Neoplasia — MCQs

On this page
A 70-year-old woman presents with a 2-week history of severe fatigue. Over the past month, she has unintentionally lost 2 kg (4.4 lb). Three years ago, she was diagnosed with myelodysplastic syndrome. Currently, she takes no medications other than aspirin for occasional knee pain. She does not smoke or drink alcohol. Her vital signs are within the normal range. On physical examination, her conjunctivae are pale. Petechiae are present on the distal lower extremities and on the soft and hard palates. Palpation reveals bilateral painless cervical lymphadenopathy. Examination of the lungs, heart, and abdomen shows no abnormalities. Laboratory studies show: Hemoglobin 9 g/dL Mean corpuscular volume 90 μm3 Leukocyte count 3000/mm3 Platelet count 20,000/mm3 A Giemsa-stained peripheral blood smear is shown in the image. Which of the following best explains these findings?
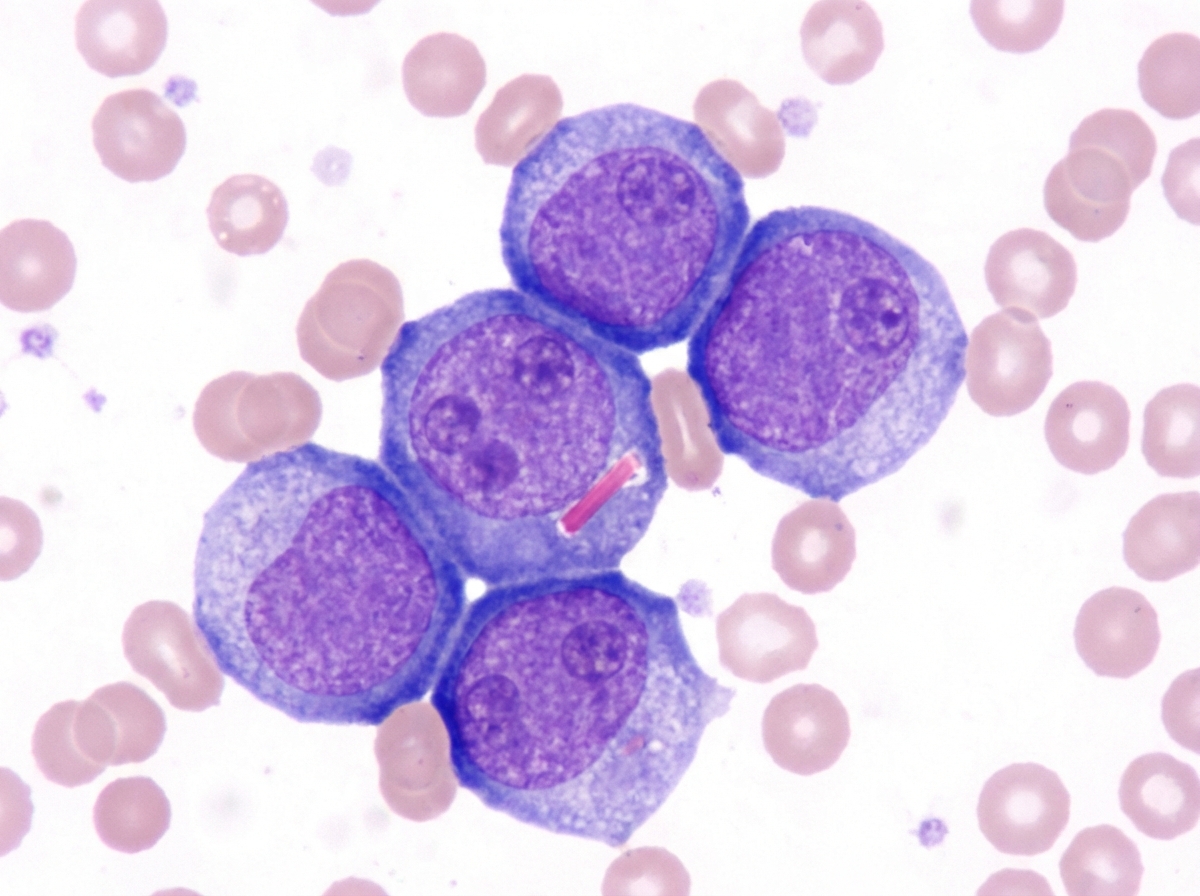
A 17-year-old boy is brought to the physician because of progressive right knee pain for the past 3 months. He reports that the pain is worse at night and while doing sports at school. He has not had any trauma to the knee or any previous problems with his joints. His vital signs are within normal limits. Examination of the right knee shows mild swelling and tenderness without warmth or erythema; the range of motion is limited. He walks with an antalgic gait. Laboratory studies show an alkaline phosphatase of 180 U/L and an erythrocyte sedimentation rate of 80 mm/h. An x-ray of the right knee is shown. Which of the following is the most likely diagnosis?
