Neoplasia — MCQs

On this page
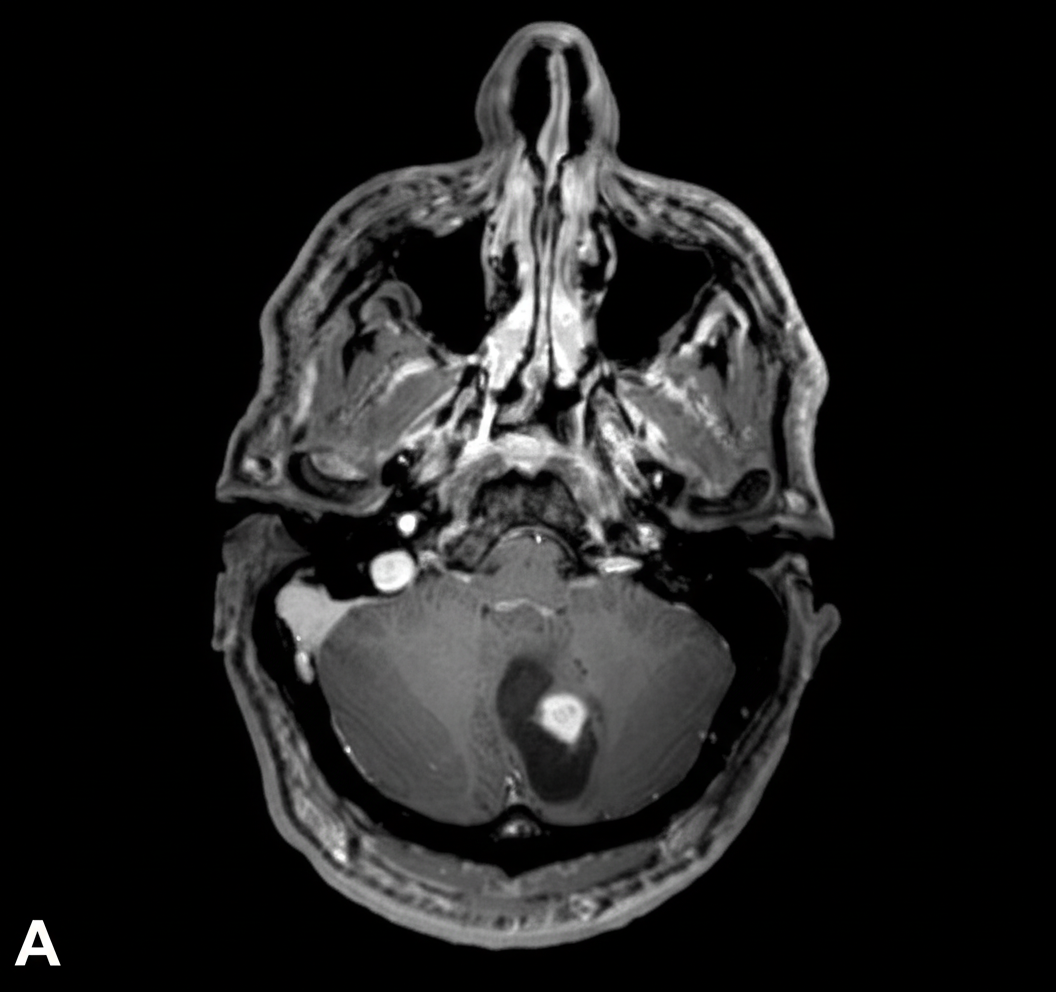
A 9-year-old girl is brought to her primary care physician because of a 4-month history of early morning headaches and worsening fatigue. The headaches are often accompanied by nausea and sometimes relieved by vomiting. She stopped going to her ballet lessons 2 weeks ago because she was embarrassed about falling frequently and having increasing difficulty performing the steps. Her temperature is 36.8°C (98.2°F), pulse is 98/min, and blood pressure is 105/65 mm Hg. She has a broad-based gait. While standing with both feet together and raising her arms, closing her eyes does not affect her balance. She is unable to perform rapid, alternating movements with her hands. An MRI of the brain is shown. Which of the following is the most likely diagnosis?
