GI — MCQs

On this page
A 52-year-old woman presents with mild epigastric pain and persistent heartburn for the past 2 months. An endoscopy is performed and reveals inflammation of the stomach mucosa without evidence of ulceration. A biopsy is performed and reveals intestinal metaplasia with destruction of a large number of parietal cells. She is diagnosed with chronic atrophic gastritis. Which of the following is characteristic of this patient’s diagnosis?
A 49-year-old woman presents to the primary care physician with complaints of recurrent episodes of right upper abdominal pain for the past 2 years. She is currently symptom-free. She mentions that the pain often occurs after a heavy fatty meal and radiates to her right shoulder. On examination, the patient has no tenderness in the abdomen and all other systemic examination is normal. Blood work shows: Leukocyte count 8,000/mm³ Total bilirubin 1.2 mg/dL Prothrombin time 12 s Aspartate transaminase 58 IU/L Alanine transaminase 61 IU/L Serum albumin 4.1 g/dL Stool occult blood negative Ultrasonography of the abdomen shows a thickened gallbladder wall with few gallstones. A hydroxy iminodiacetic acid (HIDA) scan was done which demonstrated non-filling of the gallbladder and a minimal amount of tracer in the common bile duct. Which of the following best describes a histopathological feature in the gallbladder described in this case?
A 67-year-old man with hypertension comes to the emergency department because of progressively worsening abdominal pain that started 1 week ago. The pain is localized to the right upper quadrant. He has also noticed yellowing of his eyes and skin during this time period. Physical examination shows jaundice, a distended abdomen, and tender hepatomegaly. There is no jugular venous distention. Laboratory studies show a hemoglobin concentration of 19.2 g/dL, aspartate aminotransferase of 420 U/L, alanine aminotransferase of 318 U/L, and total bilirubin of 2.2 mg/dL. Which of the following is the most likely cause of this patient's symptoms?
A 62-year-old woman with a history of hypertension, hyperlipidemia, and rheumatoid arthritis presents for evaluation of elevated serum liver chemistries. She has had three months of intense, unremitting itching. Current medications include chlorthalidone, atorvastatin, and ibuprofen. Physical exam is unremarkable. Laboratory studies show aspartate aminotransferase (AST) 42 units/L, alanine aminotransferase (ALT) 39 units/L, alkaline phosphatase 790 units/L, total bilirubin 0.8 mg/dL, and antimitochondrial antibody titer 1:80. What do you expect to see on liver biopsy?
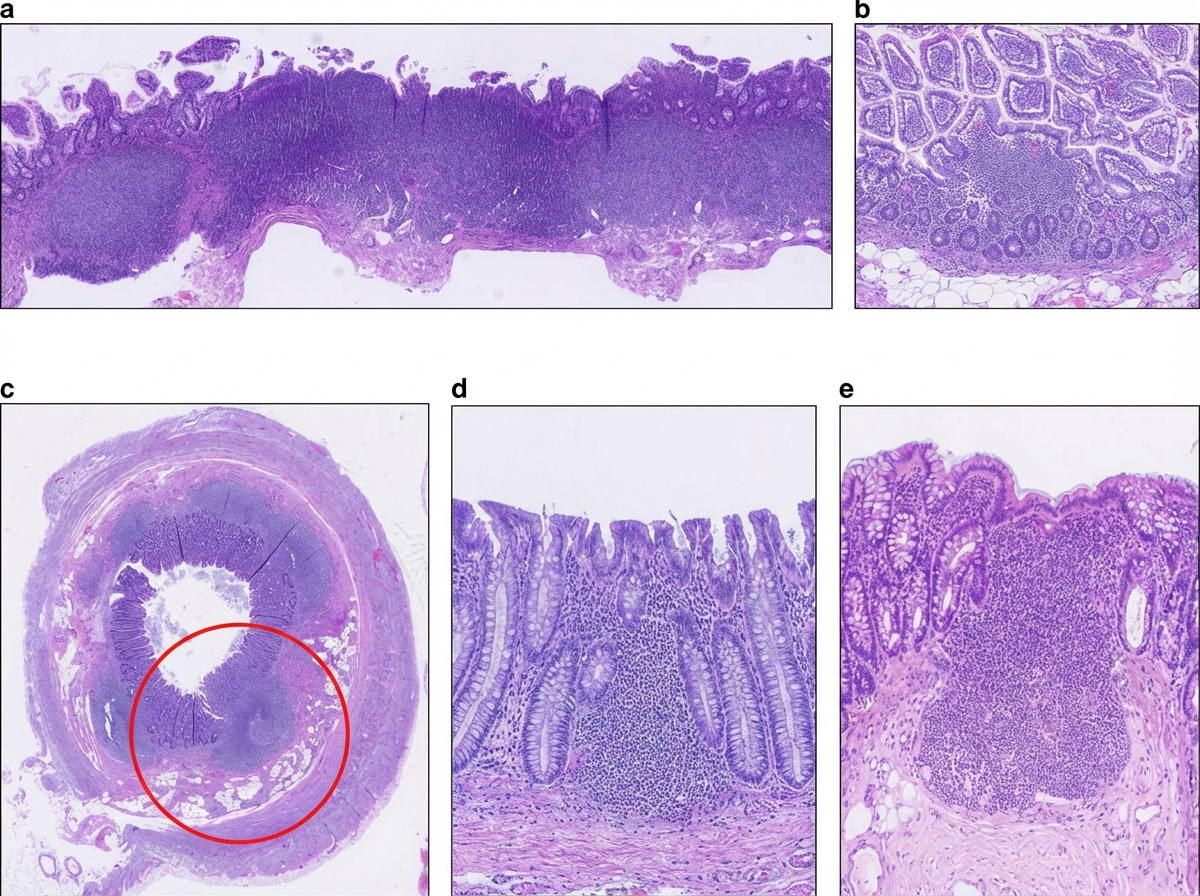
A 36-year-old man undergoes ileocecal resection after a gunshot injury. The resected ileocecal segment is sent for histological evaluation. One of the slides derived from the specimen is shown in the image. Which of the following statements regarding the structure marked within the red circle is correct?
