Neoplasia — MCQs

On this page
A 46-year-old overweight male presents to his primary care physician for an annual checkup. He has a history of gastroesophageal reflux disease (GERD) with biopsy confirming Barrett's esophagus on therapy with omeprazole. Review of systems is unremarkable, and the patient is otherwise doing well. Vitals are within normal limits and stable. The patient asks about the need for continuing his omeprazole therapy. You recommend he continue his medication because of which of the following most probable long-term sequelae associated with Barrett's esophagus?
A 43-year-old woman presents to a physician with repeated bruising, which she noticed over the last week. Some bruises developed spontaneously, while others were observed following minor trauma. The patient also mentions that she has been experiencing significant fatigue and weakness for the past 4 months and that her appetite has been considerably reduced for a few months. Past medical history is noncontributory. Both of her parents are still alive and healthy. She drinks socially and does not smoke. On physical examination, her temperature is 37.6°C (99.7°F), pulse rate is 88/min, blood pressure is 126/84 mm Hg, and respiratory rate is 18/min. Her general examination reveals mild bilateral cervical and axillary lymphadenopathy with multiple petechiae and ecchymoses over the body. Palpation of the abdomen reveals the presence of hepatomegaly and splenomegaly. Her detailed diagnostic workup, including complete blood counts, coagulation studies, and bone marrow biopsy, confirms the diagnosis of a subtype of acute myeloid leukemia, which is characterized by neoplastic proliferation of promyelocytes and good response to all-trans retinoic acid. The neoplastic cells are myeloperoxidase positive and contain azurophilic crystal rods. Which of the following genetic abnormalities is most likely to be present in this patient?
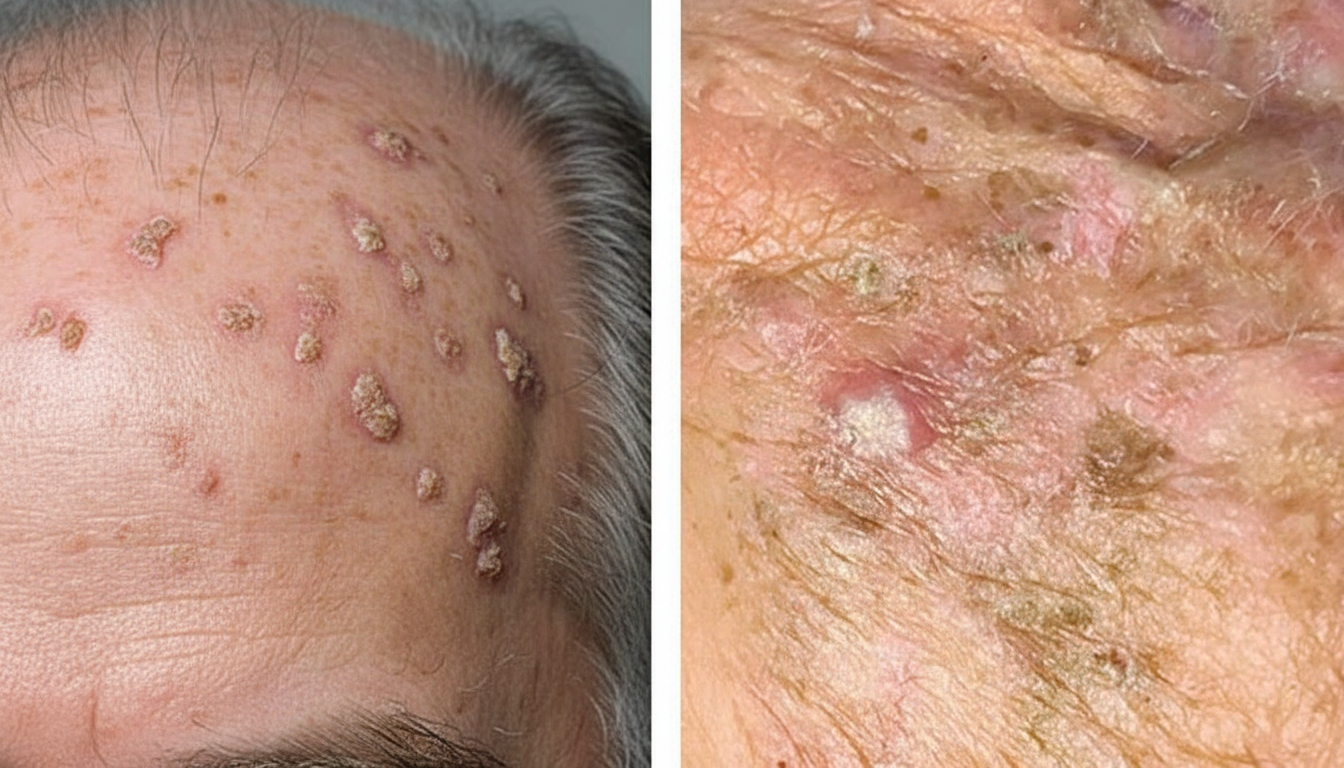
A 68-year-old man comes to the physician 3 months after noticing skin changes on his scalp. When he scrapes off the crust of the lesion, it reappears after a few days. Occasionally, his scalp itches or he notices a burning sensation. He had a mole removed on his right forearm 5 years ago. He is a retired winemaker. His vital signs are within normal limits. Examination shows multiple rough patches on his scalp. A photograph is shown. Which of the following is the most likely diagnosis?
