Neoplasia — MCQs

On this page
A previously healthy 61-year-old man comes to the physician because of a 3-month history of intermittent fever, easy fatiguability, and a 4.4-kg (9.7-lb) weight loss. Physical examination shows conjunctival pallor. The spleen is palpated 5 cm below the left costal margin. Laboratory studies show a leukocyte count of 75,300/mm3 with increased basophils, a platelet count of 455,000/mm3, and a decreased leukocyte alkaline phosphatase score. A peripheral blood smear shows increased numbers of promyelocytes, myelocytes, and metamyelocytes. Which of the following is the most likely diagnosis?
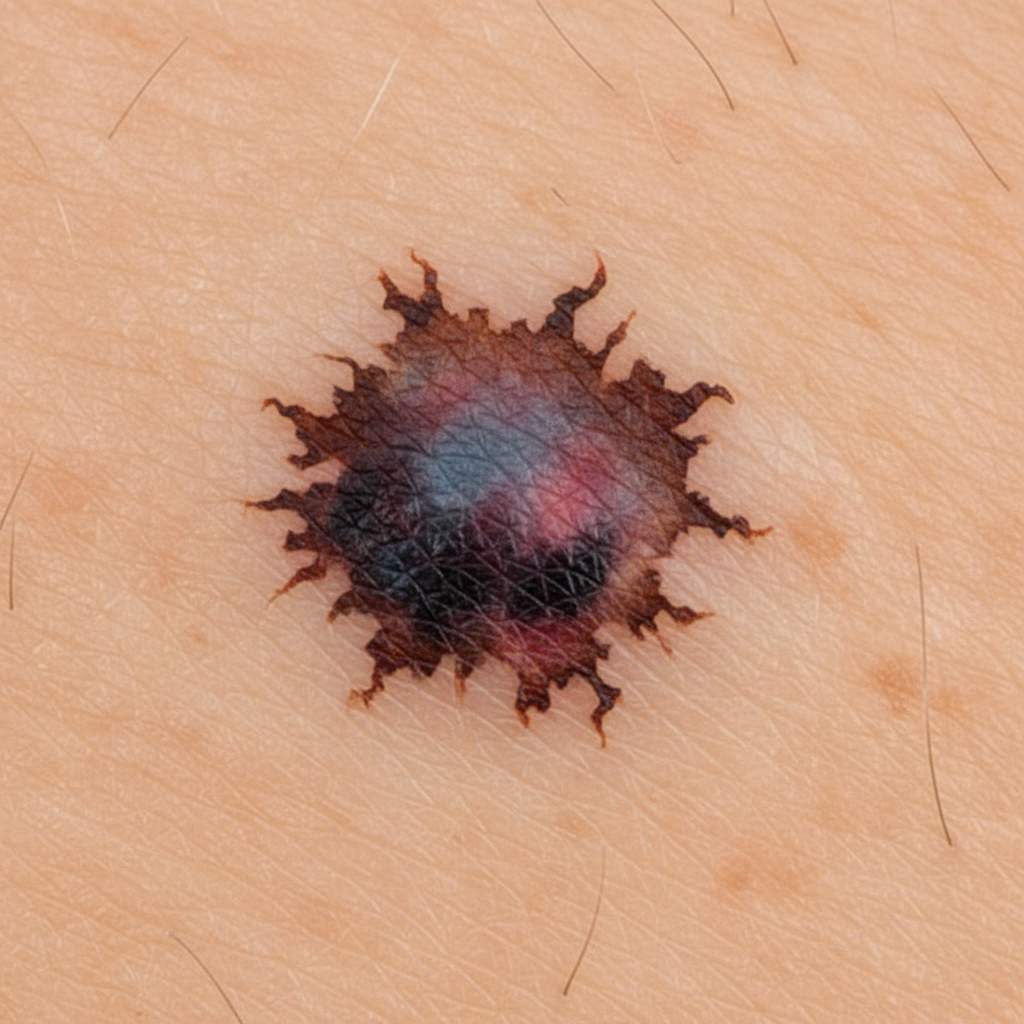
A 52-year-old Caucasian male presents to your office with an 8 mm dark lesion on his back. The lesion, as seen below, has irregular borders and marked internal color variation. Upon excisional biopsy, the presence of which of the following would best estimate the risk of metastasis in this patient's lesion?
