Gastritis and peptic ulcer disease — MCQs

A 41-year-old female complains of frequent diarrhea and abdominal pain between meals. Endoscopy reveals a duodenal ulcer distal to the duodenal bulb. CT scan of the abdomen demonstrates a pancreatic mass, and subsequent tissue biopsy of the pancreas reveals a malignant islet cell tumor. Which of the following hormones is likely to be markedly elevated in this patient:
A 45-year-old man comes to the emergency department because of a 1-day history of black, tarry stools. He has also had upper abdominal pain that occurs immediately after eating and a 4.4-kg (9.7-lb) weight loss in the past 6 months. He has no history of major medical illness but drinks 3 beers daily. His only medication is acetaminophen. He is a financial consultant and travels often for work. Physical examination shows pallor and mild epigastric pain. Esophagogastroduodenoscopy shows a bleeding 15-mm ulcer in the antrum of the stomach. Which of the following is the strongest predisposing factor for this patient's condition?
A 56-year-old woman with a longstanding history of gastroesophageal reflux presents for follow-up evaluation of endoscopically confirmed gastric and duodenal ulcers. Her symptoms have been unresponsive to proton pump inhibitors and histamine receptor antagonists in the past. Results for H. pylori infection are still pending. Which of the following changes is expected in the patient's duodenum, given her peptic ulcer disease?
A 42-year-old man comes to his primary care physician complaining of abdominal pain. He describes intermittent, burning, epigastric pain over the past 4 months. He reports that the pain worsens following meals. He had an upper gastrointestinal endoscopy done 2 months ago that showed a gastric ulcer without evidence of malignancy. The patient was prescribed pantoprazole with minimal improvement in symptoms. He denies nausea, vomiting, diarrhea, or melena. The patient has no other medical problems. He had a total knee replacement 3 years ago following a motor vehicle accident for which he took naproxen for 2 months for pain management. He has smoked 1 pack per day since the age of 22 and drinks 1-2 beers several nights a week with dinner. He works as a truck driver, and his diet consists mostly of fast food. His family history is notable for hypertension in his paternal grandfather and coronary artery disease in his mother. On physical examination, the abdomen is soft, nondistended, and mildly tender in the mid-epigastric region. A stool test is positive for Helicobacter pylori antigen. In addition to antibiotic therapy, which of the following is the most likely to decrease the recurrence of the patient's symptoms?
A 53-year-old patient presents to his primary care provider with a 1-week history of abdominal pain at night and between meals. He has attempted taking antacids, which help briefly, but then the pain returns. The patient has not noticed any changes to the color of his stool but states that he has been having some loose bowel movements. The patient reports that he has had duodenal ulcers in the past and is concerned that this is a recurrence. On exam, his temperature is 98.4°F (36.9°C), blood pressure is 130/84 mmHg, pulse is 64/min, and respirations are 12/min. The abdomen is soft, nontender, and nondistended in clinic today. A fecal occult blood test is positive for blood in the stool. During outpatient workup, H. pylori stool antigen is negative, endoscopy demonstrates duodenal ulcers, and gastrin levels are elevated after a secretin stimulation test. Which of the following should also be examined in this patient?
A 45-year-old man is brought to the emergency department because of severe abdominal pain for the past 2 hours. He has a 2-year history of burning epigastric pain that gets worse with meals. His pulse is 120/min, respirations are 22/min, and blood pressure is 60/40 mm Hg. Despite appropriate lifesaving measures, he dies. At autopsy, examination shows erosion of the right gastric artery. Perforation of an ulcer in which of the following locations most likely caused this patient's findings?
