Inflammation — MCQs

On this page
A 45-year-old construction worker presents to his primary care physician with a painful and swollen wrist joint. A joint aspiration shows crystals, which are shown in the accompanying picture. Which of the following is the most likely diagnosis?

A 23-year-old woman comes to the physician because of right-sided blurry vision and eye pain for 4 days. She has a 6-day history of low-grade fever, headache, and malaise. One year ago, she was diagnosed with Crohn disease. Her only medication is prednisone. Her temperature is 38°C (100.4°F), pulse is 84/min, and blood pressure is 112/75 mm Hg. The right eyelid is erythematous and tender; there are multiple vesicles over the right forehead and the tip of the nose. Visual acuity is 20/20 in the left eye and 20/80 in the right eye. Extraocular movements are normal. The right eye shows conjunctival injection and reduced corneal sensitivity. Fluorescein staining shows a corneal lesion with a tree-like pattern. Which of the following is the most likely diagnosis?
A 4-year-old Caucasian boy is brought by his mother to the pediatrician with a red and swollen elbow. He was playing outside a few days prior to presentation when he fell and lightly scraped his elbow on the sidewalk. He was born at 34 weeks' gestation and was in the neonatal ICU for 2 days. His temperature is 102.1°F (38.9°C), blood pressure is 105/65 mmHg, pulse is 110/min, and respirations are 20/min. On exam, he has a swollen, erythematous, fluctuant, and exquisitely tender mass on his right elbow. There is expressible purulence coming from his wound. A peripheral blood smear in this patient would most likely reveal which of the following findings?
Two days after being admitted for acute myocardial infarction, a 61-year-old man has sharp, substernal chest pain that worsens with inspiration and improves when leaning forward. Cardiac examination shows a scratchy sound best heard over the left sternal border. Histopathological examination of the infarcted myocardial tissue is most likely to show which of the following findings?
A 42-year-old man comes to the physician because of a 6-week history of intermittent fever, abdominal pain, bloody diarrhea, and sensation of incomplete rectal emptying. He also has had a 4.5-kg (10-lb) weight loss over the past 3 months. Abdominal examination shows diffuse tenderness. Colonoscopy shows circumferential erythematous lesions that extend without interruption from the anal verge to the cecum. A biopsy specimen taken from the rectum shows mucosal and submucosal inflammation with crypt abscesses. This patient is most likely at risk of developing colon cancer with which of the following characteristics?
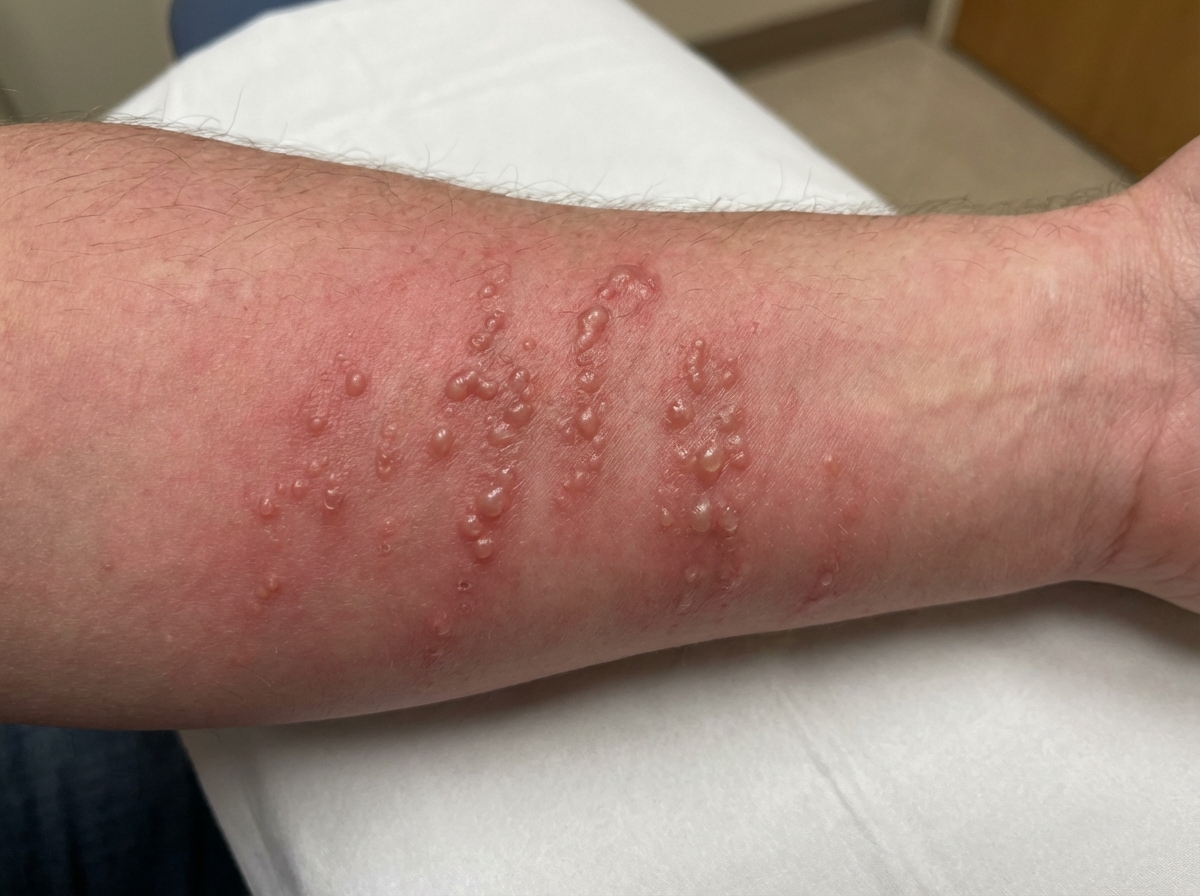
A 42-year-old woman comes to the clinic with a complaint of a severely itchy and painful rash on her hands and legs for a day. On further questioning, she revealed that she loves nature and goes on trekking to the woods frequently. She just returned from a similar trip, 2 days ago. On physical examination, a prominent rash along with multiple blisters is noted on the ventral aspect of her right forearm. A photograph of the rash is shown. Which of the following is the most likely reaction that the patient is experiencing?
