Neoplasia — MCQs

On this page
A 52-year-old Caucasian man presents to the clinic for evaluation of a mole on his back that he finds concerning. He states that his wife noticed the lesion and believes that it has been getting larger. On inspection, the lesion is 10 mm in diameter with irregular borders. A biopsy is performed. Pathology reveals abnormal melanocytes forming nests at the dermo-epidermal junction and discohesive cell growth into the epidermis. What is the most likely diagnosis?
A 55-year-old man comes to the physician for a routine health visit. He feels well except for occasional left-sided abdominal discomfort and left shoulder pain. He has smoked 1 pack of cigarettes daily for 20 years. He does not drink alcohol. His pulse is 85/min and his blood pressure is 130/70 mmHg. Examination shows a soft, nontender abdomen. The spleen is palpated 5 cm below the costal margin. There is no lymphadenopathy present. The remainder of the examination shows no abnormalities. Laboratory studies show: Hemoglobin 12.2 g/dL Hematocrit 36 % Leukocyte count 34,000/mm3 Platelet count 450,000/mm3 Cytogenetic testing of his blood cells is pending. Further evaluation of this patient is most likely to show which of the following findings?
A 35-year-old male presents to his physician with the complaint of fatigue and weakness for six months. His physician orders a CBC which demonstrates anemia and thrombocytopenia. During the subsequent work up, a bone marrow biopsy is performed which ultimately leads to the diagnosis of acute promyelocytic leukemia. Which of the following translocations and fusion genes would be present in this patient?
A 70-year-old man is brought to the emergency department by his wife because of lethargy, confusion, and nausea for the past 2 days. He has previously been healthy and has no past medical history. His only medications are a daily multivitamin and acetaminophen, which he takes daily for hip pain. Vital signs are within normal limits. He is disoriented to place and time but recognizes his wife. The remainder of his physical examination shows no abnormalities. Laboratory studies show a hemoglobin concentration of 9.1 g/dL, a serum calcium concentration of 14.7 mg/dL, and a serum creatinine of 2.2 mg/dL (previously 0.9 mg/dL). Which of the following is the most likely underlying mechanism of this patient's condition?
