GI — MCQs

On this page
A 22-year-old man comes to the physician because of a 3-week history of abdominal pain, loose, non-bloody stools, and intermittent nausea. He also reports intermittent fever. He has not had vomiting, tenesmus, or rectal pain. He has no history of serious illness and takes no medications. His vital signs are within normal limits. Rectal exam is unremarkable. Laboratory studies show a leukocyte count of 15,200/mm3 and an erythrocyte sedimentation rate of 44 mm/h. Test of the stool for occult blood and stool studies for infection are negative. A CT scan of the abdomen shows mural thickening and surrounding fat stranding of discrete regions of the terminal ileum and transverse colon. A colonoscopy is performed and biopsy specimens of the affected areas of the colon are taken. Which of the following findings is most specific for this patient's most likely diagnosis?
A 22-year-old woman presents to the emergency department with a 3-day history of fever and abdominal pain. She says that the pain is located in the left lower quadrant of the abdomen and feels crampy in nature. The pain has been associated with bloody diarrhea and joint tenderness. She has no past medical history but says that she returned 2 weeks ago from vacation in Asia where she tried many new foods. Her family history is significant for multiple cancers in close relatives. Physical exam reveals swollen ulcers on her legs, and colonoscopy reveals contiguous ulcerations from the rectum through the descending colon. Which of the following is associated with the most likely cause of this patient's symptoms?
A 45-year-old man comes to the physician for his routine health maintenance examination. He was diagnosed with diabetes mellitus 4 years ago. His medical history is otherwise unremarkable. He takes no medications other than daily metformin. He has consumed a can of beer every night for the past 10 years. His blood pressure is 145/90 mm Hg. His body mass index is 31 kg/m2. Physical examination shows no abnormalities. Laboratory studies show: Partial thromboplastin time (activated) 30 seconds (N=25-40 seconds) Prothrombin time 13 seconds (N=11-15 seconds) International normalized ratio 1.2 Serum albumin 4 g/dL Bilirubin, total 0.9 mg/dL Direct 0.2 mg/dL Alkaline phosphatase 45 U/L Aspartate aminotransferase (AST, GOT) 43 U/L Alanine aminotransferase (ALT, GPT) 56 U/L γ-Glutamyltransferase (GGT) 43 U/L (N=5-50 U/L) Hepatitis A antibody Negative Hepatitis B surface antigen Negative Hepatitis C antibody Negative Liver biopsy shows excessive intracellular fat accumulation, hepatocyte ballooning, and perivenular infiltration of lymphocytes and neutrophils without significant fibrosis. Which of the following best describes these findings?
A 28-year-old man comes to the physician because of a 6-month history of progressive fatigue and intermittent diarrhea. During this time, he has had a 6-kg (13-lb) weight loss. Physical examination shows pale conjunctivae. Abdominal examination shows tenderness to palpation in the lower quadrants. An image from a colonoscopy of the descending colon is shown. Further evaluation is most likely to show which of the following findings?
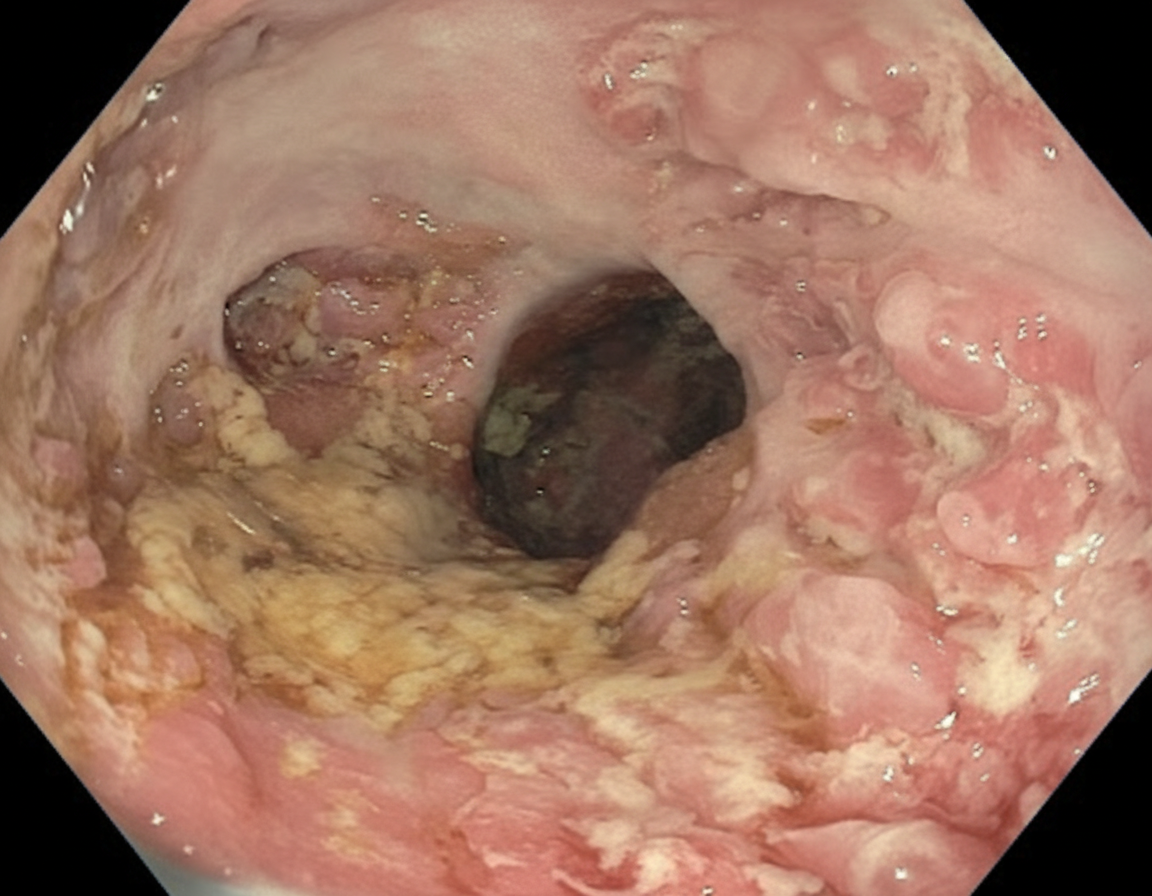
A 35-year-old Caucasian female presents with anemia, malaise, bloating, and diarrhea. Past genetic testing revealed that this patient carries the HLA-DQ2 allele. The physician suspects that the patient's presentation is dietary in cause. Which of the following findings would definitively confirm this diagnosis?
