Neoplasia — MCQs

On this page
A previously healthy 75-year-old woman comes to the physician because of fatigue and decreasing exercise tolerance over the past 6 weeks. She also has intermittent episodes of dizziness. She has never smoked and does not drink alcohol. She takes a daily multivitamin. She appears pale. Physical examination shows a smooth liver that is palpable 1 cm below the costal margin. The spleen is not palpable. Laboratory studies show: Hemoglobin 9.8 g/dL MCV 104 fL Reticulocyte count 0.2 % Folate 21 ng/mL (N = 2–20) Vitamin B12 789 pg/mL (N = 200–900) A peripheral blood smear shows anisocytosis and bone marrow aspirate shows ringed sideroblasts. This patient is most likely to develop which of the following?
A 52-year-old man is brought to the emergency department because of headaches, vertigo, and changes to his personality for the past few weeks. He was diagnosed with HIV 14 years ago and was started on antiretroviral therapy at that time. Medical records from one month ago indicate that he followed his medication schedule inconsistently. Since then, he has been regularly taking his antiretroviral medications and trimethoprim-sulfamethoxazole. His vital signs are within normal limits. Neurological examination shows ataxia and apathy. Mini-Mental State Examination score is 15/30. Laboratory studies show: Hemoglobin 12.5 g/dL Leukocyte count 8400/mm3 Segmented neutrophils 80% Eosinophils 1% Lymphocytes 17% Monocytes 2% CD4+ T-lymphocytes 90/μL Platelet count 328,000/mm3 An MRI of the brain with contrast shows a solitary ring-enhancing lesion involving the corpus callosum and measuring 4.5 cm in diameter. A lumbar puncture with subsequent cerebrospinal fluid analysis shows slight pleocytosis, and PCR is positive for Epstein-Barr virus DNA. Which of the following is the most likely diagnosis?
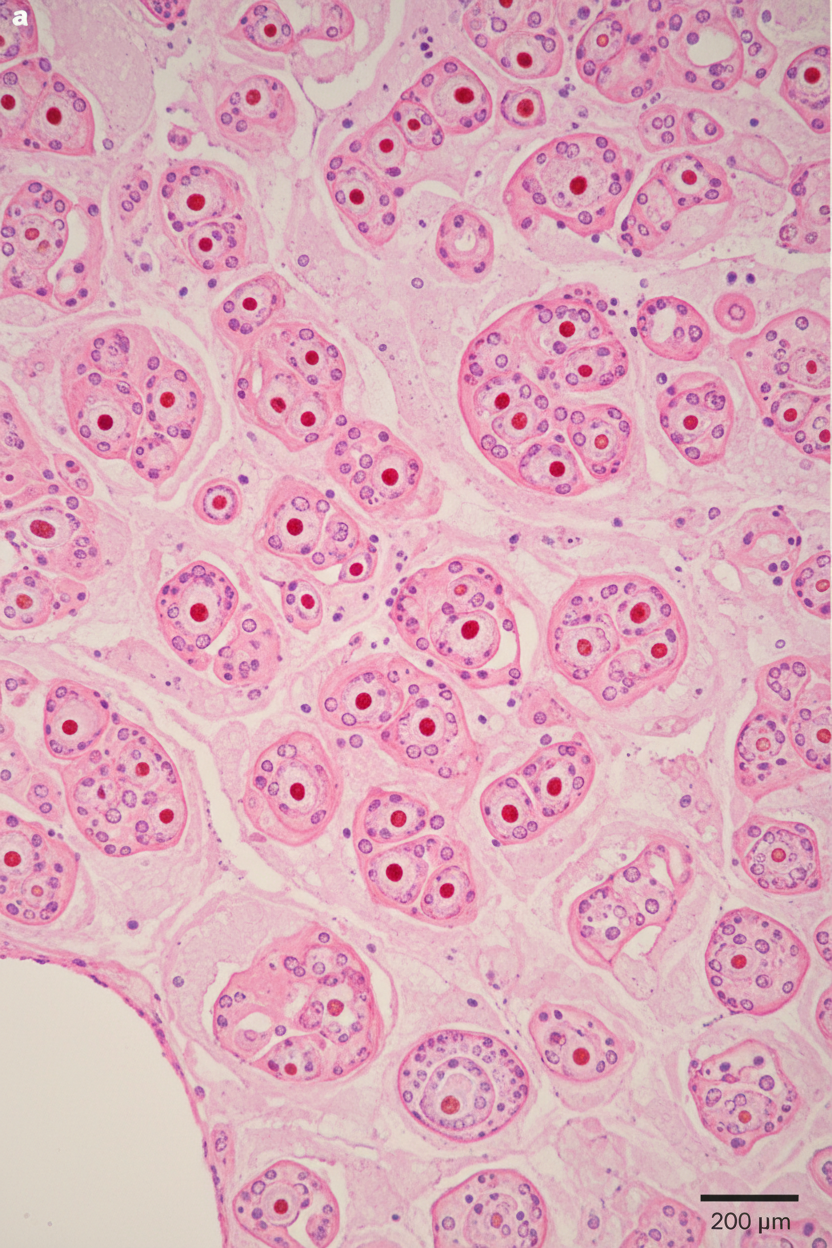
A 57-year-old man comes to the physician with a 3-month history of right flank pain. Urinalysis shows 60 RBC/hpf. Renal ultrasound shows a 3 cm, well-defined mass in the upper pole of the right kidney. A photomicrograph of a section of the resected mass is shown. Which of the following is the most likely diagnosis?