A 38-year-old woman comes to the physician for a 3-month history of bloody discharge from the right nipple. Her mother died of breast cancer at the age of 69 years. Mammography 6 months ago did not show any abnormalities. Examination of the breast shows expression of a small amount of serosanguinous fluid from the right nipple; there are no palpable breast masses or axillary lymphadenopathy. Ultrasonography of the right breast shows a single dilated duct. Which of the following is the most likely diagnosis?
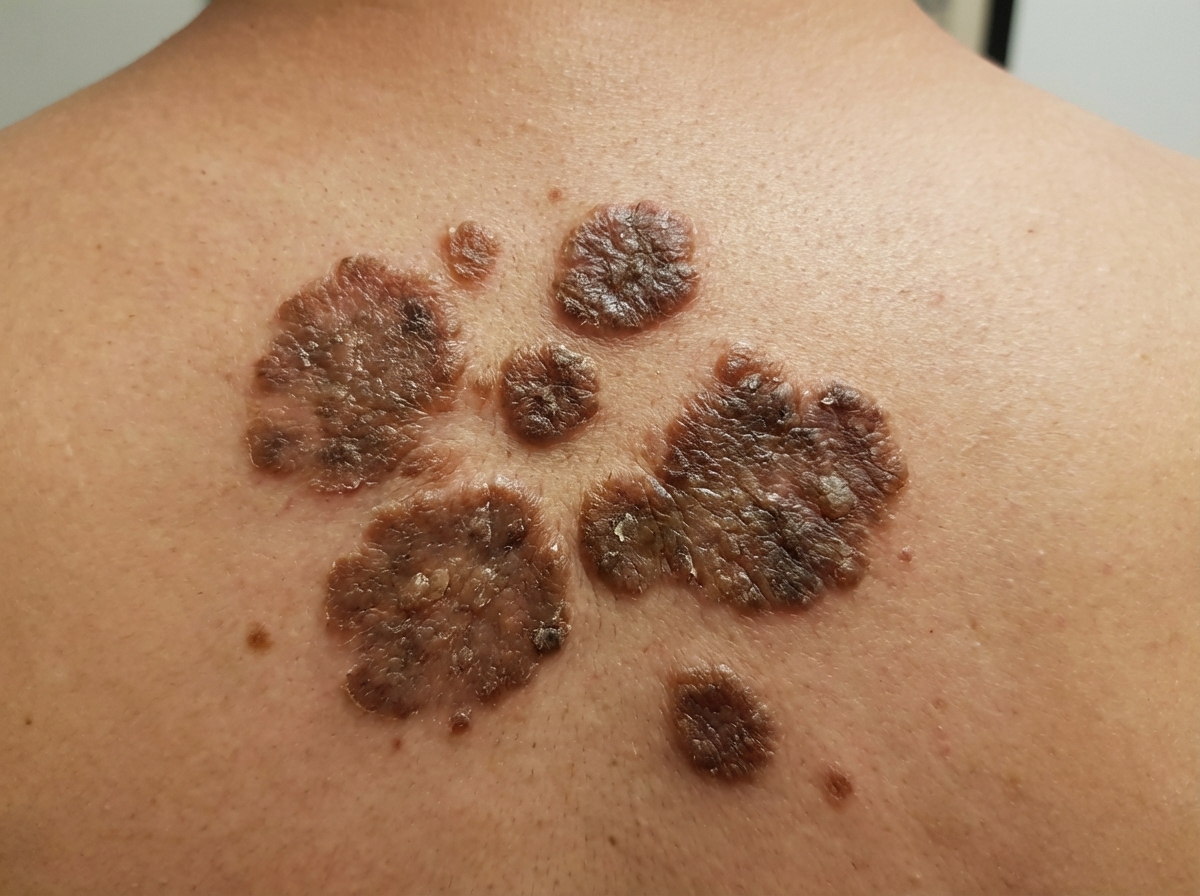
A 68-year-old man comes to the physician because of a 3-month history of a painless skin lesion on his neck. The lesion has gradually become darker in color. Sometimes it is itchy. He also noticed one similar lesion on his lower back. He is a retired gardener. He has smoked half a pack of cigarettes daily for 40 years. His temperature is 36.7°C (98°F), pulse is 72/min, and blood pressure is 123/78 mm Hg. Physical examination shows a 0.8-cm hyperpigmented papule on his neck and a 0.6-cm hyperpigmented papule on his lower back, both of which have a greasy and wax-like appearance. A photograph of the neck is shown. Which of the following is the most likely diagnosis?
A 68-year-old man comes to the physician for evaluation of a lump in his left axilla that he first noticed 1 year ago. He reports that the size of the mass has varied over time and that there have been similar masses in his neck and groin. He has not had fever, weight loss, or night sweats. Physical examination shows a nontender, rubbery mass in the left axilla and a similar, smaller mass in the right groin. His spleen is palpable 3 cm below the left costal margin. Laboratory studies, including complete blood count, are within reference ranges. Genetic analysis obtained on resection of the axillary mass shows a t(14;18) translocation. Which of the following is the most likely diagnosis?
A 45-year-old woman gravida 1, para 1, comes to the physician because of a 2-month history of a right breast lump and a 4.5-kg (10-lb) weight loss. She has not had any breast pain or nipple discharge. She had right breast mastitis 10 years ago while breastfeeding but has no other history of serious illness. Palpation of the right breast shows a 3-cm firm