A 24-year-old man comes to the physician because of 2 episodes of bleeding from the rectum over the past month. The patient’s father died of colon cancer at the age of 42. The patient has no history of any serious illness and takes no medications. He does not smoke. His vital signs are within normal limits. Physical examination shows a small hard mass over the right mandible that is nontender and fixed to the underlying bone. A similarly hard and painless 5 × 5 mass is palpated over the rectus abdominis muscle. On examination of the rectum, a polypoid mass is palpated at fingertip. Proctosigmoidoscopy shows numerous polyps. Which of the following best explains these findings?
A 53-year-old female visits her physician with watery diarrhea and episodic flushing. The patient reports that she is often short of breath, and a pulmonary exam reveals bilateral wheezing. A CT scan shows a mass in the terminal ileum. 24-hour urine collection shows abnormally elevated 5-hydroxyindoleacetic acid (HIAA) levels. Ultrasound demonstrates a tricuspid valve with signs of fibrosis with a normal mitral valve. A metastatic disease to which organ is most commonly associated with the patient's syndrome?
A 14-year-old boy presents to his pediatrician with a 5-day history of abdominal pain and bloody stool. He denies having a fever and says that he has not experienced any other symptoms associated with the abdominal pain. He has no past medical history and does not take any medications or supplements. His family history is significant for a grandfather who developed Alzheimer disease at age 80 and a cousin who died at age 21 from colon cancer. Physical exam is unremarkable. Based on clinical suspicion a colonoscopy is obtained showing hundreds of small polyps in the colon. A mutation of a gene on which of the following chromosomes is most likely responsible for this patient's symptoms?
