and ibuprofen without significant improvement. He reports the leg swelling began within the past 2 months and has gotten progressively worse. The patient’s medical history is significant for diabetes. His medications include metformin and aspirin. The patient works as an accountant. He smokes cigars socially. The patient’s temperature is 99°F (37.2°C), blood pressure is 130/78 mmHg, pulse is 70/min, and respirations are 14/min with an oxygen saturation of 98% on room air. Physical examination notes a tan, overweight male with 2+ edema of bilateral lower extremities. Which of the following tumor markers is most likely to be associated with this patient’s condition?
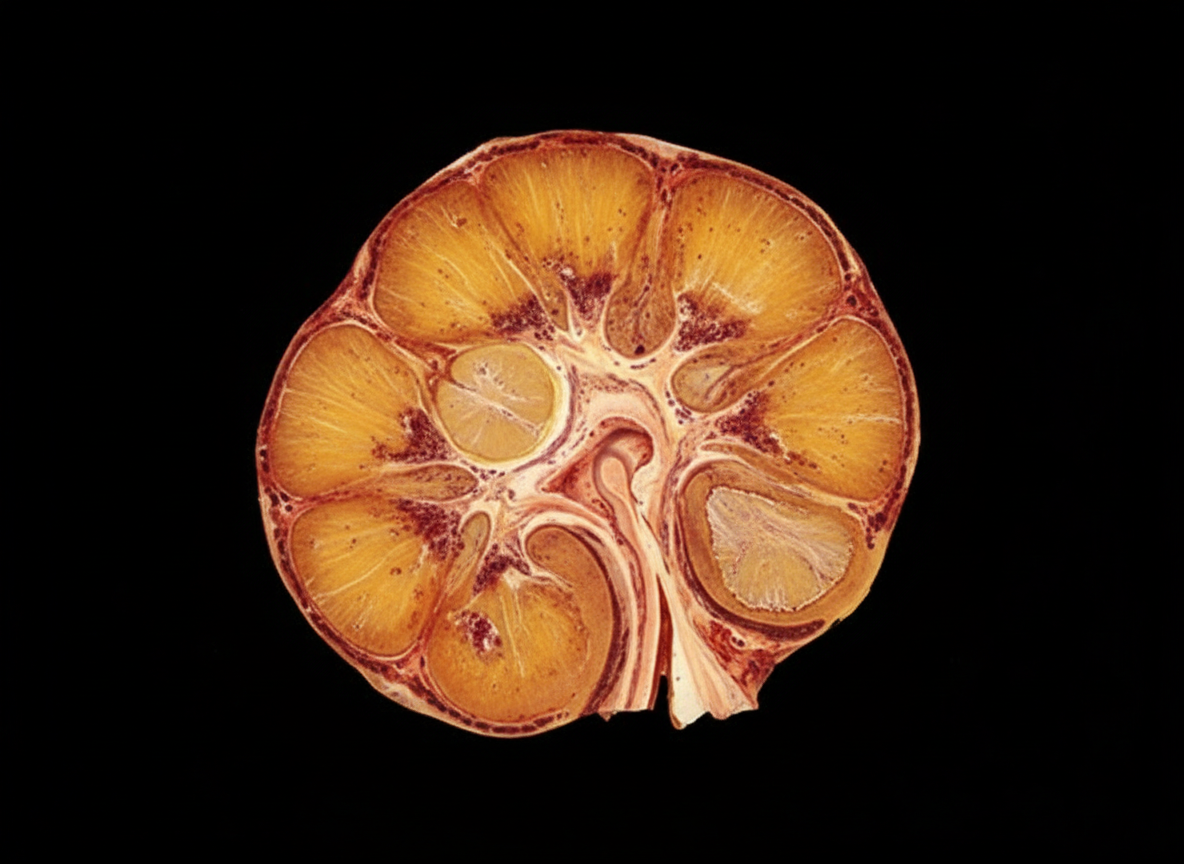
A 75-year-old man comes to the physician because of abdominal pain and nausea over the past 2 weeks and a 1-month history of pain in his knees and hips. He has smoked one pack of cigarettes daily for 30 years. Physical examination shows decreased muscle strength. Laboratory studies show: Hemoglobin 11.0 mg/dL Serum Creatinine 1.5 mg/dL Calcium 12.2 mg/dL Parathyroid hormone 115 pg/mL Parathyroid hormone-related peptide elevated Urine Blood 2+ Ultrasonography of his abdomen shows a 6-cm mass in his right kidney. Nephrectomy is performed. A photograph of the resected specimen is shown. The patient's tumor most likely originated from which of the following locations?
A 51-year-old woman comes to the physician because of a persistent cough and a 5-kg (11-lb) weight loss over the past 2 months. Yesterday, she coughed up bloody sputum. She does not smoke. Pulmonary examination shows decreased breath sounds over the right upper lobe. A CT scan of the chest shows a mass in the periphery of the right upper lobe. Histopathologic examination of a specimen obtained on CT-guided biopsy shows glandular cells with papillary components and signet ring cells that stain positive for mucin. An alteration in which of the following genes is most likely to have occurred in this patient?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
