Neoplasia — MCQs

On this page
A 41-year-old man with HIV comes to the physician because of rectal bleeding and itching for 2 weeks. During this period, he has also had pain with defecation. Four months ago, he was diagnosed with anogenital warts that were treated with cryotherapy. Over the past year, he has been sexually active with 3 male partners. He uses condoms inconsistently. Current medications are zidovudine, emtricitabine, and efavirenz. Digital rectal examination and anoscopy show an exophytic mass on the anal margin that is protruding into the anal canal. The mass is tender to palpation and bleeds easily on contact. Laboratory studies show a leukocyte count of 7,600/mm3 and a CD4+ T-lymphocyte count of 410/mm3 (N ≥ 500). A biopsy specimen of the lesion shows a well-differentiated squamous cell carcinoma. Which of the following cellular processes was most likely involved in the pathogenesis of this patient's malignancy?
A 5-year-old male is brought to his pediatrician after recurrent, prolonged upper respiratory infections over a period of several months. Physical exam reveals petechiae on the patient's legs and arms. Laboratory studies show hemoglobin: 10 g/dL, platelet count: 35,000/mm^3, leukocyte count: 6,600/mm^3. A bone marrow aspiration shows an abundance of lymphoblasts indicative of acute lymphoblastic leukemia (ALL). Positive immunostaining for which of the following would support a diagnosis of precursor B-cell leukemia?
A 65-year-old man comes to the physician for evaluation of a neck mass and weight loss. He first noticed the growing mass 2 months ago. The mass is not painful. He also has decreased appetite and intermittent abdominal pain. He has lost 10 kg (22 lb) of weight over the past 3 months. Sometimes, he wakes up in the morning drenched in sweat. He takes daily over-the-counter multivitamins. He appears pale. His pulse is 65/min, blood pressure is 110/70 mm Hg, and temperature is 38.1°C (100.6°F). Physical exam shows a painless, golf ball-sized mass in the anterior triangle of the neck. A biopsy shows large cells with a bilobed nucleus that are CD15-positive and CD30-positive. Laboratory analysis of serum shows a calcium level of 14.5 mg/dL and a parathyroid hormone level of 40 pg/mL. Which of the following is the most likely explanation of this patient's laboratory findings?
