Neoplasia — MCQs

On this page
A 40-year-old man comes to the physician because of a 1-month history of a painless lump on his neck. Two years ago, he underwent surgery for treatment-resistant hypertension, episodic headaches, and palpitations. Physical examination shows a firm, irregular swelling on the right side of the neck. Ultrasonography of the thyroid gland shows a 2-cm nodule with irregular margins and microcalcifications in the right thyroid lobe. Further evaluation of this patient is most likely to show increased serum concentration of which of the following substances?
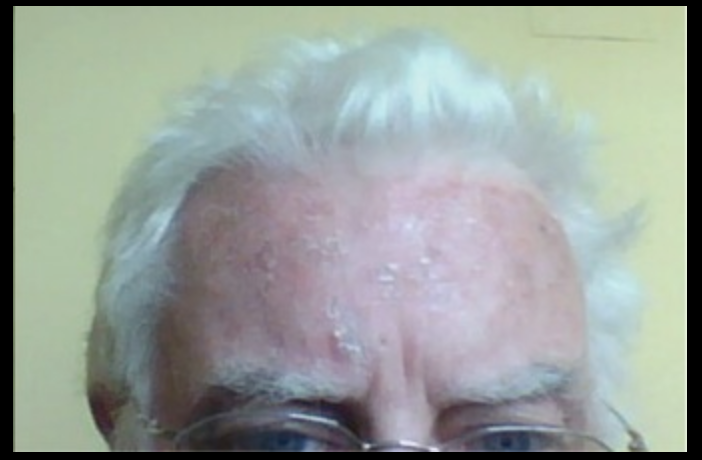
A 66-year-old man presents to his family physician complaining of a sandpaper-like sensation when he touches the lesion on his forehead. His medical history is relevant for hypertension and hypercholesterolemia, for which he is taking losartan and atorvastatin. He used to work as a gardener, but he retired 3 years ago. His vital signs are within normal limits. Physical examination of his forehead reveals male-pattern baldness and thin, adherent, yellow-colored skin lesions that feel rough to the touch (see image). His family physician refers to him to a dermatologist for further management and treatment. Which of the following conditions would the patient most likely develop if this skin condition is left untreated?
A 75-year-old woman comes to the physician because of a 3-month history of involuntary weight loss and a painless lump on her neck. Physical examination shows a firm, irregular swelling on the right side of the neck. Ultrasonography of the thyroid gland shows a 2-cm nodule with irregular margins and microcalcifications in the right thyroid lobe. A biopsy of the thyroid nodule is performed. Which of the following changes would be most consistent with anaplasia?
A 44-year-old man comes to the physician because of fatigue and increased straining during defecation for 3 months. During this time, he has lost 5 kg (12 lb) despite no change in appetite. He has a family history of colon cancer in his maternal uncle and maternal grandfather. His mother died of ovarian cancer at the age of 46. Physical examination shows conjunctival pallor. His hemoglobin concentration is 11.2 g/dL, hematocrit is 34%, and mean corpuscular volume is 76 μm3. Colonoscopy shows an exophytic mass in the ascending colon. Pathologic examination of the resected mass shows a poorly differentiated adenocarcinoma. Genetic analysis shows a mutation in the MSH2 gene. Which of the following is the most likely diagnosis?
A 32-year-old woman presents to her primary care physician for an annual checkup. She reports that she has been feeling well and has no medical concerns. Her past medical history is significant for childhood asthma but she has not experienced any symptoms since she was a teenager. Physical exam reveals a 1-centimeter hard mobile mass in the left upper outer quadrant of her breast. A mammogram was performed and demonstrated calcifications within the mass so a biopsy was obtained. The biopsy shows acinar proliferation with intralobular fibrosis. Which of the following conditions is most likely affecting this patient?
A 70-year-old man presents to the physician with a 1-month history of severe fatigue. During this time, he has unintentionally lost 2 kg (4.4 lb). Currently, he takes no medications other than aspirin for occasional knee pain. He does not smoke or drink alcohol. His vital signs are within the normal range. On physical examination, the conjunctivae are pale. Petechiae are present on the distal lower extremities and on the soft and hard palates. Palpation reveals bilateral painless cervical lymphadenopathy. Examination of the lungs, heart, and abdomen shows no abnormalities. Which of the following factors in this patient’s history or laboratory findings would most likely indicate a good prognosis?
A 5-year-old boy presents to his pediatrician with weakness. His father observed that his son seemed less energetic at daycare and kindergarten classes. He was becoming easily fatigued from mild play. His temperature is 98°F (37°C), blood pressure is 90/60 mmHg, pulse is 100/min, and respirations are 20/min. Physical exam reveals pale conjunctiva, poor skin turgor and capillary refill, and cervical and axillary lymphadenopathy with assorted bruises throughout his body. A complete blood count reveals the following: Leukocyte count: 3,000/mm^3 Segmented neutrophils: 30% Bands: 5% Eosinophils: 5% Basophils: 10% Lymphocytes: 40% Monocytes: 10% Hemoglobin: 7.1 g/dL Hematocrit: 22% Platelet count: 50,000/mm^3 The most specific diagnostic assessment would most likely show which of the following?
A 10-year-old boy is brought by his mother to his pediatrician for "skin growths." His mother reports that she started noticing small lumps arising from the patient's lips and eyelids several months ago. She also notes that he seems to suffer from frequent constipation and appears "weaker" than many of his peers. The boy's past medical history is unremarkable. His father and paternal grandmother have a history of medullary thyroid carcinoma. His height and weight are in the 85th and 45th percentiles, respectively. His temperature is 99°F (37.1°C), blood pressure is 110/65 mmHg, pulse is 90/min, and respirations are 18/min. On examination, he has an elongated face with protruding lips. There are numerous sessile painless nodules on the patient's lips, tongue, and eyelids. This patient's condition is most strongly associated with a mutation in which of the following genes?
A 55-year-old man presents to the emergency department because of an excruciating headache that started suddenly after he got home from work. He also reports having double vision. Specifically, in the last week he almost got into two car accidents with vehicles that "came out of nowhere" while he was trying to merge on the highway. Physical examination is notable for ptosis of the left eye, which is also inferiorly and laterally deviated. The patient is treated emergently and then started on a hormone replacement in order to avoid life-threatening post-treatment complications. The patient's current presentation was associated with a pathologic process that existed for several months prior to this event. Which of the following symptoms could this patient have experienced as part of that pre-existing pathology?
A 3-year-old boy was brought in by his parents for undescended testes. The physical examination showed an absence of the left testis in the scrotum. Inguinal swelling was noted on the left side and was surgically corrected. Which of the following conditions will most likely occur in the later stages of his life?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