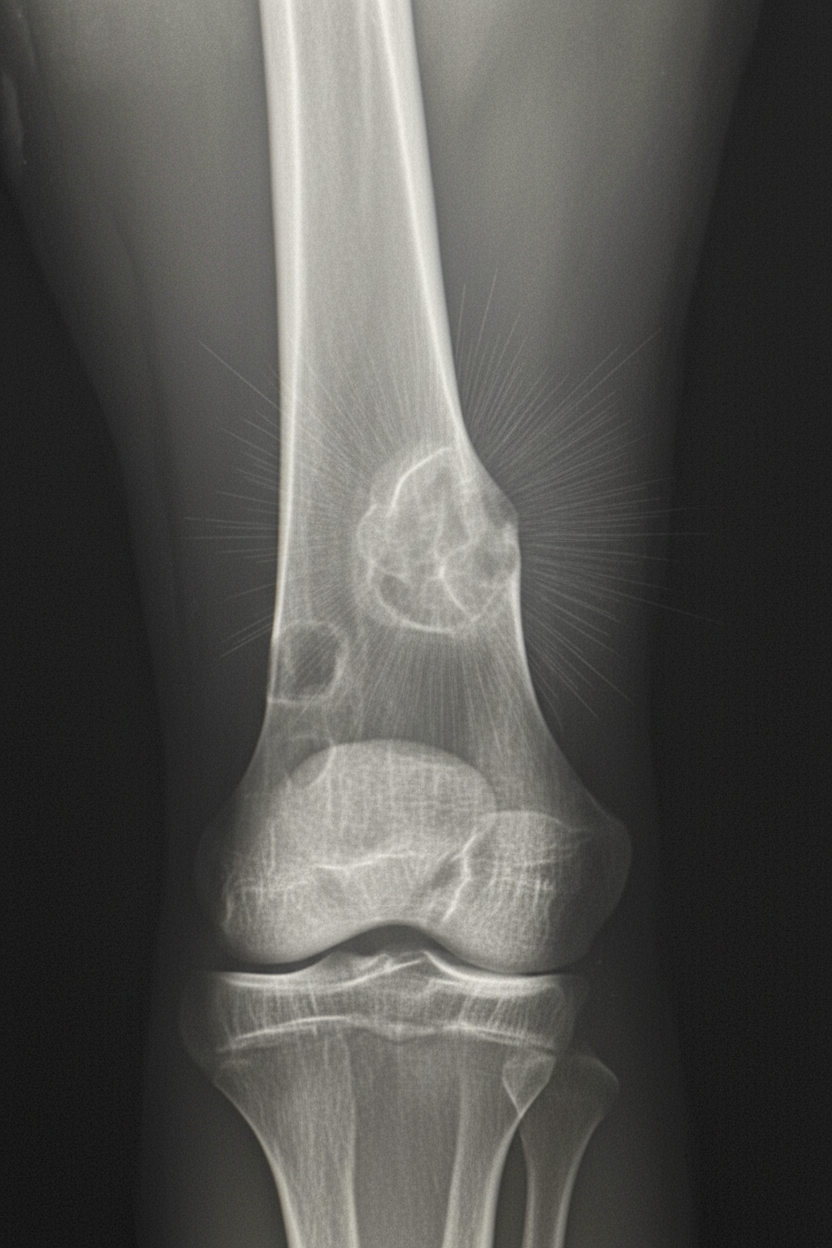
A 6-year-old boy presents to your office with loss of his peripheral vision. His mother discovered this because he was almost struck by a vehicle that "he couldn't see at all". In addition, he has been complaining of a headache for the last several weeks and had an episode of vomiting 2 days ago. He has a family history of migraines in his mother and grandmother. He is currently in the 80th percentile for height and weight. On physical exam his temperature is 99°F (37.2°C), blood pressure is 110/75 mmHg, pulse is 100/min, respirations are 19/min, and pulse oximetry is 99% on room air. He is uncooperative for the rest of the physical exam. During workup, a lesion is found in this patient. Which of the following would most likely be seen during histopathologic analysis?