A 7-year-old boy presents to the ER with progressive dysphagia over the course of 3 months and a new onset fever for the past 24 hours. The temperature in the ER was 39.5°C (103.1°F). There are white exudates present on enlarged tonsils (Grade 2). Routine blood work reveals a WBC count of 89,000/mm3, with the automatic differential yielding a high (> 90%) percentage of lymphocytes. A peripheral blood smear is ordered, demonstrating the findings in the accompanying image. The peripheral smear is submitted to pathology for review. After initial assessment, the following results are found on cytologic assessment of the cells: TdT: positive CALLA (CD 10): positive Which of the following cell markers are most likely to be positive as well?
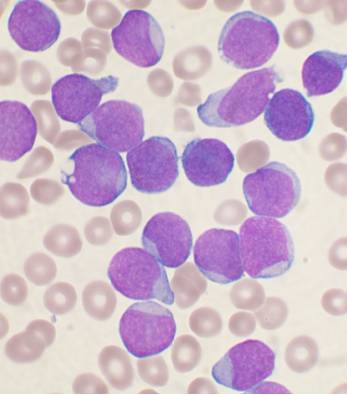
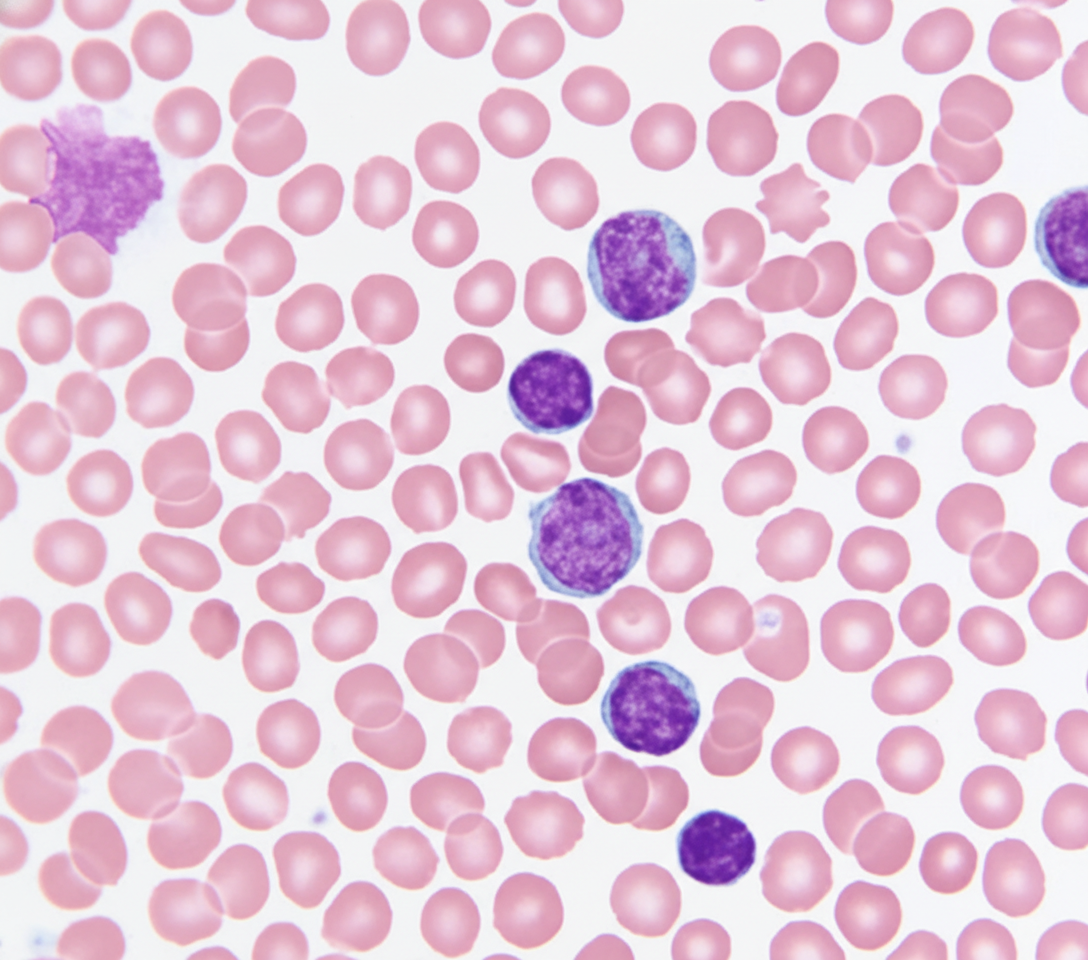
A 69-year-old Caucasian man presents for a routine health maintenance examination. He feels well. He has no significant past medical history. He takes aspirin for the occasional headaches that he has had for over several years. He exercises every day and does not smoke. His father was diagnosed with a hematologic malignancy at 79 years old. The patient’s vital signs are within normal limits. Physical examination shows no abnormalities. The laboratory test results are as follows: Hemoglobin 14.5 g/dL Leukocyte count 62,000/mm3 Platelet count 350,000/mm3 A peripheral blood smear is obtained (shown on the image). Which of the following best explains these findings?
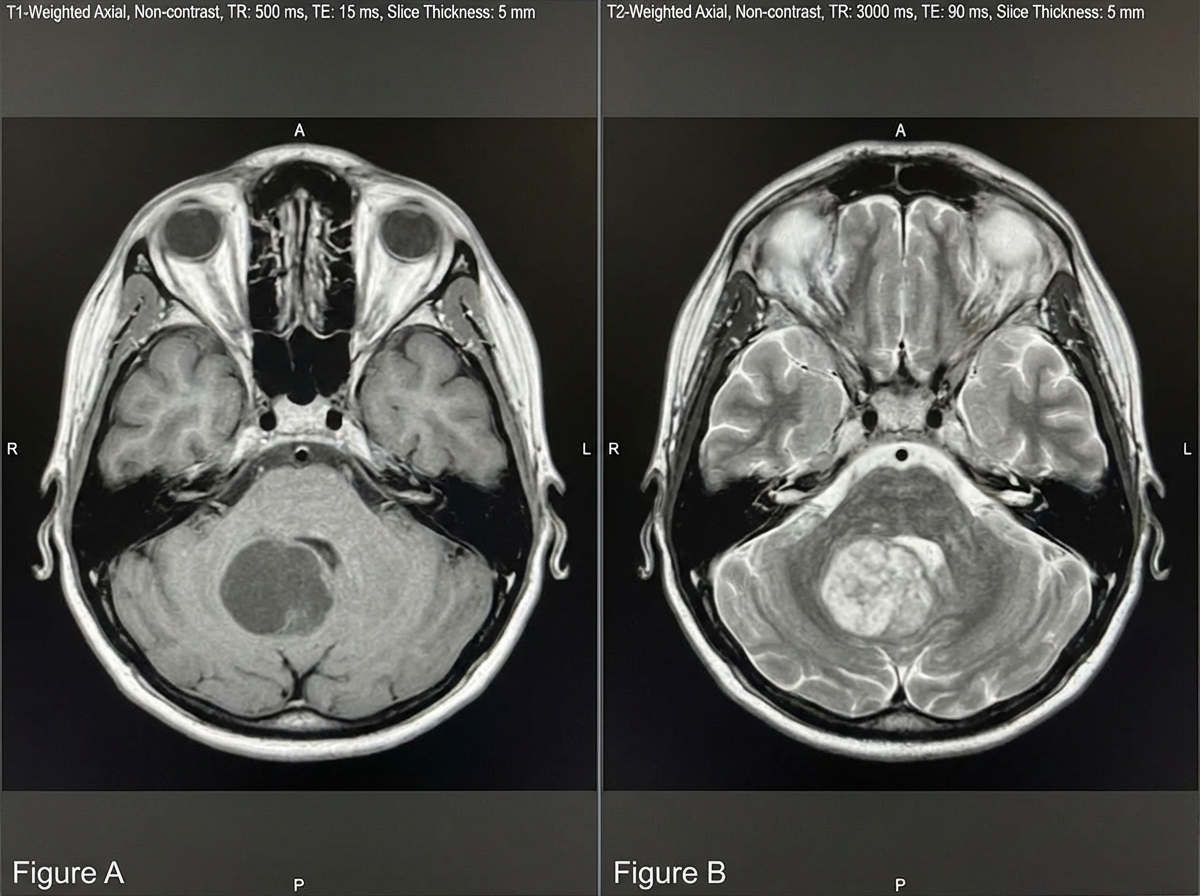
A 6-year-old boy is brought in by his mother to his pediatrician for headache and nausea. His headaches began approximately 3 weeks ago and occur in the morning. Throughout the 3 weeks, his nausea has progressively worsened, and he had 2 episodes of emesis 1 day ago. On physical exam, cranial nerves are grossly intact, and his visual field is intact. The patient has a broad-based gait and difficulty with heel-to-toe walking, as well as head titubation. Fundoscopy demonstrates papilledema. A T1 and T2 MRI of the brain is demonstrated in Figures A and B, respectively. Which of the following is most likely the diagnosis?
