Inflammation — MCQs

On this page
A 40-year-old man comes to his doctor because of 2 weeks of progressively worsening pain on the outer side of his right elbow. He does not recall any trauma to the area. The patient plays tennis recreationally and has recently gone from playing weekly to playing daily in preparation for a local tournament. He has had some pain relief with ibuprofen. On physical examination, there is tenderness over the lateral surface of the right distal humerus. The pain is reproduced by supinating the forearm against resistance. Which of the following is the most likely underlying cause of this patient's condition?
A 33-year-old man with a history of IV drug and alcohol abuse presents to the emergency department with back pain. He states that his symptoms started 3 days ago and have been gradually worsening. His temperature is 102°F (38.9°C), blood pressure is 127/68 mmHg, pulse is 120/min, respirations are 17/min, and oxygen saturation is 98% on room air. Physical exam is notable for tenderness over the mid thoracic spine. Laboratory values are only notable for a leukocytosis and an elevated ESR and CRP. Which of the following is the most likely diagnosis?
A 48-year-old male dies in the intensive care unit following a severe Streptococcus pneumoniae pneumonia and septic shock. Autopsy of the lung reveals a red, firm left lower lobe. What would you most likely find on microscopic examination of the lung specimen?
A 68-year-old man is brought to the emergency department 30 minutes after the onset of uncontrollable jerking movements of his arms and legs followed by loss of consciousness. His wife says that he seemed confused this morning and had a headache. Immediately before the shaking episode, he said that he smelled rotten eggs. He is unresponsive. Cerebrospinal fluid (CSF) analysis shows a leukocyte count of 700/μL (70% lymphocytes), a glucose concentration of 60 mg/dL, and a protein concentration of 80 mg/dL. Despite appropriate lifesaving measures, the man dies. Which of the following is most likely to be found on postmortem examination of this patient?
A 45-year-old female is undergoing renal transplantation for management of chronic renal failure secondary to glomerulonephritis. The transplant surgeon placed the donor kidney in the recipient and anastomosed the donor renal artery to the recipient's external iliac artery as well as the donor ureter to the recipient's bladder. After removing the clamps on the external iliac artery, the recipient's blood is allowed to perfuse the transplanted kidney. Within 3 minutes, the surgeon notes that the kidney does not appear to be sufficiently perfused. Upon further investigation, an inflammatory reaction is noted that led to clotting off of the donor renal artery, preventing blood flow to the transplanted organ. Which of the following best describes the pathophysiology of this complication?
A 66-year-old farmer is being evaluated for abnormal lung findings on a low dose chest CT scan obtained as part of his lung cancer screening. He has a 50-pack-year smoking history and has been hesitant to quit. He has a non-productive cough but brushes it away saying he is not bothered by it. He denies ever coughing up blood, breathlessness, chest pain, fatigue, or weight loss. He has never sought any medical care and states that he has always been in good shape. He consumes alcohol moderately and uses marijuana occasionally. He lives with his wife and has not traveled recently. On physical examination, his temperature is 37.1°C (98.8°F), blood pressure is 148/70 mm Hg, and pulse rate is 95/min. His BMI is 32 kg/m2. A general physical examination is unremarkable. Coarse breath sounds are present bilaterally. The cardiac exam is normal. Laboratory studies show a normal complete blood count and comprehensive metabolic panel. A follow-up high-resolution CT scan is performed that shows small irregular subcentimeter pulmonary nodules, several of which are cavitated in both lungs, predominantly distributed in the upper and middle zones. There is no mediastinal or hilar lymphadenopathy. A transbronchial needle aspiration of the lesion is performed which shows a nodular pattern of abundant, granular, mildly eosinophilic cells with grooved nuclei with indented nuclear membranes and a chronic inflammation that consists primarily of eosinophils. Immunohistochemical staining reveals numerous cells that stain positive for S100 and CD1a. Which of the cells of the human immune system are responsible for this lesion?
A 28-year-old man is referred to the dermatologist for 2 months of increasing appearance of multiple smooth, circular patches of complete hair loss on his scalp. He says that the patches have associated pruritus and a burning sensation, and are not improving with the over-the-counter products recommended by his hair stylist. He denies pulling his hair intentionally. Physical examination reveals no epidermal inflammation or erythema, and no fluorescence is detected under Wood’s lamp. A punch biopsy shows a peribulbar lymphocytic inflammatory infiltrate surrounding anagen follicles, resembling a swarm of bees. Which of the following is the most likely diagnosis in this patient?
A 15-year-old girl is brought to the physician by her mother for a 2-day history of abdominal pain, nausea, vomiting, diarrhea, and decreased appetite. Her last menstrual period was 3 weeks ago. Her temperature is 37.6°C (99.7°F). Abdominal examination shows tenderness to palpation with guarding in the right lower quadrant. Laboratory studies show a leukocyte count of 12,600/mm3. Which of the following is the most likely underlying cause of this patient's condition?
