GI — MCQs

On this page
A 55-year-old female comes to see her doctor for a rapidly enlarging abdomen and swelling of both legs. She was hospitalized 2 weeks ago for an upper gastrointestinal bleeding episode. On that occasion, her esophagogastroduodenoscopy showed grade 1 esophageal varices and a 1 cm clean-based antral ulcer. The patient was discharged on omeprazole. Review of symptoms shows that the patient is forgetful, does not sleep well, and is drowsy and fatigued during the day which prevents her from working full-time. She denies abdominal pain. The patient has a 10-year history of type 2 diabetes mellitus, hypertension, and hypercholesterolemia but no history of angina or coronary heart disease. She drank alcohol moderately heavy in her twenties and currently drinks less than 3 drinks per week and does not smoke. Her family history is unremarkable. On physical examination, her blood pressure is 132/82 mm Hg, pulse is 88/min, and her temperature is 37.0°C (98.6°F). She weighs 106.6 kg (235 lb) and her BMI is 33. She is alert, oriented to person, place, year, and month but not to the day. Her sclerae are nonicteric. Her pulmonary and cardiovascular exam are normal but her abdomen is distended with a fluid wave and mild tenderness to palpation. There is no hepatosplenomegaly. There is a 2+ edema to mid-calf and pedal pulses are barely palpable. Her neurological exam is without motor or sensory deficits but she demonstrates flapping tremor of her hands while asked to hold them in front of her for a few seconds and her skin exam shows a few spider telangiectasias on her face and upper chest. After an initial evaluation, lab tests were obtained: Serum sodium 133 mEq/L Serum potassium 3.8 mEq/L BUN 8 mg/dL Serum creatinine 1.0 mg/dL Serum albumin 2.5 mg/dL Aspartate aminotransferase 68 IU/ml Alanine aminotransferase 46 IU/ml Alkaline phosphatase 130 IU/ml Total bilirubin 1.8 mg/dL WBC count 4,200/mm3 Platelets 94,000/mm3 Hematocrit 35.5% Prothrombin time (INR) 1.5 A liver biopsy is performed and the results are pending. The hepatocytes causing her acute issue are predominantly located in which area of the hepatic lobule?
A 52-year-old Caucasian male presents to your office complaining of black, tarry stool. Which of the following possible causes of this patient's presentation is LEAST associated with the development of carcinoma?
A 25-year-old male presents to his primary care physician for fatigue, abdominal pain, diarrhea, and weight loss. He states that this issue has occurred throughout his life but seems to “flare up” on occasion. He states that his GI pain is relieved with defecation, and his stools are frequent, large, and particularly foul-smelling. The patient has a past medical history of an ACL tear, as well as a car accident that resulted in the patient needing a transfusion and epinephrine to treat transfusion anaphylaxis. His current medications include vitamin D and ibuprofen. He recently returned from a camping trip in the eastern United States. He states that on the trip they cooked packed meats over an open fire and obtained water from local streams. His temperature is 99.5°F (37.5°C), blood pressure is 120/77 mmHg, pulse is 70/min, respirations are 11/min, and oxygen saturation is 98% on room air. Physical exam reveals poor motor control and an ataxic gait on neurologic exam. Cardiac and pulmonary exams are within normal limits. Laboratory studies are ordered and return as below: Hemoglobin: 9.0 g/dL Hematocrit: 25% Haptoglobin: 12 mg/dL Leukocyte count: 7,500 cells/mm^3 with normal differential Platelet count: 255,000/mm^3 Serum: Na+: 140 mEq/L Cl-: 102 mEq/L K+: 5.0 mEq/L HCO3-: 24 mEq/L BUN: 24 mg/dL Glucose: 82 mg/dL Creatinine: 1.0 mg/dL Ca2+: 9.0 mg/dL LDH: 457 U/L AST: 11 U/L ALT: 11 U/L Radiography is ordered which reveals a stress fracture in the patient’s left tibia. Which of the following is the best confirmatory test for this patient’s condition?
A 59-year-old woman comes to the physician because of a 1-year history of nausea and chronic abdominal pain that is worse after eating. She has Hashimoto thyroiditis. She does not smoke or drink alcohol. A biopsy specimen of the corpus of the stomach shows destruction of the upper glandular layer of the gastric mucosa and G-cell hyperplasia. This patient is at greatest risk for which of the following conditions?
Two weeks after returning from vacation in Mexico, a 21-year-old man comes to the emergency department because of malaise, nausea, vomiting, fever, and abdominal pain. He has no history of serious illness and takes no medications. Physical examination shows scleral icterus and right upper quadrant tenderness. The liver is palpated 1.5 cm below the right costal margin. A biopsy specimen of this patient's liver would most likely show which of the following findings?