A 55-year-old male presents with complaints of intermittent facial flushing. He also reports feeling itchy after showering. On review of systems, the patient says he has been having new onset headaches recently. On physical exam, his vital signs, including O2 saturation, are normal. He has an abnormal abdominal mass palpable in the left upper quadrant. A complete blood count reveals: WBCs 6500/microliter; Hgb 18.2 g/dL; Platelets 385,000/microliter. Which of the following is most likely responsible for his presentation?
A 53-year-old man is being evaluated for a 3-week history of fatigue, difficulty to concentrate, dyspnea with exertion, dizziness, and digital pain that improves with cold. He has smoked half a pack of cigarettes a day since he was 20. His current medical history involves hypertension. He takes enalapril daily. The vital signs include a blood pressure of 131/82 mm Hg, a heart rate of 95/min, and a temperature of 36.9°C (98.4°F). On physical examination, splenomegaly is found. A complete blood count reveals thrombocytosis of 700,000 cells/μL. Lab work further shows decreased serum iron, iron saturation, and serum ferritin and increased total iron binding capacity. A blood smear reveals an increased number of abnormal platelets, and a bone marrow aspirate confirmed the presence of dysplastic megakaryocytes. A mutation on his chromosome 9 confirms the physician's suspicion of a certain clonal myeloproliferative disease. The patient is started on hydroxyurea. What is the most likely diagnosis?
A 43-year-old woman presents to your clinic for the evaluation of an abnormal skin lesion on her forearm. The patient is worried because her mother passed away from melanoma. You believe that the lesion warrants biopsy for further evaluation for possible melanoma. Your patient is concerned about her risk for malignant disease. What is the most important prognostic factor of melanoma?
An investigator studying targeted therapy in patients with gastrointestinal stromal tumors requires a reliable test to determine the spatial distribution of CD117-positive cells in biopsy specimens. Which of the following is the most appropriate test?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