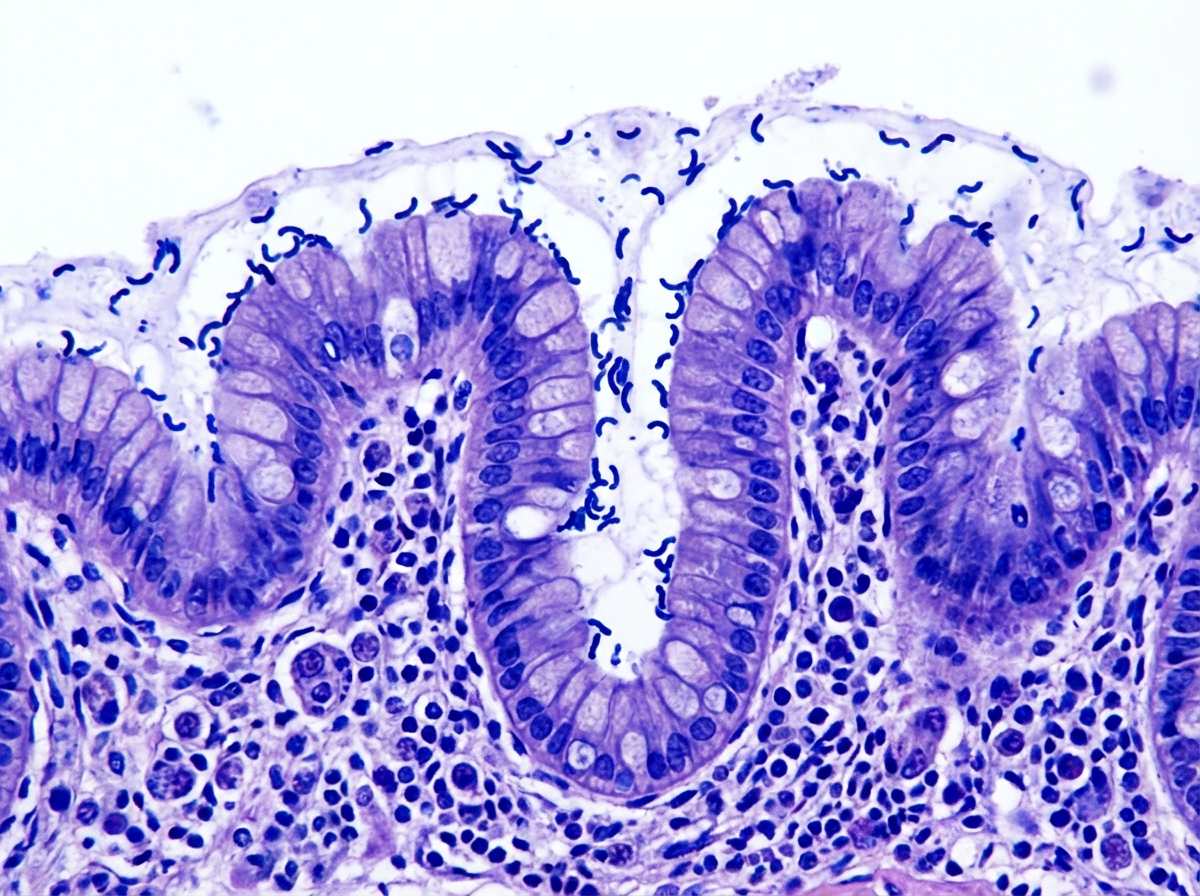
A 51-year-old man seeks evaluation from his family physician with a complaint of heartburn, which has been gradually increasing over the last 10 years. The heartburn gets worse after eating spicy foods and improves with antacids. The past medical history is benign. He is a security guard and works long hours at night. He admits to smoking 1.5 packs of cigarettes every day. Upper gastrointestinal endoscopy reveals several gastric ulcers and regions of inflammation. A biopsy is obtained, which revealed gram-negative bacteria colonized on the surface of the regenerative epithelium of the stomach, as shown in the micrograph below. Which of the following bacterial products is responsible for neutralizing the acidity of the stomach?
A 74-year-old man presents to the emergency department with sudden onset of abdominal pain that is most felt around the umbilicus. The pain began 16 hours ago and has no association with meals. He has not been vomiting, but he has had several episodes of bloody loose bowel movements. He was hospitalized 1 week ago for an acute myocardial infarction. He has had diabetes mellitus for 35 years and hypertension for 20 years. He has smoked 15–20 cigarettes per day for the past 40 years. His temperature is 36.9°C (98.4°F), blood pressure is 95/65 mm Hg, and pulse is 95/min. On physical examination, the patient is in severe pain, there is a mild periumbilical tenderness, and a bruit is heard over the epigastric area. Which of the following is the most likely diagnosis?
