Inflammation — MCQs

On this page
A 36-year-old man is brought to the emergency department by his wife 20 minutes after having a seizure. Over the past 3 days, he has had a fever and worsening headaches. This morning, his wife noticed that he was irritable and demonstrated strange behavior; he put the back of his fork, the salt shaker, and the lid of the coffee can into his mouth. He has no history of serious illness and takes no medications. His temperature is 39°C (102.2°F), pulse is 88/min, and blood pressure is 118/76 mm Hg. Neurologic examination shows diffuse hyperreflexia and an extensor response to the plantar reflex on the right. A T2-weighted MRI of the brain shows edema and areas of hemorrhage in the left temporal lobe. Which of the following is most likely the primary mechanism of the development of edema in this patient?
A 3-year-old male is brought by his mother to the pediatrician because she is concerned about a lump in his neck. She reports that the child was recently ill with a cough, nasal congestion, and rhinorrhea. She also noticed that a small red lump developed on the patient’s neck while he was sick. Although his cough and congestion subsided after a few days, the neck lump has persisted. The child has no notable past medical history. He was born at 39 weeks gestation and is in the 55th percentiles for both height and weight. His temperature is 98.6°F (37°C), blood pressure is 105/65 mmHg, pulse is 90/min, and respirations are 18/min. Physical examination reveals a small, soft, rounded mass at the midline of the neck inferior to the hyoid bone. The mass is warm and tender to palpation. It moves superiorly when the patient drinks water. Histologic examination of this lesion would most likely reveal which of the following?
A 50-year-old female presents to her physician with vesicles and tense blisters across her chest, arms, and the back of her shoulders. Physical examination reveals that blistering is not present in her oral mucosa, and the epidermis does not separate upon light stroking of the skin. The patient most likely suffers from a hypersensitivity reaction located:
A 6-year-old boy is brought to the emergency department due to a severe infection. Laboratory work shows leukocytosis of 60 × 109/L with marked left shift, but no blast cells. The patient is febrile and dehydrated. The physician believes that this is a severe reaction to the infection and orders a leukocyte alkaline phosphatase (LAP) stain on a peripheral smear. The LAP score is elevated. Which of the following statements best describes an additional characteristic of the condition this child is suffering from?
A 40-year-old man presents with a swollen left big toe that started this morning. The patient states that he attended a party last night and drank 4 glasses of whiskey. He denies any trauma to the foot. The patient has a history of similar episodes in the past that were related to alcohol use. His symptoms were previously relieved with ibuprofen. However, the pain persisted despite treatment with the medication. Physical examination reveals a tender and erythematous, swollen left 1st metatarsophalangeal joint. Which of the following events most likely contributed to his condition?
A 42-year-old woman with well-controlled HIV on antiretroviral therapy comes to the physician because of a 2-week history of a painless lesion on her right calf. Many years ago, she had a maculopapular rash over her trunk, palms, and soles that resolved spontaneously. Physical examination shows a 4-cm firm, non-tender, indurated ulcer with a moist, dark base and rolled edges. There is a similar lesion at the anus. Results of rapid plasma reagin testing are positive. Which of the following findings is most likely on microscopic examination of these lesions?
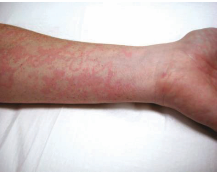
A 10-year-old boy presents with sudden shortness of breath. The patient’s mother says he was playing in the school garden 2 hours ago and suddenly started to complain of abdominal pain and vomited a few times. An hour later, he slowly developed a rash that involved his chest, arms, and legs, and his breathing became faster, with audible wheezing. He has no significant past medical history. His temperature is 37.0°C (98.6°F), blood pressure is 100/60 mm Hg, pulse is 130/min, and respirations are 25/min. On physical examination, there is a rash on his right arm (shown in the image, below). Which of the following cells will mainly be found in this patient if a histological sample is taken from the site of the skin lesion 4 hours from now?