A 55-year-old female presents to the emergency room complaining of severe abdominal pain. She reports a six-month history of worsening dull mid-epigastric pain that she had attributed to stress at work. She has lost fifteen pounds over that time. She also reports that her stools have become bulky, foul-smelling, and greasy. Over the past few days, her abdominal pain acutely worsened and seemed to radiate to her back. She also developed mild pruritus and yellowing of her skin. Her temperature is 101°F (38.3°C), blood pressure is 145/85 mmHg, pulse is 110/min, and respirations are 20/min. On examination, her skin appears yellowed and she is tender to palpation in her mid-epigastrium and right upper quadrant. She is subsequently sent for imaging. If a mass is identified, what would be the most likely location of the mass?
A 2-year-old boy is brought in to his pediatrician for a routine checkup. The parents mention that the child has been developing appropriately, although they have been noticing that the child appears to have chronic constipation. The parents report that their child does not routinely have daily bowel movements, and they have noticed that his abdomen has become more distended recently. In the past, they report that the patient was also delayed in passing meconium, but this was not further worked up. On exam, his temperature is 98.6°F (37.0°C), blood pressure is 110/68 mmHg, pulse is 74/min, and respirations are 14/min. The patient is noted to have a slightly distended abdomen that is nontender. Eventually, this patient undergoes a biopsy. Which of the following layers most likely reveals the causative pathologic finding of this disease?
A 12-month-old boy is brought to the emergency department by his mother for several hours of crying and severe abdominal pain, followed by dark and bloody stools in the last hour. The mother reports that she did not note any vomiting or fevers leading up to this incident. She does report that the boy and his 7-year-old sister recently had “stomach bugs” but that both have been fine and that the sister has gone back to school. The boy was born by spontaneous vaginal delivery at 39 weeks and 5 days after a normal pregnancy. His temperature is 100.4°F (38.0°C), blood pressure is 96/72 mmHg, pulse is 90/min, respirations are 22/min. Which of the following was most likely to play a role in the pathogenesis of this patient’s disease?
A 57-year-old man presents with fever and yellow discoloration of the skin for the past 4 days. He denies any recent weight loss or changes in urine or stool color. His past medical history is unremarkable. He admits to drinking about 130 g/day of alcohol and says he has been doing so for the past 25 years. His wife who is accompanying him during this visit adds that once her husband drank 15 cans of beer at a funeral. The patient also reports a 10-pack-year smoking history. His vital signs include: pulse 98/min, respiratory rate 13/min, temperature 38.2°C (100.8°F) and blood pressure 120/90 mm Hg. On physical examination, the patient appears jaundiced and is ill-appearing. Sclera is icteric. Abdominal examination reveals tenderness to palpation in the right upper quadrant with no rebound or guarding. Percussion reveals significant hepatomegaly extending 3 cm below the right costal margin. Laboratory studies are significant for the following: Sodium 135 mEq/L Potassium 3.5 mEq/L ALT 240 U/L AST 500 U/L A liver biopsy is obtained but the results are pending. Which of the following would most likely be seen in this patient's biopsy?
A 30-year-old man comes to the physician because of an episode of bloody vomiting this morning and a 1-week history of burning upper abdominal pain. Two weeks ago, he sustained a head injury and was in a coma for 3 days. An endoscopy shows multiple, shallow hemorrhagic lesions predominantly in the gastric fundus and greater curvature. Biopsies show patchy loss of epithelium and an acute inflammatory infiltrate in the lamina propria that does not extend beyond the muscularis mucosa. Which of the following is the most likely diagnosis?
Practice by Chapter
Esophageal pathology
Practice Questions
Gastritis and peptic ulcer disease
Practice Questions
Gastric tumors
Practice Questions
Malabsorption syndromes
Practice Questions
Inflammatory bowel diseases
Practice Questions
Intestinal infections
Practice Questions
Diverticular disease
Practice Questions
Vascular disorders of bowel
Practice Questions
Colon polyps and neoplasms
Practice Questions
Appendicitis
Practice Questions
Peritonitis
Practice Questions
Hernia complications
Practice Questions
Gastrointestinal stromal tumors
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
