Neoplasia — MCQs

On this page
A 70-year-old man presents to his physician for evaluation of fullness and swelling of the left side of the abdomen over the last month. During this time, he has had night sweats and lost 2 kg (4.4 lb) unintentionally. He has no history of severe illness and takes no medications. The vital signs include: blood pressure 115/75 mm Hg, pulse 75/min, and temperature 36.8℃ (98.2℉). The abdomen has asymmetric distention. Percussion and palpation of the left upper quadrant reveal splenomegaly. No lymphadenopathy is detected. Heart and lung examination shows no abnormalities. The laboratory studies show the following: Hemoglobin 9.5 g/dL Mean corpuscular volume 95 μm3 Leukocyte count 8,000/mm3 Platelet count 240,000/mm3 Ultrasound shows a spleen size of 15 cm, mild hepatomegaly, and mild ascites. The peripheral blood smear shows teardrop-shaped and nucleated red blood cells (RBCs) and immature myeloid cells. Marrow is very difficult to aspirate but reveals hyperplasia of all 3 lineages. The tartrate-resistant acid phosphatase (TRAP) test is negative. The cytogenetic analysis is negative for translocation between chromosomes 9 and 22. Which of the following laboratory findings is most likely to be present in this patient?
A 59-year-old woman comes to the physician because of a 2-month history of fatigue and abdominal discomfort. Over the past 6 months, she has had a 5.4-kg (12-lb) weight loss. She takes no medications. Her temperature is 37.8°C (100°F), pulse is 70/min, respirations are 13/min, and blood pressure is 125/80 mm Hg. Cardiopulmonary examination shows no abnormalities. The spleen is palpated 3 cm below the left costal margin. Laboratory studies show: Hemoglobin 9.4 g/dL Mean corpuscular volume 86 μm3 Leukocyte count 58,000/mm3 Segmented neutrophils 54% Bands 8% Lymphocytes 7% Myelocytes 5% Metamyelocytes 10% Promyelocytes 4% Blasts 5% Monocytes 1% Eosinophils 4% Basophils 2% Platelet count 850,000/mm3 Serum Creatinine 0.9 mg/dL LDH 501 U/L Bone marrow biopsy shows hyperplastic myelopoiesis with granulocytosis. Which of the following is the most appropriate next step in management?
An 11-year-old boy is brought to the pediatrician by his mother for vomiting. The patient has been vomiting for the past week, and his symptoms have not been improving. His symptoms are worse in the morning and tend to improve throughout the day. The patient also complains of occasional headaches and had diarrhea several days ago. The patient eats a balanced diet and does not drink soda or juice. The patient's brothers both had diarrhea recently that resolved spontaneously. His temperature is 99.5°F (37.5°C), blood pressure is 80/45 mmHg, pulse is 