A 52-year-old man presents with 2 months of diarrhea, abdominal pain, and fatigue. He reports a weight loss of 4 kg (8 lb). He also says his joints have been hurting recently, as well. Past medical history is unremarkable. Review of systems is significant for problems with concentration and memory. Physical examination is unremarkable. A GI endoscopy is performed with a biopsy of the small bowel. Which of the following histologic finding would most likely be seen in this patient?
A 22-year-old Caucasian female presents with severe right lower quadrant pain, malaise, and diarrhea. The physician performs an endoscopy and finds disease involvement in the terminal ileum, noting that the disease process is patchy with normal intervening mucosa. The entire wall of the region is thickened and inflamed, which may directly lead to formation of:
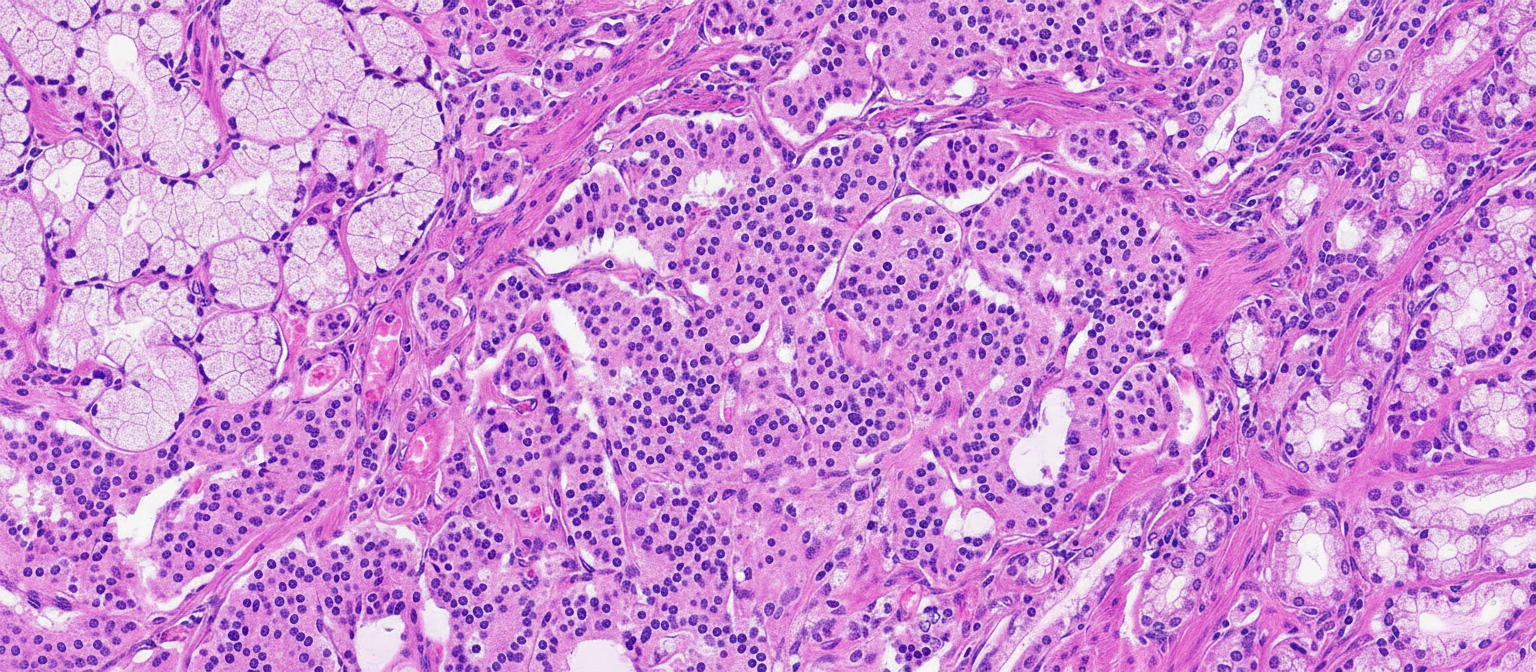
A previously healthy 67-year-old man comes to the physician because of a history of recurrent right lower abdominal pain for the past 2 years. A CT scan shows a 1.2-cm (0.47-in) mass located in the terminal ileum. He undergoes surgical removal of the mass. A photomicrograph of the resected specimen is shown. Cells from this tissue are most likely to stain positive for which of the following?
