Neoplasia — MCQs

On this page
A 40-year-old male presents to his primary care physician for a regularly scheduled check-up. Physical examination reveals nontender cervical lymphadenopathy. A biopsy of the lymph node reveals aggregates of follicular architecture, and cytogenic analysis shows a t(14;18) translocation. The protein most likely responsible for the patient’s condition does which of the following:
A 67-year-old man presents to the emergency department with altered mental status. The patient is non-verbal at baseline, but his caretakers at the nursing home noticed he was particularly somnolent recently. The patient has a past medical history of diabetes and Alzheimer dementia. His temperature is 99.7°F (37.6°C), blood pressure is 157/98 mmHg, pulse is 150/min, respirations are 16/min, and oxygen saturation is 98% on room air. Laboratory values are obtained and shown below. Hemoglobin: 9 g/dL Hematocrit: 33% Leukocyte count: 8,500/mm^3 with normal differential Platelet count: 197,000/mm^3 Serum: Na+: 139 mEq/L Cl-: 102 mEq/L K+: 4.3 mEq/L HCO3-: 25 mEq/L BUN: 37 mg/dL Glucose: 99 mg/dL Creatinine: 2.4 mg/dL Ca2+: 12.2 mg/dL The patient has lost 20 pounds over the past month. His parathyroid hormone is within normal limits, and his urinary calcium is increased. Physical exam demonstrates discomfort when the patient's lower back and extremities are palpated. Which of the following is the most accurate diagnostic test for this patient's underlying diagnosis?
A 1-year-old boy is brought to the physician for the evaluation of swelling around the eyelids. He was born at term after an uncomplicated pregnancy. He is at the 95th percentile for weight and 60th percentile for length. His blood pressure is 130/86 mm Hg. Physical examination shows an empty scrotal sac and a left-sided abdominal mass. Ophthalmologic examination shows no abnormalities. Urinalysis shows a proteinuria of 3+ and fatty casts. Abdominal ultrasound shows a hypervascular mass at the upper pole of the kidney. Which of the following best describes the pathogenesis of this patient's disease?
A 6-year-old boy is brought to the physician by his parents because of right lower extremity weakness, worsening headaches, abdominal pain, dark urine, and a 5-kg (11-lb) weight loss for the past 2 months. His teachers report that he has not been paying attention in class and his grades have been worsening. He has a history of infantile seizures. Physical examination shows a palpable abdominal mass and left costovertebral angle tenderness. Neurological exam shows decreased strength of the right lower limb. He has several acne-like angiofibromas around the nose and cheeks. Further evaluation is most likely to show which of the following?
An 11-month-old boy presents with a scaly erythematous rash on his back for the past 2 days. No significant past medical history. Family history is significant for the fact that the patient’s parents are first-degree cousins. In addition, his older sibling had similar symptoms and was diagnosed with a rare unknown skin disorder. On physical examination, whitish granulomatous plaques are present in the oral mucosa, which exhibit a tendency to ulcerate, as well as a scaly erythematous rash on his back. A complete blood count reveals that the patient is anemic. A plain radiograph of the skull shows lytic bone lesions. Which of the following immunohistochemical markers, if positive, would confirm the diagnosis in this patient?
A 32-year-old man visits his family physician for 10 months of persistent left flank pain, weight loss, and fatigue. Also, he has had hematuria a couple of times in the last month. His mother was diagnosed and treated for a pheochromocytoma when she was 36 years old, and his father died at 45 years due to myocardial infarction. His personal medical history is not relevant. He does not smoke and used to be a varsity athlete in high school and university. Physical examination shows temporal wasting, pale mucous membranes and palms, a palpable mass in the left flank, and a varicocele that does not reduce upon recumbency. His family physician sends the patient to the emergency department for an abdominal computed tomography (CT) scan, which shows a complex left renal mass and a hemangioblastoma in T10. A biopsy of the renal mass is ordered by the oncology team, which demonstrates compact cells with prominent nucleoli, eosinophilic cytoplasm within a network of a small and thin-walled vasculature. What is the most likely type of tumor in this patient?
A 72-year-old male visits his gastroenterologist for a check-up one year following resection of a 2-cm malignant lesion in his sigmoid colon. Serum levels of which of the following can be used in this patient to test for cancer recurrence?
A 15-year-old girl comes to the physician because of a sore throat and subjective fevers for the past 2 weeks. She has been feeling lethargic and is unable to attend school. She has a history of multiple episodes of streptococcal pharyngitis treated with amoxicillin. She immigrated with her family to the United States from China 10 years ago. She appears thin. Her temperature is 37.8°C (100°F), pulse is 97/min, and blood pressure is 90/60 mm Hg. Examination shows pharyngeal erythema and enlarged tonsils with exudates and palatal petechiae. There is cervical lymphadenopathy. The spleen is palpated 2 cm below the left costal margin. Her hemoglobin concentration is 12 g/dL, leukocyte count is 14,100/mm3 with 54% lymphocytes (12% atypical lymphocytes), and platelet count is 280,000/mm3. A heterophile agglutination test is positive. The underlying cause of this patient's symptoms is most likely to increase the risk of which of the following conditions?
