Neoplasia — MCQs

On this page
A 75-year-old man presents to the physician with a complaint of persistent back pain. The patient states that the pain has been constant and occurs throughout the day. He says that he has also been experiencing greater fatigue when carrying out his daily activities. On review of systems, the patient notes that he lost more than 10 pounds in the past month despite maintaining his usual diet and exercising less often due to his fatigue. Physical exam is notable for a systolic murmur at the right sternal border, mild crackles at the bases of both lungs, and tenderness to palpation of his lumbar spine. Laboratory values are below: Serum: Na+: 141 mEq/L Cl-: 101 mEq/L K+: 4.2 mEq/L HCO3-: 23 mEq/L BUN: 20 mg/dL Glucose: 101 mg/dL Creatinine: 1.6 mg/dL Ca2+: 12.8 mg/dL A peripheral blood smear is ordered for the patient’s work-up. Which of the following would be the most likely finding on peripheral blood smear?
A 70-year-old man presents to a medical office with painful micturition for 2 weeks. He denies any other symptoms. The past medical history is unremarkable. He has been a smoker most of his life, smoking approx. 1 pack of cigarettes every day. The physical examination is benign. A urinalysis shows an abundance of red blood cells. A cystoscopy is performed, which reveals a slightly erythematous area measuring 1.5 x 1 cm on the bladder mucosa. A biopsy is obtained and microscopic evaluation shows cells with an increased nuclear: cytoplasmic ratio and marked hyperchromatism involving the full thickness of the epithelium, but above the basement membrane. Which of the following best describes the biopsy findings?
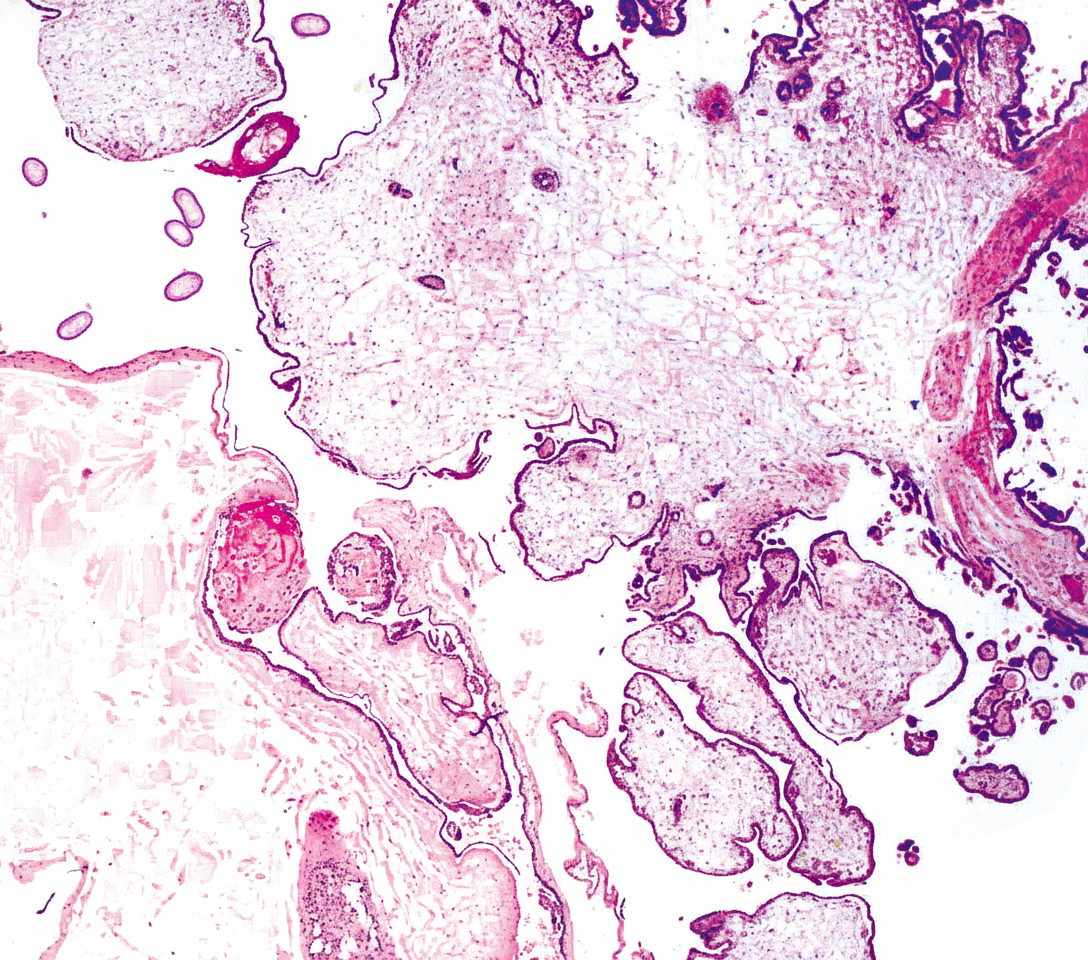
A 29-year-old female reports having a positive home pregnancy test result 9 weeks ago. She presents today with vaginal bleeding and complains of recent onset abdominal pain. Ultrasound of the patient’s uterus is included as Image A. Subsequent histologic analysis (Image B) reveals regions of both normal as well as enlarged trophoblastic villi. Which of the following is the most likely karyotype associated with this pregnancy?