A 93-year-old woman is brought to the physician because of a purple area on her right arm that has been growing for one month. She has not had any pain or itching of the area. She has hyperlipidemia, a history of basal cell carcinoma treated with Mohs surgery 2 years ago, and a history of invasive ductal carcinoma of the right breast treated with radical mastectomy 57 years ago. She has had chronic lymphedema of the right upper extremity since the mastectomy. Her only medication is simvastatin. She lives in an assisted living facility. She is content with her living arrangement but feels guilty that she is dependent on others. Vital signs are within normal limits. Physical examination shows extensive edema of the right arm. Skin exam of the proximal upper right extremity shows three coalescing, 0.5–1.0 cm heterogeneous, purple-colored plaques with associated ulceration. Which of the following is the most likely diagnosis?
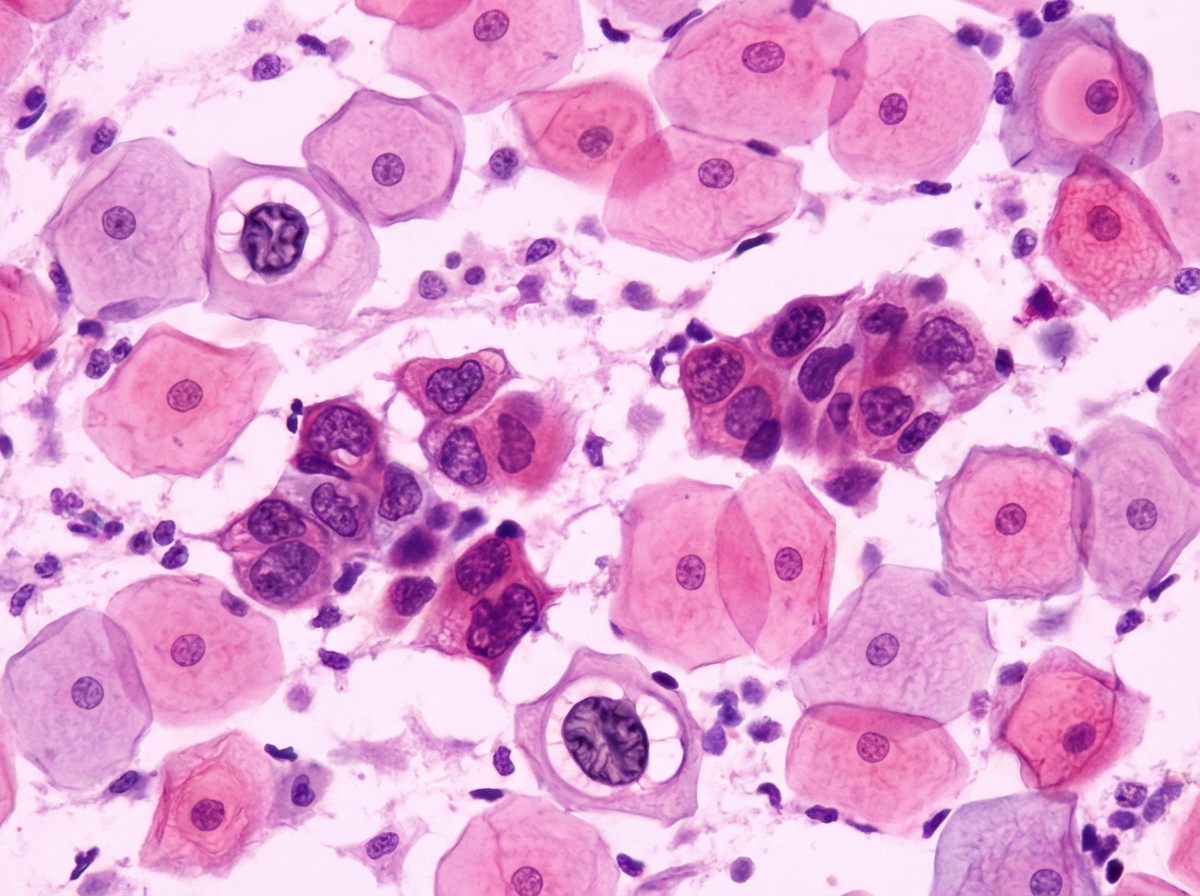
A 41-year-old woman presents with occasional dyspareunia and vaginal bleeding after a sexual encounter. She is in a monogamous relationship and uses oral contraception. She does not have a family history of gynecologic malignancies. She has smoked 1 pack of cigarettes per day for 15 years and drinks several glasses of wine daily. She has not received HPV vaccination. Her blood pressure is 120/70 mm Hg, heart rate is 71/min, respiratory rate is 14/min, and temperature is 36.7°C (98.1°F). A speculum examination shows a nulliparous cervix in the mid-plane of the vaginal vault with a red discoloration—approx. 1 × 2 cm in diameter. Bimanual examination revealed no apparent pathologic changes. A Papanicolaou smear is shown in the exhibit. Which of the following proteins is most likely to be inactivated by viral oncoproteins in the affected cells in this case?
A 53-year-old woman presents to her primary care physician in order to discuss the results of a biopsy. Two weeks ago, her mammogram revealed the presence of suspicious calcifications in her right breast, and she subsequently underwent biopsy of these lesions. Histology of the lesions revealed poorly cohesive cells growing in sheets with a nuclear to cytoplasmic ratio of 1:1. Furthermore, these cells were found to undergo invasion into the surrounding tissues. Given these findings, the patient is referred to an oncologist for further evaluation. Upon further imaging, the patient is found to have no lymph node adenopathy and no distant site metastases. Which of the following would most properly describe the lesions found in this patient?