A sexually active 37-year-old man comes to the physician because of a 7-day history of itching in the area of his genitals. He also reports burning on micturition. He has type 2 diabetes mellitus, which is well controlled with oral metformin. Pelvic examination shows tender, atrophic white papules on the glans and prepuce, with erythema of the surrounding skin. The urinary meatus is narrowed and sclerotic. Which of the following is the most appropriate next step in diagnosis?
A 29-year-old man comes to the physician because of a 3-month history of fatigue, weight loss, and multiple painless swellings on his neck and axilla. He reports that his swellings become painful after he drinks alcohol. Physical examination shows nontender cervical and axillary lymphadenopathy. A lymph node biopsy specimen shows giant binucleate cells. Which of the following is the most likely diagnosis?
A 32-year-old Caucasian man presents to the physician because of the swelling and discomfort of the right testis for 3 weeks. There is no history of trauma, fever, or night sweats. He had surgery for an undescended right testis when he was 6 months old. There is no history of liver disease or hypogonadism. He has fathered 2 children. He takes no medications and denies any illicit drug use. The vital signs are within normal limits. Palpation of the scrotum reveals a firm nontender mass that cannot be separated from the right testis. Examination of the left testis shows no abnormalities. There is no supraclavicular or inguinal lymphadenopathy. Gynecomastia is present. The rest of the physical examination is unremarkable. Ultrasound shows an enlarged right testicle with a hypoechoic mass replacing a large portion of the normal architecture. The left testis is normal. The laboratory test results are as follows: HCG Elevated AFP Elevated LDH Normal Which of the following is the most likely diagnosis?