mass with well-defined margins lateral to the right nipple. There is dimpling of the overlying skin but no rash. The left breast is normal. A mammogram shows a density with calcifications in a star-shaped formation in the same location of the mass. Histological examination of a biopsy specimen from the breast mass is most likely to show which of the following?
A 1-year-old, pale-looking boy presents with high-grade fever and ecchymosis, which he has been experiencing for the past 2 weeks. The boy has achieved all developmental milestones on time and has no history of medical illness in the past. Lab investigations reveal the following: Hemoglobin 5.5 g/dL WBC 112,000/mm3 Platelets 15,000/mm3 ESR 105/1st hour The boy is referred to a hematologist, who suspects that he may be suffering from the neoplastic proliferation of immature B cells. The physician decides to do a flow cytometry analysis. Detection of which of the following markers would help confirm the suspected diagnosis?
A 55-year-old man comes to the physician because of worsening fatigue and recurrent bleeding from his gums for 2 weeks. Physical examination shows marked pallor. There are scattered red, nonblanching pinpoint spots on his trunk and extremities. Laboratory studies show a hemoglobin of 8.0 g/dL, a leukocyte count of 80,000/mm3, and a platelet count of 104,000/mm3. Genetic analysis of a bone marrow aspirate shows leukemic cells with a balanced translocation between the long arms of chromosome 15 and 17. These cells are most likely to stain positive for which of the following?
An 85-year-old man who recently immigrated to the US from Spain presents to your office complaining of hoarseness and dysphagia for the past 2 months. He says his symptoms have been getting progressively worse, and he expresses concerns about the difficulty swallowing as he cannot eat well and has even lost 9 kg (20 lb) since his last visit 3 months ago. He denies any shortness of breath, coughing of blood, and chest pain. His bowel and bladder habit are normal. Past medical history is unremarkable. He has a 60-pack-year history of smoking tobacco and drinks alcohol occasionally. Which of the following is the most likely cause of his symptoms?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