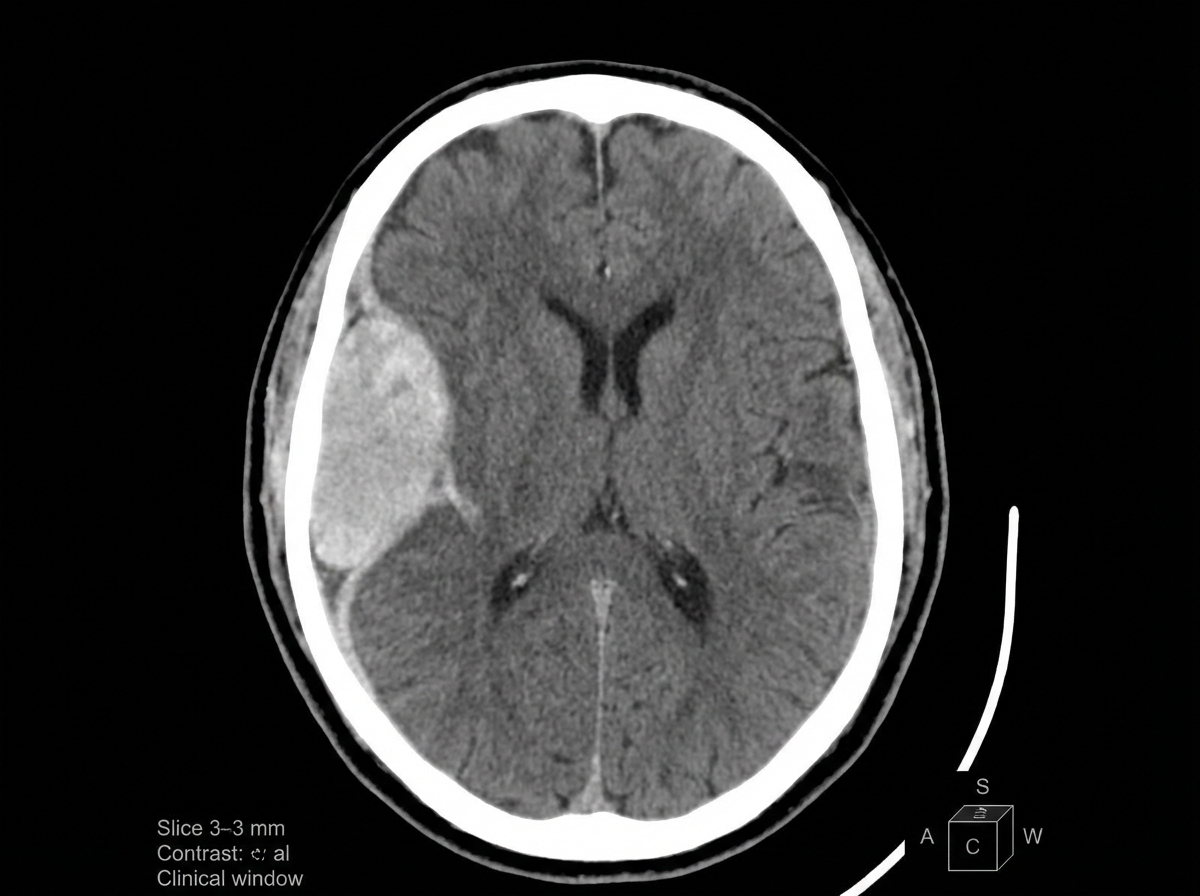
A 41-year-old woman presents to the office with a complaint of a headache for 1 month and an episode of abnormal body movement. The headaches are more severe in the morning, mostly after waking up. She doesn’t give a history of any major illness or trauma in the past. Her vital signs include: blood pressure 160/80 mm Hg, pulse 58/min, temperature 36.5°C (97.8°F), and respiratory rate 11/min. On fundoscopic examination, mild papilledema is present. Her pupils are equal and reactive to light. No focal neurological deficit can be elicited. A contrast computed tomography scan of the head is shown in the picture. Which of the following is the most likely biopsy finding in this case?