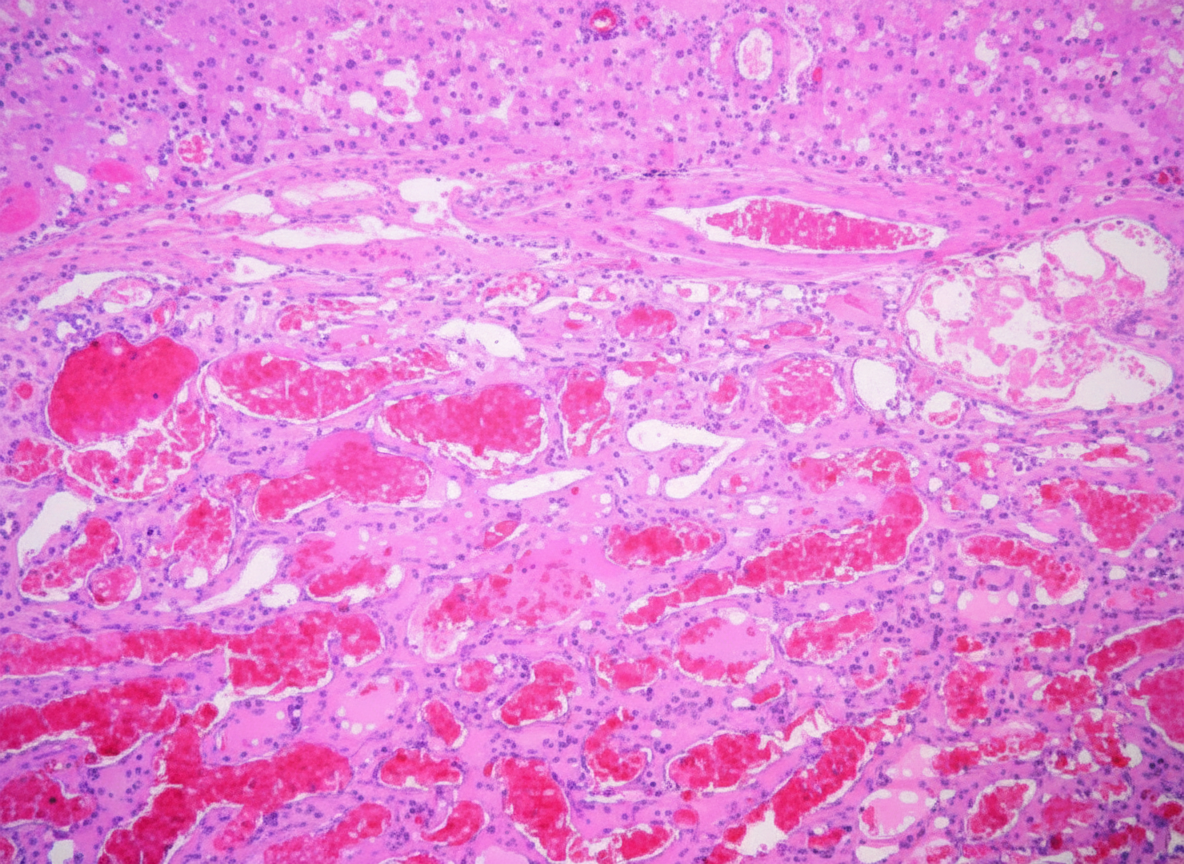
A 49-year-old woman comes to the physician with a 2-month history of mild abdominal pain, nausea, and several episodes of vomiting. She often feels full after eating only a small amount of food. Abdominal examination shows mild right upper quadrant tenderness and a liver span of 16 cm. Ultrasonography shows a 5 x 4 cm hyperechoic mass in the left lobe of the liver. The mass is surgically excised. A photomicrograph of the resected specimen is shown. Which of the following is the most likely diagnosis?