A 62-year-old man presents to his primary care physician because of abdominal pain that started after he went camping several months ago and drank from a mountain stream. This past year, he also went on a trip around the world, eating local foods at each stop. Furthermore, he has had a history of cholelithiasis and had his gallbladder removed 3 years ago. Otherwise, his medical history is significant for well-controlled hypertension and diabetes. Based on clinical suspicion, an endoscopy and biopsy was performed showing a mix of mononuclear cells and a motile, urease-positive, oxidase-positive, spiral shaped organism. The changes seen on biopsy in this patient most likely predispose him to which of the following pathologies?
A 22-year-old woman comes to the physician because of hearing loss and unsteadiness while standing and walking for the past 2 months. She needs support from a wall to prevent herself from falling. She has not had any recent injuries and has no history of serious illness. Vital signs are within normal limits. Examination shows an unsteady gait. She sways when asked to stand upright with her feet together. She is unable to hear fingers rubbing next to her ears or repeat words whispered in her ears bilaterally. An MRI of the brain shows a 3-cm tumor in the right cerebellopontine angle and a 4.5-cm tumor in the left cerebellopontine angle. This patient is most likely to develop which of the following in the future?
A 42-year-old woman presents to her primary care physician with fatigue. She reports that over the past 2 months, she has felt increasingly tired despite no changes in her diet or exercise. Her past medical history is notable for obesity, seasonal allergies, and hypertension. She takes ranitidine as needed and hydrochlorothiazide daily. Her family history is notable for colorectal cancer in her mother and maternal uncle, endometrial cancer in her maternal aunt, and ovarian cancer in her maternal grandmother. Her temperature is 98.8°F (37.1°C), blood pressure is 132/71 mmHg, pulse is 89/min, and respirations are 17/min. On exam, she has conjunctival pallor. A stool sample is hemoccult positive. A colonoscopy reveals a fungating hemorrhagic mass in the ascending colon. Which of the following processes is likely impaired in this patient?
A 65-year-old man with a 40-pack-year smoking history presents with hemoptysis and a persistent cough. Chest CT shows a 3.5 cm centrally located mass in the right main bronchus. Positron emission tomography confirms a malignant nodule. Bronchoscopy with transbronchial biopsy is performed and a specimen sample of the nodule is sent for frozen section analysis. The tissue sample is most likely to show which of the following tumor types?
A 70-year-old man is brought to the emergency department by his wife because of progressive confusion for the past 2 weeks. He has also had a 4.5-kg (10-lb) weight loss and fatigue during the last 6 months. Physical examination shows enlarged lymph nodes in the right axilla and faint expiratory wheezing in the right middle lung field. He is only oriented to person. Serum studies show a sodium concentration of 125 mEq/L and increased antidiuretic hormone concentration. An x-ray of the chest shows a right-sided hilar mass with mediastinal fullness. A biopsy of the hilar mass is most likely to show cells that stain positive for which of the following?
A 61-year-old male presents to the ER with abdominal discomfort and malaise over the past 2 weeks. He states he is married and monogamous. He has a temperature of 39.4°C (102.9°F) and complains of night sweats as well. On physical exam, he has an enlarged spleen with mild tenderness and pale nail beds. There is mild tonsillar erythema and the pulmonary exam demonstrates scattered crackles. A complete blood count demonstrates anemia, thrombocytopenia, and leukocytosis with lymphocytic predominance. A bone marrow aspiration is scheduled the next morning based on the peripheral blood smear findings but was inconclusive due to a low yield. The patient was admitted to the hospital due to the anemia and given a transfusion of packed red blood cells and wide spectrum antibiotics. He is released home the next day with instructions for primary care follow-up. Which of the following laboratory findings is most reliably positive for the primary cause of this illness?
A 4-year-old girl is brought to the physician because of a 3-week history of generalized fatigue and easy bruising. During the past week, she has also had fever and severe leg pain that wakes her up at night. Her temperature is 38.3°C (100.9°F), pulse is 120/min, and respirations are 30/min. Examination shows cervical and axillary lymphadenopathy. The abdomen is soft and nontender; the liver is palpated 3 cm below the right costal margin, and the spleen is palpated 2 cm below the left costal margin. Laboratory studies show: Hemoglobin 10.1 g/dL Leukocyte count 63,000/mm3 Platelet count 27,000/mm3 A bone marrow aspirate predominantly shows immature cells that stain positive for CD10, CD19, and TdT. Which of the following is the most likely diagnosis?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