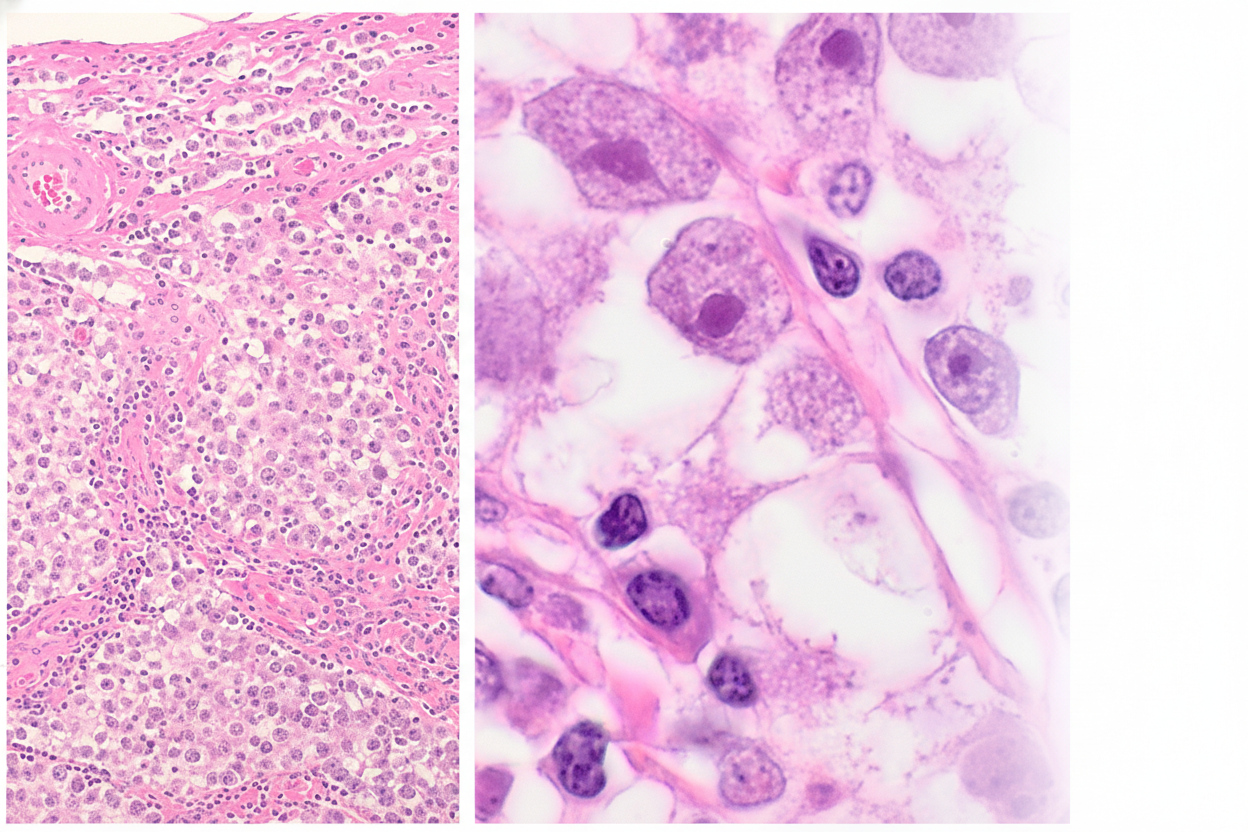
A 22-year-old man comes to the physician for the evaluation of a 2-day history of right testicular pain. At the age of 6 months, he was treated for hypospadias and cryptorchidism. Physical examination shows a rubbery, large right testicle. Orchidectomy is performed. A photomicrograph of a section of the mass is shown. Which of the following additional findings is most likely in this patient?
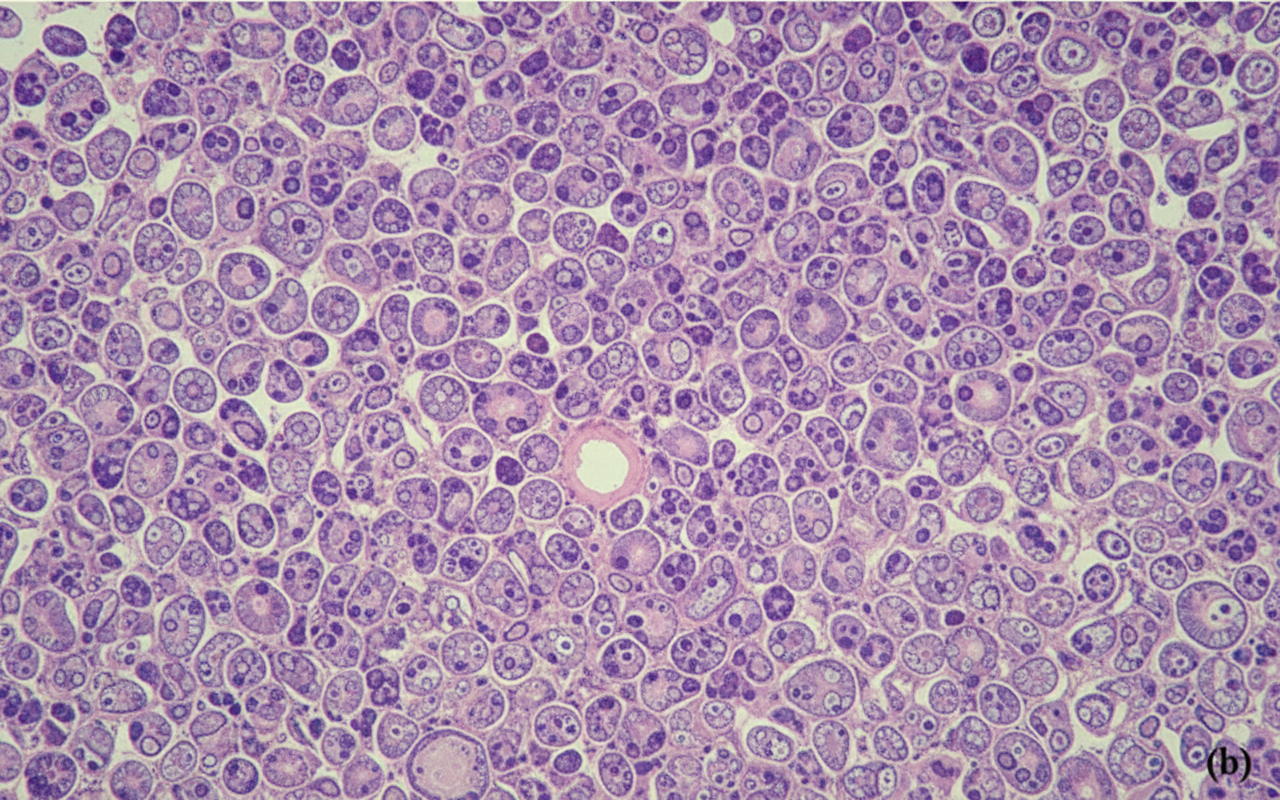
A 60-year-old woman comes to the physician because of lower back pain, generalized weakness, and weight loss that has occurred over the past 6 weeks. She also says that her urine has appeared foamy recently. Physical examination shows focal midline tenderness of the lumbar spine and conjunctival pallor. Her temperature is 100.5°F (38°C). A photomicrograph of a bone marrow biopsy specimen is shown. Further evaluation of this patient is most likely to show which of the following findings?
A 72-year-old man presents to the clinic for the evaluation of a lesion on his nose that has been slowly getting larger for the past 2 months. The patient notes no history of trauma, pruritus, or pain, but states that the size of the lesion is making his nose feel uncomfortable. On exam, the nodule is pink with rolled borders. Telangiectasias are also present within the lesion, with central ulceration. What is the characteristic histologic appearance of this lesion?
A 21-year-old male college student is very anxious about having thyroid cancer as he found a lump in his neck a few days ago. He has also had diarrhea and a feeling of warmth on his face for 3 days now. His father and uncle both have been diagnosed with thyroid cancer. The lump is about 1 cm in diameter and is fixed and nontender on palpation. Physical examination is