A 66-year-old woman presents to the emergency department with abdominal pain. Her symptoms began when she was eating dinner. She has a past medical history of obesity, constipation, intravenous drug use, and diabetes. The patient is instructed to be nil per os and is transferred to the surgical floor. Three days later she had a cholecystectomy and is recovering on the surgical floor. Her laboratory values are ordered as seen below. Hemoglobin: 11 g/dL Hematocrit: 33% Leukocyte count: 8,500/mm^3 with normal differential Platelet count: 197,000/mm^3 Serum: Na+: 139 mEq/L Cl-: 100 mEq/L K+: 4.3 mEq/L HCO3-: 25 mEq/L BUN: 20 mg/dL Glucose: 99 mg/dL Creatinine: 1.1 mg/dL Ca2+: 10.5 mg/dL Alkaline phosphatase: 533 U/L GGT: 50 U/L AST: 22 U/L ALT: 20 U/L The patient is currently asymptomatic and states that she feels well. Which of the following is associated with this patient's underlying condition?
A 56-year-old woman, gravida 3, para 3, comes to the physician because her left breast has become larger, hot, and itchy over the past 2 months. The patient felt a small lump in her left breast 1 year ago but did not seek medical attention at that time. She has hypertension and hyperlipidemia. Menarche was at the age of 11 years and menopause at the age of 46 years. Her mother died of breast cancer at the age of 45 years. The patient does not smoke or drink alcohol. Current medications include labetalol, simvastatin, and daily low-dose aspirin. She is 170 cm (5 ft 7 in) tall and weighs 78 kg (172 lb); BMI is 27 kg/m2. Her temperature is 37.7°C (99.9°F), pulse is 78/min, and blood pressure is 138/88 mm Hg. Examination shows large dense breasts. There is widespread erythema and edematous skin plaques over a breast mass in the left breast. The left breast is tender to touch and left-sided axillary lymphadenopathy is noted. Which of the following is the most likely diagnosis?
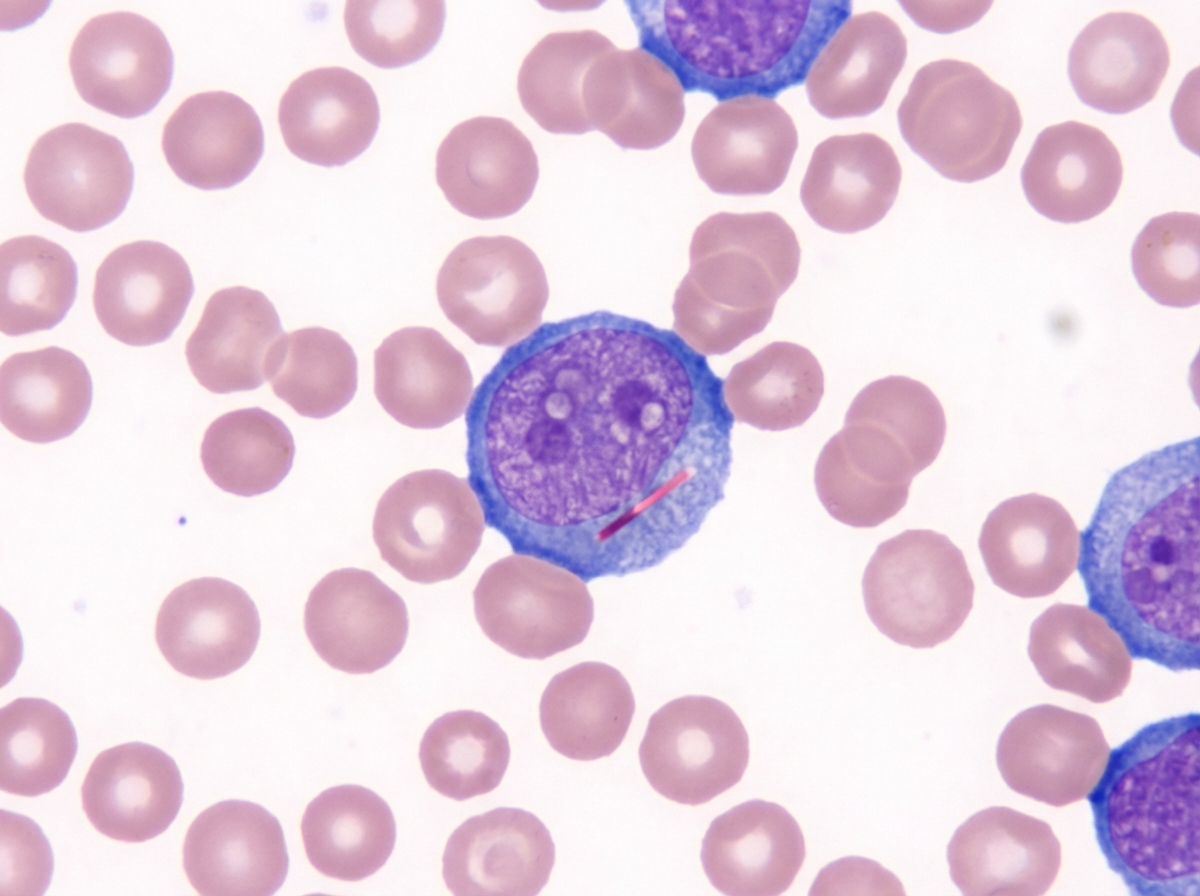
