Neoplasia — MCQs

On this page
A 65-year-old man presents to his primary care provider with excessive fatigue, weight loss, and multiple small bruises on his arms and abdomen. These symptoms started several months ago. He reports worsening fatigue and a 20-pound (9 kg) weight loss in the past month. Past medical history is significant for an asymptomatic lymphocytosis noted 6 months ago on a yearly physical. On review of systems, he denies chest pain, difficulty breathing, swelling in the extremities, or change in bowel habits. Vitals include: temperature 37.0°C (98.6°F), blood pressure 110/75 mm Hg, pulse 99/min, respirations 20/min, and oxygen saturation 91% on room air. On physical exam, the patient is listless. The cardiac exam is normal. Lungs are clear to auscultation. The abdominal exam is significant for mild splenomegaly. Scleral icterus is present and there is prominent generalized non-tender lymphadenopathy. Which of the following laboratory findings is best associated with this patient’s condition?
A 55-year-old man presents with severe fatigue and fever. His past medical history is significant for a recent history of mononucleosis from which he fully recovered 8 weeks ago. On physical examination, the patient seems pale. A chest radiograph shows multiple enlarged mediastinal lymph nodes. A biopsy of one of the enlarged mediastinal lymph nodes is performed and shows the presence of multinucleated cells with an 'owl-eye' appearance in a hypocellular background. Which of the following is the most likely diagnosis in this patient?
A 60-year-old woman presents to the dermatologist with a lesion on her lower eyelid. She noticed it a month ago and looked like a pimple. She says that it has been bleeding lately with minimal trauma which alarmed her. She says the lesion has not grown in size and is not associated with pain or pruritus. No significant past medical history. Physical examination reveals a 0.5 cm lesion that has a pearly appearance with telangiectasia and central ulceration and curled borders. The lesion is biopsied. Histopathology reveals peripheral palisading cells with large, hyperchromatic nuclei and a high nuclear: cytoplasmic ratio. Which of the following mechanisms best describes the most common mode of spread of this patient’s neoplasm?
A 70-year-old man presents for a routine checkup. He says that he recently completely lost hearing in both ears and has been having occasional flare-ups of osteoarthritis in his hands and hips. Past medical history is significant for hypertension diagnosed 25 years ago that is well controlled. Family history is significant for his brother, who recently died from prostate cancer. The patient's blood pressure is 126/84 mm Hg. Laboratory findings are significant for an alkaline phosphatase level that is more than 3 times the upper limit. Right upper quadrant ultrasound and non-contrast computed tomography of the abdomen and pelvis reveal no significant abnormalities. Which of the following is the most likely complication of this patient’s condition?
A 34-year-old woman presents to her primary care physician for a routine check-up. She complains that she is not feeling her normal self, but has no specific complaints. After a routine examination, the physician orders a full thyroid workup, including TSH, T3, and free T4. He also refers her directly to an oncologist for an initial consultation. Which type of lymphadenopathy was most likely present during the physical examination that made the primary care physician react this way?
A 43-year-old man comes to the physician because of weight loss and swelling on the left side of his neck. Physical examination shows a firm, enlarged left upper cervical lymph node that is immobile. Immunohistochemical testing performed on a biopsy specimen from the lymph node stains positive for cytokeratin. Which of the following is the most likely site of the primary neoplasm in this patient?
A 13-year-old boy is brought to the physician because of a 4-month history of worsening dizziness, nausea, and feeling clumsy. An MRI of the brain shows a well-demarcated, 4-cm cystic mass in the posterior fossa. The patient undergoes complete surgical resection of the mass. Pathologic examination of the surgical specimen shows parallel bundles of cells with eosinophilic, corkscrew-like processes. Which of the following is the most likely diagnosis?
