Neoplasia — MCQs

On this page
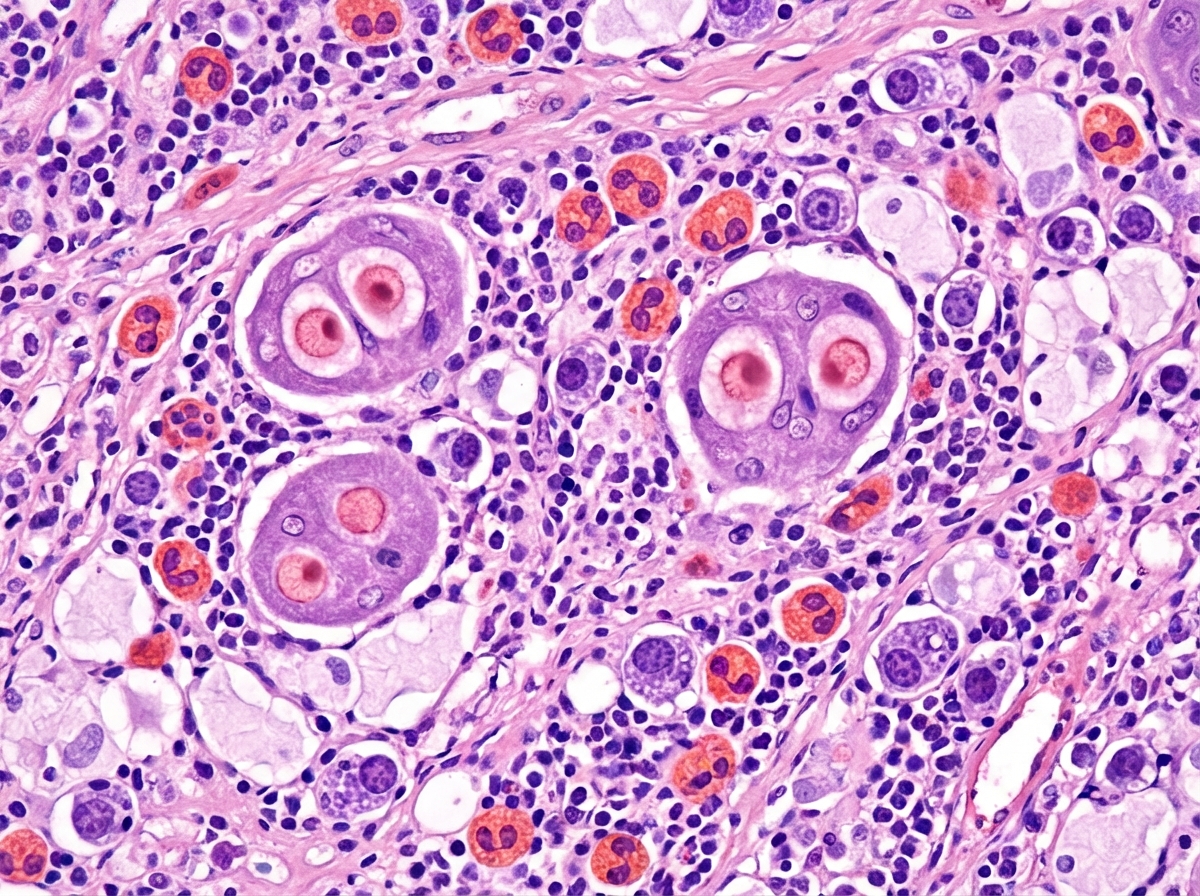
A 58-year-old man presents with a lump on his neck. He says the mass gradually onset 2 months ago and has been progressively enlarging. He denies any pain, weight loss, fevers, chills, or night sweats. Past medical history is significant for HIV, diagnosed 5 years ago, managed on a new HAART regimen he just started. The patient is afebrile and vital signs are within normal limits. Physical examination shows a 3 cm mobile firm mass on the left lateral side of the neck immediately below the level of the thyroid cartilage. A biopsy of the mass is performed and reveals atypical mononuclear cells in a background of eosinophils, plasma cells, histiocytes, atypical T-lymphocytes, and binucleated Reed-Sternberg cells (shown in image). Which of the following is the most likely diagnosis in this patient?
An 82-year-old man presents with painless swelling of the neck for the past week. He reports no recent fever, night sweats, or weight loss. He has no significant medical history, and his only medication is daily aspirin. His temperature is 36.8℃ (98.2℉). On physical examination, there are several non-tender lymph nodes, each averaging 2 cm in diameter, which are palpable in the right anterior cervical triangle. No other palpable lymphadenopathy is noted. The remainder of the physical exam is unremarkable. Laboratory studies show the following: Hemoglobin 10 g/dL Leukocyte count 8000/mm3 with a normal differential Platelet count 250,000/mm3 Erythrocyte sedimentation rate 30 mm/h An excisional biopsy of a cervical lymph node reveals the presence of Reed-Sternberg (RS) cells. Computed tomography (CT) scans and positron emission tomography (PET) scans reveal no mediastinal mass or signs of additional disease. Which of the following aspects most strongly indicates a good prognosis for this patient?