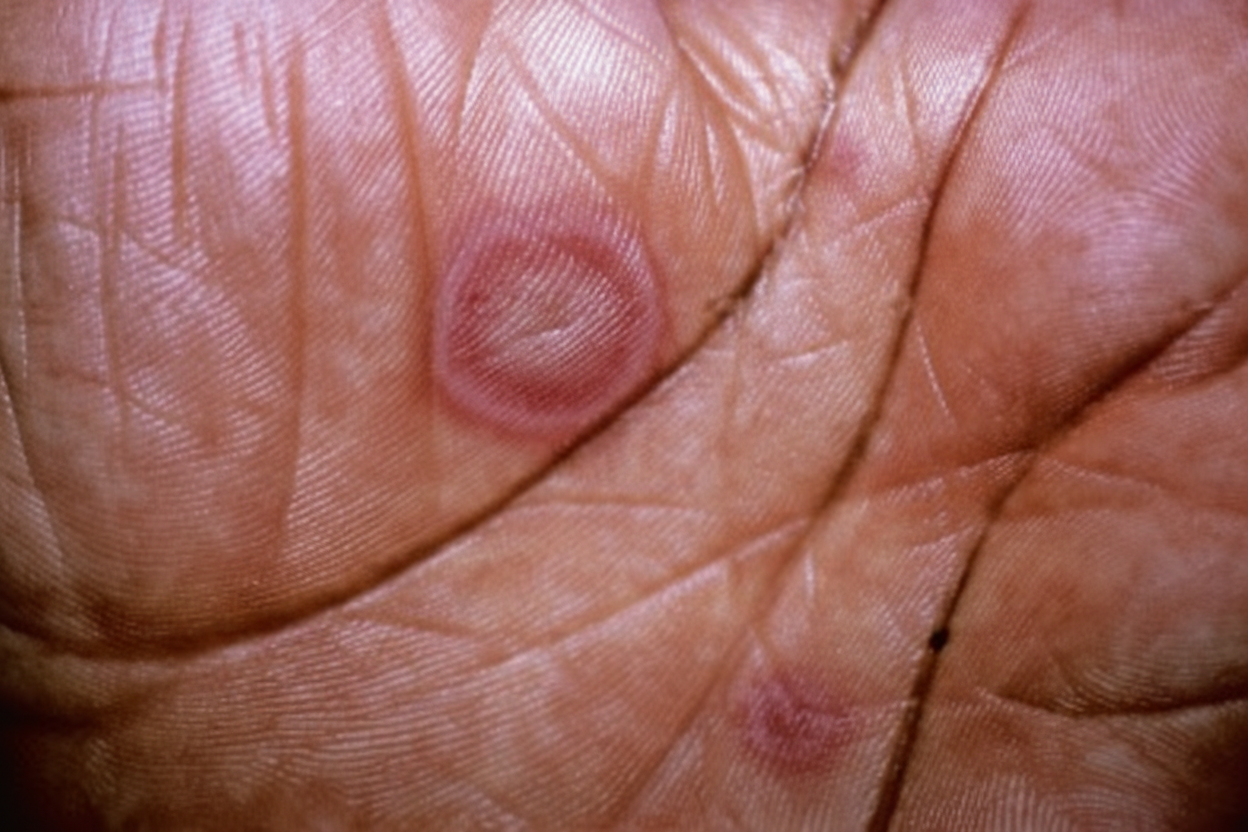
A 19-year-old man presents with painful oral ulcers and rash. He says that his symptoms started 1 week ago with a low-grade fever, malaise, and cough. Then, 3 days ago, he noted small painful red bumps on his hands and feet, which quickly worsened and spread to involve his extremities and upper torso. At the same time, multiple painful oral ulcers appeared, which have not improved. He denies any trouble breathing, pruritus, hemoptysis, hematochezia, or similar symptoms in the past. Past medical history is significant for a recent methicillin-resistant staphylococcus aureus (MRSA) skin infection 2 weeks ago secondary to a laceration on his left leg for which he has been taking trimethoprim-sulfamethoxazole. No other current medications. The patient is afebrile, and his vital signs are within normal limits. Physical examination reveals multiple raised, erythematous, circular papules averaging 1–2 cm in diameter with a central bulla, as shown in the exhibit (see image below). The cutaneous lesions occupy < 10% of his total body surface area (BSA). Nikolsky sign is negative. Multiple mucosal erosions are noted in the oral cavity. Generalized lymphadenopathy is present. A well-healing laceration is present on the left leg with no evidence of drainage or fluctuance. A cutaneous punch biopsy of one of the lesions is performed. Which of the following histopathologic features would most likely be found on this patient's biopsy?
A 34-year-old woman comes to the physician because of a 6-week history of fever and productive cough with blood-tinged sputum. She has also had a 4-kg (8.8-lb) weight loss during the same time period. Examination shows enlarged cervical lymph nodes. An x-ray of the chest shows a 2.5-cm pulmonary nodule in the right upper lobe. A biopsy specimen of the lung nodule shows caseating granulomas with surrounding multinucleated giant cells. Which of the following is the most likely underlying cause of this patient's pulmonary nodule?
Practice by Chapter
Acute inflammation mechanisms
Practice Questions
Vascular changes in inflammation
Practice Questions
Chemical mediators of inflammation
Practice Questions
Cellular components of inflammation
Practice Questions
Resolution of acute inflammation
Practice Questions
Chronic inflammation
Practice Questions
Granulomatous inflammation
Practice Questions
Systemic effects of inflammation
Practice Questions
Patterns of inflammatory response
Practice Questions
Inflammatory markers in laboratory testing
Practice Questions
Anti-inflammatory therapies
Practice Questions
Wound healing and repair
Practice Questions
Abnormalities in wound healing
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