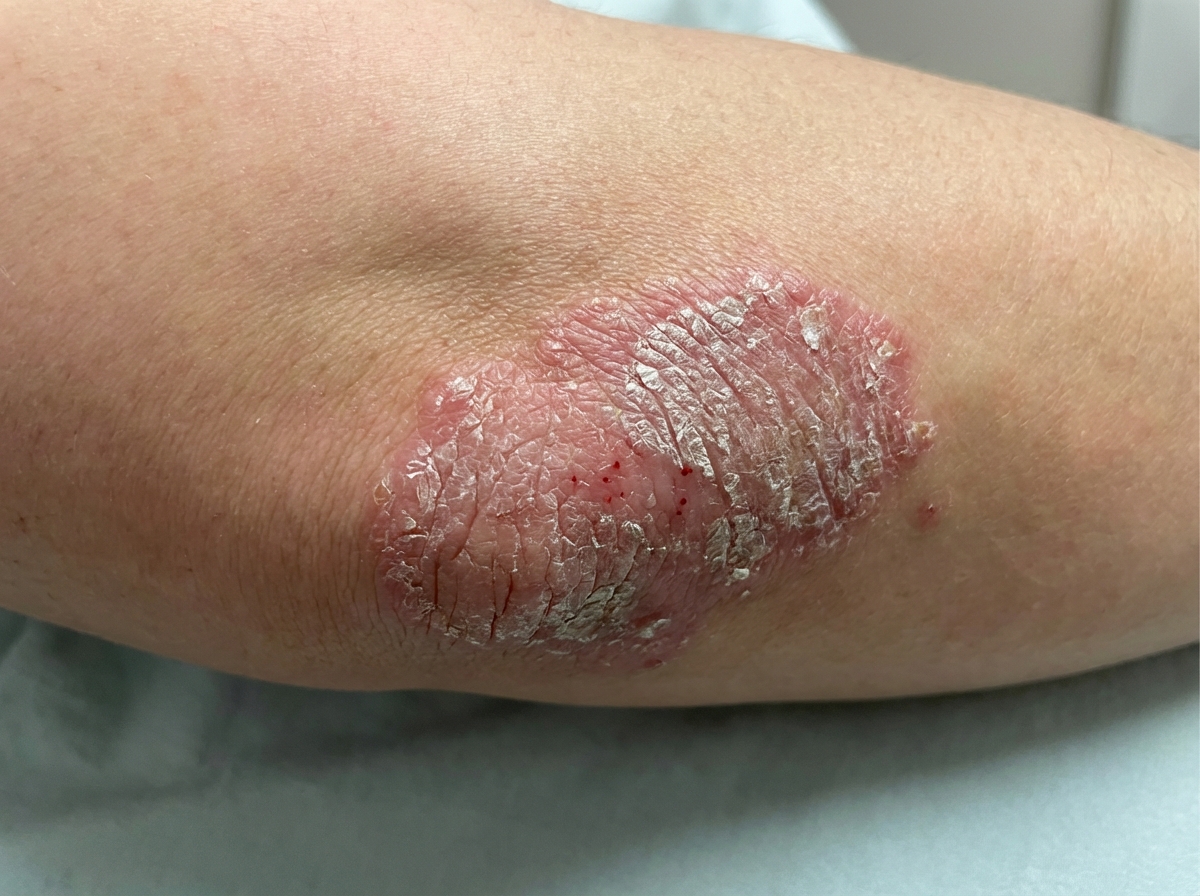
A 27-year-old man comes to the physician because of multiple, dry, scaly lesions on his elbows. The lesions appeared 4 months ago and have progressively increased in size. They are itchy and bleed when he scratches them. There is no associated pain or discharge. He was diagnosed with HIV infection 6 years ago. He has smoked a pack of cigarettes daily for the past 10 years. Current medications include raltegravir, lamivudine, abacavir, and cotrimoxazole. An image of the lesions is shown. His CD4+ T-lymphocyte count is 470/mm3 (normal ≥ 500). Which of the following is the most likely cause of this patient's skin findings?
A 37-year-old woman presents to the occupational health clinic for a new employee health screening. She has limited medical records prior to her immigration to the United States several years ago. She denies any current illness or significant medical history. Purified protein derivative (PPD) is injected on the inside of her left forearm for tuberculosis (TB) screening. Approximately 36 hours later, the patient comes back to the occupational health clinic and has an indurated lesion with bordering erythema measuring 15 mm in diameter at the site of PPD injection. Of the following options, which is the mechanism of her reaction?
A 22-year-old woman comes to the physician because of pain and swelling of her left foot. Three days ago, she cut her foot on an exposed rock at the beach. Her temperature is 37.7°C (100°F). Examination of the left foot shows edema around a fluctuant erythematous lesion on the lateral foot. Which of the following is most likely the primary mechanism for the development of edema in this patient?
Practice by Chapter
Acute inflammation mechanisms
Practice Questions
Vascular changes in inflammation
Practice Questions
Chemical mediators of inflammation
Practice Questions
Cellular components of inflammation
Practice Questions
Resolution of acute inflammation
Practice Questions
Chronic inflammation
Practice Questions
Granulomatous inflammation
Practice Questions
Systemic effects of inflammation
Practice Questions
Patterns of inflammatory response
Practice Questions
Inflammatory markers in laboratory testing
Practice Questions
Anti-inflammatory therapies
Practice Questions
Wound healing and repair
Practice Questions
Abnormalities in wound healing
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