A 12-month-old boy is brought to the physician by his parents for a 4-week history of fever, malaise, cough, and difficulty breathing. He has had recurrent episodes of gastroenteritis since birth. Cardiopulmonary examination shows subcostal retractions and crackles bilaterally. There is enlargement of the cervical, axillary, and inguinal lymph nodes. An x-ray of the chest shows bilateral consolidations. A sputum culture shows colonies of Burkholderia cepacia. A blood sample is obtained and after the addition of nitroblue tetrazolium to the sample, neutrophils remain colorless. A defect in which of the following is the most likely cause of this patient's condition?
A 33-year-old woman comes to the physician because of a 4-day history of fever, anterior neck pain, and throat swelling. She has no history of serious illness. Her temperature is 38.1°C (100.6°F) and pulse is 109/min. Physical examination shows diaphoresis and a fine tremor of the outstretched hands. The thyroid gland is enlarged, firm, and tender to palpation. Serum thyroid stimulating hormone level is 0.06 μU/mL and erythrocyte sedimentation rate is 65 mm/h. 123I scan shows an enlarged thyroid gland with diffusely decreased uptake. Histologic examination of a thyroid biopsy specimen is most likely to show which of the following findings?
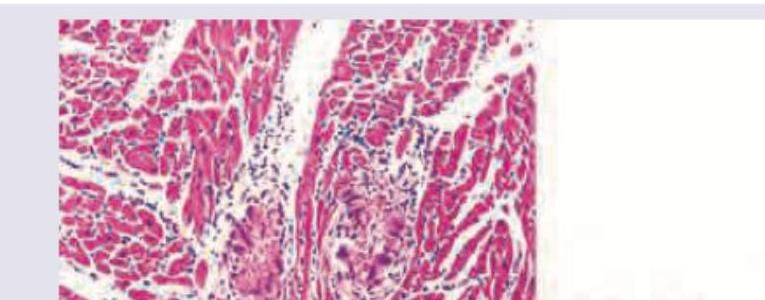
A 9-year-old boy from Eritrea is admitted to the hospital for lethargy and increased work of breathing. He has had recurrent episodes of fever, shortness of breath, and fatigue in the past 3 years. His pulse is 132/min and blood pressure is 90/66 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 82%. Auscultation of the chest shows coarse crackles in both lungs and a diastolic murmur at the cardiac apex. Despite appropriate lifesaving measures, he dies. A photomicrograph of a section of myocardium obtained at autopsy is shown. Which of the following is the most likely underlying cause of this patient's cardiac disease?
A 61-year-old-male underwent deceased donor liver transplantation 3 weeks ago. During his follow up visit he complains of nausea and abdominal pain. He has been taking all of his medications as prescribed. He has a history of alcohol abuse and his last drink was one year ago. He does not smoke cigarettes and lives at home with his wife. On physical examination temperature is 98.6°F (37°C), blood pressure is 115/80 mmHg, pulse is 90/min, respirations are 18/min, and pulse oximetry is 99% on room air. He has scleral icterus and a positive fluid wave. Liver function tests are as follows: Alkaline phosphatase: 110 U/L Aspartate aminotransferase (AST, GOT): 100 U/L Alanine aminotransferase (ALT, GPT): 120 U/L Bilirubin total: 2.2 mg/dL Liver biopsy shows mixed dense interstitial lymphocytic infiltrates in the portal triad. What is the mechanism of this reaction?
Practice by Chapter
Acute inflammation mechanisms
Practice Questions
Vascular changes in inflammation
Practice Questions
Chemical mediators of inflammation
Practice Questions
Cellular components of inflammation
Practice Questions
Resolution of acute inflammation
Practice Questions
Chronic inflammation
Practice Questions
Granulomatous inflammation
Practice Questions
Systemic effects of inflammation
Practice Questions
Patterns of inflammatory response
Practice Questions
Inflammatory markers in laboratory testing
Practice Questions
Anti-inflammatory therapies
Practice Questions
Wound healing and repair
Practice Questions
Abnormalities in wound healing
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