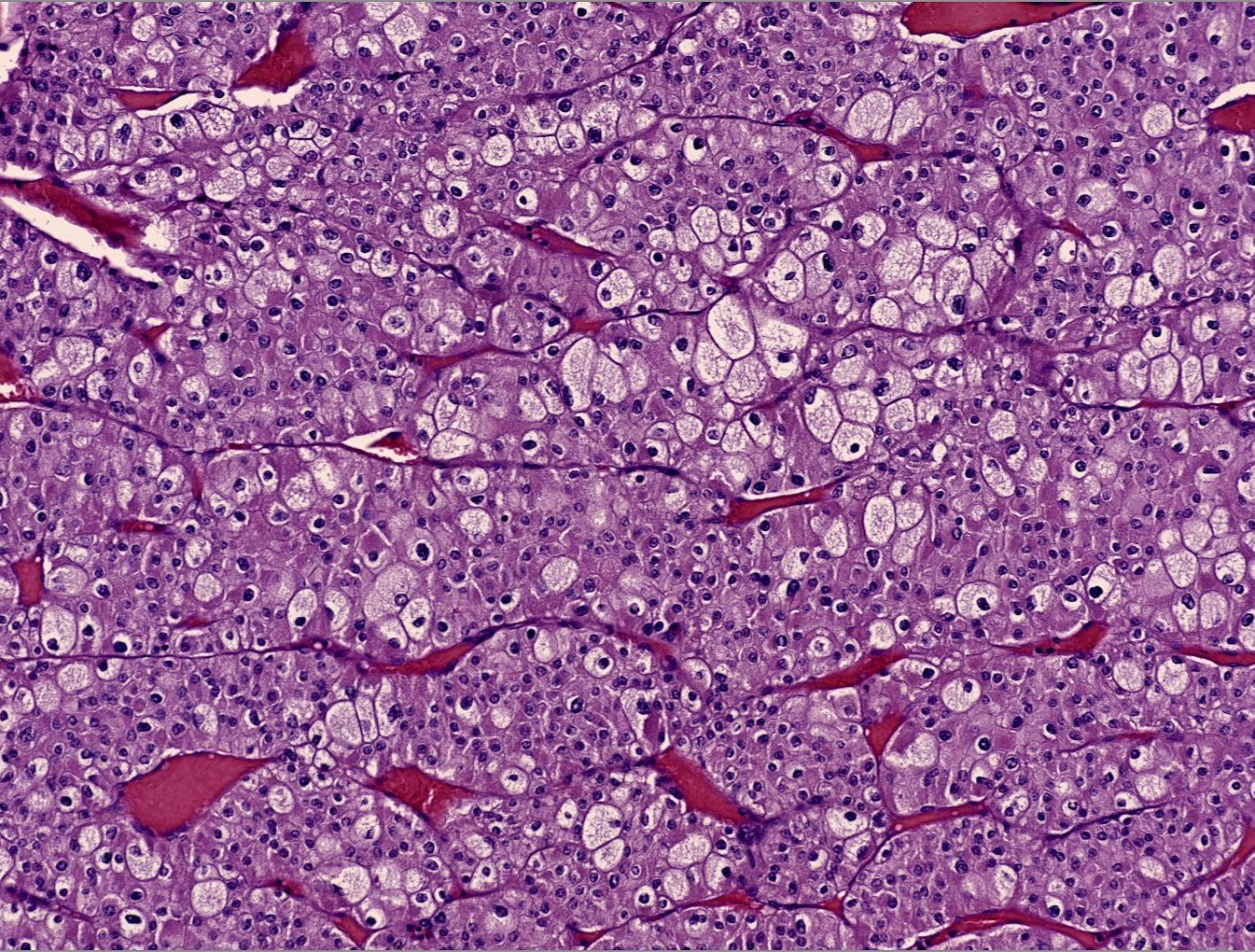
A 69-year-old man comes to the physician because of a 1-week history of blood in the urine and fatigue. He also has had a 5.0-kg (11-lb) weight loss during the past month. Physical examination shows pallor and cachexia. A nontender right flank mass is palpated. A CT scan of the chest, abdomen, and pelvis shows a 5-cm right upper pole renal mass and several pulmonary lesions. A biopsy specimen of an affected area of the lung is obtained. A photomicrograph of the biopsy specimen is shown. Molecular evaluation of the specimen is most likely to show which of the following genetic changes?
A 58-year-old woman with HIV infection is brought to the emergency department because of a 2-week history of headaches, blurred vision, and confusion. Her current medications include antiretroviral therapy and trimethoprim-sulfamethoxazole. Neurological examination shows ataxia and memory impairment. Her CD4+ T-lymphocyte count is 90/μL. Cerebrospinal fluid analysis shows lymphocytic predominant pleocytosis, and PCR is positive for Epstein-Barr virus DNA. An MRI of the brain with contrast shows a solitary, weakly ring-enhancing lesion with well-defined borders involving the corpus callosum. Which of the following is the most likely diagnosis?
An obese 63-year-old man comes to the physician because of 3 episodes of red urine over the past week. He has also had recurrent headaches and intermittent blurry vision during the past month. He has benign prostatic hyperplasia. He works as an attendant at a gas station. The patient has smoked one pack of cigarettes daily for the last 40 years. He does not drink alcohol. Current medications include tamsulosin. His temperature is 37.4°C (99.4°F), pulse is 90/min, and blood pressure is 152/95 mm Hg. Examination shows a flushed face. Cardiopulmonary examination shows no abnormalities. The abdomen is soft and non-tender. Digital rectal examination shows an enlarged prostate with no nodules. Urinalysis shows: Blood 3+ Glucose negative Protein negative WBC 1-2/hpf RBC 40-45/hpf RBC casts none Which of the following is the most likely diagnosis?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