A 27-year-old woman presents to her primary care physician for evaluation of involuntary weight loss and recurrent abdominal pain. She noticed blood in her stool several times. The medical history is significant for the polycystic ovarian syndrome. The vital signs are as follows: temperature, 38.0°C (100.4°F); heart rate, 78/min; respiratory rate, 14/min; and blood pressure, 110/80 mm Hg. The family history is notable for paternal colon cancer. A colonoscopy is performed and is presented in the picture. What findings are expected?
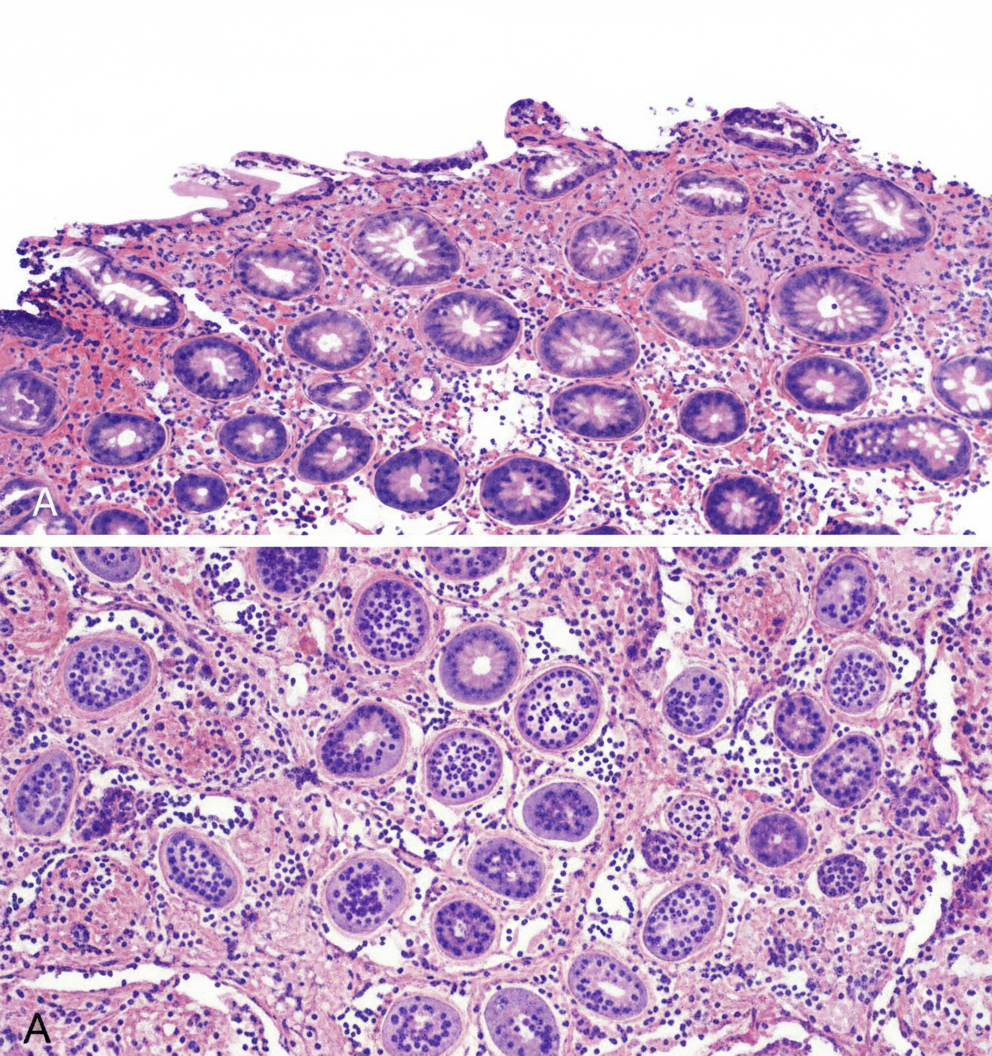
A 59-year-old woman comes to the clinic complaining of an intermittent, gnawing epigastric pain for the past 2 months. The pain is exacerbated with food and has been getting progressively worse. The patient denies any weight changes, nausea, vomiting, cough, or dyspepsia. Medical history is significant for chronic back pain for which she takes ibuprofen. Her father passed at the age of 55 due to pancreatic cancer. Labs were unremarkable except for a mild decrease in hemoglobin. What medication is most appropriate to be switched to from the current medication at this time?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