A 67-year-old woman comes to the physician because of a 9-month history of progressive fatigue. Examination shows pallor. Her hemoglobin concentration is 8.9 g/dL, mean corpuscular volume is 75 μm3, and serum ferritin is 9 ng/mL. Test of the stool for occult blood is positive. Colonoscopy shows an irregular, bleeding 3-cm exophytic ulcer in the right colon. Which of the following lesions is the greatest risk factor for this patient's condition?
A 53-year-old woman comes to the emergency department because of blurry vision, headache, and multiple episodes of nosebleeds over the last few weeks. During this time, she has also been itching a lot, especially after getting ready for work in the mornings. She has had an 8-kg (17.6-lb) weight loss and increasing fatigue during the past 6 months. Her temperature is 37.8°C (100.0°F), pulse is 80/min, respirations are 15/min, and blood pressure is 158/90 mm Hg. Physical examination shows no lesions or evidence of trauma in the nasal cavity. Her face, palms, nail beds, oral mucosa, and conjunctiva appear red. Abdominal examination shows splenomegaly. Her hemoglobin concentration is 19 g/dL, hematocrit is 58%, platelets are 450,000/μL, and erythropoietin level is below normal. A peripheral blood smear shows RBC precursor cells. Which of the following is the most likely underlying cause of this patient's condition?
A 73-year-old man is brought to the emergency department because of fever and a productive cough for 2 days. He has had increasing fatigue and dyspnea for the past 2 weeks. During this time he has lost 3 kg (6.6 lb). He received chemotherapy for myelodysplastic syndrome (MDS) 1 year ago. He is currently on supportive treatment and regular blood transfusions. He does not smoke or drink alcohol. The vital signs include: temperature 38.5℃ (101.3℉), pulse 93/min, respiratory rate 18/min, and blood pressure 110/65 mm Hg. He has petechiae distally on the lower extremities and several purpura on the trunk and extremities. Several enlarged lymph nodes are detected in the axillary and cervical regions on both sides. On auscultation of the lungs, crackles are heard in the left lower lobe area. Physical examination of the heart and abdomen shows no abnormalities. The laboratory studies show the following: Hemoglobin 9 g/dL Mean corpuscular volume 95 μm3 Leukocyte count 18,000/mm3 Platelet count 40,000/mm3 Prothrombin time 11 sec (INR = 1) Based on these findings, this patient is most likely to have developed which of the following?
A 34-year-old man comes to the physician because of a 3-week history of left testicular swelling. He has no pain. He underwent a left inguinal hernia repair as a child. He takes no medications. He appears healthy. His vital signs are within normal limits. Examination shows an enlarged, nontender left testicle. When the patient is asked to cough, there is no bulge present in the scrotum. When a light is held behind the scrotum, it does not shine through. There is no inguinal lymphadenopathy. Laboratory studies show: Hemoglobin 14.5 g/dL Leukocyte count 8,800/mm3 Platelet count 345,000/mm3 Serum Glucose 88 mg/dL Creatinine 0.8 mg/dL Total bilirubin 0.7 mg/dL Alkaline phosphatase 35 U/L AST 15 U/L ALT 14 U/L Lactate dehydrogenase 60 U/L β-Human chorionic gonadotropin 80 mIU/mL (N < 5) α-Fetoprotein 6 ng/mL (N < 10) Which of the following is the most likely diagnosis?
A 52-year-old female was found upon mammography to have branching calcifications in the right lower breast. Physical exam revealed a palpable nodularity in the same location. A tissue biopsy was taken from the lesion, and the pathology report diagnosed the lesion as comedocarcinoma. Which of the following histological findings is most likely present in the lesion?