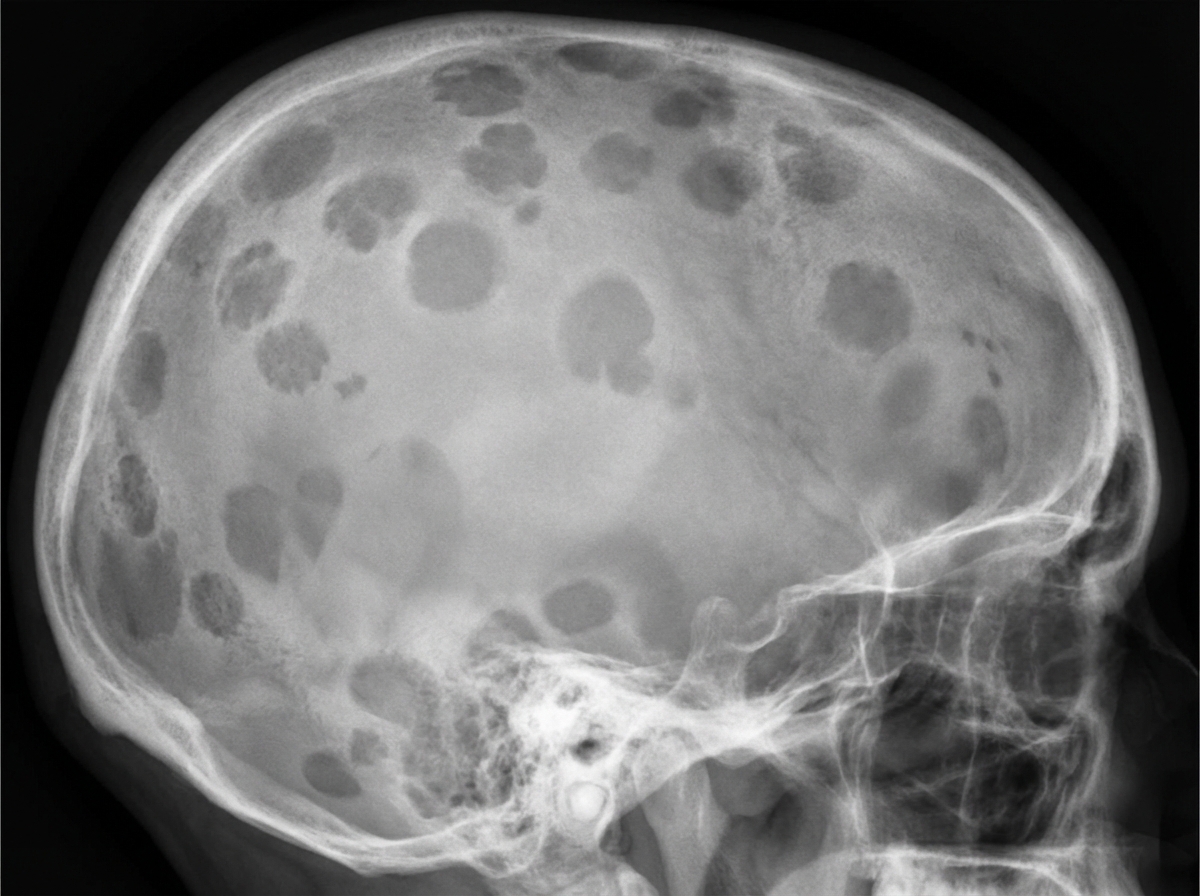
A 70-year-old man comes to the physician because of progressive fatigue and lower back pain for the past 4 months. The back pain worsened significantly after he had a minor fall while doing yard work the previous day. For the past year, he has had a feeling of incomplete emptying of his bladder after voiding. His vital signs are within normal limits. Examination shows bilateral paravertebral muscle spasm, severe tenderness over the second lumbar vertebra, and mild tenderness over the lower thoracic vertebrae. Neurologic examination shows no abnormalities. His hemoglobin is 10.5 g/dl, alkaline phosphatase is 110 U/L, and serum calcium is 11.1 mg/dl. An x-ray of the skull is shown. Which of the following is the most appropriate next step in diagnosis?
A 9-year-old boy is brought to the physician for evaluation of 2 months of progressive clumsiness, falls, and increased urinary frequency. Physical examination shows bilateral temporal visual field loss. An MRI of the head shows a small calcified suprasellar mass. The patient undergoes surgery with complete removal of the mass. Pathological examination of the specimen shows a lobular tumor composed of cysts filled with oily, brownish-yellow fluid. This mass is most likely derived from which of the following structures?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