otherwise unremarkable. Ultrasound shows a non-cystic cold nodule that requires fine needle aspiration for diagnosis. Thyroid functions tests are normal, and his calcitonin level is 346 ug/ml. Which of the following genetic mutations would warrant thyroidectomy in this patient?
A 12-year-old boy is brought in by his mother for a routine checkup. The patient’s mother says he is frequently fatigued and looks pale. She also claims that he has recently become “much quieter” than normal and is no longer interested in playing baseball with his friends. The patient’s mother believes it may just be “growing pains.” The patient has no significant medical history. He is the 90th percentile for height and weight and has been meeting all developmental milestones. The patient is afebrile, and his vital signs are within normal limits. Physical examination reveals several small bruises on the patient’s right arm and on both thighs. Laboratory findings are significant for the following: Sodium 140 mEq/L Potassium 4.2 mEq/L Chloride 101 mEq/L Bicarbonate 27 mEq/L BUN 16 mg/dL Creatinine 1.2 mg/dL Glucose (fasting) 111 mg/dL WBC 3,400/mm3 RBC 4.20 x 106/mm3 Hematocrit 22% Hemoglobin 7.1 g/dL Platelet count 109,000/mm3 A peripheral blood smear reveals myeloblasts. Which of the following is the next best step in the management of this patient?
A 62-year-old man comes to the physician because of a 2-month history of an itchy rash and a 7-kg (15-lb) weight loss. Physical examination shows multiple erythematous plaques on the arms, legs, and chest. There are palpable lymph nodes in the axillary and inguinal areas. A biopsy of a skin lesion shows aggregates of neoplastic cells within the epidermis. A peripheral blood smear is most likely to show which of the following findings in this patient?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