An otherwise healthy 56-year-old man comes to the physician for a 2-year history of recurrent upper abdominal pain and fullness that worsens after meals. Urea breath test is positive. An endoscopy shows diffuse mucosal atrophy and patchy erythema, but no ulcer. A biopsy from which of the following areas is most likely to yield an accurate diagnosis?
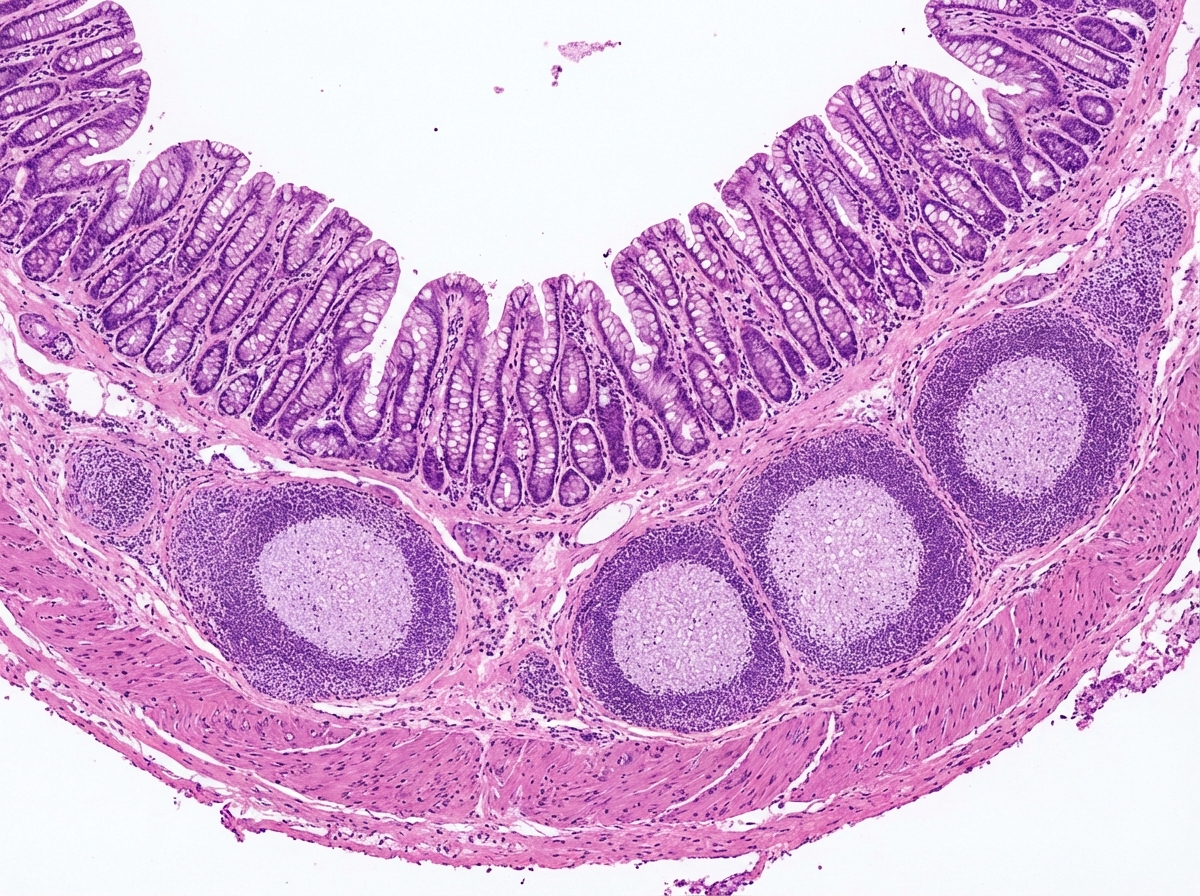
A 13-year-old boy presents to the emergency department with severe right-lower-quadrant abdominal pain. Workup reveals acute appendicitis, and he subsequently undergoes laparoscopic appendectomy. The appendix is sent for histological examination. A pathologist reviews the slide shown in the image below. Which statement about the structures marked within the yellow circles is correct?
Practice by Chapter
Esophageal pathology
Practice Questions
Gastritis and peptic ulcer disease
Practice Questions
Gastric tumors
Practice Questions
Malabsorption syndromes
Practice Questions
Inflammatory bowel diseases
Practice Questions
Intestinal infections
Practice Questions
Diverticular disease
Practice Questions
Vascular disorders of bowel
Practice Questions
Colon polyps and neoplasms
Practice Questions
Appendicitis
Practice Questions
Peritonitis
Practice Questions
Hernia complications
Practice Questions
Gastrointestinal stromal tumors
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