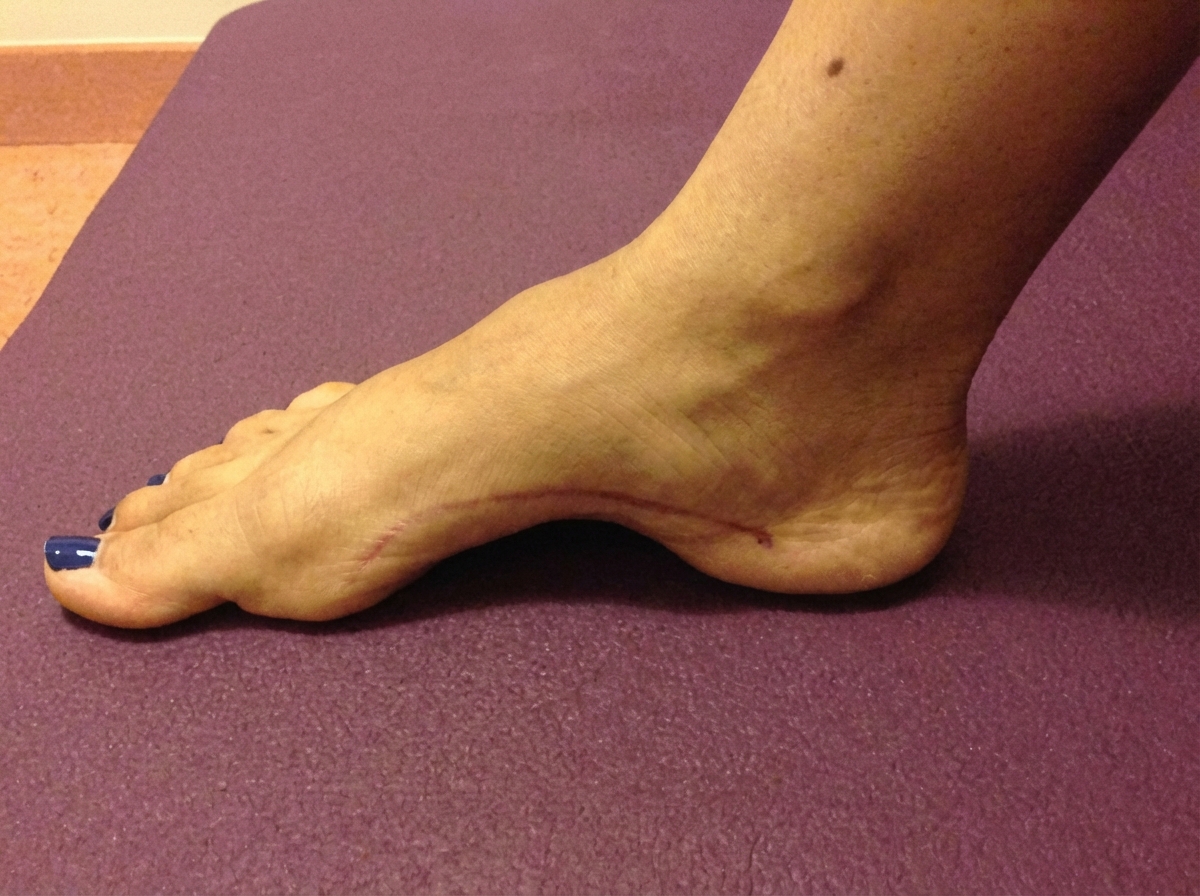
A 35-year-old man presents to the primary care office with a recent history of frequent falls. He had been able to walk normally until about a year ago when he started noticing that both of his legs felt weak. He's also had some trouble with feeling in his feet. These 2 problems have caused multiple falls over the last year. On physical exam, he has notable leg and foot muscular atrophy and 4/5 strength throughout his bilateral lower extremities. Sensation to light touch and pinprick is absent up to the mid-calf. Ankle jerk reflex is absent bilaterally. A photo of the patient's foot is shown. Which of the following best describes the etiology of this patient's condition?
A 76-year-old woman is brought to the physician because of lesions on her left arm. She first noticed them 3 months ago and they have grown larger since that time. She has not had any pain or pruritus in the area. She has a history of invasive ductal carcinoma of the left breast, which was treated with mastectomy and radiation therapy 27 years ago. Since that time, she has had lymphedema of the left arm. Physical examination shows extensive edema of the left arm. There are four coalescing, firm, purple-blue nodules on the left lateral axillary region and swelling of the surrounding skin. Which of the following is the most likely diagnosis?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