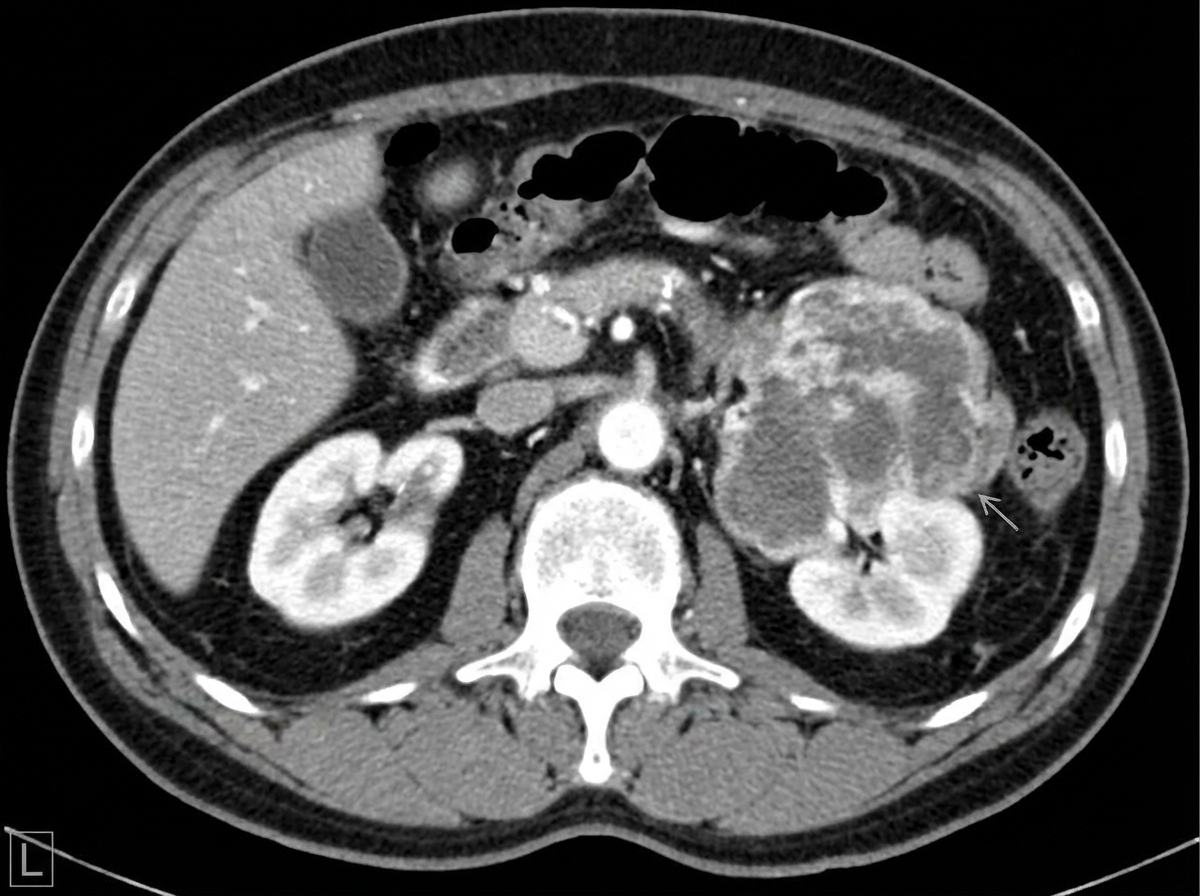
A 74-year-old male presents to his primary care physician complaining of left lower back pain. He reports a four-month history of worsening left flank pain. More recently, he has started to notice that his urine appears brown. His past medical history is notable for gout, hypertension, hyperlipidemia, and myocardial infarction status-post stent placement. He has a 45 pack-year smoking history and drinks 2-3 alcoholic beverages per day. His temperature is 100.9°F (38.3°C), blood pressure is 145/80 mmHg, pulse is 105/min, and respirations are 20/min. Physical examination is notable for left costovertebral angle tenderness. A CT of this patient’s abdomen is shown in figure A. This lesion most likely arose from which of the following cells?
A 51-year-old woman presents with the following significant and unintentional weight loss. She denies any personal history of blood clots in her past, but she says that her mother has also had to be treated for pulmonary embolism in the recent past. She also mentions that she had been struggling with her weight, so she was initially content with losing the weight, but her daughter convinced her to come to the office to be checked out. Her past medical history is significant for preeclampsia, hypertension, polycystic ovarian syndrome, and hypercholesterolemia. She currently smokes 1 pack of cigarettes per day, drinks a glass of wine per day, and she currently denies any illicit drug use, although she has a remote past of injection drug use with heroin. The vital signs include: temperature 36.7°C (98.0°F), blood pressure 126/74 mm Hg, heart rate 111/min and irregular, and respiratory rate 17/min. On physical examination, her pulses are bounding and complexion is pale, but breath sounds remain clear. Oxygen saturation was initially 91% on room air and electrocardiogram (ECG) showed atrial fibrillation. Upon further discussion with the patient, her physician discovers that she is having some cognitive difficulty. Her leukocyte count is elevated to 128,000/mm3, and she has elevated lactate dehydrogenase (LDH), uric acid, and B-12 levels. A BCR-ABL translocation is present, as evidenced by the Philadelphia chromosome. What is the most likely diagnosis for this patient?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
