Neoplasia — MCQs

On this page
A 54-year-old woman comes to the physician because of an ulcer on her left ankle for 6 years. She has had multiple ulcers over her left lower extremity during this period that have subsided with wound care and dressing. She has type 2 diabetes mellitus and gastroesophageal reflux disease. Current medications include metformin, sitagliptin, and omeprazole. She appears anxious. She is 162 cm (5 ft 4 in) tall and weighs 89 kg (196 lb); BMI is 34 kg/m2. Vital signs are within normal limits. Examination shows a 7.5-cm (3-in) ulcer with elevated, indurated margins and a necrotic floor above the left medial malleolus. There are multiple dilated, tortuous veins along the left lower extremity. There is 2+ pretibial edema of the lower extremities bilaterally. The skin around the left ankle appears darker than the right and there are multiple excoriation marks. Cardiopulmonary examination shows no abnormalities. Which of the following is the most appropriate next step in management of this patient's current condition?
A 44-year-old woman presents to the outpatient infectious disease clinic. She has a known history of HIV, well-controlled on HAART for the past 8 years. She currently has no additional significant medical conditions. She feels well and a physical examination is within normal limits. She denies any current tobacco use, alcohol use, or illicit drug use, although she has a history of heroin use (injection). Her vital signs include: temperature, 36.7°C (98.0°F); blood pressure, 126/74 mm Hg; heart rate, 87/min; and respiratory rate, 17/min. She has no complaints and is up to date on all of her vaccinations and preventative care. Which of the following malignancies can be seen and is often associated with AIDS?
A 70-year-old man is at his dermatologist’s office for the treatment of a severely pruritic erythroderma with scaling on his buttocks that has been slowly progressing over the past two weeks. The patient works as a truck driver and has a history of hypertension treated with enalapril. The patient reports having tried an over-the-counter cream on the rash without improvement. The vital signs are within normal range. On physical exam, he has multiple confluent and well-demarcated pink patches on his buttocks and legs with some scaling and enlarged inguinal lymph nodes. The dermatologist orders a skin biopsy that reveals Pautrier microabscesses. What is the most likely diagnosis?
A 37-year-old woman, G1P0, visits her gynecologist's office for a routine prenatal checkup. During her quadruple screening test, her alpha-fetoprotein, β-hCG, and pregnancy-associated plasma protein were all decreased. There is also evidence of increased nuchal translucency on the scanning of the male fetus. A confirmatory test indicates signs of a genetic syndrome. The woman is counseled that her child will most likely have a severe intellectual disability. Physical features of this condition include polydactyly, cleft palate, micrognathia and clenched fists. This genetic condition also affects the formation of the brain and can lead to stillbirth. Most babies do not survive beyond the first year of life. Which of the following is responsible for this type of genetic syndrome?
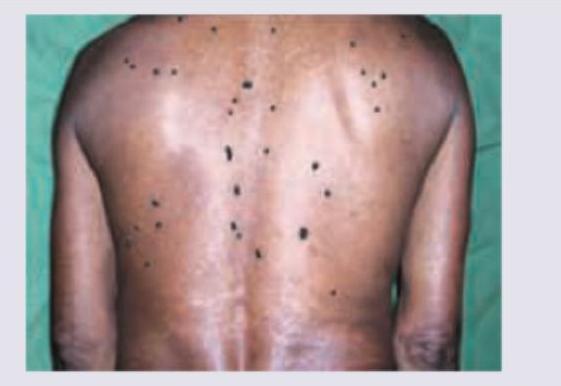
A 32-year-old woman comes to the physician for a routine examination. She has no history of serious medical illness. She appears well. Physical examination shows several hundred pigmented lesions on the back and upper extremities. A photograph of the lesions is shown. The remainder of the examination shows no abnormalities. This patient is at increased risk of developing a tumor with which of the following findings?
A 35-year-old woman comes to the physician because of a 2-month history of vaginal bleeding after intercourse. Menarche occurred at the age of 13 years and menses occur at regular 28-day intervals. Gynecologic examination shows an irregular lesion at the cervical os. Histological evaluation of a cervical biopsy specimen obtained on colposcopy confirms a diagnosis of in-situ cervical cancer. This cancer is most likely derived from which of the following types of cells?
A 32-year-old man presents to the emergency room for a generalized tonic-clonic seizure. After stabilizing the patient, a full radiologic evaluation reveals multiple contrast-enhancing lesions in the brain, lungs, and liver. According to his wife, he lost several pounds in the last few months. The medical history is relevant for cryptorchidism, with abdominal testes that were surgically transferred to the scrotum just before he turned 1-year old. His lab investigation reveals: α-fetoprotein: 9 ng/mL (normal values < 10 ng/mL) Human chorionic gonadotropin: 1,895 IU/L (normal values < 0.5 IU/L) Which of the following microscopic features best describes the lesions seen in this patient's imaging study?
A 65-year-old man presents with complaints of weakness and swollen gums for the past 3 weeks. He also says he cut his finger while cooking, and the bleeding took more than 10 minutes to stop. He has a family history of diabetes mellitus type 2 and prostate cancer. Current medications are multivitamin. His blood pressure is 122/67 mm Hg, the respiratory rate is 13/min, and the temperature is 36.7°C (98.0°F). On physical examination, the patient seems pale and lethargic. On cardiac exam, a pulmonary valve flow murmur is heard. There is significant hepatosplenomegaly present, and several oral mucosal petechiae in the oral cavity are noted. Gum hypertrophy is also present. A peripheral blood smear reveals myeloperoxidase-positive cells and Auer Rods. A bone marrow biopsy shows > 30% of blast cells. Which of the following chromosomal abnormalities is associated with this patient’s most likely diagnosis?
A 60-year-old man presents to your office because he noticed a "weird patch" on the floor of his mouth. He states that he noticed it a few months ago, but did not report it because it did not hurt. However, he is concerned because it has not regressed and seems to have changed in shape. On examination, you notice the patient has poor dentition and he admits to using chewing tobacco daily. The patch on the floor of his mouth is red with irregular borders. Which of the following would be an appropriate way to counsel this patient on his current condition?
A 47-year-old female comes to the emergency department because of increasing back pain for the past 2 weeks. She is unable to perform her daily chores. One month ago, she fell and hurt her back while working outside in the garden. The pain subsided with over-the-counter acetaminophen. She underwent a left mastectomy 1 year ago for breast cancer. She has type 2 diabetes mellitus. Current medications include metformin, sitagliptin, and a multivitamin. She appears uncomfortable. Her temperature is 38.9°C (102.0°F), pulse is 101/min, and blood pressure is 110/80 mm Hg. Examination of the back shows thoracic vertebral tenderness. She has mild stiffness on neck flexion. Muscle strength is decreased in the lower extremities. Deep tendon reflexes are 2+ bilaterally. Sensation to pain, fine touch, temperature, and proprioception is intact. Her hemoglobin concentration is 13.1 g/dL and leukocyte count is 19,300/mm3. Which of the following is the most appropriate next step in management?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