A 56-year-old man comes to the physician because of intermittent retrosternal chest pain. Physical examination shows no abnormalities. Endoscopy shows salmon pink mucosa extending 5 cm proximal to the gastroesophageal junction. Biopsy specimens from the distal esophagus show nonciliated columnar epithelium with numerous goblet cells. Which of the following is the most likely cause of this patient's condition?
A 34-year-old man with worsening refractory epigastric pain secondary to long-standing gastroesophageal reflux disease presents for endoscopic evaluation. Past medical history is also significant for type 2 diabetes mellitus that was diagnosed 3 years ago, managed medically. Current medications are metformin, metoclopramide, and omeprazole. Which of the following best describes this patient’s most likely endoscopic findings?
A 47-year-old man presents with daily substernal chest pain for the past year. In addition, he says that he often suffers from hoarseness and a cough in the mornings. His wife has also reported that he has developed bad breath. Past medical history is significant for diabetes mellitus, managed with metformin. His physical examination is unremarkable. ECG is normal. An esophagogastroduodenoscopy is performed. The lower third of the esophagus appears erythematous, and a biopsy of the gastroesophageal junction is taken. When he is given sublingual nitroglycerin, it is noted that his chest discomfort is worsened. Which of the following would be expected in this patient’s biopsy?
A 41-year-old male who takes NSAIDs regularly for his chronic back pain develops severe abdominal pain worse with eating. Upper endoscopy is performed and the medical student asks the supervising physician how the histological differentiation between a gastric ulcer and erosion is made. Which of the following layers of the gastric mucosa MUST be breached for a lesion to be considered an ulcer?
A 49-year-old woman is admitted to the hospital for the evaluation of postprandial colicky pain in the right upper quadrant of the abdomen. Abdominal ultrasound shows multiple round, hyperechoic structures within the gallbladder lumen. She undergoes a cholecystectomy. A photograph of the content of her gallbladder is shown. This patient is most likely to have which of the following additional conditions?

Practice by Chapter
Esophageal pathology
Practice Questions
Gastritis and peptic ulcer disease
Practice Questions
Gastric tumors
Practice Questions
Malabsorption syndromes
Practice Questions
Inflammatory bowel diseases
Practice Questions
Intestinal infections
Practice Questions
Diverticular disease
Practice Questions
Vascular disorders of bowel
Practice Questions
Colon polyps and neoplasms
Practice Questions
Appendicitis
Practice Questions
Peritonitis
Practice Questions
Hernia complications
Practice Questions
Gastrointestinal stromal tumors
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