A 72-year-old and his caregiver present for a follow-up after a transthoracic needle biopsy of one of the large lesions in his chest was reported as non-small cell carcinoma of the lung. Previously, a chest CT revealed numerous nodules in the lungs bilaterally. The chest CT was ordered after the patient experienced a persistent cough with hemoptysis and a history of multiple episodes of pneumonia over the past year. The patient has a history of dementia and is a poor historian. The caregiver states that the patient has no history of smoking and that he was a lawyer before he retired, 10 years ago. The caregiver can only provide a limited medical history, but states that the patient sees another doctor “to monitor his prostate”. Which of the following is true regarding the pathogenesis of the nodules seen in this patient?
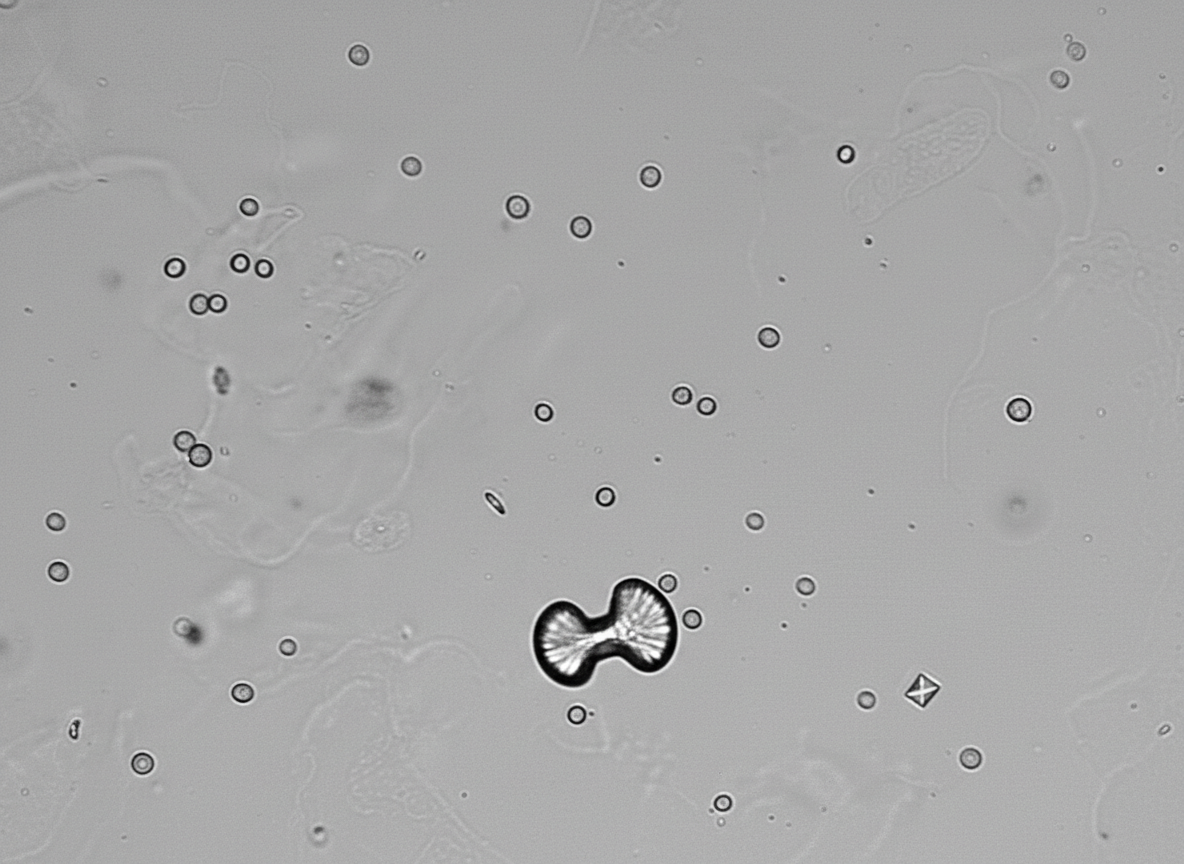
A 34-year-old patient with a history of anxiety, chronic constipation, chronic headaches, and chronic hypertension presents to the emergency room with severe right flank pain radiating to his scrotum. A urinalysis with stone analysis is performed and the results are shown in figure A. Prior to discharge, it is noted that the patients BP is still 170/110 mmHg. Furthermore, his calcium and PTH levels were both found to be increased. Which of the following representative histology slides of thyroid tissue represents a potential complication of the patients condition?
An 82-year-old man is brought to the emergency department after he was found down by his daughter. On presentation, he is alert and oriented with no obvious signs of trauma. He says that he felt lightheaded shortly before passing out and that he has been feeling extremely fatigued over the last few weeks. He has a known diagnosis of colorectal adenocarcinoma and had it surgically removed 2 months ago; however, recently he has been feeling increasingly short of breath. He has a 60-pack-year smoking history and drinks 2-3 beers a night. He worked as an insulation technician and shipyard laborer for 40 years prior to retiring at age 65. Radiographs reveal approximately a dozen new nodules scattered throughout his lungs bilaterally. Biopsy of these lesions would most likely reveal which of the following?