90/min, respirations are 16/min, and oxygen saturation is 98% on room air. On physical exam, the patient appears to be in no acute distress. Cardiopulmonary exam reveals a minor flow murmur. Neurological exam reveals cranial nerves II-XII as grossly intact with mild narrowing of the patient's visual fields. The patient's gait is stable, and he is able to jump up and down. Which of the following is the most likely direct cause of this patient's presentation?
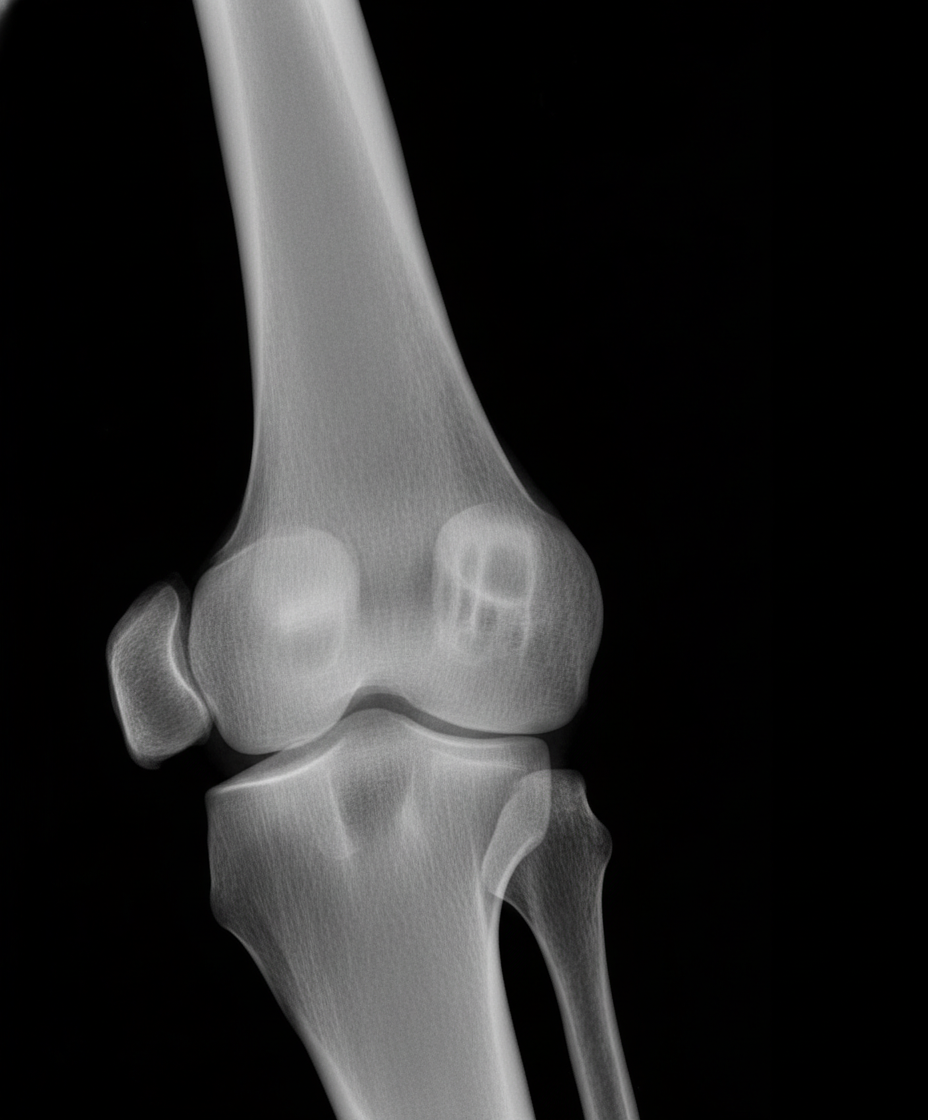
A 24-year-old man is brought to the physician because of increasing pain and swelling of the left knee for 2 months. The pain has awoken him from his sleep on multiple occasions. He tried ibuprofen but has had no relief of his symptoms. There is no family or personal history of serious illness. Vital signs are within normal limits. On examination, the left knee is mildly swollen and tender; range of motion is limited by pain. An x-ray of the left knee is shown. Which of the following is the most likely diagnosis?
A 55-year-old female presents to her primary care physician complaining of a mass in her mid-thigh. The mass has grown slowly over the past six months and is not painful. The patient’s past medical history is notable for hypertension and hyperlipidemia. She takes lisinopril and rosuvastatin. On examination, there is a firm, immobile mass on the medial aspect of the distal thigh. She has full range of motion and strength in her lower extremities and patellar reflexes are 2+ bilaterally. A biopsy of the mass reveals multiple pleomorphic smooth muscle cells with nuclear atypia. The patient subsequently initiates radiation therapy with plans to undergo surgical resection. This tumor will most strongly stain for which of the following?
A 71-year-old man presents to the primary care clinic with non-specific complaints of fatigue and malaise. His past medical history is significant for diabetes mellitus type II, hypertension, non-seminomatous testicular cancer, and hypercholesterolemia. He currently smokes 1 pack of cigarettes per day, drinks a glass of wine per day, and he currently denies any illicit drug use. His vital signs include: temperature, 36.7°C (98.0°F); blood pressure, 126/74 mm Hg; heart rate, 87/min; and respiratory rate, 17/min. On examination, his physician notices cervical and inguinal lymphadenopathy bilaterally, as well as splenomegaly. The patient comments that he has lost 18.1 kg (40 lb) over the past 6 months without a change in diet or exercise, which he was initially not concerned about. The physician orders a complete blood count and adds on flow cytometry. Based on his age and overall epidemiology, which of the following is the most likely diagnosis?