A 63-year-old man presents to the physician with fever for 5 days. He has had increasing fatigue and dyspnea for the past 2 months. During this time, he has lost 3 kg (6.6 lb). He received outpatient treatment for pneumonia last month. He had urinary tract infection 2 weeks ago. He takes no other medications other than daily low dose aspirin and recent oral antibiotics. He does not smoke or drink alcohol. The vital signs include: temperature 38.5°C (101.3°F), pulse 93/min, respiration rate 18/min, and blood pressure 110/65 mm Hg. On physical examination, he has petechiae distally on the lower extremities and several purpura on the trunk and extremities. Several enlarged lymph nodes are detected in the axillary and cervical regions on both sides. The examination of the lungs, heart, and abdomen shows no abnormalities. The laboratory test results are as follows: Hemoglobin 10 g/dL Mean corpuscular volume 90 μm3 Leukocyte count 18,000/mm3 Platelet count 40,000/mm3 A Giemsa-stained peripheral blood smear is shown by the image. Which of the following is the most likely diagnosis?
A 58-year-old lifeguard develops squamous cell carcinoma of the skin on his forehead. Which of the following most likely preceded the development of this carcinoma?
A 40-year-old woman presents to her primary care physician complaining of a several-month history of episodic sweating and heart racing. Her husband noticed that she becomes pale during these episodes. She also has progressive episodic pounding headaches which are not relieved by paracetamol. Her family history is negative for hypertension, endocrinopathies, or tumors. Vital signs reveal a blood pressure of 220/120 mm Hg, temperature (normal) and pulse of 110/min. Fundus examination reveals hypertensive retinal changes. This patient condition is most likely due to neoplasm arising from which of the following?
A 32-year-old G0P0 African American woman presents to the physician with complaints of heavy menstrual bleeding as well as menstrual bleeding in between her periods. She also reports feeling fatigued and having bizarre cravings for ice and chalk. Despite heavy bleeding, she does not report any pain with menstruation. Physical examination is notable for an enlarged, asymmetrical, firm uterus with multiple palpable, non-tender masses. Biopsy confirms the diagnosis of a benign condition. Which of the following histological characteristics would most likely be seen on biopsy in this patient?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