A 69-year-old woman comes to the physician because of lower back pain and right-sided chest pain for the past month. The pain is aggravated by movement. Over the past 2 months, she has had increasing fatigue. Her mother died of breast cancer. She has hypertension and reflux disease. Current medications include metoprolol and omeprazole. Vital signs are within normal limits. Examination shows full muscle strength. There is tenderness to palpation over the lower spine and the right lateral chest. The remainder of the examination shows no abnormalities. Laboratory studies show: Hemoglobin 9.5 g/dL Leukocyte count 7,300/mm3 Platelet count 230,000/mm3 Serum Na+ 137 mEq/L K+ 3.5 mEq/L Creatinine 1.3 mg/dL An ECG shows no evidence of ischemia. An x-ray of the chest shows lytic lesions in 2 ribs. Blood smear shows aggregations of erythrocytes. Protein electrophoresis of the serum with immunofixation shows an M-protein spike. This patient's condition is most likely associated with which of the following findings?
A 63-year-old male is accompanied by his wife to his primary care doctor complaining of shortness of breath. He reports a seven-month history of progressively worsening dyspnea and a dry non-productive cough. He has also lost 15 pounds over the same time despite no change in diet. Additionally, over the past week, his wife has noticed that the patient appears confused and disoriented. His past medical history is notable for stable angina, hypertension, hyperlipidemia, and diabetes mellitus. He currently takes aspirin, metoprolol, lisinopril, atorvastatin, metformin, and glyburide. He has smoked 1 pack of cigarettes per day for 30 years and previously worked as a mechanic at a shipyard. Physical examination reveals no wheezes, rales, or rhonchi with slightly decreased aeration in the left lower lung field. Mucus membranes are moist with normal skin turgor and capillary refill. Laboratory analysis reveals the following: Na 121 mEq/L K 3.4 mEq/L Cl 96 mEq/L HCO3 23 mEq/L Cr 1.1 mg/dl BUN 17 mg/dl A biopsy of the responsible lesions will most likely demonstrate which of the following findings?
A 65-year-old man comes to the physician for a routine health maintenance examination. He has a strong family history of colon cancer. A screening colonoscopy shows a 4 mm polyp in the upper sigmoid colon. Which of the following findings on biopsy is associated with the lowest potential for malignant transformation into colorectal carcinoma?
A 56-year-old man presents to his physician’s office with a sudden increase in urinary frequency. During the past month, he has observed that he needs more frequent bathroom breaks. This is quite unusual as he hasn’t been consuming extra fluids. He reports feeling generally unwell over the past 2 months. He has lost over 7 kg (15.4 lb) of weight and has also been feeling progressively fatigued by the end of the day. He also has a persistent cough and on a couple of occasions, he noticed blood streaks on his napkin. In addition to all of this, he has been feeling weak with frequent muscle cramps during the day. He has never been diagnosed with any medical condition in the past. He doesn’t drink but has smoked 2 packs of cigarettes daily for the last 25 years. Prior to his appointment, he took a couple of tests. The results are given below: Hemoglobin (Hb) 13.1 g/dL Serum creatinine 0.8 mg/dL Serum urea 13 mg/dL Serum sodium 129 mEq/L Serum potassium 3.2 mEq/L His chest X-ray shows a central nodule with some hilar thickening. The physician recommends a biopsy of the nodule. Which of the following histological patterns is the nodule most likely to exhibit?
A 45-year-old male reports several years of asbestos exposure while working in the construction industry. He reports smoking 2 packs of cigarettes per day for over 20 years. Smoking and asbestos exposure increase the incidence of which of the following diseases?
A 51-year-old man presents to the emergency department with an episode of syncope. He was at a local farmer's market when he fainted while picking produce. He rapidly returned to his baseline mental status and did not hit his head. The patient has a past medical history of diabetes and hypertension but is not currently taking any medications. His temperature is 97.5°F (36.4°C), blood pressure is 173/101 mmHg, pulse is 82/min, respirations are 14/min, and oxygen saturation is 98% on room air. Physical exam is notable for clear breath sounds and a S4 heart sound. Rectal exam reveals a firm and nodular prostate that is non-tender and a fecal-occult sample that is negative for blood. Which of the following is this patient's presentation most concerning for?
A 67-year-old man comes to the physician because of urinary frequency, dysuria, and blood in his urine. He has also had a 4.5-kg (10-lb) weight loss over the past 3 months and has been feeling more fatigued than usual. He smoked one pack of cigarettes daily for 40 years but quit 2 years ago. A urinalysis shows 3+ blood. Cystoscopy shows an irregular mass on the bladder wall; a biopsy is taken. Which of the following histologic findings would indicate the worst survival prognosis?
A 74-year-old man with a history of encephalomyelitis, ataxia, and nystagmus has a new diagnosis of small cell carcinoma of the lung (T2, N1, M0) is admitted to the hospital due to painless loss of vision in his right eye. A full workup reveals optic neuritis and uveitis in the affected eye. Which of the following antibodies is most likely to be present in the serum of the patient?
Practice by Chapter
Characteristics of benign vs malignant tumors
Practice Questions
Nomenclature of neoplasms
Practice Questions
Carcinogenesis models
Practice Questions
Oncogenes and proto-oncogenes
Practice Questions
Tumor suppressor genes
Practice Questions
DNA repair genes and cancer
Practice Questions
Epigenetic mechanisms in cancer
Practice Questions
Apoptosis and cancer
Practice Questions
Tumor angiogenesis
Practice Questions
Tumor invasion and metastasis
Practice Questions
Carcinogenic agents
Practice Questions
Paraneoplastic syndromes
Practice Questions
Tumor immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