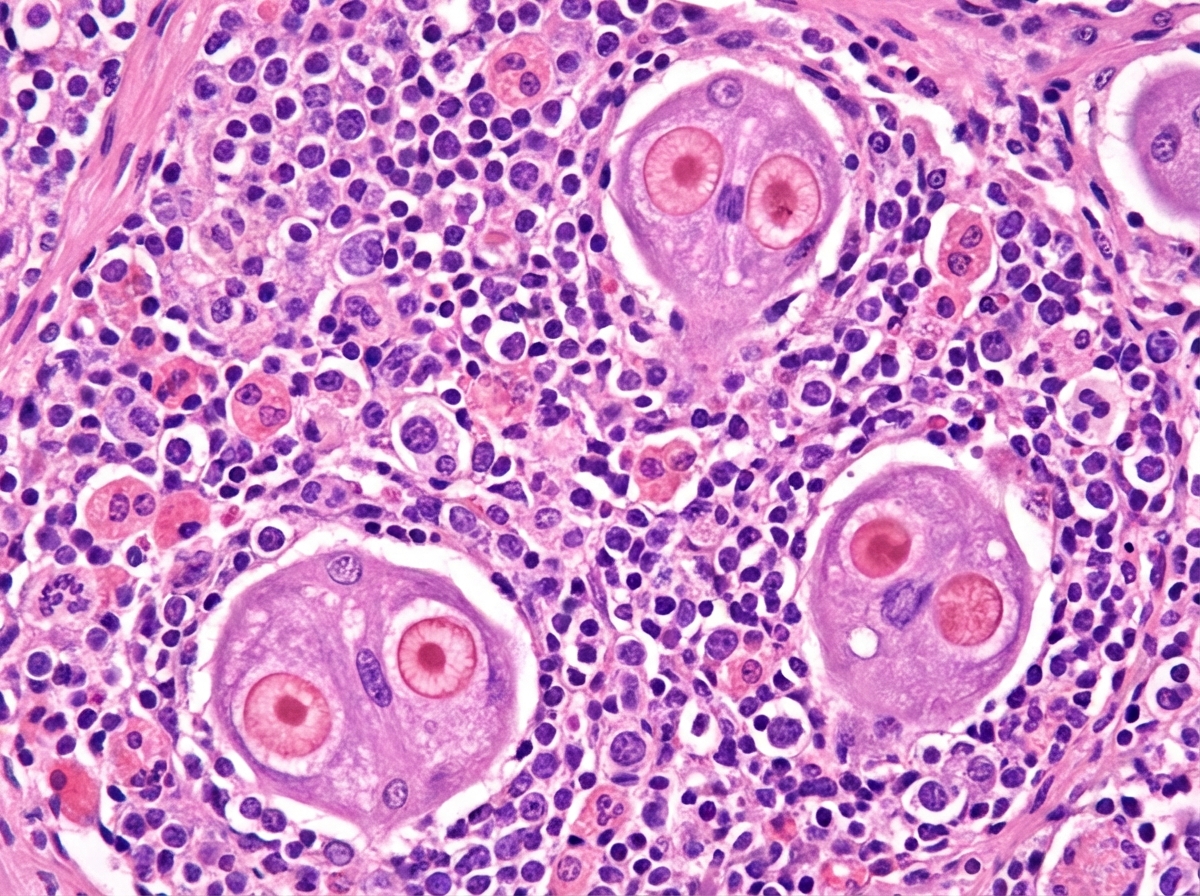
A 53-year-old man comes to the physician for recurring fever and night sweats for the past 6 months. The fevers persist for 7 to 10 days and then subside completely for about a week before returning again. During this period, he has also noticed two painless lumps on his neck that have gradually increased in size. Over the past year, he has had an 8.2-kg (18.1 lbs) weight loss. Two years ago, he had a severe sore throat and fever, which was diagnosed as infectious mononucleosis. He has smoked a pack of cigarettes daily for the past 10 years. He does not drink alcohol. His job involves monthly international travel to Asia and Africa. He takes no medications. His temperature is 39°C (102.2°F), pulse is 90/min, respirations are 22/min, and blood pressure is 105/60 mm Hg. Physical examination shows 2 enlarged, nontender, fixed cervical lymph nodes on each side of the neck. Microscopic examination of a specimen obtained on biopsy of a cervical lymph node is shown. Which of the following additional findings is most likely present in this patient?
A 64-year-old male presents to his primary care physician. Laboratory work-up and physical examination are suggestive of a diagnosis of prostatic adenocarcinoma. A tissue biopsy is obtained, which confirms the diagnosis. Which of the following is indicative of metastatic disease?
A 70-year-old man comes to the physician because of right-sided back pain, red urine, and weight loss for the last 4 months. He has smoked one pack of cigarettes daily for 40 years. A CT scan of the abdomen shows a large right-sided renal mass. Biopsy of the mass shows polygonal clear cells filled with lipids. Which of the following features is necessary to determine the tumor grade in this patient?
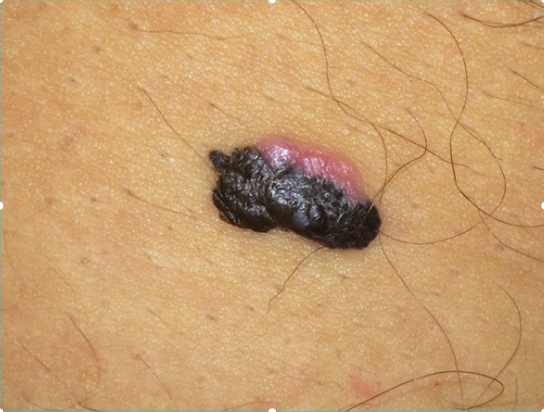
A 63-year-old man comes to the physician for the evaluation of a skin lesion on his chest. He first noticed the lesion 2 months ago and thinks that it has increased in size since then. The lesion is not painful or pruritic. He has type 2 diabetes mellitus, hypercholesterolemia, and glaucoma. The patient has smoked 1 pack of cigarettes daily for the last 40 years and drinks two to three beers on the weekend. Current medications include metformin, atorvastatin, topical timolol, and a multivitamin. Vital signs are within normal limits. The lesion is partly elevated on palpation and does not change its form on pinching. A photograph of the lesion is shown. Which of the following is the most likely diagnosis?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