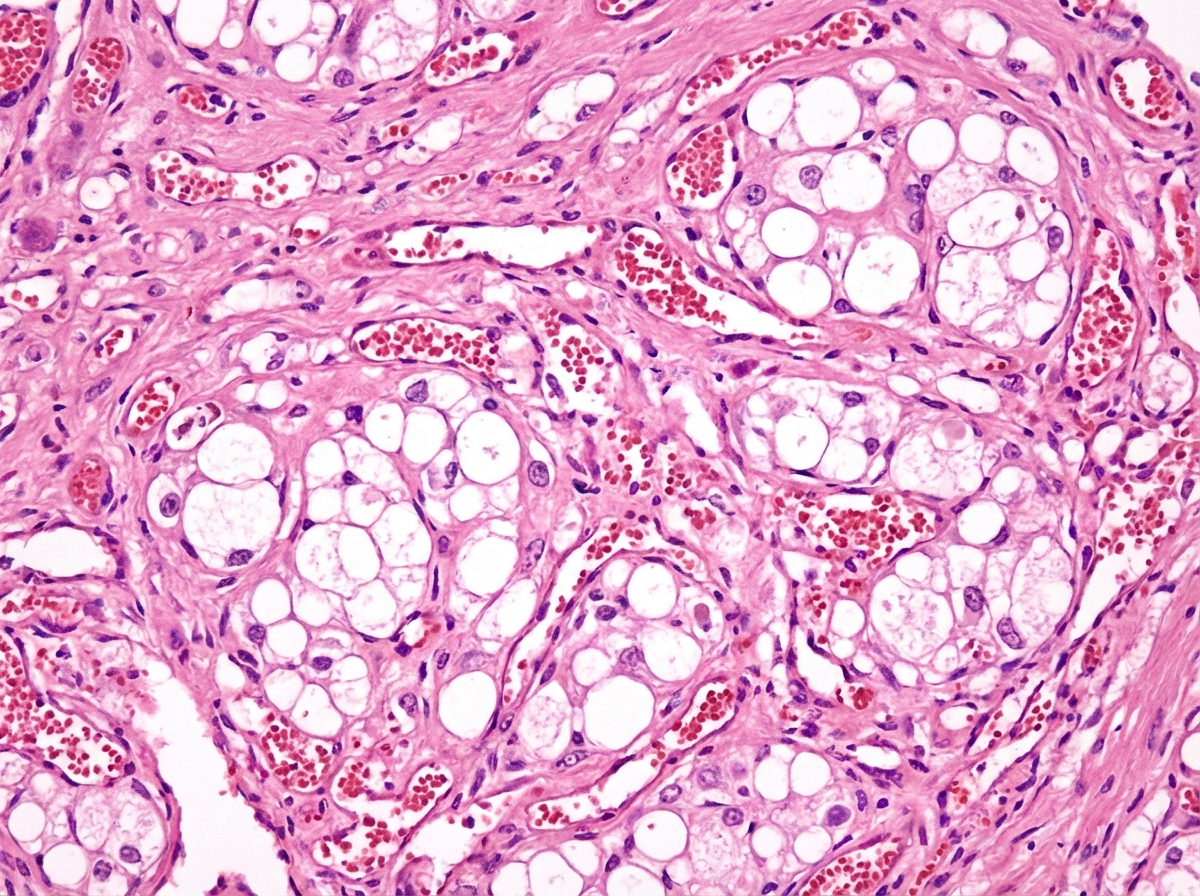
A 22-year-old man comes to the physician because of headaches and blurry vision for the past 6 months. He also reports frequent episodes of vomiting over the last month. His father has died of renal cell carcinoma at the age of 37 years. Examination shows 20/40 vision bilaterally. Fundoscopic examination shows bilateral optic disc swelling and growth of capillary vessels in the temporal peripheral retina. An MRI of the brain shows an infratentorial mass. The patient undergoes surgical resection of the mass. A photomicrograph of the resected specimen is shown. Which of the following is the most likely diagnosis?
A 16-year-old boy is brought to the physician because of a lesion that has been growing on his jaw over the past several months. He recently immigrated to the USA from Kenya with his family. Physical examination shows a 3-cm solid mass located above the left mandible. There is cervical lymphadenopathy. Biopsy of the mass shows sheets of lymphocytes and interspersed reactive histiocytes with abundant, clear cytoplasm and phagocytosed debris. Which of the following mechanisms is most likely directly responsible for the malignant transformation of this patient's cells?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
